Abstract
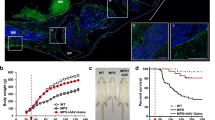
Mucopolysaccharidosis type I (MPS I) is caused by deficiency of alpha-L-iduronidase (IDUA), leading to multisystemic accumulation of glycosaminoglycans (GAG). Untreated MPS I patients may die in the first decades of life, mostly due to cardiovascular and respiratory complications. We previously reported that the treatment of newborn MPS I mice with intravenous administration of lipossomal CRISPR/Cas9 complexes carrying the murine Idua gene aiming at the ROSA26 locus resulted in long-lasting IDUA activity and GAG reduction in various tissues. Following this, the present study reports the effects of gene editing in cardiovascular, respiratory, bone, and neurologic functions in MPS I mice. Bone morphology, specifically the width of zygomatic and femoral bones, showed partial improvement. Although heart valves were still thickened, cardiac mass and aortic elastin breaks were reduced, with normalization of aortic diameter. Pulmonary resistance was normalized, suggesting improvement in respiratory function. In contrast, behavioral abnormalities and neuroinflammation still persisted, suggesting deterioration of the neurological functions. The set of results shows that gene editing performed in newborn animals improved some manifestations of the MPS I disorder in bone, respiratory, and cardiovascular systems. However, further studies will be imperative to find better delivery strategies to reach “hard-to-treat” tissues to ensure better systemic and neurological effects.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout









Similar content being viewed by others
References
Giugliani R, Federhen A, Rojas MVM, Vieira T, Artigalás O, Pinto LL, et al. Mucopolysaccharidosis I, II, and VI: Brief review and guidelines for treatment. Genet Mol Biol. 2010;33:589–604.
Hollak CEM, Wijburg FA. Treatment of lysosomal storage disorders: successes and challenges. J Inherit Metab Dis. 2014;37:587–98.
Patel P, Suzuki Y, Tanaka A, Yabe H, Kato S, Shimada T, et al. Impact of enzyme replacement therapy and hematopoietic stem cell therapy on growth in patients with Hunter syndrome. Mol Genet Metab Rep. 2014;1:184–96.
Muenzer J, Wraith JE, Clarke LA. Mucopolysaccharidosis I: management and treatment guidelines. Pediatrics. 2009;123. https://doi.org/10.1542/peds.2008-0416.
Giugliani R. Mucopolysacccharidoses: from understanding to treatment, a century of discoveries. Genet Mol Biol. 2012;35:924–31.
Hirth A, Berg A, Greve G. Successful treatment of severe heart failure in an infant with Hurler syndrome. J Inherit Metab Dis. 2007;30:820.
Soliman OII, Timmermans RGM, Nemes A, Vletter WB, Wilson JHP, ten Cate FJ, et al. Cardiac abnormalities in adults with the attenuated form of mucopolysaccharidosis type I. J Inherit Metab Dis. 2007;30:750–7.
Chan MO, Sen ES, Hardy E, Hensman P, Wraith E, Jones S, et al. Assessment of musculoskeletal abnormalities in children with mucopolysaccharidoses using pGALS. Pediatr Rheumatol Online J. 2014;12:32.
Chan D, Li A, Yam M, Li C, Fok T. Hurler’s syndrome with cor pulmonale secondary to obstructive sleep apnoea treated by continuous positive airway pressure. J Paediatr Child Health. 2003;39:558–9.
Taylor C, Brady P, O’Meara A, Moore D, Dowling F, Fogarty E. Mobility in Hurler syndrome. J Pediatr Orthop. 2008;28:163–8.
Braunlin EA, Harmatz PR, Scarpa M, Furlanetto B, Kampmann C, Loehr JP, et al. Cardiac disease in patients with mucopolysaccharidosis: presentation, diagnosis and management. J Inherit Metab Dis. 2011;34:1183–97.
Lin S-P, Shih S-C, Chuang C-K, Lee K-S, Chen M-R, Niu D-M, et al. Characterization of pulmonary function impairments in patients with mucopolysaccharidoses-changes with age and treatment. Pediatr Pulmonol. 2014;49:277–84.
Baldo G, Tavares AMV, Gonzalez E, Poletto E, Mayer FQ, Matte U, da S, et al. Progressive heart disease in mucopolysaccharidosis type I mice may be mediated by increased cathepsin B activity. Cardiovasc Pathol. 2017;27:45–50.
Poswar F de O, de Souza CFM, Giugliani R, Baldo G. Aortic root dilatation in patients with mucopolysaccharidoses and the impact of enzyme replacement therapy. Heart Vessels. 2018;34:290–5.
Ohmi K, Greenberg DS, Rajavel KS, Ryazantsev S, Li HH, Neufeld EF. Activated microglia in cortex of mouse models of mucopolysaccharidoses I and IIIB. Proc Natl Acad Sci USA. 2003;100:1902–7.
de Oliveira PG, Baldo G, Mayer FQ, Martinelli B, Meurer L, Giugliani R, et al. Characterization of joint disease in mucopolysaccharidosis type I mice. Int J Exp Pathol. 2013;94:305–11.
Braunlin E, Mackey-Bojack S, Panoskaltsis-Mortari A, Berry J, Mcelmurry R, Riddle M, et al. Cardiac functional and histopathologic findings in humans and mice with mucopolysaccharidosis type I: implications for assessment of therapeutic interventions in Hurler syndrome. Pediatr Res. 2006;59:27–32.
Garcia AR, Pan J, Lamsa JC, Muenzer J. The characterization of a murine model of mucopolysaccharidosis II (Hunter syndrome). J Inherit Metab Dis. 2007;30:924–34.
Baldo G, Mayer FQ, Martinelli B, Dilda A, Meyer F, Ponder KP, et al. Evidence of a progressive motor dysfunction in mucopolysaccharidosis type I mice. Behav Brain Res. 2012;233:169–75.
Schneider AP, Matte U, Pasqualim G, Tavares AMV, Mayer FQ, Martinelli B, et al. Deleterious effects of interruption followed by reintroduction of enzyme replacement therapy on a lysosomal storage disorder. Transl Res. 2016;176:29–37.e1.
Schuh R, Baldo G, Teixeira H. Nanotechnology applied to treatment of mucopolysaccharidoses. Expert Opin Drug Deliv. 2016;13:1709–18.
Schuh RS, Poletto E, Pasqualim G, Tavares AMV, Meyer FS, Gonzalez EA, et al. In vivo genome editing of mucopolysaccharidosis I mice using the CRISPR/Cas9 system. J Control Release. 2018;288:23–33.
Baldo G, Quoos Mayer F, Burin M, Carrillo-Farga J, Matte U, Giugliani R. Recombinant encapsulated cells overexpressing alpha-L-iduronidase correct enzyme deficiency in human mucopolysaccharidosis type I cells. Cells Tissues Organs. 2012;195:323–9.
Kubaski F, Mason RW, Nakatomi A, Shintaku H, Xie L, van Vlies NN, et al. Newborn screening for mucopolysaccharidoses: a pilot study of measurement of glycosaminoglycans by tandem mass spectrometry. J Inherit Metab Dis. 2017;40:151–8.
Baldo G, Mayer FQ, Martinelli BZ, de Carvalho TG, Meyer FS, de Oliveira PG, et al. Enzyme replacement therapy started at birth improves outcome in difficult-to-treat organs in mucopolysaccharidosis I mice. Mol Genet Metab. 2016;109:33–40.
Criée CP, Sorichter S, Smith HJ, Kardos P, Merget R, Heise D, et al. Body plethysmography—Its principles and clinical use. Respir Med. 2011;105:959–71.
Sands MS, Barker JE, Vogler C, Levy B, Gwynn B, Galvin N, et al. Treatment of murine mucopolysaccharidosis type VII by syngeneic bone marrow transplantation in neonates. Lab Investig. 1993;68:676–86.
Baldo G, Lorenzini DM, Santos DS, Mayer FQ, Vitry S, Bigou S, et al. Shotgun proteomics reveals possible mechanisms for cognitive impairment in Mucopolysaccharidosis I mice. Mol Genet Metab. 2015;114:138–45.
Hartung SD, Reddy RG, Whitley CB, McIvor RS. Enzymatic correction and cross-correction of mucopolysaccharidosis type I fibroblasts by adeno-associated virus-mediated transduction of the alpha-L-iduronidase gene. Hum Gene Ther. 1999;10:2163–72.
Kakkis ED, Muenzer J, Tiller GE, Waber L, Belmont J, Passage M, et al. Enzyme-replacement therapy in mucopolysaccharidosis I. N Engl J Med. 2001;344:182–8.
Neufeld ES, Muenzer J. The online metabolic and molecular basis of inherited disease. In: Valle D, Beaudet AL, Vogelstein B, editors. New York: MacGrow Hill; 2007.
Tomatsu S, Fujii T, Fukushi M, Oguma T, Shimada T, Maeda M, et al. Newborn screening and diagnosis of mucopolysaccharidoses. Mol Genet Metab. 2013;110:42–53.
Parini R, Deodato F, Di Rocco M, Lanino E, Locatelli F, Messina C, et al. Open issues in Mucopolysaccharidosis type I-Hurler. Orphanet J Rare Dis. 2017;12:112.
Tomatsu S, Alméciga-Díaz CJ, Montaño AM, Yabe H, Tanaka A, Dung VC, et al. Therapies for the bone in mucopolysaccharidoses. Mol Genet Metab. 2015;114:94–109.
Pievani A, Azario I, Antolini L, Shimada T, Patel P, Remoli C. Neonatal bone marrow transplantation prevents bone pathology in a mouse model of mucopolysaccharidosis type I. Blood. 2015;125:1662–71.
Azario I, Pievani A, Del Priore F, Antolini L, Santi L, Corsi A, et al. Neonatal umbilical cord blood transplantation halts skeletal disease progression in the murine model of MPS-I. Sci Rep. 2017;7:9473.
Rowan DJ, Tomatsu S, Grubb JH, Haupt B, Montaño AM, Oikawa H, et al. Long circulating enzyme replacement therapy rescues bone pathology in mucopolysaccharidosis VII murine model. Mol Genet Metab. 2012;107:161–72.
Hinton RB, Yutzey KE. Heart valve structure and function in development and disease. Annu Rev Physiol. 2011;73:29–46.
Bigg PW, Baldo G, Sleeper MM, O’Donnell PA, Bai H, Rokkam VRP, et al. Pathogenesis of mitral valve disease in mucopolysaccharidosis VII dogs. Mol Genet Metab. 2013;110:319–28.
Poletto E, Pasqualim G, Giugliani R, Matte U & Baldo G. Effects of gene therapy on cardiovascular symptoms of lysosomal storage diseases. Genet Mol Biol. 2019;42:261–85.
Berger KI, Fagondes SC, Giugliani R, Hardy KA, Lee KS, McArdle C, et al. Respiratory and sleep disorders in mucopolysaccharidosis. J Inherit Metab Dis. 2013;36:201–10.
Muhlebach MS, Wooten W, Muenzer J. Respiratory manifestations in mucopolysaccharidoses. Paediatr Respir Rev. 2011;12:133–8.
Ou L, Herzog T, Koniar BL, Gunther R, Whitley CB. High-dose enzyme replacement therapy in murine Hurler syndrome. Mol Genet Metab. 2014;111:116–22.
O’Callaghan JP, Sriram K. Glial fibrillary acidic protein and related glial proteins as biomarkers of neurotoxicity. Expert Opin Drug Saf. 2005;4:433–42.
Siemionow K, Klimczak A, Brzezicki G, Siemionow M, McLain RF. The effects of inflammation on glial fibrillary acidic protein expression in satellite cells of the dorsal root ganglion. Spine. 2009;34:1631–7.
Lund TC. Hematopoietic stem cell transplant for lysosomal storage diseases. Pediatr Endocrinol Rev. 2013;11:91–8. Suppl 1.
Almeciga-Diaz CJ, Montano AM, Barrera LA, Tomatsu S. Tailoring the AAV2 capsid vector for bone-targeting. Pediatr Res. 2018;84:545–51.
Schuh RS, Bidone J, Poletto E, Pinheiro CV, Pasqualim G, de Carvalho TG, et al. Nasal Administration of cationic nanoemulsions as nucleic acids delivery systems aiming at mucopolysaccharidosis type I gene therapy. Pharm Res. 2018;35:221.
Bidone J, Schuh RS, Farinon M, Poletto É, Pasqualim G, de Oliveira PG, et al. Intra-articular nonviral gene therapy in mucopolysaccharidosis I mice. Int J Pharm. 2018;548:151–8.
Acknowledgements
The authors were supported by National Council for Scientific and Technological Development (CNPq) (grant numbers 470888/2014-8 and 141742/2014-3), Coordenação de Aperfeiçoamento de Pessoal de Nível Superior—Brasil (CAPES) (Finance Code 001), Universidade Federal do Rio Grande do Sul, FAPERGS (Grant 02/2017—Programa Pesquisador Gaúcho numbers 17/2551-0001103-1 and 17/2551-0001273-9) and FIPE—Hospital de Clínicas de Porto Alegre, Serviço de Pesquisa Experimental (grant number 2015-0416). RSS would like to thank CNPq for the postdoctoral grant (PDJ grant number 151021/2018-0).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
About this article
Cite this article
Schuh, R.S., Gonzalez, E.A., Tavares, A.M.V. et al. Neonatal nonviral gene editing with the CRISPR/Cas9 system improves some cardiovascular, respiratory, and bone disease features of the mucopolysaccharidosis I phenotype in mice. Gene Ther 27, 74–84 (2020). https://doi.org/10.1038/s41434-019-0113-4
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41434-019-0113-4
This article is cited by
-
Efficient CRISPR/Cas9 nickase-mediated genome editing in an in vitro model of mucopolysaccharidosis IVA
Gene Therapy (2023)
-
Gene Modulation with CRISPR-based Tools in Human iPSC-Cardiomyocytes
Stem Cell Reviews and Reports (2023)
-
Delivery and assessment of a CRISPR/nCas9-based genome editing system on in vitro models of mucopolysaccharidoses IVA assisted by magnetite-based nanoparticles
Scientific Reports (2022)
-
In utero adenine base editing corrects multi-organ pathology in a lethal lysosomal storage disease
Nature Communications (2021)
-
Lysosomal storage diseases: current therapies and future alternatives
Journal of Molecular Medicine (2020)