Abstract
Aims/hypothesis
Islets have complex heterogeneity and subpopulations. Cell surface markers representing alpha, beta and delta cell subpopulations are urgently needed for investigations to explore the compositional changes of each subpopulation in obesity progress and diabetes onset, and the adaptation mechanism of islet metabolism induced by a high-fat diet (HFD).
Methods
Single-cell RNA sequencing (scRNA-seq) was applied to identify alpha, beta and delta cell subpopulation markers in an HFD-induced mouse model of glucose intolerance. Flow cytometry and immunostaining were used to sort and assess the proportion of each subpopulation. Single-cell proteomics was performed on sorted cells, and the functional status of each alpha, beta and delta cell subpopulation in glucose intolerance was deeply elucidated based on protein expression.
Results
A total of 33,999 cells were analysed by scRNA-seq and clustered into eight populations, including alpha, beta and delta cells. For alpha cells, scRNA-seq revealed that the Ace2low subpopulation had downregulated expression of genes related to alpha cell function and upregulated expression of genes associated with beta cell characteristics in comparison with the Ace2high subpopulation. The impaired function and increased fragility of ACE2low alpha cells exposure to HFD was further suggested by single-cell proteomics. As for beta cells, the CD81high subpopulation may indicate an immature signature of beta cells compared with the CD81low subpopulation, which had robust function. We also found differential expression of Slc2a2 in delta cells and a potentially stronger cellular function and metabolism in GLUT2low delta cells than GLUT2high delta cells. Moreover, an increased proportion of ACE2low alpha cells and CD81low beta cells, with a constant proportion of GLUT2low delta cells, were observed in HFD-induced glucose intolerance.
Conclusions/interpretation
We identified ACE2, CD81 and GLUT2 as surface markers to distinguish, respectively, alpha, beta and delta cell subpopulations with heterogeneous maturation and function. The changes in the proportion and functional status of islet endocrine subpopulations reflect the metabolic adaptation of islets to high-fat stress, which weakened the function of alpha cells and enhanced the function of beta and delta cells to bring about glycaemic homeostasis. Our findings provide a fundamental resource for exploring the mechanisms maintaining each islet endocrine subpopulation’s fate and function in health and disease.
Data availability
The scRNA-seq analysis datasets from the current study are available in the Gene Expression Omnibus (GEO) repository under the accession number GSE203376.
Graphical abstract

Similar content being viewed by others

Introduction
Pancreatic islets, containing various endocrine cells such as alpha, beta, delta, pancreatic polypeptide (PP) and epsilon cells, are responsible for nutrient utilisation and energy metabolism [1]. As insulin is the main regulator of blood glucose, most studies of islet dysfunction have been limited to beta cells. However, increasing evidence has emphasised the synergistic interaction of alpha, beta and delta cells in glucose homeostasis [2,3,4]. In type 2 diabetes, several studies indicate that progressive dysfunction of alpha, beta and delta cells occurs in the early stages. The metabolic load from obesity and hyperlipidaemia causes insulin resistance and higher insulin demand, which stimulates beta cell compensatory proliferation [5]. A combination of an increased proportion of alpha cells migrating towards the islet centre and inappropriately increased pulsatile glucagon secretion is another signature of type 2 diabetes [6, 7]. Furthermore, significantly decreased delta cell numbers preceding the gradual decline in beta cell numbers was observed in people with diabetes [8, 9]. The above studies indicate that the dynamic balance of each islet subpopulation is disrupted across the disease course. The prevalence of glucose intolerance in Chinese adults was 35.2% in a study based on 2018 data [10]. High energy intake characterised by high fat intake leads to insulin resistance, beta cell dysfunction and type 2 diabetes [11,12,13]. However, the changes to islet cell subsets in high-fat-induced glucose intolerance remain unclear.
Single-cell RNA sequencing (scRNA-seq) has emerged as a powerful approach to explore intercellular heterogeneity, cell–cell interactions and the unique function of individual cells in the context of the cellular microenvironment [14, 15]. Recent studies have reported the heterogeneity and diverse function of beta cells using scRNA-seq. For instance, a novel beta cell subpopulation with stem cell properties and immature characteristics could defend itself against attack from immune cells, surviving type 1 diabetes progression for a long time [16]. Human beta cells exist in three different states according to the activation of unfolded protein response (UPR) and insulin gene expression. Proliferating human beta cells were characterised by low insulin gene expression and high UPR activation [17]. Wang et al also found that the proportions of three beta cell subpopulations in type 2 diabetes varied with age and BMI [18]. In summary, functionally distinct beta cell subsets act independently or collaboratively to satisfy dynamic insulin requirements.
Although the introduction of scRNA-seq has achieved promising findings, these results are restricted to the transcriptome level. A comprehensive protein expression profile is essential in the field of islet cell subpopulations. However, traditional proteomics of islet cell subsets is challenged by low yields of FACS-sorted cell subpopulations due to limited islet cells in mouse pancreas. Thus, there is a great demand for the single-cell proteomics, which can sense and quantify more than 1000 proteins in a single mammalian cell [19]. The single-cell protein profile of circulating human CD34+ cells obtained from an efficient and straightforward mass-adaptive coating-assisted single-cell proteomics (Mad-CASP) revolutionises our knowledge of different CD34+ cell subsets [20]. Yet, single-cell proteomics studies of islet cell subpopulations are still lacking. Moreover, as previous studies mainly focused on beta cells, the heterogeneity of alpha and delta cells is not clear at present. Recent studies have shown diverse electrophysiological response of alpha cells to glucose, suggesting the existence of different alpha cell subsets [21].
In the present study, to comprehensively evaluate the adaptive changes and compensatory mechanisms, we performed scRNA-seq and single-cell proteomics to identify alpha, beta and delta cell subpopulations in a high-fat diet (HFD)-induced mouse model of glucose intolerance and provided a theoretical basis for the precise treatment and prevention of type 2 diabetes.
Methods
Mice and treatment
Four-week-old male C57BL/6J mice (GemPharmatech, China) were bred at specific-pathogen-free conditions under a 12 h/12 h light/dark cycle and randomised into groups with free access to the chow diet (CD; 13.5% fat; 5001; LabDiet, USA) or HFD (60% fat; D12492; Research Diets, USA) for 8 weeks. Bodyweight was monitored every week. Blinding was not carried out in this study. All experimental animal procedures were approved by The Medicine Animal Care Committee of Nanjing Medical University (IACUC1804001).
Glucose and insulin tolerance tests
After 8 weeks’ feeding, mice were subjected to IPGTT and ITT as described in the electronic supplementary material (ESM) Methods.
Isolation of primary islets
Human islets and pancreatic sections were provided from Tianjin First Central Hospital, China (see ESM Methods and Human Islets Checklist). All human studies were conducted according to the principles of the Declaration of Helsinki and approved by the Research Ethics Committee of Nanjing Medical University. Mouse islets were isolated as described in the ESM Methods.
Immunofluorescence staining
Immunofluorescence was performed on the paraffin-embedded pancreas sections. Pancreases were fixed, processed, stained and quantified as previously reported [22]. See ESM Methods for further details.
FACS of islet cells
FACS was used to obtain alpha, beta and delta cell subgroups. Dispersed mouse or human islets were sorted and analysed as described in the ESM Methods. Antibodies are shown in ESM Table 1.
Single-cell library preparation, RNA sequencing and dataset analysis
Islet cells from the HFD- and CD-fed mice were dispersed as single cells and scRNA-seq was performed. The reads were processed as described previously [23]. See ESM Methods for further details.
Identification of cell types and alpha, beta and delta cell subpopulations and differentially expressed gene analysis
The data were scaled and principal component analysis (PCA) was based on the top 2000 highly variable, differentially expressed genes (DEGs), as described in the ESM Methods.
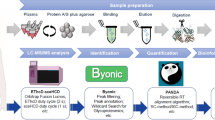
Sample preparation for single-cell proteomics of islet cells
Single-cell proteomics samples were prepared based on mass-adaptive coating of synthetic peptides as previously reported [20]. See ESM Methods for further details.
LC-MS/MS parameters
The peptide samples were subjected to LC-MS/MS using a Fusio Lumo Tribrid mass spectrometer (Thermo Scientific, USA) as previously reported [20]. See ESM Methods for further details.
Single-cell proteomics data analysis
The raw data were processed by MaxQuant (version 1.5.3.0) and fold-changes of differentially expressed proteins (DEPs) were assessed using Welch’s t tests. Single-cell proteomics samples with less than 5000 identified peptides were excluded from data analysis. See ESM Methods for further details.
Quantitative PCR
Sorted primary islet cells were lysed in TRIzol Reagent (Invitrogen, catalogue no. 15596026, USA). RNA and protein were isolated according to the manufacturers’ instructions. Quantitative PCR (qPCR) was performed as described in the ESM Methods. The primers are presented in ESM Table 2.
Western blotting
Proteins from sorted primary islet cells were isolated using TRIzol Reagent. Western blots were performed as described in the ESM Methods.
Statistical analysis
FACS data were analysed using FlowJo software (version 10.0.7, BD Biosciences, USA). Comparisons of data between two groups were carried out using two-tailed t tests. The data are presented as mean ± SD. A p value<0.05 was considered statistically significant.
Results
ScRNA-seq of mouse islet cells
An 8 week HFD induced obvious obesity, impaired glucose homeostasis, and induced insulin resistance in C57BL/6J mice (ESM Fig. 1a). Consistent with our previous research [24], HFD resulted in a compensatory hyperplasia in islet mass, especially regarding beta cells (ESM Fig. 1b). High-throughput scRNA-seq profiled an estimated 15093 cells from islets from CD-fed mice and 18906 from islets from HFD-fed mice and clustered into four principal endocrine cells, annotated based on predominant hormone gene expression: 4069 alpha (Gcg), 14,108 beta (Ins1), 1698 delta (Sst) and 666 PP (Ppy) cells. In addition, small numbers of endothelial, immune, mesenchymal and ductal cells were identified based on previously reported marker genes (Fig. 1a–d).
Identification of islet cell types. (a) UMAP visualisation (in two dimensions [UMAP_1 and UMAP_2]) of 15,093 islet cells from 5 CD-fed mice and 18,906 islet cells from 5 HFD-fed mice (different colours mark distinct cell types annotated based on the expression of signature genes; each dot represents one cell). (b) Distribution of each cell subpopulation in CD and HFD groups. (c, d) UMAP visualisation (c) and violin plots (d) of the expression of marker genes in islet cell types (depth of purple in c indicates expression level). (e–g) Top 20 enriched KEGG pathways of DEGs in (e) alpha, (f) beta and (g) delta cells between HFD and CD groups. TPM, transcripts per million; UMAP, uniform manifold approximation and projection
Based on the DEGs in alpha, beta and delta cells in the HFD group compared with the CD group (ESM Fig. 1c–e, ESM Table 3), protein processing in the endoplasmic reticulum was significantly enriched in alpha, beta and delta cells (Fig. 1e–g). Inflammation-related pathways (such as Th17 cell differentiation and IL-17 [25] and the NOD-like receptor signalling pathways [26]) were particularly enriched in alpha cells (Fig. 1e), suggesting the importance of inflammation responses to HFD-induced metabolic stress. In beta cells, calcium transport and ion channel regulation pathways (including arrhythmogenic right ventricular cardiomyopathy, hypertrophic cardiomyopathy, dilated cardiomyopathy, and the cGMP–PKG signalling pathway) were top-ranked (Fig. 1f), indicating the relevance of secretory function. Additionally, in both beta and delta cells, oxidative respiratory chain and energy production and metabolism pathways were highly significantly enriched. In delta cells, other notable pathways that were markedly influenced by HFD were protein degradation and recycling-related pathways (Fig. 1g).
Ace2 low alpha cells may represent immature alpha cells with beta cell-like characteristics
To analyse the heterogeneity of alpha cells, alpha cells were clustered into eight clusters using scRNA-seq data (Fig. 2a,b). To characterise them, we analysed the marker gene expression in the eight clusters (Fig. 2c). Interestingly, we found that Ace2, a pivotal gene associated with severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) infection, varied noticeably among the alpha cell clusters. According to the expression level of Ace2, we divided the eight alpha cell clusters into Ace2low (clusters 3 and 5) and Ace2high (clusters 0, 1, 2, 4, 6, and 7) subpopulations (Fig. 2d,e). ScRNA-seq and immunofluorescence confirmed the existence of alpha cell subgroups in both CD and HFD mouse islets (Fig. 2f,g,j). Heterogeneous expression of ACE2 also exists but ACE2 was only expressed in a small number of human alpha cells in both healthy and type 2 diabetic individuals (ESM Fig. 2).
Heterogeneous expression of Ace2 in alpha cells. (a, b) UMAP visualisation of alpha cell subpopulations (a) and violin plot of Ace2 expression distribution in these subpopulations (b). (c) Heatmap of cell marker expression in alpha cell subpopulations. (d, e) UMAP visualisation of Ace2high and Ace2low alpha cell subpopulations (d) and violin plot of Ace2 expression distribution in these subpopulations (e). (f, g) UMAP visualisation of alpha cells in the CD and HFD groups (f) and violin plot of Ace2 expression distribution in Ace2high and Ace2low alpha cell subpopulations in the CD and HFD groups (g). (h) Heatmap of differential gene expression between Ace2low and Ace2high groups. (i) Enriched KEGG pathways of DEGs in (h). (j) Glucagon (green) and ACE2 (red) co-staining of pancreatic sections (white arrows indicate ACE2low alpha cells, yellow arrows indicate ACE2high alpha cells) (scale bar, 20 μm). (k) Representative western blot of ACE2 and the beta cell function-related proteins UCN3 and GLUT2 from sorted ACE2high and ACE2low alpha cells. (l) Violin plots of key genes associated with alpha cell maturation and function: Mafb, Irx1, Fev, Ttr, Chgb and Pyy were upregulated in the Ace2high group, while Ucn3, Ero1lb and Slc2a2 were upregulated in the Ace2low group. (m–q) qPCR analysis of Ace2, alpha cell identity-related gene Mafb, and beta cell identity-related genes Mafa, Ucn3 and Ero1lb in sorted ACE2high and ACE2low alpha (α) cells isolated from C57BL/6J mice (per RNA sample from n=10 mice, ≥5 replicates). *p<0.05; **p<0.01; ***p<0.001; Student’s t test). TPM, transcripts per million; UMAP, uniform manifold approximation and projection
To explore the molecular features of Ace2-based alpha cell heterogeneity, we identified 379 DEGs between the Ace2low and Ace2high subpopulations (Fig. 2h, ESM Table 4). Kyoto Encyclopedia of Genes and Genomes (KEGG) analysis revealed that the DEGs between the Ace2low and Ace2high subpopulations were preferentially enriched in oxidative phosphorylation, metabolic pathways, alpha cell secretory function-related pathways (including cGMP–PKG, glucagon, calcium and cAMP signalling pathways) and programmed cell death and proliferation pathways (including ferroptosis, oocyte meiosis, mammalian target of rapamycin [mTOR] signalling, Rap1 signalling and phosphoinositide 3-kinase [PI3K]–Akt signalling) (Fig. 2i, ESM Table 4), indicating that Ace2 expression could distinguish between alpha cells with different functional and survival status. We also found that alpha cell-specific transcription factors (Mafb and Irx1) and alpha cell-related genes (Ttr, Chgb, Fev and Pyy) were significantly downregulated in the Ace2low group. Instead, Ace2low alpha cells started to express genes with beta cell characteristics (such as Ucn3, Ero1lb [also known as Ero1b], and Slc2a2) (Fig. 2l). Some of the results were confirmed by qPCR (Fig. 2m–q) and western blotting (Fig. 2k) on the sorted alpha cell populations. It suggested that the Ace2low subpopulation may represents immature alpha cells that appear to have beta cell-like characteristics.
Single-cell proteomics analysis of islet cell subpopulations
As mRNA expression does not fully reflect the biological activity of cells or organs, we performed single-cell proteomics analyses of islet cell subpopulations (ESM Fig. 3a). A total of 6955 proteins and 50245 peptides were identified in 36 islet cell subpopulation samples. The CVs of peptides and proteins within the groups were small and stable, and the correlation coefficients between replicates were all >0.7, indicating the excellent quality of the single-cell proteomics data (ESM Fig. 3b–d). A detailed heatmap and enriched KEGG pathways of DEPs for each cell subpopulation are shown in ESM Fig. 3e, f and ESM Tables 5 and 6.
ACE2low alpha cells may represent a state of low-capacity and fragility and susceptibility to HFD stress
FACS of islet single-cell suspensions was used to divide alpha (glucagon [GCG]+) cells into ACE2high and ACE2low groups. Notably, the proportion of ACE2high alpha cells was significantly lower in HFD mice (65.3%) than CD mice (80.0%) (Fig. 3a,b), indicating that ACE2-based alpha cell heterogeneity may be involved in the pathophysiology of diabetes. FACS-sorted ACE2low and ACE2high alpha cell subpopulations from CD and HFD mice (2000 cells per sample) were collected for single-cell proteomics analysis. The number of proteins detected varied from 3042 to 4021 and with good reproducibility (ESM Fig. 4a). PCA could also clearly differentiate ACE2low and ACE2high cells (Fig. 3c).
Single-cell proteomics indicating alpha cell subpopulation function. (a) Representative dot plots of the flow cytometry gating strategies for alpha cells, with respective (FMO) control. GCG+ alpha cells were sorted into ACE2low and ACE2high subpopulations. Representative distributions of ACE2 expression in CD and HFD groups are shown on the right. (b) Proportions of ACE2low and ACE2high alpha cell subpopulations in CD and HFD groups (n≥8 mice per group). Student’s t test: *p<0.05. (c) PCA plots of ACE2low and ACE2high single-cell proteomics samples (n=10 CD and 10 HFD mice per pair of ACE2low and ACE2high alpha cell single-cell proteomics samples, 3 replicates). (d, f) Volcano plots of DEPs between ACE2low and ACE2high subpopulations in (d) CD and (f) HFD groups. (e, g) Enriched KEGG pathways of DEPs between ACE2low and ACE2high subpopulations in (e) CD and (g) HFD groups. The top x-axis refers to the DEP number and the bottom x-axis refers to the p value. FMO, fluorescence minus one; GCG, glucagon; PC, principal component
In CD mice, there were 29 up- and 80 downregulated DEPs in ACE2low compared with ACE2high alpha cells (Fig. 3d, ESM Table 7). The KEGG pathways affected included the Ras signalling pathway and the mitogen-activated protein kinase (MAPK) signalling pathway (Fig. 3e, ESM Table 7). In HFD mice, there was a clear increase in DEPs in ACE2low compared with ACE2high alpha cells, with 17 up- and 301 downregulated DEPs (Fig. 3f). Pathways associated with nutrient and energy metabolism (including metabolic pathways, carbon metabolism, glycolysis/gluconeogenesis, pentose phosphate pathway, biosynthesis of amino acids, fructose and mannose metabolism, glutathione metabolism, starch and sucrose metabolism, and galactose metabolism) and protein degradation and recycling pathways (including endocytosis, protein processing in endoplasmic reticulum, proteasome, and lysosome pathways) were all markedly downregulated in the ACE2low group (Fig. 3g). Furthermore, cell proliferation and survival pathways (including Rap1, oocyte meiosis, neurotrophin and Hippo signalling pathway) were also downregulated. These findings strongly hinted that the metabolic and other biological activities of ACE2low alpha cells were diminished, especially in HFD mice.
Further, we analysed the DEPs and enriched KEGG pathways between the HFD and CD groups in both ACE2low and ACE2high alpha cells. There were more downregulated DEPs in ACE2low alpha cells than ACE2high alpha cells, and these downregulated DEPs were enriched in more metabolism-related pathways (ESM Fig. 4b–e, ESM Table 7). This suggested that ACE2low alpha cells are more susceptible to HFD stress and could be a group of low-capacity and fragile alpha cells, while ACE2high alpha cells may represent the main functional cell population in mice, and they could better withstand HFD stress.
Cd81 high beta cells may represent immature beta cells with weak function
To analyse the heterogeneity of beta cells, we clustered the beta cells into nine clusters and identified the top ten marker genes (Fig. 4a–c). We found that Cd81 was differentially expressed in beta cell clusters, in line with a recent study [27]. We divided the nine beta cell clusters into Cd81low (clusters 0–4 and 7) and Cd81high (clusters 5, 6 and 8) subpopulations (Fig. 4d–g). Immunostaining also confirmed the obvious heterogeneity of CD81 distribution in beta cells from both CD and HFD mice (Fig. 4j), which was verified in human islets (ESM Fig. 5). What’s more, the proportion of CD81high cells was elevated in the type 2 diabetes group (ESM Fig. 5).
Heterogeneous expression of CD81 on beta cells. (a, b) UMAP visualisation of beta cell subpopulations (a) and violin plot of Cd81 expression distribution in these subpopulations (b). (c) Heatmap of cell marker expression in beta cell subpopulations. (d, e) UMAP visualisation of Cd81high and Cd81low beta cell subpopulations (d) and violin plot of Cd81 expression distribution in these subpopulations (e). (f, g) UMAP visualisation of beta cells in the CD and HFD groups (f) and violin plot of Cd81 expression distribution in Cd81high and Cd81low beta cell subpopulations in the CD and HFD groups (g). (h) Heatmap of differential gene expression between Cd81low and Cd81high groups. (i) Enriched KEGG pathways of DEGs between Cd81low and Cd81high groups. (j) Insulin (green) and CD81 (red) co-staining of pancreatic sections (white arrows indicate CD81low beta cells, yellow arrows indicate CD81high beta cells) (scale bar, 40 μm). (k) Representative western blot of CD81 and the beta cell-related protein GLUT2 from sorted CD81low and CD81high beta cells isolated from CD and HFD C57BL/6J mice. (l) Violin plots of key genes associated with beta cell maturation and function; Mafa, Ucn3, Slc2a2, G6pc2, Sytl4, and Ero1lb were upregulated in the Cd81low group, and Mafb, Rbp4, Chga and Chgb were upregulated in the Cd81high group. (m–p) qPCR analysis of Cd81, the alpha cell identity-related gene Mafb, and beta cell identity-related genes Mafa and Ucn3 in sorted CD81low and CD81high beta (β) cells isolated from CD and HFD C57BL/6J mice (per pair of RNA samples from n=5 mice, ≥5 replicates, *p<0.05; ***p<0.001; Student’s t test). TPM, transcripts per million; UMAP, uniform manifold approximation and projection
According to the DEGs and enriched KEGG pathways in the Cd81low subpopulation relative to the Cd81high subpopulation (Fig. 4h,i, ESM Table 4), cellular metabolism and related functional pathways along with a series of stress-related and inflammatory pathways were significantly enriched. The key beta cell transcription factor Mafa and beta cell maturation markers (Ucn3, Slc2a2, G6pc2, Sytl4, and Ero1lb) had high mRNA expression in the Cd81low subpopulation, whereas immature beta cell markers (Chga, Chgb, Mafb, and Rbp4) were highly expressed in the Cd81high subpopulation (Fig. 4l), suggesting that the Cd81high subpopulation may represent a group of weakly functioning and immature beta cells. Some of the results were confirmed by qPCR (Fig. 4m–p) and western blotting (Fig. 4k) on the sorted beta cell subpopulations.
To further explore the effects of HFD on beta cell subpopulations, FACS showed that the proportion of CD81high beta cells decreased in HFD mice compared with CD mice (Fig. 5a,b). Then, FACS-sorted CD81low and CD81high beta cells were analysed using single-cell proteomics (10,000 cells per sample). The number of proteins detected varied from 3435 to 4946 and with good reproducibility (ESM Fig. 6a). PCA showed that CD81low and CD81high beta cells clustered into two separate groups (Fig. 5c).
Single-cell proteomics identification of beta cell subpopulation functions. (a) Representative dot plots of the flow cytometry gating strategies for beta cells, with respective FMO control. INS+ beta cells were sorted into CD81low and CD81high subpopulations. Representative CD81 expression distributions in CD and HFD groups are shown on the right. (b) Proportions of CD81low and CD81high beta cell subpopulations in CD and HFD groups (n≥8 mice per group). Student’s t test: *p<0.05. (c) PCA plots of CD81low and CD81high single-cell proteomics samples (per pair of CD81low and CD81high beta cell single-cell proteomics sample from n=5 CD or 5 HFD mice, 3 replicates). (d, e) Volcano plots of DEPs between CD81low and CD81high subpopulations in the (d) CD and (e) HFD groups. (f, g) Enriched KEGG pathways of DEPs between CD81low and CD81high subpopulations in the (f) CD and (g) HFD groups. The top x-axis refers to DEP number and the bottom x-axis refers to p value. (h) CD81 (green), PDX1 (red) and insulin (white) co-staining of pancreatic sections (white arrows indicate CD81low PDX1high beta cells, yellow arrows indicate CD81high PDX1low beta cells) (scale bar, 20 μm). (i) Representative western blot of PDX1 from sorted CD81high and CD81low beta cells isolated from CD and HFD C57BL/6J mice was shown on the right. FMO, fluorescence minus one; INS, insulin; PC, principal component
Comparing CD81low with CD81high beta cells, 869 up- and 373 downregulated DEPs were detected in CD mice, and 707 up- and 312 downregulated DEPs were detected in HFD mice (Fig. 5d,e, ESM Table 8). In both CD and HFD mice, pathways associated with energy metabolism (including oxidative phosphorylation and Alzheimer’s disease) were downregulated in the CD81low subpopulation (Fig. 5f,g). The downregulated DEPs involved in these pathways were also decreased in scRNA-seq between HFD and CD beta cells (ESM Table 3). The results reflect the consistency of the transcriptome and proteome, confirming the reliability of our single-cell RNA-seq and proteomics. Furthermore, in both CD and HFD mice, pancreatic and duodenal homeobox 1 (PDX1), a key transcription factor associated with beta cell maturation and functional maintenance, was significantly upregulated in CD81low cells relative to CD81high cells (ESM Table 8), the expression was further validated by immunofluorescence (Fig. 5h) and western blot analyses (Fig. 5i). Additionally, DEPs enriched in endocytosis, phagosomes, proteasomes and synaptic vesicle cycling pathways were mostly upregulated in CD81low beta cells (Fig. 5f,g), suggesting a more mature status of CD81low beta cells.
Notably, there were 324 DEPs between the HFD and CD mice in CD81low cells and 202 DEPs between the HFD and CD mice in CD81high cells (ESM Fig. 6b, d, ESM Table 8), which is much fewer than the DEPs between the CD81low and CD81high cell subpopulations (1242 DEPs in CD mice, and 1019 in HFD mice). However, the enriched pathways all seem to have no obvious relationships with beta cell maturation or functional status in either CD81low or CD81high cells (ESM Fig. 6c, e). This suggests that the effect of HFD on CD81-divided beta cell subpopulations is to change the subpopulation proportion rather than a direct effect on the subpopulation function.
HFD enhanced the function of mature GLUT2low delta cells
Although Slc2a2 (encoding GLUT2) is a beta cell signature gene, we still found a small group of delta cells with relatively high expression of Slc2a2 in scRNA-seq. Therefore, we divided the delta cells into Slc2a2low and Slc2a2high subpopulations (ESM Fig. 7a, b). According to the DEGs and enriched pathways in the Slc2a2low vs Slc2a2high subpopulations (ESM Fig. 7c, d), upregulated pathways were related to calcium ion and hormone secretion, suggesting that the Slc2a2low subgroup may be more functionally mature. However, the 8 week HFD did not alter the proportions of the two delta cell subpopulations (Fig. 6a,c). Immunofluorescence confirmed the existence of delta cell subgroups in both mouse and human islets (Fig. 6b and ESM Fig. 8).
Single-cell proteomics identification of delta cell subpopulation functions. (a) Representative dot plots of the flow cytometry gating strategies for delta cells, with respective FMO control. SST+ delta cells were sorted into GLUT2low and GLUT2high subpopulations. Representative GLUT2 expression distributions in CD and HFD groups are shown on the right. (b) Somatostatin (green) and GLUT2 (red) co-staining of pancreatic sections (white arrows indicate GLUT2low delta cells, yellow arrows indicate GLUT2high delta cells) (scale bar, 20 μm). (c) Proportions of GLUT2low and GLUT2high delta cell subpopulations in CD and HFD groups (n≥6 mice per group). (d) PCA plots of GLUT2low and GLUT2high single-cell proteomics samples. (e, f) Volcano plots of DEPs in GLUT2low relative to GLUT2high cells in (e) CD and (f) HFD groups (per pair of GLUT2low and GLUT2high delta cell single-cell proteomics samples from n=10 CD and 10 HFD mice, 3 replicates). (g, h) Enriched KEGG pathways in (g) CD and (h) HFD groups. The top x-axis refers to DEP number and the bottom x-axis refers to p value. FMO, fluorescence minus one; PC, principal component; SST, somatostatin
FACS-sorted GLUT2low and GLUT2high delta cell subpopulations from CD and HFD mice (3000 cells per sample) were used for single-cell proteomics analysis, with high reproducibility among the three replicates in each group (ESM Fig. 7e). PCA data showed that GLUT2low and GLUT2high samples clustered into two distinct populations (Fig. 6d).
In the CD mice, there were 548 up- and 171 downregulated DEPs between the GLUT2low and GLUT2high subpopulations; meanwhile, there were more upregulated (832) and fewer downregulated (102) DEPs in the HFD mice (Fig. 6e,f, ESM Table 9). KEGG analysis revealed that similar to beta cells, oxidative phosphorylation and Alzheimer’s disease pathways were significantly downregulated in the GLUT2low cells (relative to the GLUT2high cells) in the CD mice (Fig. 6g). Multiple nutrient metabolic pathways were also significantly upregulated in the GLUT2low cells in both CD and HFD mice (Fig. 6g,h). The same was true for endocytosis and protein processing in the endoplasmic reticulum-related pathways, indicating a more active metabolism in the GLUT2low subpopulation.
The number of DEPs between HFD and CD mice in GLUT2low (117) and GLUT2high (177) subpopulations was much lower than between GLUT2low and GLUT2high subpopulations in HFD (934) and CD (719) mice (ESM Fig. 7f, g, ESM Table 9). In GLUT2low delta cells, comparing HFD and CD mice, upregulated pathways such as AMPK, cGMP–PKG and mTOR signalling pathways dominated. In addition, the calcium signalling pathway, pancreatic secretion, and insulin and glucagon signalling pathways were significantly upregulated (ESM Fig. 7h), indicating that HFD promoted energy metabolism in GLUT2low delta cells. Meanwhile, some metabolic synthesis pathways were downregulated in GLUT2high delta cells (HFD vs CD) (ESM Fig. 7i). In conclusion, GLUT2low delta cells may be more functional and metabolically active than GLUT2high delta cells, and HFD further stimulates GLUT2low delta cell function and metabolism.
Discussion
The development of scRNA-seq technology and the discovery of new cell markers deepened the understanding of beta cell heterogeneity in health and disease [28, 29]. However, no surface markers have been reported to distinguish mature alpha cells. Therefore, the identification of the surface marker ACE2 is meaningful because this protein not only marks immature alpha cells but can also be used to isolate living alpha cell subtypes. Furthermore, ACE2 is widely expressed in several organs, but its expression in pancreatic islets is controversial [30,31,32,33]. We found differential distribution of ACE2 in human and mouse islets. In mouse islets, ACE2 is highly expressed in alpha cells but less in beta cells and exocrine cells, whereas in human islets, it is predominantly expressed in the core of the islet, with only a few positive alpha cells.
A recent study found that alpha cell dysfunction in type 2 diabetes is associated with a ‘beta cell-like’ electrophysiological signature, which was linked to cell maturation state and impaired alpha cell identity [34]. We found some hints of this in our own data: immature alpha cells may be functionally impaired and have beta cell characteristics. Based on this, ACE2 likely marks mature alpha cells as its reduced expression levels are associated with decreased alpha cell function maintenance-related genes and increased beta cell maturation-related genes [35,36,37]. Consistent with Xuan et al, who showed that beta cell dedifferentiation occurred in response to metabolic stress and was accompanied by ACE2 reduction [38], we also found an increased proportion of the ACE2low subpopulation after HFD.
We found that ACE2low alpha cells have significantly reduced metabolism and other biological activity and are less able to resist HFD stress, that is, they may be low-capacity and fragile alpha cells. In contrast, ACE2high alpha cells may be the major functional cell population in mice and are more able to withstand HFD stress. The increase in the proportion of the ACE2low subpopulation after an 8 week HFD suggests that HFD decreases alpha cell function, which corresponds to the scRNA-seq result that HFD alpha cells are enriched in inflammation-related pathways. We speculated that the phenomenon might be due to the elevated insulin demand caused by insulin resistance in obesity, as alpha cells achieve glucose homeostasis by reducing glucagon secretion.
As for beta cell subpopulation markers, there are similarities as well as differences between our results and those of Salinno et al. The analogous conclusion is that CD81 marks immature beta cells in both Salinno et al [27] and our study. This also shows the reliability of the method and the stability of the CD81 marker. The difference in our study is that we used a high-fat mouse model, which is closer to the natural history of glucose intolerance, and found a decreased proportion of CD81high cells after 8 weeks of HFD feeding. Salinno et al [27] found an elevated proportion of CD81high cells in the islets of streptozotocin (STZ)-treated mice and db/db mice. We hypothesise that the HFD-induced glucose-intolerant islets were in a compensatory proliferative state and required more mature CD81low beta cells to meet the body’s insulin requirements. Recent research has also found that CD81 deficiency leads to obesity, insulin resistance and adipose tissue inflammation [39]. Nevertheless, the STZ and db/db mouse models simulate severe hyperglycaemia in diabetes in which islet function fails to compensate, so the proportion of the immature CD81high cells increases, which could also explain the increased proportion of CD81high cells that we observed in islets from donors with type 2 diabetes.
Our study is unique in that we found that most of the metabolic and exocytosis pathways related to beta cell maturation [40] were upregulated in CD81low beta cells, with some difference in DEPs (such as PDX1 [41]), through single-cell proteomics, findings which are not replicated in scRNA-seq. Since the protein is the executor of biological function, these could suggest that CD81low beta cells are functionally mature. We also found that the effect of HFD on CD81-divided beta cell subpopulations is to change the subpopulation proportion rather than directly affecting subpopulation function, explaining the influence of metabolic stress on beta cell subsets.
GLUT2 mediates glucose and fructose transport and is one of the beta cell glucose-sensing mechanisms [42, 43]. We found that GLUT2low delta cells are the main delta cells found in islets that have improved function and are more metabolically active than GLUT2high delta cells. HFD further stimulates GLUT2low delta cell function and metabolism. This is consistent with the basal hypersecretion of somatostatin in HFD-fed mouse islets in our previous experiments [24]. In GLUT2high cells, according to single-cell proteomics, insulin/INS2 expression was upregulated, accompanied by downregulated nutrient metabolic pathways, which may be indicative of immature delta cells with partial beta cell characteristics. Since HFD did not alter the delta cell subpopulation ratio, the effect of HFD on delta cells mainly involved enhancing the function of the major GLUT2low subpopulation.
Several limitations of our study should be recognised. Although the subpopulation markers we identified are all membrane proteins, permeabilisation is still required to stain islet hormones, and functional validation of live islet subpopulations is still needed. Moreover, although we demonstrated the existence of subpopulations in human islets, it will be interesting to explore whether they are involved in the progression of type 2 diabetes, as well as the functional consistency between human and murine islets.
In conclusion, we found that immature islet cells partly lost their identity maintenance genes and began to show the characteristics of other endocrine cells. In HFD-induced glucose intolerance, the proportion of low-capacity and immature ACE2low alpha cells increased with the increasing ratio of functionally active and mature CD81low beta cells. The mature GLUT2low delta cells were functionally enhanced but in constant proportions. These dynamic changes reveal the metabolic plasticity of pancreatic islets in response to HFD stress. This plastic adaptation can counteract metabolic stress and restore glucose homeostasis by inhibiting the hyperglycaemic effect of alpha cells, enhancing the hypoglycaemic effect of beta cells, and increasing the regulation of alpha and beta cells by delta cells (Fig. 7). Therefore, targeting the above markers to change the distribution of islet subpopulations in order to strengthen islet function may be a useful approach to treating diabetes.
Islet cell (alpha, beta and delta) subpopulations in mice with HFD-induced islet dysfunction. In HFD-induced glucose intolerance, the proportion of low-capacity and immature ACE2low alpha cells increased at the same time as the ratio of functionally active and mature CD81low beta cells increased. The mature GLUT2low delta cells were functionally enhanced but in constant proportions. These dynamic changes reveal the metabolic plasticity of pancreatic islets in response to HFD stress. This plastic adaptation can counteract metabolic stress and restore glucose homeostasis by inhibiting the hyperglycaemic effect of alpha cells, enhancing the hypoglycaemic effect of beta cells, and increasing the regulation of alpha and beta cells by delta cells. The figure was created with BioRender.com
Data availability
The scRNA-seq analysis datasets during the current study are available in the Gene Expression Omnibus (GEO) repository under the accession number GSE203376 (www.ncbi.nlm.nih.gov/geo/query/acc.cgi?acc=GSE203376). Other datasets are available from the corresponding authors upon reasonable request.
Abbreviations
- CD:
-
Chow diet
- DEG:
-
Differentially expressed gene
- DEP:
-
Differentially expressed protein
- HFD:
-
High-fat diet
- KEGG:
-
Kyoto Encyclopedia of Genes and Genomes
- mTOR:
-
Mammalian target of rapamycin
- PCA:
-
Principal component analysis
- PDX1:
-
Pancreatic and duodenal homeobox 1
- PP:
-
Pancreatic polypeptide
- qPCR:
-
Quantitative PCR
- scRNA-seq:
-
Single-cell RNA sequencing
- UPR:
-
Unfolded protein response
References
Mastracci TL, Sussel L (2012) The endocrine pancreas: insights into development, differentiation, and diabetes. Wiley Interdiscip Rev Dev Biol 1(5):609–628. https://doi.org/10.1002/wdev.44
Molina J, Rodriguez-Diaz R, Fachado A, Jacques-Silva MC, Berggren PO, Caicedo A (2014) Control of insulin secretion by cholinergic signaling in the human pancreatic islet. Diabetes 63(8):2714–2726. https://doi.org/10.2337/db13-1371
Meulen T, Donaldson CJ, Cáceres E et al (2015) Urocortin3 mediates somatostatin-dependent negative feedback control of insulin secretion. Nat Med 21(7):769–776. https://doi.org/10.1038/nm.3872
Briant LJB, Reinbothe TM, Spiliotis I, Miranda C, Rodriguez B, Rorsman P (2018) δ-cells and β-cells are electrically coupled and regulate α-cell activity via somatostatin. J Physiol 596(2):197–215. https://doi.org/10.1113/JP274581
Hudish LI, Reusch J, Sussel L (2019) β Cell dysfunction during progression of metabolic syndrome to type 2 diabetes. J Clin Investig 129(10):4001–4008. https://doi.org/10.1172/JCI129188
Mitrakou A, Kelley D (1992) Role of reduced suppression of glucose production and diminished early insulin release in. N Engl J Med 326(1):22–22. https://doi.org/10.1056/NEJM199201023260104
Zhang X, Wang Z, Huang Y, Wang J (2015) Effects of chronic administration of alogliptin on the development of diabetes and β-cell function in high fat diet/streptozotocin diabetic mice. Diabetes Obes Metab 13(4):337–347. https://doi.org/10.1111/j.1463-1326.2010.01354.x
Mendoza RG, Perego C, Finzi G et al (2015) Delta cell death in the islet of Langerhans and the progression from normal glucose tolerance to type 2 diabetes in non-human primates (baboon, Papio hamadryas). Diabetologia 58(8):1814–1826. https://doi.org/10.1007/s00125-015-3625-5
Stone VM, Dhayal S, Brocklehurst KJ et al (2014) GPR120 (FFAR4) is preferentially expressed in pancreatic delta cells and regulates somatostatin secretion from murine islets of Langerhans. Diabetologia 57(6):1182–1191. https://doi.org/10.1007/s00125-014-3213-0
Li Y, Teng D, Shi X et al (2020) Prevalence of diabetes recorded in mainland China using 2018 diagnostic criteria from the American Diabetes Association: national cross sectional study. BMJ 369:m997. https://doi.org/10.1136/bmj.m997
Wang L, Zhou B, Zhao Z et al (2021) Body-mass index and obesity in urban and rural China: findings from consecutive nationally representative surveys during 2004–18. Lancet 398(10294):53–63. https://doi.org/10.1016/S0140-6736(21)00798-4
Pan XF, Wang L, Pan A (2021) Epidemiology and determinants of obesity in China. Lancet Diabetes Endocrinol 9(6):373–392. https://doi.org/10.1016/S2213-8587(21)00045-0
Caleyachetty R, Barber TM, Nuredin IM et al (2021) Ethnicity-specific BMI cutoffs for obesity based on type 2 diabetes risk in England: a population-based cohort study. Lancet Diabetes Endocrinol 9(7):419–426. https://doi.org/10.1016/S2213-8587(21)00088-7
Eldar A, Elowitz MB (2010) Functional roles for noise in genetic circuits. Nature 467(7312):167–173. https://doi.org/10.1038/nature09326
Huang S (2009) Non-genetic heterogeneity of cells in development: more than just noise. Development 136(23):3853–3862. https://doi.org/10.1242/dev.035139
Rui J, Deng S, Arazi A, Perdigoto AL, Liu Z, Herold KC (2017) β Cells that resist immunological attack develop during progression of autoimmune diabetes in NOD mice. Cell Metab 25(3):727–738. https://doi.org/10.1016/j.cmet.2017.01.005
Xin Y, Dominguez Gutierrez G, Okamoto H et al (2018) Pseudotime ordering of single human β-cells reveals states of insulin production and unfolded protein response. Diabetes 67(9):1783–1794. https://doi.org/10.2337/db18-0365
Wang Y, Golson M, Schug J et al (2016) Single-cell mass cytometry analysis of the human endocrine pancreas. Cell Metab 24(4):616–626. https://doi.org/10.1016/j.cmet.2016.09.007
Kelly RT (2020) Single-cell proteomics: progress and prospects. Mol Cell Proteomics 19(11):1739–1748. https://doi.org/10.1074/mcp.R120.002234
Li S, Su K, Zhuang Z et al (2022) A simple, rapid, and practical method for single-cell proteomics based on mass-adaptive coating of synthetic peptides. Sci Bull 67:581–584. https://doi.org/10.1016/j.scib.2021.12.022
Montefusco F, Cortese G, Pedersen MG (2020) Heterogeneous alpha-cell population modeling of glucose-induced inhibition of electrical activity. J Theor Biol 485:110036. https://doi.org/10.1016/j.jtbi.2019.110036
Jiang H, Li Y, Shen M et al (2022) Interferon-α promotes MHC I antigen presentation of islet β cells through STAT1-IRF7 pathway in type 1 diabetes. Immunology 166(2):210–221. https://doi.org/10.1111/imm.13468
Zakharov PN, Hu H, Wan X, Unanue ER (2020) Single-cell RNA sequencing of murine islets shows high cellular complexity at all stages of autoimmune diabetes. J Exp Med 217(6):e20192362. https://doi.org/10.1084/jem.20192362
Gao R, Fu Q, Jiang HM et al (2021) Temporal metabolic and transcriptomic characteristics crossing islets and liver reveal dynamic pathophysiology in diet-induced diabetes. iScience 24(4):102265. https://doi.org/10.1016/j.isci.2021.102265
Chehimi M, Vidal H, Eljaafari A (2017) Pathogenic role of IL-17-producing immune cells in obesity, and related inflammatory diseases. J Clin Med 6(7):68. https://doi.org/10.3390/jcm6070068
Platnich JM, Muruve DA (2019) NOD-like receptors and inflammasomes: A review of their canonical and non-canonical signaling pathways. Arch Biochem Biophys 670:4–14. https://doi.org/10.1016/j.abb.2019.02.008
Salinno C, Büttner M, Cota P, Tritschler S, Lickert H (2021) CD81 marks immature and dedifferentiated pancreatic β-cells. Mol Metab 49:101188. https://doi.org/10.1016/j.molmet.2021.101188
Avrahami D, Klochendler A, Dor Y, Glaser B (2017) Beta cell heterogeneity: an evolving concept. Diabetologia 60(8):1363–1369. https://doi.org/10.1007/s00125-017-4326-z
Yu XX, Xu CR (2020) Understanding generation and regeneration of pancreatic β cells from a single-cell perspective. Development 147(7):dev179051. https://doi.org/10.1242/dev.179051
Steenblock C, Richter S, Berger I, Barovic M, Bornstein SR (2021) Viral infiltration of pancreatic islets in patients with COVID-19. Nat Commun 12(1):3534. https://doi.org/10.1038/s41467-021-23886-3
Coate KC, Cha J, Shrestha S et al (2020) SARS-CoV-2 cell entry factors ACE2 and TMPRSS2 are expressed in the microvasculature and ducts of human pancreas but are not enriched in β cells. Cell Metab 32(6):1028–1040. https://doi.org/10.1016/j.cmet.2020.11.006
Fignani D, Licata G, Brusco N et al (2020) SARS-CoV-2 receptor angiotensin I-converting enzyme type 2 (ACE2) is expressed in human pancreatic β-cells and in the human pancreas microvasculature. Front Endocrinol 11:596898. https://doi.org/10.3389/fendo.2020.596898
Kusmartseva I, Wu W, Syed F, Heide V, Atkinson MA (2020) Expression of SARS-CoV-2 entry factors in the pancreas of normal organ donors and individuals with COVID-19. Cell Metab 32(6):P1041–P1051. https://doi.org/10.1016/j.cmet.2020.11.005
Dai XQ, Camunas-Soler J, Briant LJB et al (2022) Heterogenous impairment of α cell function in type 2 diabetes is linked to cell maturation state. Cell Metab 34(2):256–268.e5. https://doi.org/10.1016/j.cmet.2021.12.021
Artner I, Lay JL, Hang Y et al (2006) MafB: an activator of the glucagon gene expressed in developing islet alpha- and beta-cells. Diabetes 55(2):297–304. https://doi.org/10.2337/diabetes.55.02.06.db05-0946
Nishimura W, Kondo T, Salameh T et al (2006) A switch from MafB to MafA expression accompanies differentiation to pancreatic beta-cells. Dev Biol 293(2):526–539. https://doi.org/10.1016/j.ydbio.2006.02.028
Qiu WL, Zhang YW, Feng Y, Li LC, Yang L, Xu CR (2017) Deciphering pancreatic islet β cell and α cell maturation pathways and characteristic features at the single-cell level. Cell Metab 25(5):1194–1205.e4. https://doi.org/10.1016/j.cmet.2017.04.003
Xuan X, Gao F, Ma X et al (2018) Activation of ACE2/angiotensin (1–7) attenuates pancreatic β cell dedifferentiation in a high-fat-diet mouse model. Metabolism 81:83–96. https://doi.org/10.1016/j.metabol.2017.12.003
Oguri Y, Shinoda K, Kim H, Alba DL, Kajimura S (2020) CD81 controls beige fat progenitor cell growth and energy balance via FAK signaling. Cell 182(3):563–577. https://doi.org/10.1016/j.cell.2020.06.021
Barsby T, Otonkoski T (2022) Maturation of beta cells: lessons from in vivo and in vitro models. Diabetologia 65(6):917–930. https://doi.org/10.1007/s00125-022-05672-y
Nasteska D, Fine NHF, Ashford FB et al (2021) PDX1LOW MAFALOW β-cells contribute to islet function and insulin release. Nat Commun 12(1):674. https://doi.org/10.1038/s41467-020-20632-z
Corpe CP, Eck P, Wang J, Al-Hasani H, Levine M (2013) Intestinal dehydroascorbic acid (DHA) transport mediated by the facilitative sugar transporters, GLUT2 and GLUT8. J Biol Chem 288(13):9092–9101. https://doi.org/10.1074/jbc.M112.436790
Mueckler M, Kruse M, Strube M, Riggs AC, Chiu KC, Permutt MA (1994) A mutation in the Glut2 glucose transporter gene of a diabetic patient abolishes transport activity. J Biol Chem 269(27):17765. https://doi.org/10.1016/S0021-9258(17)32372-4
Acknowledgements
The authors wish to thank all research staff in Department of Endocrinology of the First Affiliated Hospital of Nanjing Medical University who participated in this work. We would like to thank S. Wang of Tianjin First Central Hospital for providing human islet and pancreatic tissue. We would like to thank the Core Facility of the First Affiliated Hospital of Nanjing Medical University for its help in the experiments. The graphical abstract and Fig. 7 were created with BioRender.com.
Authors’ relationships and activities
The authors declare that there are no relationships or activities that might bias, or be perceived to bias, their work.
Contribution statement
TY and KX directed the study, were responsible for study design, interpretation of data, and overall project management, and revised the manuscript and approved the final version to be published. QF, HJ, and YQ performed the cell and animal experiments, wrote the first draft of the manuscript, and reviewed and edited the final manuscript. HL, HD, YZ, YC, SL, and XX contributed to the acquisition of data and analysis of data and revised the manuscript. YH, RG, SZ, and YL acquired, analysed, and interpreted the data, and reviewed and edited the manuscript. All authors have approved the final version to be published. TY is responsible for the integrity of the work as a whole.
Funding
This work was supported by the National Natural Science Foundation of China (81830023, 82070803, 82100838 and 82100837).
Author information
Authors and Affiliations
Corresponding authors
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
ESM
(PDF 2326 kb)
ESM Table 1
(XLSX 11 kb)
ESM Table 2
(XLSX 9 kb)
ESM Table 3
(XLSX 87 kb)
ESM Table 4
(XLSX 130 kb)
ESM Table 5
(XLSX 39184 kb)
ESM Table 6
(XLSX 1235 kb)
ESM Table 7
(XLSX 1562 kb)
ESM Table 8
(XLSX 1895 kb)
ESM Table 9
(XLSX 1888 kb)
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Fu, Q., Jiang, H., Qian, Y. et al. Single-cell RNA sequencing combined with single-cell proteomics identifies the metabolic adaptation of islet cell subpopulations to high-fat diet in mice. Diabetologia 66, 724–740 (2023). https://doi.org/10.1007/s00125-022-05849-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00125-022-05849-5