Abstract
Introduction
Shiga toxin 2a (Stx2a) induces hemolytic uremic syndrome (STEC HUS) by targeting glomerular endothelial cells (GEC).
Objectives
We investigated in a metabolomic analysis the response of a conditionally immortalized, stable glomerular endothelial cell line (ciGEnC) to Stx2a stimulation as a cell culture model for STEC HUS.
Methods
CiGEnC were treated with tumor necrosis factor-(TNF)α, Stx2a or sequentially with TNFα and Stx2a. We performed a metabolomic high-throughput screening by lipid- or gas chromatography and subsequent mass spectrometry. Metabolite fold changes in stimulated ciGEnC compared to untreated cells were calculated.
Results
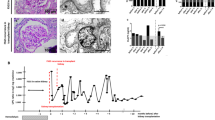
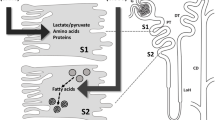
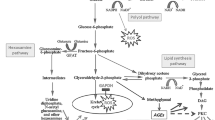
320 metabolites were identified and investigated. In response to TNFα + Stx2a, there was a predominant increase in intracellular free fatty acids and amino acids. Furthermore, lipid- and protein derived pro-inflammatory mediators, oxidative stress and an augmented intracellular energy turnover were increased in ciGEnC. Levels of most biochemicals related to carbohydrate metabolism remained unchanged.
Conclusion
Stimulation of ciGEnC with TNFα + Stx2a is associated with profound metabolic changes indicative of increased inflammation, oxidative stress and energy turnover.




Similar content being viewed by others
Data availability
All data generated or analysed during this study are included in this published article and its supplementary information files. Further, a list of all analyzed metabolites by name, superordinate metabolite group, biochemical sub-pathway and fold change of the respective intracellular concentration is uploaded as Supplementary Table 1 in the online supplements and is available via figshare.com (https://doi.org/10.6084/m9.figshare.7749521). Original mass spectral data are also uploaded on figshare.com and can be found via this link: https://doi.org/10.6084/m9.figshare.9817115.
References
Bauwens, A., Bielaszewska, M., Kemper, B., Langehanenberg, P., Von Bally, G., Reichelt, R., et al. (2011). Differential cytotoxic actions of Shiga toxin 1 and Shiga toxin 2 on microvascular and macrovascular endothelial cells. Thrombosis and Haemostasis, 105(3), 515–528.
Betzen, C., Plotnicki, K., Fathalizadeh, F., Pappan, K., Fleming, T., Bielaszewska, M., et al. (2016). Shiga Toxin 2a—Induced endothelial injury in hemolytic uremic syndrome: A metabolomic analysis. Journal of Infectious Diseases, 213(6), 1031–1040.
Chan, Y. S., & Ng, T. B. (2016). Shiga toxins: From structure and mechanism to applications. Applied Microbiology and Biotechnology, 100(4), 1597–1610.
Dehaven, C. D., Evans, A. M., Dai, H., & Lawton, K. A. (2010). Organization of GC/MS and LC/MS metabolomics data into chemical libraries. Journal of Cheminformatics, 2(1), 9.
Ergonul, Z., Hughes, A. K., & Kohan, D. E. (2003). Induction of apoptosis of human brain microvascular endothelial cells by Shiga Toxin 1. The Journal of Infectious Diseases, 187(1), 154–158.
Evans, A. M., DeHaven, C. D., Barrett, T., Mitchell, M., & Milgram, E. (2009). Integrated, nontargeted ultrahigh performance liquid chromatography/electrospray ionization tandem mass spectrometry platform for the identification and relative quantification of the small-molecule complement of biological systems. Analytical Chemistry, 81(16), 6656–6667.
Fakhouri, F., Zuber, J., Frémeaux-Bacchi, V., & Loirat, C. (2017). Haemolytic uraemic syndrome. The Lancet, 390(10095), 681–696.
Ferraris, V., Acquier, A., Ferraris, J. R., Vallejo, G., Paz, C., & Mendez, C. F. (2011). Oxidative stress status during the acute phase of haemolytic uraemic syndrome. Nephrology, dialysis, transplantation: Official publication of the European Dialysis and Transplant Association—European Renal Association, 26(3), 858–864.
Gomez, S. A., Abrey-Recalde, M. J., Panek, C. A., Ferrarotti, N. F., Repetto, M. G., Mejías, M. P., et al. (2013). The oxidative stress induced in vivo by Shiga toxin-2 contributes to the pathogenicity of haemolytic uraemic syndrome. Clinical and Experimental Immunology, 173(3), 463–472.
Gvozdjáková, A. (2008). Carnitine. Mitochondrial medicine: Mitochondrial metabolism, diseases, diagnosis and therapy, 5(3), 357–366.
Hughes, A. K., Stricklett, P. K., Schmid, D., & Kohan, D. E. (2000). Cytotoxic effect of Shiga toxin-1 on human glomerular epithelial cells. Kidney International, 57(6), 2350–2359.
Johannes, L., & Römer, W. (2010). Shiga toxins—from cell biology to biomedical applications. Nature Reviews Microbiology, 8(2), 105–116.
Kaur, J., & Debnath, J. (2015). Autophagy at the crossroads of catabolism and anabolism. Nature Reviews Molecular Cell Biology, 16(8), 461–472.
Komatsu, M., Waguri, S., Ueno, T., Iwata, J., Murata, S., Tanida, I., et al. (2005). Impairment of starvation-induced and constitutive autophagy in Atg7-deficient mice. Journal of Cell Biology, 169(3), 425–434.
Lee, M. S., Cherla, R. P., Jenson, M. H., Leyva-Illades, D., Martinez-Moczygemba, M., & Tesh, V. L. (2011). Shiga toxins induce autophagy leading to differential signalling pathways in toxin-sensitive and toxin-resistant human cells. Cellular Microbiology, 13(10), 1479–1496.
Meisen, I., Rosenbrück, R., Galla, H. J., Hüwel, S., Kouzel, I. U., Mormann, M., et al. (2013). Expression of Shiga toxin 2e glycosphingolipid receptors of primary porcine brain endothelial cells and toxin-mediated breakdown of the blood-brain barrier. Glycobiology, 23(6), 745–759.
Melton-Celsa, A. R. (2014). Shiga toxin (Stx) classification, structure, and function. Microbiology Spectrum, 2(3), 1–21.
Mizushima, N., & Klionsky, D. J. (2007). Protein turnover via autophagy: Implications for metabolism. Annual Review of Nutrition, 27, 19–40.
Nakatogawa, H., Suzuki, K., Kamada, Y., & Ohsumi, Y. (2009). Dynamics and diversity in autophagy mechanisms: Lessons from yeast. Nature Reviews Molecular Cell Biology, 10(7), 458–467.
Nieman, D. C., Shanely, R. A., Gillitt, N. D., Pappan, K. L., & Lila, M. A. (2013). Serum metabolic signatures induced by a three-day intensified exercise period persist after 14 h of recovery in runners. Journal of Proteome Research, 12(10), 4577–4584.
Noris, M., & Remuzzi, G. (2005). Hemolytic uremic syndrome. Journal of the American Society of Nephrology, 16(4), 1035–1050.
Obrig, T. G., Louise, C. B., Lingwood, C. A., Boyd, B., Barley-Maloney, L., & Daniel, T. O. (1993). Endothelial heterogeneity in Shiga toxin receptors and responses. Journal of Biological Chemistry, 268(21), 15484–15488.
Obrig, T. G., Seaner, R. M., Bentz, M., Lingwood, C. A., Boyd, B., Smith, A., et al. (2003). Induction by sphingomyelinase of Shiga toxin receptor and Shiga toxin 2 sensitivity in human microvascular endothelial cells. Infection and Immunity, 71(2), 845–849.
Potter, B. J., Sorrentino, D., & Berk, P. D. (1989). Mechanisms of cellular uptake of free fatty acids. Annual Review of Nutrition, 9(1), 253–270.
Satchell, S. C., Tasman, C. H., Singh, A., Ni, L., Geelen, J., Von Ruhland, C. J., et al. (2006). Conditionally immortalized human glomerular endothelial cells expressing fenestrations in response to VEGF. Kidney International, 69(9), 1633–1640.
Schmid, D. I., & Kohan, D. E. (2001). Effect of shigatoxin-1 on arachidonic acid release by human glomerular epithelial cells. Kidney International, 60(3), 1026–1036.
Singh, R., Kaushik, S., Wang, Y., Xiang, Y., Novak, I., Komatsu, M., et al. (2009). Autophagy regulates lipid metabolism. Nature, 458(7242), 1131–1135.
Tang, B., Li, Q., Zhao, X., Wang, H., Li, N., Fang, Y., et al. (2015). Shiga toxins induce autophagic cell death in intestinal epithelial cells via the endoplasmic reticulum stress pathway. Autophagy, 11(2), 344–354.
Tesh, V. L. (2012). Activation of cell stress response pathways by Shiga toxins. Cellular Microbiology, 14(1), 1–9.
Zou, M.-H. (2015). Tryptophan-kynurenine pathway is dysregulated in inflammation and immune activation. Frontiers in Bioscience, 20(7), 4363.
Acknowledgements
We thank Prof. Peter Nawroth for kindly providing the laboratory facilities and Dr. Thomas Fleming for his valuable input and methodical assistance.
Funding
This work was supported by a Physician Scientist fellowship grant from the Medical Faculty of the University of Heidelberg to C.P., C.B. and N.R.
Author information
Authors and Affiliations
Contributions
CP designed and performed research, analyzed and interpreted the data and wrote the first draft of the paper; KLP, CB and APO performed research, analyzed and interpreted the data; KLP, SCS, PWM, MB, HK and BT designed research, analyzed and interpreted the data, NR directed, designed, analyzed and interpreted the data and wrote the paper.
Corresponding author
Ethics declarations
Conflict of interest
KL.P. is an employee of Metabolon, Inc. and, as such, has affiliations with or financial involvement with Metabolon, Inc. The authors have no other relevant affiliations or financial involvement with any organization or entity with a financial interest in or financial conflict with the subject matter or materials discussed in the manuscript apart from those disclosed. Besides that, there are no other financial or non-financial conflicts of interest.
Research involving human and/or animal participants
This article does not contain any studies with human and/or animal participants performed by any of the authors.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Patry, C., Plotnicki, K., Betzen, C. et al. Metabolomic analysis of Shiga toxin 2a-induced injury in conditionally immortalized glomerular endothelial cells. Metabolomics 15, 131 (2019). https://doi.org/10.1007/s11306-019-1594-2
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s11306-019-1594-2