Abstract
Objective
To compare short-term outcomes of very low birthweight (VBLW, <1500 g) neonates by maternal HIV status.
Design
Retrospective hospital-based cohort in Cape Town, South Africa.
Results
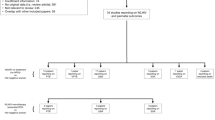
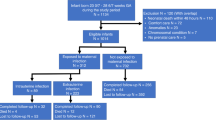
Of 1579 mothers, 316 (20%) were HIV-positive; 183/316 (58%) received ≥8 weeks of antenatal antiretrovirals. HIV-exposed neonates (HIVE, vs HIV-unexposed, HIVU) had increased risk of necrotising enterocolitis (NEC; OR 1.93, 95% CI 1.27–2.92) and invasive ventilation (OR 1.35, 95% CI 1.01–1.79). Extremely low birthweight (ELBW, <1000 g) modified the HIV-exposure-mortality relationship: among ELBW neonates, HIVE vs HIVU mortality OR 1.75 (95% CI 1.13–2.69); among non-ELBW, OR 0.89 (95% CI 0.54–1.49). Antiretrovirals (≥8 vs <8 weeks/none) reduced NEC (OR 0.46, 95% CI 0.22–0.97) and invasive ventilation risks (OR 0.57, 95% CI 0.32–0.99). HIV-PCR results were available for 228/316 (72%) HIVE neonates; 11/228 (5%) tested positive.
Conclusions
Among VLBW neonates, HIV-exposure was associated with increased risk of adverse short-term outcomes; antenatal antiretrovirals were protective.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout

Similar content being viewed by others
Data and coding availability
The datasets and statistical coding generated during the current study are available from the corresponding author on reasonable request.
References
UNAIDS. AIDSinfo. 2018. http://aidsinfo.unaids.org/. Accessed 30 April 2019.
UNAIDS. Women and HIV: a spotlight on adolescent girls and young women. 2019. http://www.unaids.org/en/resources/documents/2019/women-and-hiv. Accessed 30 April 2019.
Evans C, Jones CE, Prendergast AJ. HIV-exposed, uninfected infants: new global challenges in the era of paediatric HIV elimination. Lancet Infect Dis. 2016;16:e92–107.
Brennan AT, Bonawitz R, Gill CJ, Thea D, Kleinman M, Useem J, et al. A meta-analysis assessing all-cause mortality in HIV-exposed uninfected compared to HIV-unexposed uninfected infants and children. AIDS. 2016;30:2351–60.
le Roux SM, Abrams EJ, Donald KA, Brittain K, Phillips TK, Nguyen KK, et al. Growth trajectories of breastfed HIV-exposed uninfected and HIV-unexposed children under conditions of universal maternal antiretroviral therapy: a prospective study. The Lancet Child Adolesc Health. 2019;3:234–44.
le Roux SM, Abrams EJ, Nguyen K, Myer L. Clinical outcomes of HIV-exposed, HIV-uninfected children in sub-Saharan Africa. Trop Med Int Health. 2016;21:829–45.
Slogrove AL, Esser MM, Cotton MF, Speert DP, Kollmann TR, Singer J, et al. A prospective cohort study of common childhood infections in South African HIV-exposed uninfected and HIV-unexposed Infants. Pediatr Infect Dis J. 2017;36:e38–44.
Powis KM, Smeaton L, Hughes MD, Tumbare EA, Souda S, Jao J, et al. In-utero triple antiretroviral exposure associated with decreased growth among HIV-exposed uninfected infants in Botswana. AIDS. 2016;30:211–20.
Zash RM, Souda S, Leidner J, Binda K, Hick C, Powis K, et al. High proportion of deaths attributable to hiv among postpartum women in botswana despite widespread uptake of antiretroviral therapy. AIDS Patient Care STDs. 2017;31:14–9.
Goetghebuer T, Rowland-Jones SL, Kollmann TR. Editorial: immune mechanisms underlying the increased morbidity and mortality of HIV-Exposed Uninfected (HEU) children. Front Immunol. 2017;8:1060.
Uthman OA, Nachega JB, Anderson J, Kanters S, Mills EJ, Renaud F, et al. Timing of initiation of antiretroviral therapy and adverse pregnancy outcomes: a systematic review and meta-analysis. Lancet HIV. 2017;4:e21–30.
Wedi CO, Kirtley S, Hopewell S, Corrigan R, Kennedy SH, Hemelaar J. Perinatal outcomes associated with maternal HIV infection: a systematic review and meta-analysis. Lancet HIV. 2016;3:e33–48.
Katz J, Lee ACC, Kozuki N, Lawn JE, Cousens S, Blencowe H, et al. Mortality risk in preterm and small-for-gestational-age infants in low-income and middle-income countries: a pooled country analysis. Lancet. 2013;382:417–25.
Desfrere L, de Oliveira I, Goffinet F, El Ayoubi M, Firtion G, Bavoux F, et al. Increased incidence of necrotizing enterocolitis in premature infants born to HIV-positive mothers. AIDS. 2005;19:1487–93.
Ballot DE, Davies VA, Cooper PA, Chirwa T, Argent A, Mer M. Retrospective cross-sectional review of survival rates in critically ill children admitted to a combined paediatric/neonatal intensive care unit in Johannesburg, South Africa, 2013–2015. BMJ Open. 2016;6:e010850.
Tiam M, Velaphi S. Maternal human immunodeficiency virus status and morbidity and mortality in very low birthweight infants. Paediatr Int Child Health. 2017;37:14–20.
Chokoe MJ, Wright CA, Bezuidenhout J, Moore SW, Smith J. Necrotizing enterocolitis in HIV-exposed and nonexposed infants: clinical presentation and histopathological features. Pediatr Dev Pathol. 2012;15:293–7.
Strydom K, Nel DG, Dhansay MA, Van Niekerk E. The effect of maternal HIV status and treatment duration on body composition of HIV-exposed and HIV-unexposed preterm, very and extremely low-birthweight infants. Paediatr Int Child Health. 2018;38:163–74.
Vermont Oxford Network. Manuals and Forms. 2017. https://vtoxford.zendesk.com/hc/en-us/categories/360000861394-Manuals-and-Forms. Accessed 19 May 2019.
Goga AE, Dinh TH, Jackson DJ, Lombard CJ, Puren A, Sherman G, et al. Population-level effectiveness of PMTCT Option A on early mother-to-child (MTCT) transmission of HIV in South Africa: implications for eliminating MTCT. J Glob Health. 2016;6:020405.
The South African Antiretroviral Treatment Guidelines. South African Department of Health. 2013. http://www.sahivsoc.org/upload/documents/2013%20ART%20Guidelines-Short%20Combined%20FINAL%20draft%20guidelines%2014%20March%202013.pdf. Accessed 14 Sep 2015.
PAWC. PMTCT Clinical Guidelines Update, 2013. https://www.westerncape.gov.za/assets/departments/health/wcp_2013_pmtct_clinical_guidelines_update_final_replacement_2.pdf. Accessed 6 Oct 2016.
WHO. Consolidated guidelines on the use of antiretroviral drugs for treating and preventing HIV infection. Recommendations for a public health approach. Second edition. 2016. http://apps.who.int/iris/bitstream/10665/246200/1/9789241511124-eng.pdf. Accessed 28 July 2016.
Levin C, Le Roux DM, Harrison MC, Tooke L. HIV transmission to premature very low birth weight infants. Pediatr Infect Dis J. 2017;36:860–2.
Horbar JD. The Vermont Oxford Network: evidence-based quality improvement for neonatology. Pediatrics. 1999;103(1 Suppl E):350–9.
Arikawa S, Rollins N, Jourdain G, Humphrey J, Kourtis AP, Hoffman I, et al. Contribution of maternal antiretroviral therapy and breastfeeding to 24-month survival in human immunodeficiency virus-exposed uninfected children: an individual pooled analysis of African and Asian studies. Clin Infect Dis. 2018;66:1668–77.
Lilian RR, Kalk E, Technau KG, Sherman GG. Birth diagnosis of HIV infection in infants to reduce infant mortality and monitor for elimination of mother-to-child transmission. Pediatr Infect Dis J. 2013;32:1080–5.
Van Niekerk E, Autran CA, Nel DG, Kirsten GF, Blaauw R, Bode L. Human milk oligosaccharides differ between HIV-infected and HIV-uninfected mothers and are related to necrotizing enterocolitis incidence in their preterm very-low-birth-weight infants. J Nutr. 2014;144:1227–33.
Karpelowsky JS, van Mil S, Numanoglu A, Leva E, Millar AJW. Effect of maternal human immunodeficiency virus status on the outcome of neonates with necrotizing enterocolitis. J Pediatr Surg. 2010;45:315–8.
Nino DF, Sodhi CP, Hackam DJ. Necrotizing enterocolitis: new insights into pathogenesis and mechanisms. Nat Rev Gastroenterol Hepatol. 2016;13:590–600.
Slogrove AL, Frigati L, Gray DM. Maternal HIV and paediatric lung health. Paediatr Respir Rev. 2017;21:47–53.
UNAIDS. Global AIDS Update 2018. Miles to go: closing gaps, breaking barriers, righting injustices. http://www.unaids.org/sites/default/files/media_asset/miles-to-go_en.pdf. Accessed 23 Nov 2018.
Acknowledgements
We are grateful to the Paediatric Management Group, Life Health care for sponsorship of data collection, and to the Vermont Oxford Network for waiving annual membership fees.
Author information
Authors and Affiliations
Contributions
LR prepared this article and conducted this study in fulfilment of the requirements of an MMed in Paediatrics. She was included in the conceptualisation and design of the study and supervised while conducting the background literature review, data capturing, preliminary analysis and early drafts. SLR conducted final data analysis and interpretation. LT acted as the primary supervisor with additional input from MH. LT and MH conceptualised this study and have been involved in critical reviewing of the data capture, analysis, interpretation and final editing. All authors contributed to and approved the final manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
About this article
Cite this article
Riemer, L.J., Le Roux, S.M., Harrison, M.C. et al. Short-term outcomes of HIV-exposed and HIV-unexposed preterm, very low birthweight neonates: a longitudinal, hospital-based study. J Perinatol 40, 445–455 (2020). https://doi.org/10.1038/s41372-019-0541-4
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41372-019-0541-4