Abstract
The paradigm of one drug against multiple targets, known as unimolecular polypharmacology, offers the potential to improve efficacy while overcoming some adverse events associated with the treatment. This approach is best exemplified by targeting two or three class B1 G protein-coupled receptors, namely, glucagon-like peptide-1 receptor (GLP-1R), glucagon receptor (GCGR) and glucose-dependent insulinotropic polypeptide receptor for treatment of type 2 diabetes and obesity. Some of the dual and triple agonists have already shown initial successes in clinical trials, although the molecular mechanisms underlying their multiplexed pharmacology remain elusive. In this study we employed structure-based site-directed mutagenesis together with pharmacological assays to compare agonist efficacy across two key signaling pathways, cAMP accumulation and ERK1/2 phosphorylation (pERK1/2). Three dual agonists (peptide 15, MEDI0382 and SAR425899) and one triple agonist (peptide 20) were evaluated at GLP-1R and GCGR, relative to the native peptidic ligands (GLP-1 and glucagon). Our results reveal the existence of residue networks crucial for unimolecular agonist-mediated receptor activation and their distinct signaling patterns, which might be useful to the rational design of biased drug leads.
Similar content being viewed by others
Introduction
The secretin subfamily of G protein-coupled receptors (GPCRs) comprise 15 receptors that regulate cardiovascular, metabolic and immune responses [1,2,3]. They share the seven transmembrane (7TM) topology and a large extracellular domain (ECD). In a “two-domain/step” binding mode of this class of GPCRs, the C terminus of a peptide initially binds to the ECD to enable subsequent interaction of its N terminus with the TM domain [4,5,6], thereby inducing conformational changes that activate an array of intracellular signal transducers. These events are supported by extensive molecular and pharmacological studies, where the transmembrane domain (TMD) residues play broad roles in both ligand recognition and conformational propagation associated with signaling efficacy and biased agonism [7,8,9,10,11,12,13,14].
Glucagon-like peptide-1 receptor (GLP-1R), glucagon receptor (GCGR) and glucose-dependent insulinotropic polypeptide receptor (GIPR) are key players in the regulation of energy metabolism and considered as therapeutic targets for metabolic diseases [15]. Of significance is glycemic control and weight loss efficacies demonstrated by GLP-1R agonists [16, 17] despite some side-effects mainly in the gastrointestinal tract [18, 19]. GLP-1R, GCGR, and GIPR have high sequence homologies and overlapping downstream signaling cascades, such as canonical cyclic adenosine monophosphate (cAMP) accumulation. However, each receptor variably couples to secondary proteins resulting in different physiological functions [20]. Dual agonists at GLP-1R and GCGR were thus developed to provide a balanced therapeutic outcome [21, 22]. Glucagon promotes lipid metabolism, ketogenesis and has a central satiating effect, which decreases food intake and increases energy expenditure [23,24,25], leading to a more pronounced weight loss effect than GLP-1R agonism alone [26].
Like GLP-1, GIP exerts its insulinotropic action via pancreatic β cells. It also targets adipose tissues and enhances lipid accumulation, whereas central GIPR activation may lower food intake and aid weight loss [27,28,29]. The concept of a dual agonist at GLP-1R and GIPR could be realized by modulating the glucagonotropic effect of GIP through balanced activation of each receptor [22, 30].
Development of triple agonists at GLP-1R, GCGR and GIPR has attracted much attention since simultaneous activation of GCGR and GIPR in addition to GLP-1R may reduce both hyperglycemic and obesogenic risks [26, 31,32,33]. Indeed, several dual and triple agonists have entered into clinical trials based on successful preclinical evaluations [34,35,36,37,38], albeit a profound polypharmacological knowledge of these unimolecular ligands is still required [39]. It is essential to understand how changes in peptide sequences affect signal propagation and receptor activation, as engagement of unimolecular agonists with a target receptor may alter the magnitude, timing and spectrum of intracellular signaling and engender modified functional outcomes compared to native or selective ligands. We recently demonstrated such functional differences for unimolecular agonists acting at GCGR and GLP-1R, or GIPR and GLP-1R [40, 41]. As such, it is clear that engineering peptides to enable their simultaneous engagement with multiple receptors also alters how they activate their cognate receptors. This is not surprising as biased agonism is commonly observed for GLP-1R, even with relatively minor changes to peptide sequence [42]. The exact spectrum of signaling and regulation within each of GLP-1R, GCGR and GIPR that will give rise to optimal clinical response is unknown but a key first step is to understand molecular details underlying differences in peptide pharmacology. Mutagenesis studies have been shown to provide a more nuanced molecular insight into the specific domains and amino acids in the 7TM pocket and adjacent extracellular loops (ECLs) that are important for biased agonism of ligands of an individual receptor, as has been illustrated for the GLP-1R [9, 14, 43, 44].
In this study, we compared the functional impacts of site-directed receptor mutagenesis on three dual agonists of GLP-1R and GCGR, peptide 15 [45], MEDI0382 [26, 46] and SAR425899 [35, 36], and a triple agonist, peptide 20 [47, 48] that also targets GIPR. The effects of mutation were assessed across two key signaling pathways, cAMP accumulation and ERK1/2 phosphorylation (pERK1/2), associated with GLP-1R and GCGR functioning and evaluated relative to GLP-1 and glucagon (included as study controls).
Materials and methods
Peptides
Human glucagon was purchased from ProsPec (Rehovot, Israel). All other peptides were synthesized by GL Biochem (Shanghai, China).
Cell culture and receptor expression
FlpIn-Chinese hamster ovary (CHO) cells were isogenically integrated with the wild-type (WT) or mutant GLP-1R or GCGR using Gateway technology (Invitrogen, Carlsbad, CA, USA), as described by Chang et al. [49]. Stable cells were grown in F12, Dulbecco’s modified Eagle’s medium (Gibco, ThermoFisher Scientific, Waltham, MA, USA) supplemented with 10% FBS (Gibco), 100 units/mL penicillin, 100 µg/mL streptomycin and 600 μg/mL hygromycin B (Invitrogen) and incubated in a humidified environment at 37 °C in 5% CO2.
Cell surface expression levels were verified by NovoCyte flow cytometer (FACS, ACEA Biosciences, San Diego, CA, USA). Surface expression levels were measured using the previously published procedure after cells were seeded (2 × 104 cells/well) into 6-well culture plates [49]. GLP-1R expressing cells were treated with mouse monoclonal anti-myc tag antibody (ab9106, 1:200, Abcam, Cambridge, UK) and Alexa Fluor 488-conjugated goat anti-mouse antibody (SA00013-2, 1:1000, Proteintech, Rosemont, USA). Primary and secondary antibodies for GCGR-expressing cells were anti-GCGR (ab137649, 1:100, Abcam) and anti-rabbit Alexa-488-conjugated antibodies (1:1000, Cell Signaling Technology, Danvers, MA, USA).
cAMP signaling assay
WT or mutant GLP-1R- or GCGR-transfected CHO cells were seeded at a density of 1.2 × 104 cells/well into 384-well culture plates and cultured overnight at 37 °C in a 5% CO2 environment. After discarding the medium, the cells were incubated with the assay buffer in the presence of 3-isobutyl-1-methylxanthine (IBMX) and different concentrations of agonists, as previously described [49]. On an EnVision plate reader (PerkinElmer, Boston, MA, USA), cAMP signals were detected using a LANCE cAMP detection kit (PerkinElmer). Absolute cAMP levels were calculated by interpolating signal counts into the cAMP standard curve. After that, the data were standardized to the response elicited by 100 µM forskolin (Sigma-Aldrich, St. Louis, MO, USA).
ERK1/2 phosphorylation signaling assay
CHO cells stably expressing WT or mutant GLP-1Rs or GCGRs were cultured (3 × 104 cells/well) overnight in 96-well plates at 37 °C in a 5% CO2 incubator. The cells were serum starved in FBS-free medium for at least 6 h prior to overnight incubation. To determine the peak response time point in the presence of a saturating concentration of agonist, pERK1/2 time course experiments were performed over a 20 min for each agonist. Concentration-response experiments were then carried out after stimulation with varying concentrations of each peptide over that peak time using the AlphaScreen SureFire ERK1/2 (p-Thr202/Tyr204) assay kit (PerkinElmer) as previously established [41]. The data were first normalized to the maximum response of 10% FBS stimulation for 7 min, and subsequently to the peak response of the WT.
Binding assay
CHO cells stably expressing WT or mutant GLP-1Rs or GCGRs were seeded into 96-well culture plates (5 × 104 cells/well) and incubated for 24 h at 37 °C in 5% CO2. After two washes and incubation for 2 h at 37 °C in blocking buffer (F12 with 0.1% BSA and 33 mM HEPES), the cells were treated with 125I–GLP-1 or 125I-glucagon (40 pM) (PerkinElmer) as well as increasing concentrations of unlabeled peptides. Following overnight incubation at 4 °C, cells were washed three times with ice-cold PBS and lysed in PBS with 1% Triton X-100 and 20 mM Tris-HCl. Fifty microliters of scintillation cocktail (PerkinElmer) were then added and the radioactivity (counts per minute, CPM) was counted on a MicroBeta2 microplate counter (PerkinElmer). Data were normalized to the response of WT and analyzed using a three-parameter logistic equation.
Data analysis
GraphPad Prism 8.0 (GraphPad, San Diego, CA, USA) was adopted to analyze curve fitting with a non-linear, three-parameter logistic equation to determine Emax (the maximal response for each peptide) and pEC50 (the negative logarithm of the calculated concentration of agonist that produces half the maximal response). The data were first normalized to the maximal response elicited by the controls (forskolin for cAMP and FBS for pERK1/2), and then to the maximal response of the WT receptor. The efficacy of each mutant was derived using the Black and Leff operational model of agonism [50] and then adjusted to directly measure transduction ratio (τ/KA) as previously reported [51]. This ratio is subsequently adjusted to the FACS-measured cell-surface expression level (c), yielding τ/KAc, with errors transmitted from both τ/KA and cell surface expression. These values were statistically compared relative to those of the WT receptor using a one-way analysis of variance and Dunnett’s post-test. Significance was accepted at P < 0.05.
Results
In this study, three GLP-1R/GCGR dual agonists, peptide 15 [45], MEDI0382 [26, 46] and SAR425899 [35, 36], with the latter two in clinical trials, and a GLP-1R/GCGR/GIPR triagonist peptide 20 [47, 48] together with GLP-1 and glucagon were assessed through site-directed mutagenesis at 32 residues of GLP-1R and GCGR, across competitive radiolabeled ligand binding profiles, cAMP and pERK1/2 pathways (Fig. 1 and Supplementary Fig. S1). These 32 residues locate at the extracellular half of TMs 1–3 and 5–7 and ECL2 that mainly recognize the peptide N terminus (within 5 Å), and several of them were found to be the determinants of biased signaling at glucagon family receptors in previous reports [7,8,9,10, 12,13,14] including R5.40bA and Q7.49bA. Wootten numbering system in superscript is used to label them illustrating the location and orientation relative to the conserved residue [14]. Of 32, 25 residues were mutated to alanine and 7 residues to non-alanine amino acids that are located on homologous sites of GLP-1R and GCGR. The effects of mutations were determined for each peptide, using an operational model of Black and Leff [50] to obtain the transduction ratio (log τ/KA), which was corrected to cell surface expression (log τ/KAc) to offset expression level differences of the mutants and compared to the WT receptor. Given that the previous pharmacology evaluation (cAMP signaling) of alanine mutations have been limited to two peptides (glucagon and peptide 15) and one receptor (GCGR [49]), it is better to compare the effects of mutations across different signaling pathways in a more systematic manner. This will allow us to determine functionally important residues in ligand binding and biased signaling, taking into the account of their biased profiles in WT GLP-1R and GCGR [41] (Figs. 2–10 and Supplementary Tables S1–S5).
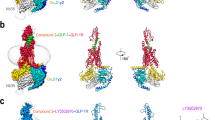
a Three distinct unimolecular dual agonists (Peptide 15, MEDI0382 and SAR425899) that target GLP-1R (blue) and GCGR (green), as well as a triple agonist (Peptide 20) that also targets GIPR (red), were assessed. b Single-letter peptide sequences of mono-, dual and triple agonists. The colored residues denoted the distinct amino acids in mono-agonist sequences, GLP-1 (blue), glucagon (GCG, green) and GIP (red). The peptides were modified in the following places. Aib aminoisobutyric acid, D-Ser D enantiomer of Ser, K* C16 fatty acid (palmitic acid) at the ε-amino group of lysine with a γ-glutamic acid spacer, K# lysine with a γE-C16 acyl linked through the side chain amine, NH2 C-terminal amide. c GLP-1R (PDB 6X18) structure was shown as cyan ribbon, with bound ligand in sandy brown. The location of homologous residues selected for mutation were highlighted in yellow. Pharmacological analyses (cell surface expression, cAMP accumulation and pERK1/2) were made to compare the effects of mutation on dual and triple agonist induced signaling responses relative to the controls (GLP-1 and GCG). This figure was created using BioRender.
Receptor expression values are the mean data from individual experiments performed in duplicate in CHO cells stably expressing the wild-type (WT) or mutant GLP-1Rs (a) or GCGRs (b). The results were presented as % WT and colored depending on the fold change in expression levels that were different from 100% of WT expression with 95% confidence intervals. Superscript numbers for mutant residues were based on the Wootten class B1 GPCR numbering scheme [14]. *P < 0.05 and **P < 0.001, statistical significance determined by one-way ANOVA followed by Dunnett’s test.
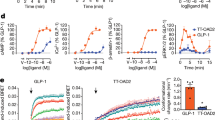
Concentration-response curves were generated in CHO cells stably expressing WT and mutant GLP-1 receptors for GLP-1 (a–d), peptide 15 (e–h), MEDI0382 (i–l), SAR425899 (m–p) and peptide 20 (q–t). The data were first converted to absolute cAMP levels, then normalized to the maximal response elicited by the WT GLP-1R and presented as % WT. The values were obtained in duplicate and fitted to a three-parameter logistic regression equation. The Wootten class B1 GPCR numbering scheme was used to assign superscript numbers to the mutant residues [14].
Concentration-response curves were generated in CHO cells stably expressing WT and mutant GLP-1 receptors. pERK1/2 responses were measured for GLP-1 (a–d), peptide 15 (e–h), MEDI0382 (i–l), SAR425899 (m–p) and peptide 20 (q–t). Data were normalized to the maximal response and then expressed as a percentage of the WT receptor. Values shown as means ± SEM from 4 (mutants) to 8 (WT) independent experiments were fitted to a three-parameter logistic regression equation. The Wootten class B1 GPCR numbering scheme was used to assign superscript numerals to mutant residues [14].
Signaling efficacies (log τ/KA) of cAMP accumulation and pERK1/2 were calculated using the operational model of Black and Leff [50] and corrected with the receptor expression level (log τ/KAc). Left and right panels show cAMP and pERK1/2 levels, respectively, upon stimulation by peptide 15, MEDI0382, SAR425899, peptide 20 and GLP-1. Compared to the wild-type (WT) receptor, mutants with significantly different mean values were color coded according to the fold change. Green dashed line represented the value of the WT receptor. ND, not determined due to poor signal or insufficient robustness to fit dose-response curve. Transmembrane domains (TMDs) are the vertical gray shaded divisions illustrated by numbers. The Wootten class B1 GPCR numbering scheme was used to assign superscript numerals to mutant residues [14]. One-way ANOVA with Dunnett’s post-test was used to determine the level of statistical significance.
The active state GLP-1R structure (PDB 6X18) was presented in tube helices with alanine mutated residues in a color-coded spherical format. Effects on cAMP (a–e) and pERK1/2 (f–j) responses evoked by GLP-1 (a, f), peptide 15 (b, g), MEDI0382 (c, h), SAR425899 (d, i) and peptide 20 (e, j) were presented. Chimera was used to visualize molecular images.
Concentration-response curves were generated in CHO cells stably expressing WT and mutant GCG receptors for GCG (a–d), peptide 15 (e–h), MEDI0382 (i–l), SAR425899 (m–p) and peptide 20 (q–t). The data were first converted to absolute cAMP levels, then normalized to the maximal response elicited by the WT GCGR and presented as % WT. The values were obtained in duplicate and fitted to a three-parameter logistic regression equation. The Wootten class B1 GPCR numbering scheme was used to assign superscript numbers to the mutant residues [14].
Concentration-response curves were generated in CHO cells stably expressing WT and mutant GCG receptors. pERK1/2 responses were measured for GCG (a–d), peptide 15 (e–h), MEDI0382 (i–l), SAR425899 (m–p) and peptide 20 (q–t). Data were normalized to the maximal response and then expressed as a percentage of the WT receptor. Values shown as means ± SEM from 4 (mutants) to 8 (WT) independent experiments were fitted to a three-parameter logistic regression equation. The Wootten class B1 GPCR numbering scheme was used to assign superscript numerals to mutant residues [14].
Signaling efficacies (log τ/KA) of cAMP accumulation and pERK1/2 were calculated using the operational model of Black and Leff [50] and corrected with the receptor expression level (log τ/KAc). Left and right panels show cAMP and pERK1/2 levels, respectively, upon stimulation by peptide 15, MEDI0382, SAR425899, peptide 20 and GCG. Compared to the wild-type (WT) receptor, mutants with significantly different mean values were color coded according to the fold change. Green dashed line represented the value of the WT receptor. ND, not determined due to insufficient signal that could be quantified. Transmembrane domains (TMDs) are the vertical gray shaded divisions illustrated by numbers. The Wootten class B1 GPCR numbering scheme was used to assign superscript numerals to mutant residues [14]. One-way ANOVA with Dunnett’s post-test was used to determine the level of statistical significance.
The active state GCGR structure (PDB 6LML) was presented in tube helices with alanine mutated residues in a color-coded spherical format. Effects on cAMP (a–e) and pERK1/2 (f–j) responses evoked by GCG (a, f), peptide 15 (b, g), MEDI0382 (c, h), SAR425899 (d, i) and peptide 20 (e, j) were presented. Chimera was used to visualize molecular images.
Effects of mutation on surface expression
Cell surface expression of WT and mutant GLP-1Rs and GCGRs were quantified by FACS (Fig. 2 and Supplementary Tables S2 and S4). Although there were some variabilities in the expression levels between experiments, a number of GLP-1R mutants drastically decreased surface expression, with the greatest reduction of K1972.67bI in TM2 and E3646.53bA in TM6 (<20% of WT), followed by moderate effects (20%–39% WT) for five mutants (Y1451.40bA, Y1521.47bA, R1902.60bA, K1972.67bA and E3877.42bD) (Fig. 2a and Supplementary Table S2). Twelve mutants had expression levels ranging from 40% to 80% (Y1451.40bQ, R1902.60bK, V1942.64bA, F2303.33bA, Q2343.37bA, V2373.40bI, N2403.43bA, W297ECL2A, R299ECL2S, N300ECL2A, R3105.40bA and H3636.52bA), and five (Y1481.43bA in TM1 and R3807.35bA, T3917.46bA, T3917.46bS and Q3947.49bA in TM7) were highly expressed (>150% of WT), with Y1481.43bA and Q3947.49bA being the most overexpressed mutants (increased by 1.14-fold and 1.64-fold, respectively). The remaining GLP-1R mutants were expressed similarly to the WT receptor (Fig. 2a and Supplementary Table S2). In comparison, GCGR mutants had less variation in expression levels. Except two mutants, Y1451.43bA and N2383.43bA, which lowered expression by 38% and 41%, respectively, the majority of them expressed at least 60% of the WT receptor (Fig. 2b and Supplementary Table S4).
Effects of mutation on cAMP accumulation
Upon agonist binding, GLP-1R and GCGR couple to heterotrimeric stimulatory G protein and activating adenylate cyclase to increase intracellular cAMP levels. pEC50 and Emax values of the four unimolecular agonists were determined at both mutant and WT GLP-1Rs and GCGRs. The cAMP responses of these agonists on WT receptors are consistent with our previous work [41]. Specifically, among the three dual agonists, SAR425899 exhibited a GLP-1R selectivity (pEC50 = 9.46 ± 0.03 vs. 10.30 ± 0.03) over GCGR (pEC50 = 7.21 ± 0.18 vs. 10.99 ± 0.03) relative to the native peptides (GLP-1 and glucagon), in agreement with an earlier report [35]. MEDI0382 displayed a slightly diminished potency, and peptide 15 showed an equivalent potency at both receptors (Figs. 3 and 7 and Supplementary Tables S2 and S4) compared to the native peptides [26, 45]. Likewise, the triple agonist peptide 20 was equipotent at the three receptors (Figs. 3 and 7 and Supplementary Tables S2 and S4) [47].
Effects of GLP-1R mutants
The functional impact of GLP-1R mutants on agonist-elicited cAMP accumulation demonstrated a similar trend shared by of the three dual agonists and GLP-1, after correction to cell surface expression of WT (Fig. 5 and Supplementary Table S3). Four mutants (W297ECL2A, N300ECL2A, R3105.40bA and H3636.52bA) were found to reduce the agonist potency (EC50) of GLP-1 and three dual peptides by over 1000-fold (Figs. 3c, g, k, o, 5, 6a–d and Supplementary Tables S2 and S3). R3807.35bA had a similar magnitude for GLP-1 and two dual peptides except MEDI0382, whose potency was reduced by 550-fold (Figs. 3d, h, p, 5, 6a, b, d and Supplementary Tables S2 and S3). Specifically, K1972.67bA and K1972.67bI showed a negative effect on GLP-1, MEDI0382 and SAR425899 potency of more than 400-fold (Figs. 3a, b, i, j, m, n, 5, 6a, c, d and Supplementary Tables S2 and S3), while that rendered by Y1481.43bA, F2303.33bA, Q2343.37bA and V2373.40bA on MEDI0382 and SAR425899 was significantly less (reduced by about 100-fold; Figs. 3i, j, m, n, 5, 6c, d and Supplementary Tables S2 and S3). In terms of peptide 20, W297ECL2A, R3105.40bA and H3636.52bA were able to reduce its potency by over 10-fold (Figs. 3s, 5, 6e and Supplementary Tables S2 and S3). Improved pEC50 values were seen with two mutants (Y1451.40bA and Y1451.40bQ) for GLP-1, peptide 15 and SAR425899 (Figs. 3a, e, m, 5, 6a, b, d and Supplementary Tables S2 and S3).
In TM1, the greatest reduction in EC50 was observed in Y1481.43bA for MEDI0382 (58-fold) and SAR425899 (105-fold) (Figs. 3i, m, 5, 6c, d and Supplementary Tables S2 and S3), while its impact on other peptides was minor (decreased by three-fold for peptide 15 and GLP-1, increased by two-fold for peptide 20; Figs. 3a, e, q, 5, 6a, b, e and Supplementary Tables S2 and S3). A similar phenomenon was seen in Y1521.47bA that moderately reduced the potencies of GLP-1, peptide 15, peptide 20, MEDI0382 and SAR425899 (about 3- to 39-fold), while Y1451.40bA and Y1451.40bQ showed little influence (Figs. 3a, e, i, m, q, 5, 6a–e and Supplementary Tables S2 and S3). In TM2, only GLP-1 reduced cAMP accumulation by 10- to 100-fold when R1902.60b was mutated to alanine or lysine (Figs. 3a, 5, 6a and Supplementary Tables S2 and S3). K1972.67bA failed to induce cAMP responses elicited by all the peptides except MEDI0382 that decreased cAMP signaling by more than 1000-fold relative to WT (Figs. 3i, 5, 6c and Supplementary Tables S2 and S3). Interestingly, K1972.67bI drastically reduced cAMP production caused by GLP-1 (7943-fold) compared to the other agonists with lower impact (Figs. 3b, 5, 6a and Supplementary Tables S2 and S3), indicative of a different peptide recognition mechanism. Meanwhile, Y2052.75bA had a greater impact for MEDI0382 (EC50 reduction by 112-fold) and SAR425899 (EC50 reduction by 513-fold) than the others (Figs. 3j, n, 5, 6c, d and Supplementary Tables S2 and S3).
In TM3, V2373.40bI exhibited an almost identical dose-response feature as WT for all peptides, while V2373.40bA reduced the agonist potency by 8- to 220-fold for four peptides except peptide 20 (Figs. 3b, f, j, n, r, 5, 6a–e and Supplementary Tables S2 and S3). Similar trends of potency reduction were observed for GLP-1, peptide 15, MEDI0382 and SAR425899 in mutants such as F2303.33bA (10- to 174-fold), M2333.36bA (3- to 35-fold) and Q2343.37bA (45- to 331-fold) (Figs. 3b, f, j, n, 5, 6a–d and Supplementary Tables S2 and S3). Notably, N2403.43bA selectively diminished GLP-1 potency by 8-fold but improved the potency for peptide 15 (2-fold), SAR425899 (2-fold) and MEDI0382 (3-fold) (Figs. 3b, f, j, n, 5, 6a–d and Supplementary Tables S2 and S3). As far as ECL2 is concerned, W297ECL2A and N300ECL2A both greatly reduced the potency of GLP-1 (by 4570-fold and 1047-fold), peptide 15 (by 5495-fold and 1071-fold), MEDI0382 (by 1819-fold and 1175-fold), SAR425899 (by 4571-fold and 1122-fold) and peptide 20 (by 26-fold and 2-fold), respectively (Figs. 3c, g, k, o, s, 5, 6a–e and Supplementary Tables S2 and S3). Another two mutants (R299ECL2A and R299ECL2S) also decreased the potencies of GLP-1 (by 66-fold and 17-fold), peptide 15 (by 13-fold and 14-fold), MEDI0382 (by 58-fold and 55-fold) and SAR425899 (by 20-fold and 61-fold), respectively, but not peptide 20 (Figs. 3c, g, k, o, 5, 6a–d and Supplementary Tables S2 and S3). Looking at TM5 and TM6, two mutants (R3105.40bA and H3636.52bA) diminished the potencies of all the peptides by over 1000-fold except peptide 20 (about 10-fold), while the effects of N3205.50bA on the former four peptides (except peptide 20) were weaker (Figs. 3c, g, k, o, 5, 6a–d and Supplementary Tables S2 and S3).
Of the eight mutations made in TM7, R3807.35bA, L3847.39bA and L3887.43bA displayed 25- to over 1000-fold potency reductions for GLP-1, peptide 15, MEDI0382 and SAR425899, except the 6-fold change of L3887.43bA for SAR425899 (Figs. 3d, h, l, p, 5, 6a–d and Supplementary Tables S2 and S3). While E3877.42bD only decreased GLP-1 potency by 29-fold, R3807.35bA profoundly affected pEC50 values of GLP-1 (6.74 ± 0.07), MEDI0382 (5.76 ± 0.04), peptide 15 (7.02 ± 0.06) and SAR425899 (6.22 ± 0.11), and the impact of L3847.39bA and L3887.43bA on the four peptides (except peptide 20) was less significant (Figs. 3d, h, l, p, 5, 6a–d and Supplementary Tables S2 and S3). The variation among the three dual agonists was mainly found in E3877.42bA and E3877.42bD. The former had no effect on the pEC50 values of GLP-1, MEDI0382 and SAR425899 while the latter caused significant changes when bound by GLP-1 and MEDI0382 (Figs. 3d, l, p, 5, 6a, c, d and Supplementary Tables S2 and S3). The remaining three mutants (T3917.46bA, T3917.46bS and Q3947.49bA) had similar or even improved signaling profiles for all the five agonists except that T3917.46bS and Q3947.49bA slightly reduced the efficacy (log τ/KAc) of peptide 15 (by 4-fold) and peptide 20 (by 5-fold), respectively (Figs. 3h, t, 5, 6b, e and Supplementary Tables S2 and S3). It follows that the residues showing the most pronounced effect on cAMP signaling are located in ECL2 and TMs 5-7 of W297ECL2A, R3105.40bA, H3636.52bA and R3807.35bA (Figs. 5 and 6).
Effect of GCGR mutants
A diverse pattern of agonist-induced cAMP responses was observed at the WT and 32 mutant GCGRs for three dual and one triple peptides. SAR425899 abrogated or insufficiently elicited cAMP signaling in 3 and 11 GCGR mutants, respectively, a reflection of its low potency at the WT receptor (pEC50 = 7.21 ± 0.18) compared to that of the WT GLP-1R (pEC50 = 9.46 ± 0.03) and consistent with our previous findings [41] (Figs. 7m–p, 9, 10d and Supplementary Tables S4 and S5). Specifically, W295ECL2A, R3085.40bA and R3787.35bA reduced the potencies of all peptides by over 700-fold, with the exception of R3085.40bA for peptide 20 (68-fold) (Figs. 7c, d, g, h, k, l, o, p, s, t, 9, 10a–e and Supplementary Tables S4 and S5). Y1451.43bA, Y1491.47bA, V1912.64bA, I1942.67bK, N298ECL2A, N3185.50bA, E3626.53bA, D3857.42bA and L3867.43bA decreased peptide 15 potency by over 100-fold, and only Y1451.43bA, N298ECL2A, N3185.50bA and L3867.43bA achieved the same for MEDI0382 and peptide 20 (Figs. 7e–i, k, l, q, s, t, 9, 10b, c, e and Supplementary Tables S4 and S5). Besides, K1872.60bR, S297ECL2R and S3897.46bA showed markedly enhanced pEC50 values for MEDI0382 (Figs. 7i, k, l, 9, 10c and Supplementary Tables S4 and S5).
The mutations in TM1 displayed a similar trend of impact for all the peptides, albeit to various extents. For example, Y1451.43bA reduced the agonist potencies by 116-, 238-, 101-, 95- and 142-fold for glucagon, peptide 15, MEDI0382, SAR425899 and peptide 20, respectively (Figs. 7a, e, i, m, q, 9, 10a–e and Supplementary Tables S4 and S5). As such, Y1491.47b A markedly decreased log τ/KAc (104-fold) of peptide 15 compared to WT, while that of the other peptides were moderately affected (51- to 57-fold), except SAR425899 that showed a notable right-shifted dose-response curve (Figs. 7e, m, 9, 10b, d and Supplementary Tables S4 and S5). Modest effects of Q1421.40bA on SAR425899 as well as Q1421.40bY on MEDI0382 and peptide 20 were recorded (Figs. 7i, m, q, 9, 10c–e and Supplementary Tables S4 and S5). All the agonists were affected by V1912.64bA and I1942.67bK in TM2, for instance, peptide 15 (524-fold, 879-fold), MEDI0382 (277-fold, 205-fold) and glucagon (198-fold, 375-fold), whereas I1942.67bA had a more profound reduction for glucagon (Figs. 7a, b, e, f, i, j, 9, 10a–c and Supplementary Tables S4 and S5). Substitution of K1872.60b by arginine slightly improved the potencies of peptide 15, MEDI0382 and SAR425899, while alanine mutation exhibited decreased potencies for all the five peptides (Figs. 7e, i, m, 9, 10b–d and Supplementary Tables S4 and S5).
In TM3, a greater reduction in log τ/KAc for SAR425899 at the six selected mutants was observed (Figs. 7n, 9, 10d and Supplementary Tables S4 and S5), while low to moderate reductions (4- to 54-fold) were associated with A2283.33bF, Q2323.37bA and N2383.43bA for all the peptides (Figs. 7b, f, j, n, r, 9, 10a–e and Supplementary Tables S4 and S5). In ECL2, S297ECL2R revealed an opposing activity for MEDI0382 (pEC50 improved by 12-fold) and SAR425899 (pEC50 decreased by 5-fold) while W295ECL2A had a negative impact on all the peptides (Figs. 7c, g, k, o, s, 9, 10a–e and Supplementary Tables S4 and S5). In TM5, R3085.40bA and N3185.50bA generally reduced the potencies of all the peptides relative to WT, especially R3085.40bA for peptide 15 (2754-fold), MEDI0382 (794-fold) and glucagon (708-fold) (Figs. 7c, g, k, 9, 10a–c and Supplementary Tables S4 and S5), in addition to the abolishment of SAR425899 efficacy by these mutants (Figs. 7o, 9, 10d and Supplementary Tables S4 and S5). In TM6, H3616.52bA reduced the cAMP activities of peptide 15, MEDI0382 and SAR425899 relative to glucagon (Figs. 7g, k, o vs. 7c, 9, 10a–d and Supplementary Tables S4 and S5), while E3626.53bA diminished the effect for all peptides (Figs. 7c, g, k, o, s, 9, 10 a–e and Supplementary Tables S4 and S5).
Of the 8 mutations made in TM7, R3787.35bA and L3867.43bA drastically reduced the activity (>100-fold) of all the agonists except SAR425899 (Figs. 7d, h, l, p, t, 9, 10a–e and Supplementary Tables S4 and S5). Two other mutants (L3827.39bA and D3857.42bA) only caused moderate decreases in agonist potencies ranging from 2- to 114-fold except L3827.39bA for SAR425899 (Figs. 7d, h, l, p, t, 9, 10a–e and Supplementary Tables S4 and S5). S3897.46bA, S3897.46bT and Q3927.49bA demonstrated similar dose-response characteristics as WT for all peptides except SAR425899 (Figs. 7d, h, l, p, t, 9, 10a–e and Supplementary Tables S4 and S5). Collectively, the residues showing the most pronounced effect on cAMP signaling are located in ECL2 and TMs 5–7 (Fig. 9 and Supplementary Table S5).
Effects of mutation on ERK1/2 phosphorylation
The peak time of GLP-1R and GCGR mediated pERK1/2 responses was found to be between 5–12 min following agonist stimulation (Supplementary Figs. S2 and S3). Like cAMP signaling, we observed similar patterns of pERK1/2 at the WT receptors elicited by mono-, dual and triple agonists, consistent with earlier reports [7, 41] but different from that transduced by the mutants (Supplementary Tables S2–S5).
Effect of GLP-1R mutants
Most mutants displayed similar pERK1/2 responses elicited by all the peptides compared to WT GLP-1R with different potencies. R1902.60bA, R1902.60bK, V2373.40bA, W297ECL2A, R3105.40bA and R3807.35bA for GLP-1, Y1481.43bA and R299ECL2S for peptide 15, Y2052.75bA for GLP-1, peptide 15 and SAR425899, T3917.46bS for peptide 15 and SAR425899, all lowered pERK1/2 signaling by over 10- to 1000-fold, whereas R1902.60bA enhanced that induced by MEDI0382 (32-fold) (Figs. 4a–i, n, p, 5, 6f–i and Supplementary Tables S2 and S3). The effects of Y1481.43bA, Y2052.75bA and R299ECL2S for peptide 15 as well as T3917.46bS for both peptide 15 and SAR425899 on pERK1/2 were more significant than that on cAMP accumulation (Figs. 4e–h, p vs. 3e–h, p, 5, 6g, i and Supplementary Tables S2 and S3). However, modest to non-measurable responses were seen in several mutants, such as K1972.67bA and H3636.52bA at GLP-1R in response to all the peptides (Figs. 4a, c, e, g, i, k, m, o, q, s, 5, 6f–j and Supplementary Tables S2 and S3). Additionally, ligand-specific abolishment was observed for GLP-1 (K1972.67bI), peptide 15 (R1902.60bK, K1972.67bI and W297ECL2A), MEDI0382 and SAR425899 (W297ECL2A) and peptide 20 (Y2052.75bA and W297ECL2A) (Figs. 4b, e–g, k, o, r, s, 5, 6f–j and Supplementary Tables S2 and S3).
In TM1, there was a moderate reduction (about 20-fold) in efficacy (log τ/KAc) at Y1481.43bA for peptide 15, while R1902.60bA and R1902.60bK in TM2 selectively decreased GLP-1-induced pERK1/2, but MEDI0382 was able to increase the response mediated via R1902.60bA by 32-fold (Figs. 4a, e, i, 5 and Supplementary Tables S2 and S3). Moreover, Y2052.75bA reduced the log τ/KAc of GLP-1, peptide 15 and SAR425899 (26-, 17- and 111-fold), respectively (Figs. 4b, f, n, 5, 6f, g, i and Supplementary Tables S2 and S3). Of the remaining mutants, V2373.40bA, R3105.40bA, R3807.35bA and W297ECL2A significantly reduced pERK1/2 induced by GLP-1 (39- to 72-fold), with W297ECL2A capable of abolishing pERK1/2 elicited by the other peptides (Figs. 4b–d, g, k, o, s, 5, 6f–j and Supplementary Tables S2 and S3). Besides, peptide 15 signaling was diminished by R299ECL2S (16-fold) and T3917.46bS (19-fold), and the latter also affected that of SAR425899 by 37-fold (Figs. 4g, h, p, 5, 6g, i and Supplementary Tables S2 and S3).
Effect of GCGR mutants
Similar to the protocol above, pERK1/2 was assessed at WT and mutant GCGRs with the same peak time window of 5–12 min (Figs. 8 and 9 and Supplementary Fig. S3). Marked reduction of pERK1/2 was seen in Y1491.47bA (by 48-fold), W295ECL2A (by 211-fold) and R3787.35bA (by 44-fold) upon glucagon stimulation while K1872.60bA and N3185.50bA completely abolished the response (Figs. 8a, c, d, 9, 10f and Supplementary Tables S4 and S5). The former two mutants reduced log τ/KAc of peptide 15 by 63- and 30-fold, respectively (Figs. 8e, g, 9, 10g and Supplementary Tables S4 and S5). Interestingly, K1872.60bA and N3185.50bA also blocked pERK1/2 elicited by the other four peptides, suggesting their important roles in GCGR signal transduction (Figs. 8e, g, i, k, m, o, q, s, 9, 10g–j and Supplementary Tables S4 and S5). Such a blockade of pERK1/2 by mutant GCGRs was readily seen with peptide 15 (V1912.64bA and R3787.35bA), MEDI0382 (V1912.64bA, A2283.33bF, M2313.36bA and W295ECL2A), SAR425899 (V1912.64bA, A2283.33bF, M2313.36bA, W295ECL2A, R3085.40bA, R3787.35bA and L3867.43bA) and peptide 20 (Y1491.47bA, A2283.33bF, W295ECL2A and N298ECL2A) (Figs. 8e, h, i–k, m–p, q–s, 9, 10g–j and Supplementary Tables S4 and S5). Another interesting mutant is Q2323.37bA, which has lower efficacies for peptide 15 (log τ/KAc = 6.16 ± 0.32), MEDI0382 (log τ/KAc = 5.59 ± 0.80) and peptide 20 (log τ/KAc = 6.96 ± 0.77), but only peptide 20 moderately reduced pERK1/2 at M2313.36bA (Figs. 8f, j, r, 9, 10g, h, j and Supplementary Tables S4 and S5). Additionally, Q1421.40bY, D3857.42bE and S3897.46bT showed reduced potency trend for MEDI0382 relative to WT (Figs. 8i, l, 9, 10h and Supplementary Tables S4 and S5). No significant alteration in pERK1/2 was noted among the remaining mutants for glucagon, dual and triple agonists (Fig. 9 and Supplementary Table S5).
Discussion
GLP-1R, GCGR and GIPR are three related peptide hormone receptors with important roles in glucose homeostasis and energy metabolism. Combinatorial agonism at them has shown great promises in the treatment of type 2 diabetes and obesity. Indeed, encouraging results were obtained in clinical trials of unimolecular dual and triple agonists showing superior human efficacy and safety profiles [22, 34,35,36,37,38]. Meanwhile, biased signaling, based on the fact that GPCRs may couple to different intracellular effectors to generate distinct physiological responses, has emerged as an alternative strategy for drug discovery. For example, oxyntomodulin, which acts on both GLP-1R and GCGR, was found to be biased toward pERK1/2 over cAMP relative to GLP-1 [52]. Therefore, it is important to investigate the dynamic nature of peptide-receptor interaction within the framework of unimolecular dual and triple agonists, where mutagenesis studies combined with pharmacological analyses would provide informative and thoughtful insights into the above two topics.
Closely related receptors have highly variable folding efficiencies. Defect in receptor folding and maturation may result in different cell surface expression level of GLP-1R vs. GCGR with homologous mutations [53] (Fig. 2). We employed an operational model to calculate the transduction ratio τ/KA, which is obtained from model fitting of concentration–response data and gives a composite measure of functional affinity and efficacy, useful to evaluate the effect of mutations on GLP-1R and GCGR signaling [14, 50, 54]. The transduction ratio can also be corrected for changes in cell surface receptor expression, allowing comparison of mutant effects even when the expression levels vary [51]. The GLP-1R/GCGR dual agonists were developed by introducing chemical modifications to glucagon aimed at enhancing potency or achieving co-agonism at both receptors. Of which, peptide 15 and MEDI0382 retrieve six residues (Q23GLP-1, A24GLP-1, K26GLP-1, E27GLP-1, I29GLP-1 and A30GLP-1) or two residues (A30GLP-1 and G35GLP-1) from GLP-1 (the superscript refers to amino acid in the native peptide sequence), respectively (Fig. 1b). SAR425899, a homolog of exendin-4, has 4 residues from GLP-1 (E21GLP-1, A24GLP-1, I29GLP-1 and G35GLP-1) (Fig. 1b). The first 12 residues of these peptides that form rich contacts with TMD have high similarities to GLP-1 or glucagon (Fig. 1b).
According to the peptide-bound GLP-1R, GCGR and GIPR structures, all peptides insert into the TMD orthosteric pocket along TM1 and TM2 with the formation of massive polar and nonpolar interactions [48, 55,56,57]. In this study, both Y1481.43bA and Y1521.47bA reduced cAMP signaling induced by the three dual agonists and GLP-1 but did not affect that elicited by peptide 20 (Figs. 3a, e, i, m, q, 5, 6a–e and Supplementary Tables S2 and S3). As shown in the recently reported GLP-1- or peptide 20-bound GLP-1R‒Gs structures [48, 55], Y1481.43b and Y1521.47b form a hydrogen bond and stacking interactions with E9GLP-1/Q3Peptide 20 that were further stabilized by R1902.60b and F12GLP-1/F6Pepetide 20, respectively. Obviously, these interactions could be abolished by both alanine and lysine substitutions (Figs. 3a, e, i, m, q, 5, 6a–e and Supplementary Tables S2 and S3). Similar to oxyntomodulin [11], Q3 of all the three dual agonists is likely to form hydrogen bonds with Y1521.47b and R1902.60b, and stacking interactions with Y1481.43b. As demonstrated by log τ/KAc, the latter interactions appear to be greater for MEDI0382 and SAR425899 relative to other peptides (Figs. 3i, m, vs. 3a, e, q, 5, 6a–e and Supplementary Tables S2 and S3). Likewise, the homologous residues at GCGR, Y1451.43bA, Y1491.47bA and K1872.60bA, showed a similar trend in cAMP signaling as they interact with Q3P and F6P in all the peptides (Figs. 1b, 7a, e, i, m, q, 9, 10a–e and Supplementary Tables S4 and S5). Unlike the alanine substitution at K1872.60b, the arginine substitution did not affect the potencies of the agonists, suggesting an essential role of the positively charged residue at this site (Figs. 9 and 10 and Supplementary Table S5). On the other hand, the potency of cAMP signaling mediated by the WT GCGR was lower for SAR425899 (about 100-fold weaker than that mediated by GLP-1R) and could not be measured at these mutants (Figs. 7m, 9, 10d and Supplementary Tables S4 and S5). Reflected by the peptide 15-bound GCGR structure [49], Y1491.47b was found to interact with Q3Peptide 15 that stabilizes the N terminus of peptide 15 in the TMD core besides the polar interactions between S8Peptide 15 and N298ECL2A. Similar interactions would likely be observed for these residues among other dual and triple agonists [48], as exemplified by marked reduction in cAMP signaling of glucagon and four other peptides (Figs. 9 and 10 and Supplementary Table S5). As far as pERK1/2 is concerned, mutations at 1.43b and 1.47b at both receptors produced negative results, even though the differences are not statistically significant in general, except Y1481.43bA for peptide 15 at GLP-1R and Y1491.47bA for glucagon and peptide 15 at GCGR (Figs. 4e, 5, 8a, e, 9 and Supplementary Tables S2–S5), and the effect of Y1491.47bA at GCGR was unmeasurable for peptide 20 (Figs. 8q and 9 and Supplementary Tables S4 and S5). The impact of Y2052.75bA at the top of TM2 in proximity of ECL1 was more pronounced on cAMP signaling induced by dual agonists vs. mono- and triple agonists (Figs. 3j, n vs. 3b, r, 5, 6a, c–e and Supplementary Tables S2 and S3), while a significant reduction in pERK1/2 elicited by GLP-1, peptide 15 and SAR425899 was observed at this mutant (Figs. 4b, f, n, 5, 6f, g, i and Supplementary Tables S2 and S3).
The N terminus His of the peptides (GLP-1 and oxyntomodulin) interacts with residues at 3.37b, 5.40b, 6.53b and 7.42b [11]; however, these interactions were more profound at E3626.53bA and D3857.42bA at GCGR for cAMP responses than the homologous residues at GLP-1R (Figs. 3, 5 vs. 7, 9 and Supplementary Tables S2–S5). Of which, alanine rather than glutamic acid or aspartic acid substitution at 7.42b unsurprisingly caused a larger reduction in peptide-TM7 interactions, as shown by E3877.42bD in GLP-1R and D3857.42bE in GCGR for cAMP signaling, thereby making the potency of dual agonists lower than that of alanine mutation although such a change was only statistically significant for D3857.42bA (Figs. 3, 5 vs. 7, 9 and Supplementary Tables S2–S5). Nonetheless, E3877.42bA and E3877.42bD at GLP-1R as well as D3857.42bA and D3857.42bE at GCGR did not affect pERK1/2 for the peptides studied with an exception of MEDI0382 that displayed a 50-fold decrease in log τ/KAc at GCGR mutant D3857.42bE (Figs. 8l, 9, 10h and Supplementary Tables S4 and S5). These differences may have resulted from sequence variation in the second position of peptides (serine for peptide 15, MEDI0382 and glucagon, α-aminoisobutyric acid for peptide 20 and D-serine for SAR425899) (Fig. 1b). Three key mutants that structurally reduced GLP-1 interactions and hence, cAMP accumulation are M2333.36bA, Q2343.37bA and E3877.42bD [8]. M2333.36bA and Q2343.37bA also negatively impacted cAMP signaling induced by the three dual agonists (Figs. 3f, j, n, 5, 6b–d and Supplementary Tables S2 and S3). The central polar network of GLP-1R is comprised of R2.60b, N3.43b, N5.50b, H6.52b, E6.53b and Q7.49b, which are highly conserved among class B1 GPCRs and located at the bottom of the peptide-binding pocket. It contributes constitutively to signal propagation [14, 58]. In line with previous reports [14], mutations of this network, e.g., K1972.67bA and H3636.52bA at GLP-1R and K1872.60bA and E3626.53bA at GCGR, weakened or disrupted both signaling pathways elicited by all the peptides studied (Figs. 3–5, 7–9 and Supplementary Tables S2–S5), albeit the effect of E3626.53bA on pERK1/2 was marginal (Figs. 8 and 9 and Supplementary Tables S4 and S5). In addition, K1972.67bI decreased cAMP responses induced by GLP-1 strongly, by MEDI0382 and SAR425899 moderately and by peptide 15 modestly (Figs. 3b, f, j, n, 5, 6a–d and Supplementary Tables S2 and S3). It had an equivalent effect to the WT GLP-1R when stimulated by peptide 20 (Figs. 3r, 5, 6e and Supplementary Tables S2 and S3). Both R1902.60bA and R1902.60bK only marginally influenced the potency of dual agonists but caused a large impact on cAMP and pERK1/2 responses induced by GLP-1 (Figs. 3a, 4a, 5, 6a, f and Supplementary Tables S2 and S3). The homologous residues at GCGR were found to act similarly on both pathways after stimulation by the peptides studied (Figs. 7–9 and Supplementary Tables S4 and S5). K1872.60bA reduced the potency while K1872.60bR did the opposite for all the peptides (Fig. 9 and Supplementary Table S5). However, substituting alanine rather than lysine at I1942.67b did not significantly reduce cAMP signaling (Figs. 7 and 9 and Supplementary Tables S4 and S5). This could be explained by (1) attractive or repulsive interaction between oppositely charged residues or (2) a hydrogen bond between R1902.60b and E3646.53b in GLP-1R, while the transient interaction between K1872.60b and E3626.53b in GCGR led to a preserved response [8, 10].
ECL2 is important for peptide recognition [43, 59]. W297ECL2A, R299ECL2A, R299ECL2S and N300ECL2A in GLP-1R significantly lowered cAMP responses elicited by the three dual agonists (Figs. 3g, k, o, 5, 6 and Supplementary Tables S2 and S3). A similar trend was seen for pERK1/2 mediated by these mutants, with reduced responses induced by GLP-1 at W297ECL2A and by peptide 15 at R299ECL2S being statistically significant (Figs. 4c, g, 5, 6f, g and Supplementary Tables S2 and S3). The homologous mutants (W295ECL2A and N298ECL2A) at GCGR drastically reduced cAMP signaling induced by the peptides studied (>100-fold), except N298ECL2A that showed a 34-fold decrease upon glucagon stimulation while S297ECL2A and S297ECL2R either exhibited an equal potency to WT or displayed variable activities exerted by SAR425899 or MEDI0382 in the case of S297ECL2R (Figs. 7, 9, 10 and Supplementary Tables S4 and S5). The impact on glucagon or peptide 15 induced pERK1/2 was only observed at W295ECL2A at GCGR (>10-fold reduction) (Figs. 8c, g, 9, 10f, g and Supplementary Tables S4 and S5). W297ECL2A, N300ECL2A and R3105.40bA caused the greatest reduction in cAMP responses induced by the dual agonists (Fig. 5 and Supplementary Table S3). W297ECL2A and R3105.40bA also reduced the efficacy of peptide 20 (Figs. 3s, 5, 6e and Supplementary Tables S2 and S3). Likewise, W295ECL2A, N298ECL2A, R3085.40bA and N3185.50bA at GCGR drastically lowered cAMP production regulated by the agonists assessed, except SAR425899 that neither induced observable responses even at 100 μM nor elicited measurable signals among the mutants (Figs. 7c, g, k, o, s and 9 and Supplementary Tables S4 and S5). R3105.40b and R3085.40b are the two conserved peptide-interaction sites in GLP-1R and GCGR, respectively, important for peptide-mediated Gs coupling [12, 13, 51, 59, 60]. R3105.40bA at GLP-1R reduced cAMP accumulation elicited by mono- and dual (>100-fold) as well as triple (about 10-fold) agonists (Figs. 3 and 5 and Supplementary Tables S2 and S3). Meanwhile, R3085.40bA at GCGR markedly decreased that induced by mono-, dual and triple agonists excluding SAR425899 ranging from 49- to 2089-fold (Figs. 7 and 9 and Supplementary Tables S4 and S5). However, such reductions were not observed for pERK1/2 (Figs. 5 and 9 and Supplementary Tables S3 and S5), consistent with previous report that Gs-mediated cAMP production is linked with the conformational dynamics in TM5 [51].
TM6, ECL3 and TM7 are highlighted as key regions for biased signaling [55]. All the dual agonists showed variable interactions with TM6 residues at both 6.52b and 6.53b of GCGR concerning cAMP production, with the exception of SAR425899 at the latter site (Figs. 7, 9, 10 and Supplementary Tables S4 and S5). For pERK1/2, interactions were reduced at 6.53b of GCGR among the dual agonists (Figs. 8–10 and Supplementary Tables S4 and S5). H3636.52bA in TM6 of GLP-1R substantially engaged all the peptides studied with regard to cAMP signaling but abolished pERK1/2 (Figs. 3–5 and Supplementary Tables S2 and S3). R3807.35bA at GLP-1R significantly reduced cAMP accumulation (over 100-fold) elicited by mono- and dual agonists but not peptide 20. Only GLP-1 induced pERK1/2 was significantly decreased by 68-fold, suggesting that the role of R3807.35b is differentiated between these two pathways (Figs. 3–5 and Supplementary Tables S2 and S3). The homologous mutation at GCGR, R3787.35bA, attenuated cAMP responses evoked by all the peptides, especially SAR425899 that showed a complete abolishment (Figs. 7 and 9 and Supplementary Tables S4 and S5). Indeed, the conserved receptor residue R7.35b forms multiple hydrogen bonds and salt bridges with the conserved peptide residues T5P and D9P.
In this study, we interrogated the potential mechanisms governing ligand binding, receptor activation and propagation of signaling pathways such as cAMP accumulation and ERK1/2 phosphorylation associated with multiplexed pharmacology and unimolecular dual and triple agonists of GLP-1R, GCGR and GIPR. Our findings provide valuable insights into biased agonism as well as the design of better therapeutic agents against multiple targets simultaneously.
References
Sekar R, Singh K, Arokiaraj AW, Chow BK. Pharmacological actions of glucagon-like peptide-1, gastric inhibitory polypeptide, and glucagon. Int Rev Cell Mol Biol. 2016;326:279–341.
Karageorgos V, Venihaki M, Sakellaris S, Pardalos M, Kontakis G, Matsoukas MT, et al. Current understanding of the structure and function of family B GPCRs to design novel drugs. Hormones. 2018;17:45–59.
Davenport AP, Scully CCG, de Graaf C, Brown AJH, Maguire JJ. Advances in therapeutic peptides targeting G protein-coupled receptors. Nat Rev Drug Discov. 2020;19:389–413.
Zhao LH, Yin Y, Yang D, Liu B, Hou L, Wang X, et al. Differential requirement of the extracellular domain in activation of class B G protein-coupled receptors. J Biol Chem. 2016;291:15119–30.
Hoare SR. Mechanisms of peptide and nonpeptide ligand binding to class B G-protein-coupled receptors. Drug Discov Today. 2005;10:417–27.
Pal K, Melcher K, Xu HE. Structure and mechanism for recognition of peptide hormones by class B G-protein-coupled receptors. Acta Pharmacol Sin. 2012;33:300–11.
Lei S, Clydesdale L, Dai A, Cai X, Feng Y, Yang D, et al. Two distinct domains of the glucagon-like peptide-1 receptor control peptide-mediated biased agonism. J Biol Chem. 2018;293:9370–87.
Yang D, de Graaf C, Yang L, Song G, Dai A, Cai X, et al. Structural determinants of binding the seven-transmembrane domain of the glucagon-like peptide-1 receptor (GLP-1R). J Biol Chem. 2016;291:12991–3004.
Wootten D, Reynolds CA, Smith KJ, Mobarec JC, Koole C, Savage EE, et al. The extracellular surface of the GLP-1 receptor is a molecular trigger for biased agonism. Cell. 2016;165:1632–43.
Siu FY, He M, de Graaf C, Han GW, Yang D, Zhang Z, et al. Structure of the human glucagon class B G-protein-coupled receptor. Nature. 2013;499:444–9.
Deganutti G, Liang YL, Zhang X, Khoshouei M, Clydesdale L, Belousoff MJ, et al. Dynamics of GLP-1R peptide agonist engagement are correlated with kinetics of G protein activation. Nat Commun. 2022;13:92.
Coopman K, Wallis R, Robb G, Brown AJ, Wilkinson GF, Timms D, et al. Residues within the transmembrane domain of the glucagon-like peptide-1 receptor involved in ligand binding and receptor activation: modelling the ligand-bound receptor. Mol Endocrinol. 2011;25:1804–18.
Dods RL, Donnelly D. The peptide agonist-binding site of the glucagon-like peptide-1 (GLP-1) receptor based on site-directed mutagenesis and knowledge-based modelling. Biosci Rep. 2015;36:e00285.
Wootten D, Simms J, Miller LJ, Christopoulos A, Sexton PM. Polar transmembrane interactions drive formation of ligand-specific and signal pathway-biased family B G protein-coupled receptor conformations. Proc Natl Acad Sci USA. 2013;110:5211–6.
Sloop KW, Emmerson PJ, Statnick MA, Willard FS. The current state of GPCR-based drug discovery to treat metabolic disease. Br J Pharmacol. 2018;175:4060–71.
Drucker DJ. Mechanisms of action and therapeutic application of glucagon-like peptide-1. Cell Metab. 2018;27:740–56.
Cho YM, Fujita Y, Kieffer TJ. Glucagon-like peptide-1: glucose homeostasis and beyond. Annu Rev Physiol. 2014;76:535–59.
Madsbad S. Review of head-to-head comparisons of glucagon-like peptide-1 receptor agonists. Diabetes Obes Metab. 2016;18:317–32.
Sharma D, Verma S, Vaidya S, Kalia K, Tiwari V. Recent updates on GLP-1 agonists: current advancements & challenges. Biomed Pharmacother. 2018;108:952–62.
Wootten D, Miller LJ, Koole C, Christopoulos A, Sexton PM. Allostery and biased agonism at class B G protein-coupled receptors. Chem Rev. 2017;117:111–38.
Baggio LL, Drucker DJ. Glucagon-like peptide-1 receptor co-agonists for treating metabolic disease. Mol Metab. 2021;46:101090.
Knerr PJ, Mowery SA, Finan B, Perez-Tilve D, Tschop MH, DiMarchi RD. Selection and progression of unimolecular agonists at the GIP, GLP-1, and glucagon receptors as drug candidates. Peptides. 2020;125:170225.
Scott RV, Bloom SR. Problem or solution: the strange story of glucagon. Peptides. 2018;100:36–41.
Galsgaard KD, Pedersen J, Knop FK, Holst JJ, Wewer Albrechtsen NJ. Glucagon receptor signaling and lipid metabolism. Front Physiol. 2019;10:413.
Filippi BM, Abraham MA, Yue JT, Lam TK. Insulin and glucagon signaling in the central nervous system. Rev Endocr Metab Disord. 2013;14:365–75.
Henderson SJ, Konkar A, Hornigold DC, Trevaskis JL, Jackson R, Fritsch Fredin M, et al. Robust anti-obesity and metabolic effects of a dual GLP-1/glucagon receptor peptide agonist in rodents and non-human primates. Diabetes Obes Metab. 2016;18:1176–90.
Finan B, Muller TD, Clemmensen C, Perez-Tilve D, DiMarchi RD, Tschop MH. Reappraisal of GIP pharmacology for metabolic diseases. Trends Mol Med. 2016;22:359–76.
Zhang Q, Delessa CT, Augustin R, Bakhti M, Collden G, Drucker DJ, et al. The glucose-dependent insulinotropic polypeptide (GIP) regulates body weight and food intake via CNS-GIPR signaling. Cell Metab. 2021;33:833–44.
NamKoong C, Kim MS, Jang BT, Lee YH, Cho YM, Choi HJ. Central administration of GLP-1 and GIP decreases feeding in mice. Biochem Biophys Res Commun. 2017;490:247–52.
Capozzi ME, DiMarchi RD, Tschop MH, Finan B, Campbell JE. Targeting the incretin/glucagon system with triagonists to treat diabetes. Endocr Rev. 2018;39:719–38.
Brandt SJ, Gotz A, Tschop MH, Muller TD. Gut hormone polyagonists for the treatment of type 2 diabetes. Peptides. 2018;100:190–201.
Jall S, Sachs S, Clemmensen C, Finan B, Neff F, DiMarchi RD, et al. Monomeric GLP-1/GIP/glucagon triagonism corrects obesity, hepatosteatosis, and dyslipidemia in female mice. Mol Metab. 2017;6:440–6.
Finan B, Ma T, Ottaway N, Müller TD, Habegger KM, Heppner KM, et al. Unimolecular dual incretins maximize metabolic benefits in rodents, monkeys, and humans. Sci Transl Med. 2013;5:209ra151.
Ambery PD, Klammt S, Posch MG, Petrone M, Pu W, Rondinone C, et al. MEDI0382, a GLP-1/glucagon receptor dual agonist, meets safety and tolerability endpoints in a single-dose, healthy-subject, randomized, phase 1 study. Br J Clin Pharmacol. 2018;84:2325–35.
Tillner J, Posch MG, Wagner F, Teichert L, Hijazi Y, Einig C, et al. A novel dual glucagon-like peptide and glucagon receptor agonist SAR425899: results of randomized, placebo-controlled first-in-human and first-in-patient trials. Diabetes Obes Metab. 2019;21:120–8.
Visentin R, Schiavon M, Gobel B, Riz M, Cobelli C, Klabunde T, et al. Dual glucagon-like peptide-1 receptor/glucagon receptor agonist SAR425899 improves beta-cell function in type 2 diabetes. Diabetes Obes Metab. 2020;22:640–7.
Parker VER, Robertson D, Wang T, Hornigold DC, Petrone M, Cooper AT, et al. Efficacy, safety, and mechanistic insights of cotadutide, a dual receptor glucagon-like peptide-1 and glucagon agonist. J Clin Endocr Metab. 2020;105:dgz047.
Frias JP, Bastyr EJ 3rd, Vignati L, Tschop MH, Schmitt C, Owen K, et al. The sustained effects of a dual GIP/GLP-1 receptor agonist, NNC0090-2746, in patients with type 2 diabetes. Cell Metab. 2017;26:343–52.
Anighoro A, Bajorath J, Rastelli G. Polypharmacology: challenges and opportunities in drug discovery. J Med Chem. 2014;57:7874–87.
Yuliantie E, Darbalaei S, Dai A, Zhao P, Yang D, Sexton PM, et al. Pharmacological characterization of mono-, dual- and tri-peptidic agonists at GIP and GLP-1 receptors. Biochem Pharmacol. 2020;177:114001.
Darbalaei S, Yuliantie E, Dai A, Chang R, Zhao P, Yang D, et al. Evaluation of biased agonism mediated by dual agonists of the GLP-1 and glucagon receptors. Biochem Pharmacol. 2020;180:114150.
Hager MV, Clydesdale L, Gellman SH, Sexton PM, Wootten D. Characterization of signal bias at the GLP-1 receptor induced by backbone modification of GLP-1. Biochem Pharmacol. 2017;136:99–108.
Koole C, Wootten D, Simms J, Miller LJ, Christopoulos A, Sexton PM. Second extracellular loop of human glucagon-like peptide-1 receptor (GLP-1R) has a critical role in GLP-1 peptide binding and receptor activation. J Biol Chem. 2012;287:3642–58.
Moon MJ, Lee YN, Park S, Reyes-Alcaraz A, Hwang JI, Millar RP, et al. Ligand binding pocket formed by evolutionarily conserved residues in the glucagon-like peptide-1 (GLP-1) receptor core domain. J Biol Chem. 2015;290:5696–706.
Day JW, Ottaway N, Patterson JT, Gelfanov V, Smiley D, Gidda J, et al. A new glucagon and GLP-1 co-agonist eliminates obesity in rodents. Nat Chem Biol. 2009;5:749–57.
Ambery P, Parker VE, Stumvoll M, Posch MG, Heise T, Plum-Moerschel L, et al. MEDI0382, a GLP-1 and glucagon receptor dual agonist, in obese or overweight patients with type 2 diabetes: a randomised, controlled, double-blind, ascending dose and phase 2a study. Lancet. 2018;391:2607–18.
Finan B, Yang B, Ottaway N, Smiley DL, Ma T, Clemmensen C, et al. A rationally designed monomeric peptide triagonist corrects obesity and diabetes in rodents. Nat Med. 2015;21:27–36.
Zhao F, Zhou Q, Cong Z, Hang K, Zou X, Zhang C, et al. Structural insights into multiplexed pharmacological actions of tirzepatide and peptide 20 at the GIP, GLP-1 or glucagon receptors. Nat Commun. 2022;13:1057.
Chang R, Zhang X, Qiao A, Dai A, Belousoff MJ, Tan Q, et al. Cryo-electron microscopy structure of the glucagon receptor with a dual-agonist peptide. J Biol Chem. 2020;295:9313–25.
Black JW, Leff P. Operational models of pharmacological agonism. Proc R Soc Lond B Biol Sci. 1983;220:141–62.
Yuliantie E, van der Velden WJC, Labroska V, Dai A, Zhao F, Darbalaei S, et al. Insights into agonist-elicited activation of the human glucose-dependent insulinotropic polypeptide receptor. Biochem Pharmacol. 2021;192:114715.
Koole C, Wootten D, Simms J, Valant C, Sridhar R, Woodman OL, et al. Allosteric ligands of the glucagon-like peptide 1 receptor (GLP-1R) differentially modulate endogenous and exogenous peptide responses in a pathway-selective manner: implications for drug screening. Mol Pharmacol. 2010;78:456–65.
Tao YX, Conn PM. Chaperoning G protein-coupled receptors: from cell biology to therapeutics. Endocr Rev. 2014;35:602–47.
Kenakin T, Christopoulos A. Signalling bias in new drug discovery: detection, quantification and therapeutic impact. Nat Rev Drug Discov. 2013;12:205–16.
Zhang X, Belousoff MJ, Zhao P, Kooistra AJ, Truong TT, Ang SY, et al. Differential GLP-1R binding and activation by peptide and non-peptide agonists. Mol Cell. 2020;80:485–500.
Qiao A, Han S, Li X, Li Z, Zhao P, Dai A, et al. Structural basis of Gs and Gi recognition by the human glucagon receptor. Science. 2020;367:1346–52.
Zhao F, Zhang C, Zhou Q, Hang K, Zou X, Chen Y, et al. Structural insights into hormone recognition by the human glucose-dependent insulinotropic polypeptide receptor. eLife. 2021;10:e68719.
Wootten D, Reynolds CA, Koole C, Smith KJ, Mobarec JC, Simms J, et al. A hydrogen-bonded polar network in the core of the glucagon-like peptide-1 receptor is a fulcrum for biased agonism: lessons from class B crystal structures. Mol Pharmacol. 2016;89:335–47.
Graaf C, Donnelly D, Wootten D, Lau J, Sexton PM, Miller LJ, et al. Glucagon-like peptide-1 and its class B G protein-coupled receptors: a long march to therapeutic successes. Pharmacol Rev. 2016;68:954–1013.
Liang YL, Belousoff MJ, Zhao P, Koole C, Fletcher MM, Truong TT, et al. Toward a structural understanding of class B GPCR peptide binding and activation. Mol Cell. 2020;77:656–68.
Acknowledgements
We are indebted to Elita Yuliantie for technical assistance and to Patrick M. Sexton and Denise Wootten for valuable advices. This work was partially supported by National Natural Science Foundation of China 81872915 (MW), 82073904 (MW), 82121005 (DY), 81973373 (DY) and 21704064 (QZ); National Science & Technology Major Project of China—Key New Drug Creation and Manufacturing Program 2018ZX09735–001 (MW) and 2018ZX09711002–002–005 (DY); National Science & Technology Major Project of China—Innovation 2030 for Brain Science and Brain-Inspired Technology 2021ZD0203400 (QZ); the National Key Basic Research Program of China 2018YFA0507000 (MW); Novo Nordisk-CAS Research Fund grant NNCAS-2017–1-CC (DY) and SA-SIBS Scholarship Program (DY).
Author information
Authors and Affiliations
Contributions
MW and DY supervised the research; SD, RC, YC and AD performed experiments; SD, RC and DY analyzed data; SD, QZ and MW wrote the paper with inputs from all the co-authors.
Corresponding authors
Ethics declarations
Competing interests
The authors declare no competing interests.
Supplementary information
Rights and permissions
Springer Nature or its licensor holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Darbalaei, S., Chang, Rl., Zhou, Qt. et al. Effects of site-directed mutagenesis of GLP-1 and glucagon receptors on signal transduction activated by dual and triple agonists. Acta Pharmacol Sin 44, 421–433 (2023). https://doi.org/10.1038/s41401-022-00962-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41401-022-00962-y