Science Bulletin ( IF 18.8 ) Pub Date : 2021-07-27 , DOI: 10.1016/j.scib.2021.07.033 Tingting Liu 1 , Jing Dai 2 , Zhitao Yang 3 , Xiaoqi Yu 4 , Yanping Xu 5, 6, 7 , Xinming Shi 2 , Dong Wei 4 , Zihan Tang 1 , Guanqun Xu 2 , Wenxin Xu 4 , Yu Liu 2 , Ce Shi 2 , Qi Ni 2 , Chengde Yang 1 , Xinxin Zhang 4 , Xuefeng Wang 2 , Erzhen Chen 3 , Jieming Qu 5, 6, 7
|
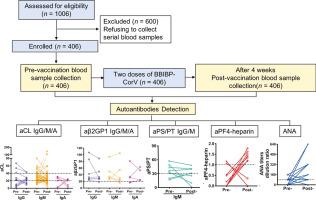
The presence of antiphospholipid antibodies was shown to be associated with thrombosis in coronavirus disease 2019 (COVID-19) patients. Recently, according to reports from several studies, the vaccine-induced immune thrombotic thrombocytopenia is mediated by anti-platelet factor 4 (PF4)-polyanion complex in adenovirus-vectored COVID-19 vaccine recipients. It is impendent to explore whether inactivated COVID-19 vaccine widely used in China influences prothrombotic autoantibody production and induces thrombosis. In this prospective study, we recruited 406 healthcare workers who received two doses, 21 days apart, of inactivated severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) vaccine (BBIBP-CorV, Sinopharm). Paired blood samples taken before vaccination and four weeks after the second vaccination were used in detecting prothrombotic autoantibodies, including anticardiolipin (aCL), anti-β2 glycoprotein I (aβ2GP1), anti-phosphatidylserine/prothrombin (aPS/PT), and anti-PF4-heparin. The seroconversion rate of SARS-CoV-2 specific antibodies was 95.81% (389/406) four weeks after vaccination. None of the subjects had spontaneous thrombosis or thrombocytopenia over a minimum follow-up period of eight weeks. There was no significant difference in the presence of all ten autoantibodies between samples collected before and after vaccination: for aCL, IgG (7 vs. 8, P = 0.76), IgM (41 vs. 44, P = 0.73), IgA (4 vs. 4, P = 1.00); anti-β2GP1, IgG (7 vs. 6, P = 0.78), IgM (6 vs. 5, P = 0.76), IgA (3 vs. 5, P = 0.72); aPS/PT IgG (0 vs. 0, P = 1.00), IgM (6 vs. 5, P = 0.76); aPF4-heparin (2 vs. 7, P = 0.18), and antinuclear antibody (ANA) (18 vs. 21, P = 0.62). Notably, seven cases presented with anti-PF4-heparin antibodies (range: 1.18–1.79 U/mL) after vaccination, and none of them exhibited any sign of thrombotic disorder. In conclusion, inactivated SARS-CoV-2 vaccine does not influence the profile of antiphospholipid antibody and anti-PF4-heparin antibody nor increase the risk of thrombosis.











































 京公网安备 11010802027423号
京公网安备 11010802027423号