Abstract
Oral cancers affect millions of people globally, with increasing incidences among adults aged 35 and above. Poor drug uptake by lesions in the oral cavity following systemic administration, as well as limited localized treatment modalities for oral tumors, result in poor patient quality of life and high mortality. Here, we describe a solid, dissolvable, bioadhesive alginate patch containing freeze-dried doxorubicin-loaded liposomes as a local treatment for oral tumors located on the tongue. By varying the alginate-to-liposome ratio in the mucoadhesive patch, we could control the degree of bioadhesion to the tongue and the release profile of the drug-loaded liposomes from the matrix. In vitro, exposing squamous cell carcinoma (SCC) to the alginate mucoadhesive patch or tablet resulted in dose-dependent cancer-cell death. In vivo, the efficacy of the local treatment was demonstrated in mice bearing orthotopic SCC tumors in the tongue. The bioadhesive patch, applied directly above the lesion, significantly reduced the tumor size and treatment-associated side effects compared to implanted patches or systemic drug administration. This study demonstrates that local bioadhesive therapies are effective in treating cancers of the oral cavity.
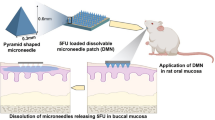
Graphical abstract






Similar content being viewed by others
References
Torre LA, et al. Global cancer statistics, 2012. Ca-a Cancer Journal for Clinicians. 2015;65(2):87–108. https://doi.org/10.3322/caac.21262.
Ferrazzano GF, et al. Cyanobacteria and microalgae as sources of functional foods to improve human general and oral health. Molecules. 2020;25(21). https://doi.org/10.3390/molecules25215164.
Parkin DM, et al. Global cancer statistics, 2002. Ca-a Cancer Journal for Clinicians. 2005;55(2):74–108. https://doi.org/10.3322/canjclin.55.2.74.
Ferlay J, et al. Estimates of worldwide burden of cancer in 2008: GLOBOCAN 2008. Int J Cancer. 2010;127(12):2893–917. https://doi.org/10.1002/ijc.25516.
Gupta B, Johnson NW, Kumar N. Global epidemiology of head and neck cancers: a continuing challenge. Oncology. 2016;91(1):13–23. https://doi.org/10.1159/000446117.
Chi AC, T.A.D., Brad W. Neville, Oral Cavity and oropharyngeal squamous cell carcinoma—an update. Oral & Oropharyngeal Cancer Update. 2015;65(5):402–21. https://doi.org/10.3322/caac.21293.
Montero PH, Patel SG. Cancer of the oral cavity. Surg Oncol Clin N Am. 2015;24(3):491–508. https://doi.org/10.1016/j.soc.2015.03.006.
Hashibe M, et al. Interaction between tobacco and alcohol use and the risk of head and neck cancer: pooled analysis in the International Head and Neck Cancer Epidemiology Consortium. Cancer Epidemiol Biomarkers Prev. 2009;18(2):541–50. https://doi.org/10.1158/1055-9965.EPI-08-0347.
Weatherspoon DJ, et al. Oral cavity and oropharyngeal cancer incidence trends and disparities in the United States: 2000–2010. Cancer Epidemiol. 2015;39(4):497–504. https://doi.org/10.1016/j.canep.2015.04.007.
Kumar M, Nanavati N, Modi TG, Dobariya C. Oral cancer: etiology and risk factors. J Cancer Res Ther. 2016;12(2):458–63. https://doi.org/10.4103/0973-1482.186696.
Furness S, et al. Interventions for the treatment of oral cavity and oropharyngeal cancer: chemotherapy. Cochrane Database Syst Rev. 2010;(1469–493X (Electronic)). https://doi.org/10.1002/14651858.CD006386.pub2.
Thanki K, Gangwal RP, Sangamwar AT, Jain S. Oral delivery of anticancer drugs: challenges and opportunities. J Control Release. 2013;28:170(1):15–40. https://doi.org/10.1016/j.jconrel.2013.04.020.
Markopoulos C. aspects on oral squamous cell carcinoma. Open Dent J. 2012;6:126–30. https://doi.org/10.2174/1874210601206010126.
Smart JD. The basics and underlying mechanisms of mucoadhesion. Adv Drug Deliv Rev. 2005;57(11):1556–68. https://doi.org/10.1016/j.addr.2005.07.001.
Macedo AS, Castro PM, Roque L, Thomé NJ, Reis CP, Pintado ME, Fonte P. Novel and revisited approaches in nanoparticle systems for buccal drug delivery. J Control Release. 2020;320: 125–141. https://doi.org/10.1016/j.jconrel.2020.01.006.
Galey WR, Lonsdale HK, Nacht S. Invitro permeability of skin and buccal mucosa to selected drugs and tritiated-water. J Investig Dermatol. 1976;67(6):713–7. https://doi.org/10.1111/1523-1747.ep12598596.
Gandhi RB, Robinson JR. Oral cavity as a site for bioadhesive drug-delivery. Adv Drug Deliv Rev. 1994;13(1–2):43–74. https://doi.org/10.1016/0169-409x(94)90026-4.
Bansil R, Turner BS. Mucin structure, aggregation, physiological functions and biomedical applications. Curr Opin Colloid Interface Sci. 2006;11(2–3):164–70. https://doi.org/10.1016/j.cocis.2005.11.001.
Lee KY, Mooney DJ. Alginate: properties and biomedical applications. Prog Polym Sci. 2012;37(1):106–26. https://doi.org/10.1016/j.progpolymsci.2011.06.003.
Kesavan K, Nath G, Pandit JK. Preparation and in vitro antibacterial evaluation of gatifloxacin mucoadhesive gellan system. Daru-Journal of Pharmaceutical Sciences. 2010;18(4):237–46.
Sosnik A, das Neves J, Sarmento B. Mucoadhesive polymers in the design of nano-drug delivery systems for administration by non-parenteral routes: A review. Prog Polym Sci. 2014;39(12):2030–2075. https://doi.org/10.1016/j.progpolymsci.2014.07.010.
George M, Abraham TE. Polyionic hydrocolloids for the intestinal delivery of protein drugs: alginate and chitosan - a review. J Control Release. 2006;114(1):1–14. https://doi.org/10.1016/j.jconrel.2006.04.017.
Torchilin VP. Recent advances with liposomes as pharmaceutical carriers. Nat Rev Drug Discovery. 2005;4(2):145–60. https://doi.org/10.1038/nrd1632.
Ostro MJ, Cullis PR. Use of liposomes as injectable-drug delivery systems. Am J Hosp Pharm. 1989;46(8):1576–87. https://doi.org/10.1093/ajhp/46.8.1576.
Franks F. Freeze-drying of bioproducts: putting principles into practice. Eur J Pharm Biopharm. 1998;45(3):221–9. https://doi.org/10.1016/S0939-6411(98)00004-6.
Abdelwahed W, Degobert G, Fessi H. Investigation of nanocapsules stabilization by amorphous excipients during freeze-drying and storage. Eur J Pharm Biopharm. 2006;63(2):87–94. https://doi.org/10.1016/j.ejpb.2006.01.015.
Abdelwahed W, et al. Freeze-drying of nanoparticles: formulation, process and storage considerations. Adv Drug Deliv Rev. 2006;58(15):1688–713. https://doi.org/10.1016/j.addr.2006.09.017.
Tang XL, Pikal MJ. Design of freeze-drying processes for pharmaceuticals: Practical advice. Pharm Res. 2004;21(2):191–200. https://doi.org/10.1023/B:Pham.0000016234.73023.75.
Williams NA, Polli GP. The lyophilization of pharmaceuticals: a literature review. J Parenter Sci Technol. 1984;38(2):48–59.
Crowe JH, Hoekstra FA, Crowe LM. Anhydrobiosis. Annu Rev Physiol. 1992;54:579–99. https://doi.org/10.1146/annurev.ph.54.030192.003051.
Crowe LM, Reid DS, Crowe JH. Is trehalose special for preserving dry biomaterials? Biophys J. 1996;71(4):2087–93. https://doi.org/10.1016/S0006-3495(96)79407-9.
Crommelin DJA, Vanbommel EMG. Stability of liposomes on storage - freeze-dried, frozen or as an aqueous dispersion. Pharm Res. 1984;4:159–63. https://doi.org/10.1023/A:1016344523988.
Haran G, et al. Transmembrane ammonium-sulfate gradients in liposomes produce efficient and stable entrapment of amphipathic weak bases. Biochem Biophys Acta. 1993;1151(2):201–15. https://doi.org/10.1016/0005-2736(93)90105-9.
Marques MRC, Loebenberg R, Almukainzi M. Simulated Biological fluids with possible application in dissolution testing. Dissolut Technol. 2011;18(3):15–28. https://doi.org/10.14227/Dt180311p15.
Ansar SM, Mudalige T. Direct and simultaneous determination of intra-liposomal and external sulfate in liposomal doxorubicin formulations by capillary electrophoresis/inductively coupled plasma-tandem mass spectrometry (CE/ICP-MS/MS). Int J Pharm. 2019;561:283–288 S0378517319301784. https://doi.org/10.1016/j.ijpharm.2019.03.003.
Albrecht K, et al. Preparation of thiomer microparticles and in vitro evaluation of parameters influencing their mucoadhesive properties. Drug Dev Ind Pharm. 2006;32(10):1149–57. https://doi.org/10.1080/03639040600712334.
Issman L, Talmon Y. Cryo-SEM specimen preparation under controlled temperature and concentration conditions. J Microsc. 2012;246(1):60–9. https://doi.org/10.1111/j.1365-2818.2011.03587.x.
Rosenberg M, Talmon Y, Kopelman IJ. The microstructure of spray-dried microcapsules. Food Microstructure. 1988;7(1):15–23.
Pohl H. A Scanning electron microscopy specimen holder for viewing different angles of a single specimen. Microsc Res Tech. 2010;73(12):1073–6. https://doi.org/10.1002/jemt.20835.
Inc., A. Adobe Illustrator. CC 2019 (23.0.3): Available from: Adobe Illustrator. 2019.
Cook MT, Khutoryanskiy VV. Mucoadhesion and mucosa-mimetic materials-A mini-review. Int J Pharm. 2015;495(2):991–8. https://doi.org/10.1016/j.ijpharm.2015.09.064.
Drummond DC, et al. Optimizing liposomes for delivery of chemotherapeutic agents to solid tumors. Pharmacol Rev. 1999;51(4):691–743.
Crowe LM, et al. Prevention of fusion and leakage in freeze-dried liposomes by carbohydrates. Biochem Biophys Acta. 1986;861(1):131–40. https://doi.org/10.1016/0005-2736(86)90411-6.
Tsvetkova NM, et al. Effect of sugars on headgroup mobility in freeze-dried dipalmitoylphosphatidylcholine bilayers: solid-state P-31 NMR and FTIR studies. Biophys J. 1998;75(6):2947–55. https://doi.org/10.1016/S0006-3495(98)77736-7.
Liu J, Chen C, Li W. Protective mechanisms of α,α-trehalose revealed by molecular dynamics simulations. Mol Simul. 2018;44:100–109. https://doi.org/10.1080/08927022.2017.1342126.
Allison SD, et al. Effects of drying methods and additives on structure and function of actin: mechanisms of dehydration-induced damage and its inhibition. Arch Biochem Biophys. 1998;358(1):171–81. https://doi.org/10.1006/abbi.1998.0832.
Barenholz Y. Doxil (R) - The first FDA-approved nano-drug: lessons learned. J Control Release. 2012;160(2):117–34. https://doi.org/10.1016/j.jconrel.2012.03.020.
Cox PJ, et al. Development and evaluation of a multiple-unit oral sustained release dosage form for S(+)-ibuprofen: preparation and release kinetics. Int J Pharm. 1999;193(1):73–84. https://doi.org/10.1016/S0378-5173(99)00320-8.
Liew CV, et al. Evaluation of sodium alginate as drug release modifier in matrix tablets. Int J Pharm. 2006;309(1–2):25–37. https://doi.org/10.1016/j.ijpharm.2005.10.040.
Skoug JW, et al. Qualitative evaluation of the mechanism of release of matrix sustained-release dosage forms by measurement of polymer release. J Control Release. 1993;27(3):227–45. https://doi.org/10.1016/0168-3659(93)90154-W.
Kalyanaraman B, et al. Doxorubicin-induced apoptosis: implications in cardiotoxicity. Mol Cell Biochem. 2002;234(1):119–24. https://doi.org/10.1023/A:1015976430790.
Tahover E, Patil YP, Gabizon AA. Emerging delivery systems to reduce doxorubicin cardiotoxicity and improve therapeutic index: focus on liposomes. Anticancer Drugs. 2015;26(3):241–58.
Ta HT, et al. A chitosan–dipotassium orthophosphate hydrogel for the delivery of doxorubicin in the treatment of osteosarcoma. Biomaterials. 2009;3605–3613.
Zhang R, et al. Catalase-loaded cisplatin-prodrug-constructed liposomes to overcome tumor hypoxia for enhanced chemo-radiotherapy of cancer. Biomaterials. 2017;138:13–21. https://doi.org/10.1016/j.biomaterials.2017.05.025.
Acknowledgements
The authors acknowledge the support of the Technion Integrated Cancer Center (TICC), the Russell Berrie Nanotechnology Institute (RBNI), and the Lorry I. Lokey Interdisciplinary Center for Life Sciences & Engineering. The authors wish to thank Dr. Naama Koifman for her help with cryo-SEM imaging. The authors would like to thank Ms. Natalie Page for proofreading of the article.
Funding
This project received funding from the Israel Ministry of Economy for a Kamin Grant (52752, 63379, 69230). A. Schroeder acknowledges the contribution of European Union’s Horizon 2020 research and innovation programme under grant agreement No 680242-ERC-[Next-Generation Personalized Diagnostic Nanotechnologies for Predicting Response to Cancer Medicine]; Israel Science Foundation (1778/13, 1421/17); Israel Ministry of Science and Technology (3–17418); Phospholipid Research Center Grant (ASC-2018–062/1–1); Leventhal 2020 COVID19 Research Fund (ATS #11947); Louis family Cancer Research Fund; a Mallat Family Foundation grant; The Unger Family Fund; Carrie Rosenblatt Cancer Research Fund; Alon and Taub Fellowships.
Supplementary data are available online, and from the corresponding author upon reasonable request.
Author information
Authors and Affiliations
Contributions
Material preparation, data collection, and data analysis were done by Layan Habib, Mohammed Alyan, and Yasmine Ghantous. All authors contributed to the study’s conception and design and read and approved the final manuscript.
Corresponding author
Ethics declarations
Ethics approval and consent to participate
All animal experiments were approved by, and were in compliance with, the Technion ethics committee (Approval numbers IL-056–05-16, IL-098–08-20), and all national and institutional guidelines for the care and use of laboratory animals were followed. No human studies were carried out by the authors for this article.
Consent for publication
Not applicable.
Competing interests
Based on the research funding, a provisional patent application was submitted by Bianco-Peled H, Schroeder A, Abu El-Naaj I, Habib L, Alyan M and Ghantous Y.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Habib, L., Alyan, M., Ghantous, Y. et al. A mucoadhesive patch loaded with freeze-dried liposomes for the local treatment of oral tumors. Drug Deliv. and Transl. Res. 13, 1228–1245 (2023). https://doi.org/10.1007/s13346-022-01224-4
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13346-022-01224-4