Abstract
Purpose
Cancer-inflammation prognostic index (CIPI) is calculated by multiplying the concentration of carcinoembryonic antigen by neutrophil-to-lymphocyte ratio. CIPI has been reported as a prognostic factor for colorectal cancer. Although carcinoembryonic antigen and neutrophil-to-lymphocyte ratio have been reported as prognostic factors for non-small cell lung cancer (NSCLC), it has not been investigated whether CIPI is a useful marker.
Methods
We analyzed the prognostic factors, including CIPI, in 700 NSCLC patients treated by pulmonary resection. We also analyzed a subgroup of 482 patients with pathological stage I NSCLC.
Result
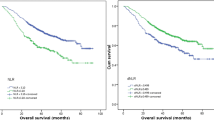
CIPI > 14.59 (P < 0.01), maximum standardized uptake value (SUVmax) > 5.35 (P < 0.01), lymphatic invasion (P = 0.01), and pathological stage (P < 0.01) were significant factors for relapse-free survival (RFS) in multivariate analysis. SUVmax > 5.35 (P < 0.01) and pathological stage (P < 0.01) were revealed as significant factors for overall survival in the multivariate analysis. In the subanalysis, CIPI > 14.88 (P = 0.01) and SUVmax > 5.07 (P < 0.01) were significant factors for RFS of pathological stage I NSCLC in multivariate analysis.
Conclusion
CIPI was a significant factor for RFS in NSCLC patients treated surgically, even in those with pathological stage I disease. SUVmax was also a significant factor for RFS and overall survival in NSCLC patients treated surgically, and for RFS in patients with pathological stage I NSCLC.
Trial Registration
The Institutional Review Board of Kanazawa Medical University approved the protocol of this retrospective study (Approval Number: I392), and written informed consent was obtained from all patients.


Similar content being viewed by others
Data Availability
The datasets generated and/or analyzed during the current study are not publicly available due to [our institutional restrictions e.g., them containing information that could compromise research participant privacy/consent], but are available from the corresponding author on reasonable request.
References
Siegel RL, Miller KD, Wagle NS, Jemal A (2023) Cancer statistics, 2023. CA Cancer J Clin 73:17–48
Zahorec R (2001) Ratio of neutrophil to lymphocyte counts—rapid and simple parameter of systemic inflammation and stress in critically ill. Bratisl Lek Listy 102:5–14
Tomita M, Shimizu T, Ayabe T, Yonei A, Onitsuka T (2011) Preoperative neutrophil to lymphocyte ratio as a prognostic predictor after curative resection for non-small cell lung cancer. Anticancer Res 31:2995–2998
Forget P, Machiels JP, Coulie PG, Berliere M, Poncelet AJ, Tombal B et al (2013) Neutrophil:lymphocyte ratio and intraoperative use of ketorolac or diclofenac are prognostic factors in different cohorts of patients undergoing breast, lung, and kidney cancer surgery. Ann Surg Oncol 3:650–660
Shimizu K, Okita R, Saisho S, Maeda A, Nojima Y, Nakata M (2015) Preoperative neutrophil/lymphocyte ratio and prognostic nutritional index predict survival in patients with non-small cell lung cancer. World J Surg Oncol 13:291
Motono N, Mizoguchi T, Ishikawa M, Iwai S, Iijima Y, Hidetaka U (2022) Prognostic value of neutrophil-to-lymphocyte ratio and prognostic nutrition index in patients with non-small cell lung cancer receiving pulmonary resection. World J Surg Res 5:1401
Su YL, Tsai KL, Chiu TJ, Lin YM, Lee KC, Lu CC et al (2021) Development and validation of a novel serum prognostic marker for patients with metastatic colorectal cancer on regorafenib treatment. Cancers 13:5080
You JF, Hsu YJ, Chern YJ, Cheng CC, Jong BK, Liao CK et al (2022) Preoperative cancer inflammation prognostic index as a superior predictor of short- and long-term outcomes in patients with stage I-III colorectal cancer after curative surgery. Cancers 14:6232
Grunnet M, Sorensen JB (2012) Carcinoembryonic antigen (CEA) as tumor marker in lung cancer. Lung Cancer 76:138–143
Brinkman GL, Coates EO (1963) The effect of bronchitis, smoking, and occupation on ventilation. Am Rev Respir Dis 87:684–693
Li D, Yuan X, Liu J, Li C, Li W (2018) Prognostic value of prognostic nutritional index in lung cancer: a meta-analysis. J Thorac Dis 10:5298–5307
Qiu C, Qu X, Shen X, Zheng C, Zhu L, Meng L et al (2015) Evaluation of prognostic nutritional index in patients undergoing radical surgery with nonsmall cell lung cancer. Nutr Cancer 67:741–747
Kim YS, Kim SJ, Kim TK, Kim IJ, Kim YD, Lee MK (2011) Prediction of survival and cancer recurrence using F-18 FDG PET/CT in patients with surgically resected early stage (Stage I and II) non-small cell lung cancer. Neoplasma 58:245–250
Nitadori J, Bograd AJ, Morales EA, Rizk NP, Dunphy MPS, Sima CS et al (2013) Preoperative consolidation-to-tumor ratio and SUVmax stratify the risk of recurrence in patients undergoing limited resection for lung adenocarcinoma ≤2cm. Ann Surg Oncol 20:4282–4288
Motono N, Ueno M, Tanaka M, Machida Y, Usuda K, Sakuma T et al (2014) Differences in the prognostic significance of the SUVmax between patients with resected pulmonary adenocarcinoma and squamous cell carcinoma. Asian Pac J Cancer Prev 15:10171–10174
Felip E, Altorki N, Zhou C, Csőszi T, Vynnychenko I, Goloborodko O et al (2021) Adjuvant atezolizumab after adjuvant chemotherapy in resected stage IB–IIIA non-small-cell lung cancer (IMpower010): a randomised, multicentre, open-label, phase 3 trial. Lancet 398:1344–1357
Wu YL, John T, Grohe C, Majem M, Goldman JW, Kim SW et al (2021) Postoperative chemotherapy use and outcomes from ADAURA: osimertinib as adjuvant therapy for resected EGFR-mutated NSCLC. J Thorac Oncol 17:423–433
Kato H, Ichinose Y, Ohta M, Hata E, Tsubota N, Tada H et al (2004) A randomized trial of adjuvant chemotherapy with uracil-tagafur for adenocarcinoma for the lung. N Engl J Med 350:1713–1721
Tsutani Y, Imai K, Ito H, Miyata Y, Ikeda N, Nakayama H et al (2022) Adjuvant chemotherapy for high-risk pathologic stage I non-small cell lung cancer. Ann Thorac Surg 113:1608–2161
Rizzo A, Cantale O, Mogavero A, Garetto L, Racca M, Venesio T et al (2023) Assessing the role of colonic and other anatomical sites uptake by [18F]FDG-PET/CT and immune-inflammatory peripheral blood indexes in patients with advanced non-small cell lung cancer treated with first-line immune checkpoint inhibitors. Thorac Cancer 14:2473–2483
Cvetkovic L, Régis C, Richard C, Derosa L, Leblond A, Malo J et al (2021) Physiologic colonic uptake of 18F-FDG on PET/CT is associated with clinical response and gut microbiome composition in patients with advanced non-small cell lung cancer treated with immune checkpoint inhibitors. Eur J Nucl Med Mol Imaging 48:1550–1559
Acknowledgements
We thank Cathel Kerr, BSc, PhD, from Edanz (https://jp.edanz.com/ac) for editing a draft of this manuscript.
Funding
This study has not been funded.
Author information
Authors and Affiliations
Contributions
NM performed the research, collected and analyzed the data and wrote the paper. TM, MI, SI, and YI contributed to sample collection. HU contributed to supervision of this study and revision of the manuscript. All authors have read and approved the manuscript, and ensure that this is the case.
Corresponding author
Ethics declarations
Competing interests
The authors declare that they have no competing interests.
Ethical Approval and Consent to Participate
The present study was conducted in accordance with the amended Declaration of Helsinki. The Institutional Review Boards of Kanazawa Medical University approved the protocol (approval number: I392), and written informed consent was obtained from all of the patients.
Consent to Publish
Not applicable.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Motono, N., Mizoguchi, T., Ishikawa, M. et al. Prognostic Impact of Cancer Inflammation Prognostic Index for Non-small Cell Lung Cancer. Lung 201, 603–610 (2023). https://doi.org/10.1007/s00408-023-00649-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00408-023-00649-z