Abstract
Summary
This population-based study investigated the association between depression and bone mineral density (BMD), fractures, and osteoporosis in the US population. We found that participants with depression had lower BMD and were more likely to have fractures and osteoporosis.
Background
Depression, fractures, and osteoporosis are common in middle-aged and elderly, but their associations remained unclear.
Objective
To investigate the association between depression and bone mineral density (BMD), osteoporosis, and fracture in a middle-aged and elderly US population.
Methods
A nationally representative cross-sectional study used the National Health and Nutrition Examination Survey (NHANES) datasets. Depression was assessed and stratified using the Patient Health Questionnaire (PHQ-9). The multiple logistic regression models and the logistic binary regression models were used to analyze the association between depression and BMD, fractures, and osteoporosis. Gender, age, race, educational level, poverty ratio, body mass index (BMI), smoke, alcohol use, physical activity, and diabetes were included as covariates. Subgroup analysis was also conducted on gender, age, race, and education level.
Results
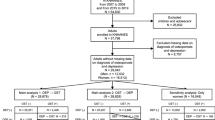
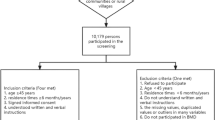
In total, 9766 participants were included after a series of exclusions, and 4179 (42.79%) had at least mild depressive symptoms. Compared to the participants without depression, those with depression had a lower total femur, femoral neck, and total spine BMD after adjusting multiple covariates. The multivariable-adjusted logistic binary regression models demonstrated that participants with depression more likely have hip fractures (OR = 1.518, 95% CI: 1.377–2.703, P = 0.000), spine fractures (OR = 1.311, 95% CI: 1.022–1.678, P = 0.030), and osteoporosis (OR = 1.621, 95% CI: 1.388–1.890, P = 0.000). Subgroup analysis revealed that depressed participants who were males, non-Hispanic White, ≤ 70 years, and not highly educated had a lower BMD and easily had osteoporosis.
Conclusion
Depression was associated with lower BMD, particularly in the spine, males, Hispanic-White, and not highly educated populations. Moreover, people with depression were more likely to have fractures and osteoporosis.



Similar content being viewed by others
Data availability
The datasets are available on https://www.cdc.gov/nchs/nhanes/index.htm, and further inquiries can be directed to the corresponding authors.
References
Wright NC, Looker AC, Saag KG, Curtis JR, Delzell ES, Randall S et al (2014) The recent prevalence of osteoporosis and low bone mass in the United States based on bone mineral density at the femoral neck or lumbar spine. J Bone Miner Res 29:2520–2526. https://doi.org/10.1002/jbmr.2269
Marshall D, Johnell O, Wedel H (1996) Meta-analysis of how well measures of bone mineral density predict occurrence of osteoporotic fractures. Br Med J 312:1254–1259. https://doi.org/10.1136/bmj.312.7041.1254
Cummings SR, Kelsey JL, Nevitt MC, Odowd KJ (1985) Epidemiology of osteoporosis and osteoporotic fractures. Epidemiol Rev 7:178–208. https://doi.org/10.1093/oxfordjournals.epirev.a036281
Kanis JA (2002) Diagnosis of osteoporosis and assessment of fracture risk. Lancet 359:1929–1936. https://doi.org/10.1016/s0140-6736(02)08761-5
Reginster JY, Burlet N (2006) Osteoporosis: a still increasing prevalence. Bone 38:4–9. https://doi.org/10.1016/j.bone.2005.11.024
Hernlund E, Svedbom A, Ivergard M, Compston J, Cooper C, Stenmark J et al (2013) Osteoporosis in the European Union: medical management, epidemiology and economic burden. Arch Osteoporos 8:115. https://doi.org/10.1007/s11657-013-0136-1
Rachner TD, Khosla S, Hofbauer LC (2011) Osteoporosis: now and the future. Lancet 377:1276–1287. https://doi.org/10.1016/s0140-6736(10)62349-5
Cizza G, Ravn P, Chrousos GP, Gold PW (2001) Depression: a major, unrecognized risk factor for osteoporosis? Trends Endocrinol Metab 12:198–203. https://doi.org/10.1016/s1043-2760(01)00407-6
Cizza G, Primma S, Csako G (2009) Depression as a risk factor for osteoporosis. Trends Endocrinol Metab 20:367–373. https://doi.org/10.1016/j.tem.2009.05.003
Kok RM, Reynolds CF 3rd (2017) Management of depression in older adults: a review. Jama 317:2114–2122. https://doi.org/10.1001/jama.2017.5706
Whooley MA, Kip KE, Cauley JA, Ensrud KE, Nevitt MC, Browner WS (1999) Depression, falls, and risk of fracture in older women. Study of Osteoporotic Fractures Research Group. Arch Intern Med 159:484–490. https://doi.org/10.1001/archinte.159.5.484
Forsén L, Meyer HE, Søgaard AJ, Naess S, Schei B, Edna TH (1999) Mental distress and risk of hip fracture. Do broken hearts lead to broken bones? J Epidemiol Community Health 53:343–347. https://doi.org/10.1136/jech.53.6.343
Cheng BH, Chen PC, Yang YH, Lee CP, Huang KE, Chen VC (2016) Effects of depression and antidepressant medications on hip fracture: a population-based cohort study in Taiwan. Medicine (Baltimore) 95:e4655. https://doi.org/10.1097/md.0000000000004655
Wu Q, Liu B, Tonmoy S (2018) Depression and risk of fracture and bone loss: an updated meta-analysis of prospective studies. Osteoporos Int 29:1303–1312. https://doi.org/10.1007/s00198-018-4420-1
Ozsoy S, Esel E, Turan MT, Kula M, Demir H, Kartalci S et al (2005) Is there any alteration in bone mineral density in patients with depression? Turk Psikiyatri Dergisi 16:77–82
Oh SM, Kim HC, Ahn SV, Rhee Y, Suh I (2012) Association between depression and bone mineral density in community-dwelling older men and women in Korea. Maturitas 71:142–146. https://doi.org/10.1016/j.maturitas.2011.11.007
Charles LE, Fekedulegn D, Miller DB, Wactawski-Wende J, Violanti JM, Andrew ME et al (2012) Depressive symptoms and bone mineral density among police officers in a northeastern US City. Global J Health Sci 4:39–50. https://doi.org/10.5539/gjhs.v4n3p39
He B, Lyu Q, Yin L, Zhang M, Quan Z, Ou Y (2021) Depression and osteoporosis: a Mendelian randomization study. Calcif Tissue Int 109:675–684. https://doi.org/10.1007/s00223-021-00886-5
Robbins J, Hirsch C, Whitmer R, Cauley J, Harris T, Cardiovascular Hlth S (2001) The association of bone mineral density and depression in an older population. J Am Geriatr Soc 49:732–736. https://doi.org/10.1046/j.1532-5415.2001.49149.x
Tolea MI, Black SA, Carter-Pokras OD, Kling MA (2007) Depressive symptoms as a risk factor for osteoporosis and fractures in older Mexican American women. Osteoporos Int 18:315–322. https://doi.org/10.1007/s00198-006-0242-7
Wright NC, Looker AC, Saag KG, Curtis JR, Delzell ES, Randall S et al (2014) The recent prevalence of osteoporosis and low bone mass in the United States based on bone mineral density at the femoral neck or lumbar spine. J Bone Miner Res 29:2520–2526. https://doi.org/10.1002/jbmr.2269
Kesmodel US (2018) Cross-sectional studies - what are they good for? Acta Obstet Gynecol Scand 97:388–393. https://doi.org/10.1111/aogs.13331
CDC. NHANES 2017-2018 Brochures and Consent Documents. 2021; Available from: https://wwwn.cdc.gov/nchs/nhanes/continuousnhanes/documents.aspx?Cycle=2017-2018
Kroenke K, Spitzer RL, Williams JB (2001) The PHQ-9: validity of a brief depression severity measure. J Gen Intern Med 16:606–613. https://doi.org/10.1046/j.1525-1497.2001.016009606.x
Kroenke K, Spitzer RL (2002) The PHQ-9: a new depression diagnostic and severity measure. Psychiatr Ann 32:509–515. https://doi.org/10.3928/0048-5713-20020901-06
Spitzer RL, Kroenke K, Williams JB (1999) Validation and utility of a self-report version of PRIME-MD: the PHQ primary care study. Primary Care Evaluation of Mental Disorders. Patient Health Questionnaire. Jama 282:1737–1744. https://doi.org/10.1001/jama.282.18.1737
Zimmerman M (2019) Using the 9-item patient health questionnaire to screen for and monitor depression. JAMA 322:2125–2126. https://doi.org/10.1001/jama.2019.15883
Heymsfield SB, Wang J, Heshka S, Kehayias JJ, Pierson RN (1989) Dual-photon absorptiometry: comparison of bone mineral and soft tissue mass measurements in vivo with established methods. Am J Clin Nutr 49:1283–1289. https://doi.org/10.1093/ajcn/49.6.1283
Sommerhage V, Kull I, Schweiger U, Rudolf S (2013) Bone mineral density in a cohort of Estonian women with major depression. Arch Osteoporos 8:4. https://doi.org/10.1007/s11657-013-0163-y
Schweiger U, Weber B, Deuschle M, Heuser I (2000) Lumbar bone mineral density in patients with major depression: evidence of increased bone loss at follow-up. Am J Psychiatr 157:118–120. https://doi.org/10.1176/ajp.157.1.118
Laudisio A, Marzetti E, Cocchi A, Bernabei R, Zuccala G (2008) Association of depressive symptoms with bone mineral density in older men: a population-based study. Int J Geriatr Psychiatry 23:1119–1126. https://doi.org/10.1002/gps.2037
Wong SYS, Lau EMC, Lynn H, Leung PC, Woo J, Cummings SR et al (2005) depression and bone mineral density: is there a relationship in elderly Asian men? Results from Mr. Os (Hong Kong). Osteoporos Int 16:610–615. https://doi.org/10.1007/s00198-004-1730-2
Yazici AE, Bagis S, Tot E, Sahin G, Yazici K, Erdogan C (2005) Bone mineral density in premenopausal women with major depression. Joint Bone Spine 72:540–543. https://doi.org/10.1016/j.jbspin.2004.12.011
Mezuk B, Eaton WW, Golden SH, Wand G, Lee HB (2008) Depression, antidepressants, and bone mineral density in a population-based cohort. J Gerontol Series a-Biol Sci Med Sci 63:1410–1415. https://doi.org/10.1093/gerona/63.12.1410
Whooley MA, Cauley JA, Zmuda JM, Haney EM, Glynn NW (2004) Depressive symptoms and bone mineral density in older men. J Geriatr Psychiatry Neurol 17:88–92. https://doi.org/10.1177/0891988704264537
Halbreich U, Palter S (1996) Accelerated osteoporosis in psychiatric patients: possible pathophysiological processes. Schizophr Bull 22:447–454. https://doi.org/10.1093/schbul/22.3.447
Sewell MDE, Jiménez-Sánchez L, Shen X, Edmondson-Stait AJ, Green C, Adams MJ et al (2021) Associations between major psychiatric disorder polygenic risk scores and blood-based markers in UK biobank. Brain Behav Immun 97:32–41. https://doi.org/10.1016/j.bbi.2021.06.002
Skowrońska-Jóźwiak E, Gałecki P, Głowacka E, Wojtyła C, Biliński P, Lewiński A (2020) Bone metabolism in patients treated for depression. Int J Environ Res Public Health 17. https://doi.org/10.3390/ijerph17134756
Alesci S, Martinez PE, Kelkar S, Ilias I, Ronsaville DS, Listwak SJ et al (2005) Major depression is associated with significant diurnal elevations in plasma interleukin-6 levels, a shift of its circadian rhythm, and loss of physiological complexity in its secretion: clinical implications. J Clin Endocrinol Metab 90:2522–2530. https://doi.org/10.1210/jc.2004-1667
Kahl KG, Rudolf S, Dibbelt L, Stoeckelhuber BM, Gehl HB, Hohagen F et al (2005) Decreased osteoprotegerin and increased bone turnover in young female patients with major depressive disorder and a lifetime history of anorexia nervosa. Osteoporos Int 16:424–429. https://doi.org/10.1007/s00198-004-1711-5
Zavos HMS, Zunszain PA, Jayaweera K, Powell TR, Chatzivasileiadou M, Harber-Aschan L et al (2021) Relationship between CRP and depression: a genetically sensitive study in Sri Lanka. J Affect Disord 297:112–117. https://doi.org/10.1016/j.jad.2021.10.003
Gold PW (2021) The PPARg system in major depression: pathophysiologic and therapeutic implications. Int J Mol Sci 22. https://doi.org/10.3390/ijms22179248
Gold PW (2015) The organization of the stress system and its dysregulation in depressive illness. Mol Psychiatry 20:32–47. https://doi.org/10.1038/mp.2014.163
Battaglino R, Vokes M, Schulze-Späte U, Sharma A, Graves D, Kohler T et al (2007) Fluoxetine treatment increases trabecular bone formation in mice. J Cell Biochem 100:1387–1394. https://doi.org/10.1002/jcb.21131
Manelli F, Giustina A (2000) Glucocorticoid-induced osteoporosis. Trends Endocrinol Metab 11:79–85. https://doi.org/10.1016/s1043-2760(00)00234-4
Aspera-Werz RH, Ehnert S, Heid D, Zhu S, Chen T, Braun B et al (2018) Nicotine and cotinine inhibit catalase and glutathione reductase activity contributing to the impaired osteogenesis of SCP-1 cells exposed to cigarette smoke. Oxidative Med Cell Longev 2018:3172480. https://doi.org/10.1155/2018/3172480
Satarug S, Moore MR (2004) Adverse health effects of chronic exposure to low-level cadmium in foodstuffs and cigarette smoke. Environ Health Perspect 112:1099–1103. https://doi.org/10.1289/ehp.6751
Lee LL, Lee JS, Waldman SD, Casper RF, Grynpas MD (2002) Polycyclic aromatic hydrocarbons present in cigarette smoke cause bone loss in an ovariectomized rat model. Bone 30:917–923. https://doi.org/10.1016/s8756-3282(02)00726-3
Lu Y, Di YP, Chang M, Huang X, Chen Q, Hong N et al (2021) Cigarette smoke-associated inflammation impairs bone remodeling through NFκB activation. J Transl Med 19:163. https://doi.org/10.1186/s12967-021-02836-z
Rudäng R, Darelid A, Nilsson M, Nilsson S, Mellström D, Ohlsson C et al (2012) Smoking is associated with impaired bone mass development in young adult men: a 5-year longitudinal study. J Bone Miner Res 27:2189–2197. https://doi.org/10.1002/jbmr.1674
Santiago HA, Zamarioli A, Sousa Neto MD, Volpon JB (2017) Exposure to secondhand smoke impairs fracture healing in rats. Clin Orthop Relat Res 475:894–902. https://doi.org/10.1007/s11999-016-5184-6
Sinaki M, Offord KP (1988) Physical activity in postmenopausal women: effect on back muscle strength and bone mineral density of the spine. Arch Phys Med Rehabil 69:277–280
Nilsson M, Ohlsson C, Eriksson AL, Frändin K, Karlsson M, Ljunggren O et al (2008) Competitive physical activity early in life is associated with bone mineral density in elderly Swedish men. Osteoporos Int 19:1557–1566. https://doi.org/10.1007/s00198-008-0600-8
Michaëlsson K, Olofsson H, Jensevik K, Larsson S, Mallmin H, Berglund L et al (2007) Leisure physical activity and the risk of fracture in men. PLoS Med 4:e199. https://doi.org/10.1371/journal.pmed.0040199
Lagerros YT, Hantikainen E, Michaëlsson K, Ye W, Adami HO, Bellocco R (2017) Physical activity and the risk of hip fracture in the elderly: a prospective cohort study. Eur J Epidemiol 32:983–991. https://doi.org/10.1007/s10654-017-0312-5
Cizza G, Nguyen VT, Eskandari F, Duan Z, Wright EC, Reynolds JC et al (2010) Low 24-hour adiponectin and high nocturnal leptin concentrations in a case-control study of community-dwelling premenopausal women with major depressive disorder: the premenopausal, osteopenia/osteoporosis, women, alendronate, depression (POWER) study. J Clin Psychiatry 71:1079–1087. https://doi.org/10.4088/JCP.09m05314blu
Grace AA (2016) Dysregulation of the dopamine system in the pathophysiology of schizophrenia and depression. Nat Rev Neurosci 17:524–532. https://doi.org/10.1038/nrn.2016.57
Yirmiya R, Goshen I, Bajayo A, Kreisel T, Feldman S, Tam J et al (2006) Depression induces bone loss through stimulation of the sympathetic nervous system. Proc Natl Acad Sci U S A 103:16876–16881. https://doi.org/10.1073/pnas.0604234103
Barrett-Connor E, Von Mühlen DG, Kritz-Silverstein D (1999) Bioavailable testosterone and depressed mood in older men: the Rancho Bernardo study. J Clin Endocrinol Metab 84:573–577
Nelson HDM (2008) Lancet 371:760–770. https://doi.org/10.1016/s0140-6736(08)60346-3
Blunt BA, Klauber MR, Barrett-Connor EL, Edelstein SL (1994) Sex differences in bone mineral density in 1653 men and women in the sixth through tenth decades of life: the Rancho Bernardo study. J Bone Miner Res 9:1333–1338. https://doi.org/10.1002/jbmr.5650090903
Orwoll ES, Oviatt SK, Mann T (1990) The impact of osteophytic and vascular calcifications on vertebral mineral density measurements in men. J Clin Endocrinol Metab 70:1202–1207. https://doi.org/10.1210/jcem-70-4-1202
Richards JB, Rivadeneira F, Inouye M, Pastinen TM, Soranzo N, Wilson SG et al (2008) Bone mineral density, osteoporosis, and osteoporotic fractures: a genome-wide association study. Lancet 371:1505–1512. https://doi.org/10.1016/s0140-6736(08)60599-1
Willing M, Sowers M, Aron D, Clark MK, Burns T, Bunten C et al (1998) Bone mineral density and its change in white women: estrogen and vitamin D receptor genotypes and their interaction. J Bone Miner Res 13:695–705. https://doi.org/10.1359/jbmr.1998.13.4.695
Chrzastek Z, Guligowska A, Soltysik B, Pigłowska M, Borowiak E, Kostka J et al (2021) Association of lower nutritional status and education level with the severity of depression symptoms in older adults-a cross sectional survey. Nutrients 13. https://doi.org/10.3390/nu13020515
Acknowledgements
We thank the NHANES Project for providing the data free of charge and all NHANES Project staff and anonymous participants.
Funding
This work was supported by the National Natural Science Foundation of China (81874017, 81960403, and 82060405); the Natural Science Foundation of Gansu Province of China (20JR5RA320); and the Cuiying Scientific and Technological Innovation Program of Lanzhou University Second Hospital (CY2017-ZD02).
Author information
Authors and Affiliations
Contributions
Ming Ma designed the study and prepared the first draft of the paper. The authors Xiaolong Liu, Gengxin Jia, Zhongcheng Liu, Kun Zhang, and Liangzhi He contributed to the analysis work. The authors Bin Geng and Yayi Xia administrated, reviewed, edited, and supervised this work. All authors revised the paper critically for intellectual content and approved the final version. All authors agree to be accountable for the work and ensure that any questions relating to the accuracy and integrity of the paper are investigated and properly resolved. Ming Ma, Xiaolong Liu, and Gengxin Jia friendly shared the first authorship.
Corresponding author
Ethics declarations
Ethics approval and consent to participate
The National Center for Health Statistics (NCHS) Research Ethics Review Board (ERB) approved this study. Participants were voluntary, confidential, and signed the informed consent form. Further information can be found at https://www.cdc.gov/nchs/nhanes/irba98.htm.
Conflicts of interest
None.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
Springer Nature or its licensor holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Ma, M., Liu, X., Jia, G. et al. The association between depression and bone metabolism: a US nationally representative cross-sectional study. Arch Osteoporos 17, 113 (2022). https://doi.org/10.1007/s11657-022-01154-1
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s11657-022-01154-1