Abstract
Background
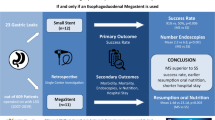
Endoscopy is the gold standard for the treatment of postoperative gastric leaks (GL). Large fistulas are associated with high rate of treatment failure. The objective of this study was to assess the clinical efficacy of a combining technique using a covered stent (CS) crossing through pigtails (PDs) for large postsurgical GL leaks.
Methods
All consecutive patients with large (> 10 mm) postsurgical GL treated endoscopically with a combination of a CS and PDs were included in a single-center retrospective study. The primary endpoint was the rate of GL closure.
Results
A total of 29 patients were included. Twenty-five patients underwent sleeve gastrectomy. The fistula (median diameter 15 mm) was diagnosed 6 days (IQR 4–9) after surgery. Technical success was observed in all procedures. After a median follow-up of 10.7 months (IQR 3.8–20.7), GL closure was observed in 82.7% with a median time of 63 days (IQR 40–90). Surgical management was finally necessary in four patients after a median of 186 days (IQR 122–250). No complications related to combined endoscopic treatment were observed especially stent migration during the follow-up.
Conclusion
An endoscopic strategy combining CS crossing through PDs appears to be effective, safe and well tolerated for the treatment of large GL.



Similar content being viewed by others
Change history
27 December 2022
A Correction to this paper has been published: https://doi.org/10.1007/s00464-022-09847-x
Abbreviations
- PG :
-
Pigtail
- CS :
-
Cover stent
- GL :
-
Gastric leak
References
Kim J, Azagury D, Eisenberg D et al (2015) ASMBS position statement on prevention, detection, and treatment of gastrointestinal leak after gastric bypass and sleeve gastrectomy, including the roles of imaging, surgical exploration, and nonoperative management. Surg Obes Relat Dis 11:739–748. https://doi.org/10.1016/j.soard.2015.05.001
Gjeorgjievski M, Imam Z, Cappell MS et al (2020) A comprehensive review of endoscopic management of sleeve gastrectomy leaks. J Clin Gastroenterol 55(7):551–576. https://doi.org/10.1097/MCG.0000000000001451
Martínez Hernández A, Beltrán Herrera H, Martínez García V et al (2022) Stent management of leaks after bariatric surgery: a systematic review and meta-analysis. Obes Surg 32:1034–1048. https://doi.org/10.1007/s11695-022-05890-8
Badurdeen DS, Lamond K, Gandsas A et al (2019) Endoscopic strategies for the treatment of postbariatric surgery leaks and fistulas. Tech Gastrointest Endosc 21:71–82. https://doi.org/10.1016/j.tgie.2019.03.011
Murino A, Arvanitakis M, Le Moine O et al (2015) Effectiveness of endoscopic management using self-expandable metal stents in a large cohort of patients with post-bariatric leaks. Obes Surg 25:1569–1576. https://doi.org/10.1007/s11695-015-1596-8
da Martins B, C. (2014) Endoscopic management and prevention of migrated esophageal stents. WJGE 6(2):49. https://doi.org/10.4253/wjge.v6.i2.49
Conio M, Savarese MF, Baron TH et al (2020) A newly designed over-the-scope-clip device to prevent fully covered metal stents migration: a pilot study. Tech Innov Gastrointest Endosc 22:167–171. https://doi.org/10.1016/j.tige.2020.05.004
Giuliani A, Romano L, Marchese M et al (2019) Gastric leak after laparoscopic sleeve gastrectomy: management with endoscopic double pigtail drainage. A systematic review. Surg Obes Relat Dis 15(8):1414–1419. https://doi.org/10.1016/j.soard.2019.03.019
Nedelcu M, Manos T, Cotirlet A et al (2015) Outcome of leaks after sleeve gastrectomy based on a new algorithm adressing leak size and gastric stenosis. Obes Surg 25:559–563. https://doi.org/10.1007/s11695-014-1561-y
Caiazzo R, Marciniak C, Wallach N et al (2020) Malignant leakage after sleeve gastrectomy: endoscopic and surgical approach. Obes Surg 30:4459–4466. https://doi.org/10.1007/s11695-020-04818-4
Manos T, Nedelcu M, Nedelcu A et al (2021) Leak after sleeve gastrectomy: updated algorithm of treatment. Obes Surg 31:4861–4867. https://doi.org/10.1007/s11695-021-05656-8
Rebibo L, Hakim S, Brazier F et al (2016) New endoscopic technique for the treatment of large gastric fistula or gastric stenosis associated with gastric leaks after sleeve gastrectomy. Surg Obes Relat Dis 12:1577–1584. https://doi.org/10.1016/j.soard.2016.04.026
Kichler K, Rosenthal RJ, DeMaria E et al (2019) Reoperative surgery for nonresponders and complicated sleeve gastrectomy operations in patients with severe obesity. An international expert panel consensus statement to define best practice guidelines. Surg Obes Relat Dis 15(2):173–186. https://doi.org/10.1016/j.soard.2018.11.006
Rosenthal RJ (2012) International sleeve gastrectomy expert panel consensus statement: best practice guidelines based on experience of > 12,000 cases. Surg Obes Relat Dis 8:8–19. https://doi.org/10.1016/j.soard.2011.10.019
Gagner M, Deitel M, Erickson AL et al (2013) Survey on laparoscopic sleeve gastrectomy (LSG) at the fourth international consensus summit on sleeve gastrectomy. Obes Surg 23:2013–2017. https://doi.org/10.1007/s11695-013-1040-x
Lafeuille P, Wallenhorst T, Lupu A et al (2021) Endoscopic submucosal dissection combined with clip for closure of gastrointestinal fistulas including those refractory to previous therapy. Endoscopy. https://doi.org/10.1055/a-1641-7938
Rogalski P, Swidnicka-Siergiejko A, Wasielica-Berger J et al (2021) Endoscopic management of leaks and fistulas after bariatric surgery: a systematic review and meta-analysis. Surg Endosc 35:1067–1087. https://doi.org/10.1007/s00464-020-07471-1
Law R, Prabhu A, Fujii-Lau L et al (2018) Stent migration following endoscopic suture fixation of esophageal self-expandable metal stents: a systematic review and meta-analysis. Surg Endosc 32:675–681. https://doi.org/10.1007/s00464-017-5720-9
Donatelli G, Dumont J-L, Cereatti F et al (2015) Treatment of leaks following sleeve gastrectomy by endoscopic internal drainage (EID). Obes Surg 25:1293–1301. https://doi.org/10.1007/s11695-015-1675-x
Cosse C, Rebibo L, Brazier F et al (2018) Cost-effectiveness analysis of stent type in endoscopic treatment of gastric leak after laparoscopic sleeve gastrectomy. Br J Surg 105:570–577. https://doi.org/10.1002/bjs.10732
Kim Y-I, Lee JY, Khalayleh H et al (2022) Efficacy of endoscopic management for anastomotic leakage after gastrectomy in patients with gastric cancer. Surg Endosc 36:2896–2905. https://doi.org/10.1007/s00464-021-08582-z
Thomsen T, Villebro N, Møller AM (2014) Interventions for preoperative smoking cessation. Cochrane Database Syst Rev. https://doi.org/10.1002/14651858.CD002294.pub4
Sørensen LT (2012) Wound healing and infection in surgery: the clinical impact of smoking and smoking cessation: a systematic review and meta-analysis. Arch Surg 147:373. https://doi.org/10.1001/archsurg.2012.5
Stenberg E, dos Reis Falcão LF, O’Kane M et al (2022) Guidelines for perioperative care in bariatric surgery: enhanced recovery after surgery (ERAS) society recommendations: a 2021 update. World J Surg 46:729–751. https://doi.org/10.1007/s00268-021-06394-9
Nimeri A, Ibrahim M, Maasher A et al (2016) Management algorithm for leaks following laparoscopic sleeve gastrectomy. Obes Surg 26:21–25. https://doi.org/10.1007/s11695-015-1751-2
Bashah M, Khidir N, EL-Matbouly M. (2020) Management of leak after sleeve gastrectomy: outcomes of 73 cases, treatment algorithm and predictors of resolution. Obes Surg 30(2):515–520. https://doi.org/10.1007/s11695-019-04203-w
Spota A, Cereatti F, Granieri S et al (2021) Endoscopic management of bariatric surgery complications according to a standardized algorithm. Obes Surg 31:4327–4337. https://doi.org/10.1007/s11695-021-05577-6
Funding
None.
Author information
Authors and Affiliations
Contributions
CY, and SH were involved in study concept and design. CY and JPLM contributed to acquisition of data. CY, MF, SH, FB were involved in analysis and interpretation of data. CY was involved in drafting of the manuscript and is Guarantor of the article. CY, SH, JPLM, FB, MF, ENK, MP contributed to critical revision of the manuscript for important intellectual content and approval of the final manuscript.
Corresponding author
Ethics declarations
Disclosures
Mathurin Fumery: lecture and consultant fees from Abbvie, Pfizer, MSD, Takeda, Ferring, Janssen, Boehringer, Celgene, Gilead, Galapagos, Biogen, Amgen. Clara Yzet: lecture and consultant fees Abbvie, Takeda, Janssen, Galapagos. Sami Hakim, Mathieu Pioche, Jean-phillippe Le Mouel, Constance Deschepper, Pierre Lafeuille, Richard Delcenserie, Thierry Yzet, Eric Nguyen-Khac and Franck Brazier have no conflicts of interest or financial ties to disclose.
Ethical approval
The protocol was approved by the institutional review board (CNIL committee: Comite Consultatif sur le Traitement de l’Information en matière de Recherche dans le domaine de la Sante) No PI2020_843_0155.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Yzet, C., Hakim, S., Pioche, M. et al. Endoscopic treatment of large gastric leaks after gastrectomy using the combination of double pigtail drains crossing a covered stent. Surg Endosc 36, 9469–9475 (2022). https://doi.org/10.1007/s00464-022-09623-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-022-09623-x