Abstract
Aim/hypothesis
The physiological counterregulatory response to hypoglycaemia is reported to be organised hierarchically, with hormone responses usually preceding symptomatic awareness and autonomic responses preceding neuroglycopenic responses. To compare thresholds for activation of these responses more accurately between people with or without type 1 diabetes, we performed a systematic review on stepped hyperinsulinaemic–hypoglycaemic glucose clamps.
Methods
A literature search in PubMed and EMBASE was conducted. We included articles published between 1980 and 2018 involving hyperinsulinaemic stepped hypoglycaemic glucose clamps among people with or without type 1 diabetes. Key exclusion criteria were as follows: data were previously published; other patient population; a clamp not the primary intervention; and an inadequate clamp description. Glycaemic thresholds for counterregulatory hormone and/or symptom responses to hypoglycaemia were estimated and compared using generalised logrank test for interval-censored data, where the intervals were either extracted directly or calculated from the data provided by the study. A glycaemic threshold was defined as the glucose level at which the response exceeded the 95% CI of the mean baseline measurement or euglycaemic control clamp. Because of the use of interval-censored data, we described thresholds using median and IQR.
Results
A total of 63 articles were included, whereof 37 papers included participants with type 1 diabetes (n=559; 67.4% male sex, aged 32.7±10.2 years, BMI 23.8±1.4 kg/m2) and 51 papers included participants without diabetes (n=733; 72.4% male sex, aged 31.1±9.2 years, BMI 23.6±1.1 kg/m2). Compared with non-diabetic control individuals, in people with type 1 diabetes, the median (IQR) glycaemic thresholds for adrenaline (3.8 [3.2–4.2] vs 3.4 [2.8–3.9 mmol/l]), noradrenaline (3.2 [3.2–3.7] vs 3.0 [2.8–3.1] mmol/l), cortisol (3.5 [3.2–4.2]) vs 2.8 [2.8–3.4] mmol/l) and growth hormone (3.8 [3.3–3.8] vs. 3.2 [3.0–3.3] mmol/l) all occurred at lower glucose levels in people with diabetes than in those without diabetes (all p≤0.01). Similarly, although both autonomic (median [IQR] 3.4 [3.4–3.4] vs 3.0 [2.8–3.4] mmol/l) and neuroglycopenic (median [IQR] 3.4 [2.8–N/A] vs 3.0 [3.0–3.1] mmol/l) symptom responses were elicited at lower glucose levels in people with type 1 diabetes, the thresholds for autonomic and neuroglycopenic symptoms did not differ for each individual subgroup.
Conclusions/interpretation
People with type 1 diabetes have glycaemic thresholds for counterregulatory hormone and symptom responses at lower glucose levels than people without diabetes. Autonomic and neuroglycopenic symptoms responses are generated at about similar levels of hypoglycaemia. There was a considerable variation in the methodology of the articles and the high insulin doses in most of the clamps may affect the counterregulatory responses.
Funding
This article has received funding from the Innovative Medicines Initiative 2 Joint Undertaking (JU) under grant agreement no. 777460.
Registration
This systematic review is registered in PROSPERO (CRD42019120083).
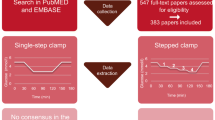
Graphical abstract

Similar content being viewed by others

Introduction
Iatrogenic hypoglycaemia is a continuous threat for most people with type 1 diabetes, occurring weekly or even daily as a consequence of treatment with insulin [1]. Falling glucose levels in the hypoglycaemic range elicit a hierarchically organised counterregulatory response, starting with the suppression of insulin production by beta cells, followed by the release of hormones (glucagon, adrenaline, noradrenaline, cortisol and growth hormone) and finally the appearance of (warning) symptoms to induce a behavioural response (i.e. ingest carbohydrates), aimed at restoring glucose levels. Overall, it is generally considered that hypoglycaemia first elicits autonomic symptoms, hence termed warning symptoms, followed by neuroglycopenic symptoms, usually thought to reflect cerebral glucopenia [2].
The hyperinsulinaemic clamp is a methodology that has been widely employed to study the impact of varying degrees of hypoglycaemia in counterregulatory responses and used to determine the threshold for activation of the individual components [3, 4]. With this method, insulin is infused intravenously at a constant rate sufficient to cause plasma glucose levels to fall, alongside a variable intravenous glucose infusion titrated against frequent glucose measurements to achieve hypoglycaemia at predefined glucose plateaus. During each plateau, counterregulatory hormone concentrations and symptom scores are measured to define the glucose level at which a response can be first detected.
Although reported to be organised hierarchically, the glycaemic thresholds at which these responses occur are not fixed, showing inter- and intra-individual variability, and are influenced by prior exposure to hypo- and hyperglycaemia, as well as by age and duration of diabetes [5, 6]. In addition, factors such as the inability to dissipate insulin, blunted glucagon secretion and reduced catecholaminergic responses in people with type 1 diabetes [7] can influence each component of the counterregulatory hormone and symptom response and so thresholds may differ between those with and without type 1 diabetes. Whether in type 1 diabetes per se, glycaemic thresholds differ from those in people without diabetes remains to be determined. To explore the glycaemic thresholds for counterregulatory hormone and symptom responses, we performed a systematic review on hyperinsulinaemic stepped hypoglycaemic glucose clamps reporting counterregulatory and/or symptom responses in people with or without type 1 diabetes.
Methods
The search string and selection of publications for this systematic review have been published previously [8]. See electronic supplementary material (ESM Methods) for the search strategy. The protocol is published in PROSPERO (CRD42019120083): https://www.crd.york.ac.uk/prospero/display_record.php?RecordID=120083. All articles with stepped clamps from the systematic review were included in this article. Only English-language articles were included.
Data sources and search strategy
A literature search was conducted in PubMed and EMBASE in November 2018. All articles available online in the databases and published from 1980 to 2018 were included. The search used a combination of free text words, MeSH (PubMed), and Emtree (EMBASE) terms. All titles and abstracts identified from the electronic search via PubMed and EMBASE were imported to COVIDENCE [8] software, version 1.0, which streamlines the review process. The search strategy (ESM Methods) was developed in collaboration with an information specialist at Nordsjællands Hospital, Denmark, with input from clinicians and academics in the review team. Details on study selection have been published previously [4]. To obtain additional data missing in the articles, we contacted the corresponding authors.
Data extraction
A total of 3887 articles were identified, 547 full-text articles were assessed for eligibility and 383 were included in the systematic review [4]. Out of these 383 articles, 108 reported a stepped hyperinsulinaemic–hypoglycaemic glucose clamp in people with type 1 diabetes and/or people without diabetes. People were classified as having a reduced awareness of hypoglycaemia when it was stated by the paper or when they had a history of severe hypoglycaemic events. Articles were included if they provided data about glycaemic thresholds or when it was possible to calculate these. Forty-five articles were excluded due to lack of information, resulting in 63 articles being included in the systematic review (ESM Table 1) [3, 6, 9,10,11,12,13,14,15,16,17,18,19,20,21,22,23,24,25,26,27,28,29,30,31,32,33,34,35,36,37,38,39,40,41,42,43,44,45,46,47,48,49,50,51,52,53,54,55,56,57,58,59,60,61,62,63,64,65,66,67,68,69]. Of these, the glycaemic thresholds were provided in 47 papers, and 17 contained sufficient data (mean±SD of baseline and every step) to calculate these for at least one counterregulatory hormone (i.e. glucagon, adrenaline, noradrenaline, cortisol and/or growth hormone) or for symptom responses. In one of the included articles, the glycaemic threshold was provided for some of the counterregulatory hormones and calculated for others. Of the 47 articles that provided the glycaemic thresholds, 42 articles determined the thresholds based on the 95% CI, and three articles used ANOVA. In two articles, information on how glycaemic thresholds were determined was missing. Of the 42 papers that based the glucose thresholds on 95% CI, 17 articles did this on the basis of exceeding the 95% CI of data derived from euglycaemic control experiments and 23 papers of data derived from baseline measurements. Two additional papers used a euglycaemic control clamp and although those two papers did not mentioned whether the data were derived from the control clamp or from baseline measurements, we assumed that the data derived from the control clamp. We used the glucose values of the clamped phases below and above the provided or calculated glycaemic threshold for the survival analysis (see Statistics). For example, when a paper used the glucose steps 4.0, 3.0 and 2.5 mmol/l and found the threshold for adrenaline to be at a glucose level of 3.5 mmol/l, the glucose steps 4.0 and 3.0 mmol/l were included in the survival analysis. For people with type 1 diabetes, thresholds for glucagon responses were excluded because a response was often absent or not provided (n=58). Symptom scores were classified as autonomic (sweating, anxiety, tremor, palpitations, feeling hot and tingling) or neuroglycopenic (difficulty speaking, confusion, dizziness, irritability, blurred vision and drowsiness). See the Preferred Reporting Items for Systematic Review and Meta-Analyses (PRISMA) flow diagram for an overview of the process (ESM Fig. 1). Quality assessment was ensured by two reviewers extracting information, and by crosschecking of all the included articles. In studies where glucose measurements were derived from whole blood, these were converted to plasma glucose values, assuming plasma glucose levels to be 11.1% higher than whole blood measurements [70].
Statistics
Results are shown with standard descriptive statistical methods. Continuous data are shown as means with SD, which for readability reasons applies to both normal and non-normal distributed data. We used data provided by the articles on both the glucose value below and the glucose value above the determined glycaemic thresholds (i.e. interval-censored data). When these were not provided by the article, we calculated these values from the plasma glucose level at which the counterregulatory hormone or symptom response first exceeded the 95% CI of the mean baseline measurement. When needed, we determined the 95% CI from the provided sample size. As the thresholds are not known by their value, but only up to the interval in which they are censored, statistical methods such as t tests and linear regression are not applicable. Methods to deal with interval-censored data have been developed in a survival data context and use survival data terminology [71]. Therefore, we described thresholds using median and IQR, and used logrank tests to compare the thresholds in people with or without diabetes and people with normal awareness of hypoglycaemia or impaired awareness of hypoglycaemia. We assessed a potential effect of HbA1c and diabetes duration on glucose thresholds by including these variables as explanatory variables in Cox regression analyses for interval-censored data. Note that we apply these interval-censored survival data techniques such that the ‘event’ is the occurrence of a threshold and, instead of ‘follow-up’ time that increases until the ‘event’ has happened we have the glucose level increasing until a threshold has occurred. A level of statistical significance was set to 5% (two-sided). Statistical analyses were performed using IBM SPSS Statistics for Windows, version 25 (IBM Corp., Armonk, NY, USA) and SAS 9.4 (SAS Institute, Cary, NC, USA).
Results
The 63 included studies involved 1332 participants with a median of 16 participants (range 6–90) per study, of which 11 exclusively enrolled people with type 1 diabetes, 26 only participants without diabetes, and 26 included both. The participants were generally young, had a normal BMI, and were more often male than female (Table 1).
The hypoglycaemic clamps were designed with a variable number of steps, with the most frequently used number of steps after the normoglycaemic phase being four (n=27, 43%) and three (n=18, 29%). In the four-step clamps, the mean achieved plasma glucose levels were 4.4±0.1 mmol/l, 3.7±0.1 mmol/l, 3.1±0.1 mmol/l and 2.5±0.1 mmol/l, respectively. For the three-step clamps, the mean achieved plasma glucose levels were 4.6±0.4 mmol/l, 3.7±0.1 mmol/l and 3.0±0.1 mmol/l. Twenty-six articles used whole blood to measure blood glucose values and 37 measured glucose values in plasma.
Glycaemic thresholds for counterregulatory hormone responses
All but one [6] of the studies (98%) provided data to either calculate or extract the glycaemic threshold for counterregulatory hormone responses to hypoglycaemia. The median (IQR) glycaemic threshold for the glucagon response in people without diabetes was 3.8 (3.0–3.8) mmol/l. The glycaemic thresholds for eliciting hormone responses all occurred at lower glucose levels in people with diabetes than in those without diabetes (all p<0.01, Figs 1, 2): 3.8 (3.2–4.2) vs 3.4 (2.8–3.9) mmol/l for adrenaline; 3.2 (3.2–3.7) vs 3.0 (2.8–3.1) mmol/l for noradrenaline; 3.5 (3.2–4.2) vs 2.8 (2.8–3.4) mmol/l for cortisol and 3.8 (3.3–3.8) vs 3.2 (3.0–3.3) mmol/l for growth hormone. This was also true when the analysis was restricted to the studies that examined both people with type 1 diabetes and healthy control individuals (ESM Fig. 2). There were no differences between studies using vs not using euglycaemic control experiments (ESM Fig. 3). Neither the duration of diabetes nor the level of glycaemic control (as measured by HbA1c) was associated with the glycaemic threshold level for any of the measured hormones (ESM Table 2).
The glycaemic thresholds for the release of the counterregulatory hormones adrenaline (a; p=0.007), noradrenaline (b; p<0.001), cortisol (c; p<0.001) and growth hormone (d; p<0.001), and for eliciting autonomic (e; p=0.01) and neuroglycopenic (f; p=0.007) symptomatic responses are shown in non-parametric complementary cumulative distribution curves (‘survival’ curves). The p values refer to the comparison of curves of people with type 1 diabetes and without diabetes with a generalised logrank test for interval-censored survival curves. The values on the vertical axis show the probability that the threshold is larger than the corresponding value on the glucose level axis (horizontal axis)
Glycaemic thresholds for symptom responses
A total of 25 studies (40%) provided data to either calculate or extract the glycaemic threshold for symptom responses to hypoglycaemia [6, 13, 16,17,18, 20, 23, 24, 26, 29, 31, 33,34,35,36,37, 46, 51,52,53, 56, 57, 58, 63, 68]. The median (IQR) glycaemic threshold for the appearance of autonomic symptoms was 3.4 (3.4–3.4) mmol/l in those without diabetes and 3.0 (2.8–3.4) mmol/l in people with type 1 diabetes (p=0.01). Similarly, the glycaemic thresholds for the appearance of neuroglycopenic symptoms averaged 3.4 (2.8–N/A) mmol/l and 3.0 (3.0–3.1) mmol/l in people without and with type 1 diabetes, respectively (p=0.007) (Figs 1, 2). There were no differences between studies using or not using euglycaemic control experiments, except for a small but significant difference in the neuroglycopenic symptoms in people with diabetes, where the curves of the euglycaemic control experiments were at a lower glucose levels (p=0.003; ESM Fig. 3). Glycaemic thresholds did not differ between autonomic and neuroglycopenic symptoms, either in people with diabetes or in those without diabetes. Restricting the analysis to studies that included both people with type 1 diabetes and healthy control individuals or to studies without cognitive function tests (which could potentially alert participant awareness for neuroglycopenic symptoms) did not materially change this. Neither the duration of diabetes nor the level of glycaemic control (as measured by HbA1c) was associated with the glycaemic threshold level for symptom responses in people with diabetes (ESM Table 2).
Sensitivity analyses of awareness of hypoglycaemia status
Based on 13 of the articles that included people with impaired awareness status, the curves in the graph for glycaemic thresholds were mostly at lower glucose levels in people with impaired hypoglycaemic awareness (vs those without): 3.0 (3.0–3.0 mmol/l) vs 3.5 (2.8–3.9 mmol/l) for adrenaline; 2.6 (2.6–N/A mmol/l) vs 3.1 (2.8–3.1 mmol/l) for noradrenaline; and N/A (2.6–N/A) vs 3.3 (3.2–3.7 mmol/l) for growth hormone. This difference did not reach statistical significance for cortisol (2.8 [2.5–3.0 mmol/l] vs 3.3 [2.8–3.4 mmol/l]) (ESM Fig. 4). In addition, for autonomic and neuroglycopenic symptom generation, glucose levels were lower in people with impaired awareness; this difference was only significant for autonomic symptoms (N/A [N/A–N/A mmol/l] vs 3.3 [3.3–3.4 mmol/l], p<0.001) and not for neuroglycopenic symptoms (3.0 [3.0–N/A mmol/l] vs 3.0 [3.0–N/A] mmol/l, p=0.448) (ESM Fig. 4).
Sensitivity analyses of glycaemic threshold in three- and four-step clamps
When we restricted the analyses to either the three-step or four-step clamps alone, the differences in glycaemic thresholds between people with vs without diabetes for adrenaline, noradrenaline, cortisol and growth hormone remained largely unchanged (Table 2). The same was true for the glycaemic thresholds for autonomic and neuroglycopenic symptom perception (Table 2). Additionally, when comparing the glycaemic thresholds for counterregulatory responses in three- and four-step clamps separately for each subgroup (participants with type 1 diabetes and healthy participants), there were numerical but no statistically significant differences (Table 2).
Discussion
This systematic review shows that in people without diabetes, the glycaemic thresholds for release of counterregulatory hormone responses ranged between 3.2 and 3.8 mmol/l, with upper limits of the IQR as high as 4.2 mmol/l, whereas lower glucose levels were required to elicit symptoms of hypoglycaemia. Compared with non-diabetic control individuals, the release of counterregulatory hormones and generation of symptoms occurred at lower glucose levels in people with type 1 diabetes, in part dependent on awareness status but independent of HbA1c and duration of diabetes. In both the subgroup with and the subgroup without type 1 diabetes, glycaemic thresholds for the emergence of autonomic or neuroglycopenic symptoms were about similar within each subgroup.
Based on hypoglycaemic glucose clamp studies dating back to the 1980s, it is commonly assumed that the physiological response to hypoglycaemia in healthy people occurs at glucose levels below 3.9 mmol/l, with the release of glucagon and adrenaline, whereas glucose levels below 3.3–3.5 mmol/l are reported to trigger symptomatic awareness [72]. The current analysis, which collectively combines data from a large number of individual clamp studies involving more than 1300 individuals, shows that on average much lower glucose levels are required to elicit an acute counterregulatory hormone response and symptom response in both people with type 1 diabetes and in those without diabetes (except for the adrenaline response in people without diabetes). As for glycaemic thresholds for autonomic and neuroglycopenic symptoms in people without diabetes, these appear to be elicited at glucose levels of 3.0–3.4 mmol/l and 3.1–3.7 mmol/l, respectively.
In people with type 1 diabetes, we observed glycaemic thresholds at 0.2–0.7 and 0.4 mmol/l lower glucose levels for counterregulatory hormone and symptom responses, respectively, compared with people without diabetes, although with a wide range, suggesting greater variability in those with type 1 diabetes. This large variability in glycaemic thresholds in type 1 diabetes can probably be explained by different prior hypoglycaemia exposure rates between individuals [7], the loss of glucagon secretion within years after diagnosis [9, 10], blunted catecholamine responses and impaired hypoglycaemic awareness [11, 12]. Indeed, we found clear suggestions of glycaemic thresholds for release of particularly adrenaline and appearance of autonomic symptoms to occur at lower glucose levels in people with impaired awareness of hypoglycaemia. These data are in line with studies showing that prior exposure to recurrent hypoglycaemia, which often is the rule in people with impaired awareness, shifts the glycaemic thresholds for counterregulatory responses to lower glucose levels [6, 15].
We found no evidence that strict glycaemic control had an impact on glycaemic thresholds. This is important, since strict glycaemic control, as reflected by low HbA1c, is sometimes viewed as a proxy for greater exposure to hypoglycaemia and higher HbA1c as the opposite. Our data underscore, however, that merely directing people with type 1 diabetes to allow their HbA1c to increase is not expected to alter glycaemic thresholds or the associated burden of hypoglycaemia unless the rate of hypoglycaemia drops considerably [6, 32, 60].
Remarkably, we found no evidence for different glycaemic thresholds for the appearance of autonomic or neuroglycopenic symptoms, neither in people with type 1 diabetes nor in those without. These results contrast with the commonly held assumption that the appearance of hypoglycaemic symptoms is hierarchically organised [13, 14]. One explanation for this apparent discrepancy may be the more immediate recognition of autonomic (e.g. sweating and palpitations) as compared with neuroglycopenic (e.g. difficulty in thinking or speaking) symptoms, unless engaged in something requiring information processing, so that the first is usually mentioned as initial symptoms. Additionally, focusing on autonomic symptoms when educating people with diabetes about hypoglycaemia may reinforce such assumptions whereas in fact such a hierarchy in symptomatology seemingly does not exist.
We could not investigate the glycaemic threshold for the glucagon response in people with diabetes. Most studies did not report on glycaemic thresholds for this response to hypoglycaemia in participants with type 1 diabetes, whereas those that did described a large variety in thresholds, including absent responses. In addition, it is possible that some studies did not reach glucose levels that were sufficiently low to elicit a glucagon response. Although the glucagon response is probably retained in adults with a short duration of type 1 diabetes, contributing to their often good glycaemic control combined with low hypoglycaemia risk [15, 16], it is almost universally lost within the first few years after diagnosis [14, 15]. This observation has been linked to progressive loss of pancreatic beta cells, which are thought to control alpha cell responses to hypoglycaemia [73]. Additionally, reliable measurement of glucagon was problematic at the time when most of the studies were performed. However, this should not distract from the fact that in human physiology, the glucagon response plays a prominent role in glucose counterregulation.
In this systematic review, the calculation of glucose thresholds depended on the predefined glucose steps of the studies that were included in the survival curve analysis for interval-censored data. We included both the glucose level of the first counterregulatory response and the level prior to it to obtain a more realistic ‘glycaemic threshold value’. However, it could still be argued whether a stepped clamp is the optimal study design to determine glycaemic thresholds for counterregulatory responses to hypoglycaemia or whether gradually lowering glucose levels would be more precise for defining these cut-off values. Nevertheless, two studies dating back to the 1990s that used such a gradual glucose-lowering method to assess glycaemic thresholds in children with type 1 diabetes reported results that were in line with our findings [17, 18].
Age and diabetes duration did not influence the glycaemic thresholds, which contrasts with previous studies that showed that older age and longer diabetes duration were associated with altered counterregulatory hormone and symptom responses [19,20,21]. There are two explanations for this apparent discrepancy. First, the mentioned loss of the glucagon response, usually occurring within 5 years after diabetes diagnosis, and the resultant greater exposure to hypoglycaemia may lead to a ‘sudden’ shift of glycaemic thresholds for counterregulatory responses to lower glucose levels [74]. Indeed, those with retained beta cell function are at lower risk of hypoglycaemia than those who have completely lost beta cell function [75]. The studies analysed in this review included relatively few participants with very short or very long duration of diabetes and also the age range was rather narrow, which limited our ability to detect an effect of diabetes duration or age. Second, it is also possible that age and/or diabetes duration affect the magnitude of counterregulatory responses to hypoglycaemia, rather than the glycaemic thresholds.
A strength of this systematic review is that the large number of participants provided more precision to estimate glycaemic thresholds for counterregulatory responses to hypoglycaemia with sufficient accuracy in both people with type 1 diabetes and people without diabetes. There are also limitations. First, the calculation of glycaemic thresholds depends on the level and number of glycaemic plateaus, the difference between the separate plateaus, and the number of participants, none of which were consistent across studies. However, we applied interval-censored data statistical methodology to control for these issues and two studies using a graded stepped hypoglycaemic clamp reported similar results [18, 19]. Additionally, three-step and four-step clamps resulted in broadly similar threshold levels and we found no evidence for a modulating effect of the number of participants in each study. Second, the relatively high doses of insulin used in most clamp studies may affect the counterregulatory hormone and symptom responses to hypoglycaemia, which could alter glycaemic thresholds when compared with hypoglycaemia occurring spontaneously. However, since such an effect would equally affect participants, this would not explain differences (or its absence) between participant subgroups or counterregulatory responses. Finally, we corrected for glucose levels measured in whole blood, assuming these to be 11% lower than glucose levels measured in plasma [70]. Although this relationship may be different under conditions of hyperinsulinaemia and hypoglycaemia because of different haematocrit levels [76], we considered this effect to be minimal.
The ADA defines hypoglycaemia in people with diabetes non-numerically as ‘all episodes of an abnormally low plasma glucose concentration that expose the individual to potential harm’ [77]. What constitutes a hypoglycaemic event in the treatment of diabetes is under debate and depends both on the setting and on individual factors. Indeed, it should be acknowledged that glucose levels below which counterregulatory responses are elicited show high intra- and interindividual variability, and this is supported by the ranges around the median glycaemic threshold levels reported here, particularly in people with diabetes. Nevertheless, our analysis in people without diabetes are in line with the International Hypoglycaemia Study Group (IHSG) classification for hypoglycaemia, particularly regarding level 1 hypoglycaemia [78]. However, it should be appreciated that this analysis was based on data obtained during experimental hypoglycaemia and that evidence from other sources, particularly spontaneous hypoglycaemia in daily clinical practice, is additionally needed to further solidify the IHSG classification.
In conclusion, this systematic review shows that counterregulatory hormone responses measured during stepped hyperinsulinaemic–hypoglycaemic glucose clamps are initiated at a median plasma glucose level of 3.8 mmol/l and that both autonomic and neuroglycopenic hypoglycaemic symptoms start at similar glucose levels of around 3.4 mmol/l in people without diabetes. In people with type 1 diabetes, the release of counterregulatory hormones and generation of warning symptoms occur at glucose levels that are 0.1–0.4 mmol/l lower than in people without diabetes, and sometimes at even lower levels in those with impaired awareness. These data may inform clinical practice as well as the conduction of future clinical trials and studies investigating hypoglycaemia, and contribute to discussions about refining the classification of hypoglycaemia.
Data availability
The datasets generated during and/or analysed during the current study are available from the corresponding author on reasonable request.
Abbreviations
- IHSG:
-
International Hypoglycaemia Study Group
- N/A:
-
Not applicable/calculable
References
Cryer PE, Davis SN, Shamoon H (2003) Hypoglycemia in diabetes. Diabetes Care 26:1902–1912. https://doi.org/10.2337/diacare.26.6.1902
Senthilkumaran M, Zhou XF, Bobrovskaya L (2016) Challenges in Modelling Hypoglycaemia-Associated Autonomic Failure: A Review of Human and Animal Studies. Int J Endocrinol. 2016:9801640. https://doi.org/10.1155/2016/9801640
Sherwin RS (1993) Evaluation of hypoglycemic counterregulation using a modification of the Andres glucose clamp. Exp Gerontol 28:371–380. https://doi.org/10.1016/0531-5565(93)90064-K
Fabricius TW, Verhulst CEM, Kristensen PL et al (2021) Hyperinsulinaemic–hypoglycaemic glucose clamps in human research: a systematic review of the literature. Diabetologia 64(4):727–736. https://doi.org/10.1007/s00125-020-05361-8
Zammitt NN, Frier BM (2005) Hypoglycemia in type 2 diabetes: Pathophysiology, frequency, and effects of different treatment modalities. Diabetes Care 28:2948–2961. https://doi.org/10.2337/diacare.28.12.2948
Dagogo-Jack SE, Craft S, Cryer PE (1993) Hypoglycemia-associated autonomic failure in insulin-dependent diabetes mellitus. Recent antecedent hypoglycemia reduces autonomic responses to, symptoms of, and defense against subsequent hypoglycemia. J Clin Invest 91:819–828. https://doi.org/10.1172/JCI116302
Martín-Timón I (2015) Mechanisms of hypoglycemia unawareness and implications in diabetic patients. World J Diabetes 6:912. https://doi.org/10.4239/wjd.v6.i7.912
Covidence (2019) Covidence - Better systematic review management. In: Cochrane. https://www.covidence.org/home. Accessed 13 Jan 2020
Dantz D, Bewersdorf J, Fruehwald-Schultes B et al (2002) Vascular endothelial growth factor: a novel endocrine defensive response to hypoglycemia. J Clin Endocrinol Metab 87:835–840. https://doi.org/10.1210/JCEM.87.2.8215
De Galan BE, Tack CJ, Lenders JW et al (2003) Effect of 2 weeks of theophylline on glucose counterregulation in patients with type 1 diabetes and unawareness of hypoglycemia. Clin Pharmacol Ther 74:77–84. https://doi.org/10.1016/S0009-9236(03)00093-6
Meyer C, Großmann R, Mitrakou A et al (1998) Effects of autonomic neuropathy on counterregulation and awareness of hypoglycemia in type 1 diabetic patients. Diabetes Care 21:1960–1966. https://doi.org/10.2337/DIACARE.21.11.1960
Gabriely I, Wozniak R, Hawkins M, Shamoon H (2001) Troglitazone amplifies counterregulatory responses to hypoglycemia in nondiabetic subjects. J Clin Endocrinol Metab 86:521–528. https://doi.org/10.1210/JCEM.86.2.7197
Dagogo-Jack S, Askari H, Morrill B et al (2000) Physiological responses during hypoglycaemia induced by regular human insulin or a novel human analogue, insulin glargine. Diabetes, Obes Metab 2:373–383. https://doi.org/10.1046/J.1463-1326.2000.00109.X
Matyka K, Evans M, Lomas J et al (1997) Altered hierarchy of protective responses against severe hypoglycemia in normal aging in healthy men. Diabetes Care 20:135–141. https://doi.org/10.2337/diacare.20.2.135
Fanelli C, Pampanelli S, Lalli C et al (1997) Long-term intensive therapy of IDDM patients with clinically overt autonomic neuropathy: effects on hypoglycemia awareness and counterregulation. Diabetes 46:1172–1181. https://doi.org/10.2337/DIAB.46.7.1172
Mitrakou A, Ryan C, Veneman T et al (1991) Hierarchy of glycemic thresholds for counterregulatory hormone secretion, symptoms, and cerebral dysfunction. Am J Physiol 260:E67–E74. https://doi.org/10.1152/AJPENDO.1991.260.1.E67
Jones TW, Boulware SD, Kraemer DT et al (1991) Independent effects of youth and poor diabetes control on responses to hypoglycemia in children. Diabetes 40:358–363. https://doi.org/10.2337/diab.40.3.358
Vea H, Jorde R, Sager G et al (1992) Reproducibility of glycaemic thresholds for activation of counterregulatory hormones and hypoglycaemic symptoms in healthy subjects. Diabetologia 35(10):958–961. https://doi.org/10.1007/BF00401425
Schwartz NS, Clutter WE, Shah SD, Cryer PE (1987) Glycemic thresholds for activation of glucose counterregulatory systems are higher than the threshold for symptoms. J Clin Invest 79:777–781. https://doi.org/10.1172/JCI112884
Powers WJ, Boyle PJ, Hirsch IB, Cryer PE (1993) Unaltered cerebral blood flow during hypoglycemic activation of the sympathochromaffin system in humans. Am J Physiol 265:R8883–R8887. https://doi.org/10.1152/AJPREGU.1993.265.4.R883
Bingham E, Hopkins D, Pernet A et al (2003) The effects of KATP channel modulators on counterregulatory responses and cognitive function during acute controlled hypoglycaemia in healthy men: a pilot study. Diabet Med 20:231–237. https://doi.org/10.1046/J.1464-5491.2003.00922.X
Fanelli CG, Epifano L, Rambotti AM et al (1993) Meticulous prevention of hypoglycemia normalizes the glycemic thresholds and magnitude of most of neuroendocrine responses to, symptoms of, and cognitive function during hypoglycemia in intensively treated patients with short-term IDDM. Diabetes 42:1683–1689. https://doi.org/10.2337/DIAB.42.11.1683
Mellman MJ, Davis MR, Brisman M, Shamoon H (1994) Effect of antecedent hypoglycemia on cognitive function and on glycemic thresholds for counterregulatory hormone secretion in healthy humans. Diabetes Care 17:183–188. https://doi.org/10.2337/DIACARE.17.3.183
Meneilly GS, Cheung E, Tuokko H (1994) Counterregulatory hormone responses to hypoglycemia in the elderly patient with diabetes. Diabetes 43:403–410. https://doi.org/10.2337/DIAB.43.3.403
Meneilly GS, Cheung E, Tuokko H (1994) Altered responses to hypoglycemia of healthy elderly people. J Clin Endocrinol Metab 78:1341–1348. https://doi.org/10.1210/JCEM.78.6.8200936
Snorgaard O, Lassen LH, Rosenfalck AM, Binder C (1991) Glycaemic thresholds for hypoglycaemic symptoms, impairment of cognitive function, and release of counterregulatory hormones in subjects with functional hypoglycaemia. J Intern Med 229:343–350. https://doi.org/10.1111/J.1365-2796.1991.TB00357.X
Fanelli C, Pampanelli S, Epifano L et al (1994) Relative roles of insulin and hypoglycaemia on induction of neuroendocrine responses to, symptoms of, and deterioration of cognitive function in hypoglycaemia in male and female humans. Diabetologia 37:797–807. https://doi.org/10.1007/BF00404337
Schultes B, Peters A, Kern W et al (2005) Processing of food stimuli is selectively enhanced during insulin-induced hypoglycemia in healthy men. Psychoneuroendocrinology 30:496–504. https://doi.org/10.1016/J.PSYNEUEN.2004.12.006
Smith D, Pernet A, Rosenthal JM et al (2004) The effect of modafinil on counter-regulatory and cognitive responses to hypoglycaemia. Diabetologia 47:1704–1711. https://doi.org/10.1007/S00125-004-1513-5
Koivikko ML, Salmela PI, Airaksinen KEJ et al (2005) Effects of sustained insulin-induced hypoglycemia on cardiovascular autonomic regulation in type 1 diabetes. Diabetes 54:744–750. https://doi.org/10.2337/DIABETES.54.3.744
Rickels MR, Schutta MH, Mueller R et al (2007) Glycemic thresholds for activation of counterregulatory hormone and symptom responses in islet transplant recipients. J Clin Endocrinol Metab 92:873–879. https://doi.org/10.1210/JC.2006-2426
Fanelli C, Pampanelli S, Epifano L et al (1994) Long-term recovery from unawareness, deficient counterregulation and lack of cognitive dysfunction during hypoglycaemia, following institution of rational, intensive insulin therapy in IDDM. Diabetologia 37:1265–1276. https://doi.org/10.1007/BF00399801
Fanelli C, Pampanelli S, Calderone S et al (1995) Effects of recent, short-term hyperglycemia on responses to hypoglycemia in humans. Relevance to the pathogenesis of hypoglycemia unawareness and hyperglycemia-induced insulin resistance. Diabetes 44:513–519. https://doi.org/10.2337/DIAB.44.5.513
Brierley EJ, Broughton DL, James OFW, Alberti KGMM (1995) Reduced awareness of hypoglycaemia in the elderly despite an intact counter-regulatory response. QJM An Int J Med 88:439–445. https://doi.org/10.1093/OXFORDJOURNALS.QJMED.A069086
Evans ML, Matyka K, Lomas J et al (1998) Reduced counterregulation during hypoglycemia with raised circulating nonglucose lipid substrates: evidence for regional differences in metabolic capacity in the human brain? J Clin Endocrinol Metab 83:2952–2959. https://doi.org/10.1210/JCEM.83.8.4937
Boyle PJ, Nagy RJ, O’Connor AM et al (1994) Adaptation in brain glucose uptake following recurrent hypoglycemia. Proc Natl Acad Sci U S A 91:9352–9356. https://doi.org/10.1073/PNAS.91.20.9352
Fruehwald-Schultes B, Born J, Kern W et al (2000) Adaptation of cognitive function to hypoglycemia in healthy men. Diabetes Care 23:1059–1066. https://doi.org/10.2337/DIACARE.23.8.1059
Kerr D, Macdonald IA, Tattersall RB (1989) Adaptation to mild hypoglycaemia in normal subjects despite sustained increases in counter-regulatory hormones. Diabetologia 32:249–254. https://doi.org/10.1007/BF00285293
Weinger K, Jacobson AM, Draelos MT et al (1995) Blood glucose estimation and symptoms during hyperglycemia and hypoglycemia in patients with insulin-dependent diabetes mellitus. Am J Med 98:22–31. https://doi.org/10.1016/S0002-9343(99)80077-1
Maran A, Crepaldi C, Trupiani S et al (2000) Brain function rescue effect of lactate following hypoglycaemia is not an adaptation process in both normal and type I diabetic subjects. Diabetologia 43:733–741. https://doi.org/10.1007/S001250051371
Maran A, Crepaldi C, Del Piccolo F et al (2017) Cognitive, neurophysiologic and metabolic sequelae of previous hypoglycemic coma revealed by hyperinsulinemic-hypoglycemic clamp in type 1 diabetic patients. Metab Brain Dis 32:1543–1551. https://doi.org/10.1007/s11011-017-0041-1
Kinsley BT, Widom B, Simonson DC (1995) Differential regulation of counterregulatory hormone secretion and symptoms during hypoglycemia in IDDM. Effect of glycemic control. Diabetes Care 18:17–26. https://doi.org/10.2337/DIACARE.18.1.17
Amiel SA, Pottinger RC, Archibald HR et al (1991) Effect of antecedent glucose control on cerebral function during hypoglycemia. Diabetes Care 14:109–118. https://doi.org/10.2337/DIACARE.14.2.109
Hermanns N, Plate M, Kulzer B et al (2008) Effect of experimentally induced hypoglycemia and different insulin levels on feelings of hunger in type 1 diabetic patients. Exp Clin Endocrinol Diabetes 116:255–261. https://doi.org/10.1055/S-2007-993143
Amiel SA, Sherwin RS, Simonson DC, Tamborlane WV (1988) Effect of intensive insulin therapy on glycemic thresholds for counterregulatory hormone release. Diabetes 37:901–907. https://doi.org/10.2337/diab.37.7.901
Kinsley BT, Simonson DC (1996) Evidence for a hypothalamic-pituitary versus adrenal cortical effect of glycemic control on counterregulatory hormone responses to hypoglycemia in insulin-dependent diabetes mellitus. J Clin Endocrinol Metab 81:684–691. https://doi.org/10.1210/JCEM.81.2.8636289
Gabriely I, Hawkins M, Vilcu C et al (2002) Fructose amplifies counterregulatory responses to hypoglycemia in humans. Diabetes 51:893–900. https://doi.org/10.2337/DIABETES.51.4.893
De Galan BE, Netea MG, Smits P, Van Der Meer JWM (2003) Hypoglycaemia downregulates endotoxin-induced production of tumour necrosis factor-alpha, but does not affect IL-1beta, IL-6, or IL-10. Cytokine 22:71–76. https://doi.org/10.1016/S1043-4666(03)00113-3
Mokan M, Mitrakou A, Veneman T et al (1994) Hypoglycemia unawareness in IDDM. Diabetes Care 17:1397–1403. https://doi.org/10.2337/DIACARE.17.12.1397
Fanelli CG, Paramore DS, Hershey T et al (1998) Impact of nocturnal hypoglycemia on hypoglycemic cognitive dysfunction in type 1 diabetes. Diabetes 47:1920–1927. https://doi.org/10.2337/DIABETES.47.12.1920
Meyer C, Hering BJ, Großmann R et al (1998) Improved glucose counterregulation and autonomic symptoms after intraportal islet transplants alone in patients with long-standing type I diabetes mellitus. Transplantation 66:233–240. https://doi.org/10.1097/00007890-199807270-00017
Oltmanns KM, Deininger E, Wellhoener P et al (2003) Influence of captopril on symptomatic and hormonal responses to hypoglycaemia in humans. Br J Clin Pharmacol 55:347–353. https://doi.org/10.1046/j.1365-2125.2003.01771.x
Kerr D, Macdonald IA, Tattersali RB (1989) Influence of duration of hypoglycemia on the hormonal counterregulatory response in normal subjects. J Clin Endocrinol Metab 68:1118–1122. https://doi.org/10.1210/jcem-68-6-1118
Taverna M, M’bemba J, Sola A et al (2000) Insufficient adaptation of hypoglycaemic threshold for cognitive impairment in tightly controlled type 1 diabetes. Diabetes Metab 26(1):58–64
Maran A, Lomas J, Macdonald IA, Amiel SA (1995) Lack of preservation of higher brain function during hypoglycaemia in patients with intensively-treated IDDM. Diabetologia 38:1412–1418. https://doi.org/10.1007/BF00400601
Deininger E, Oltmanns KM, Wellhoener P et al (2001) Losartan attenuates symptomatic and hormonal responses to hypoglycemia in humans. Clin Pharmacol Ther 70(4):362–369. https://doi.org/10.1016/S0009-9236(01)26448-0
Jones TW, McCarthy G, Tamborlane WV et al (1990) Mild hypoglycemia and impairment of brain stem and cortical evoked potentials in healthy subjects. Diabetes 39:1550–1555. https://doi.org/10.2337/DIAB.39.12.1550
George E, Marques JL, Harris ND et al (1997) Preservation of physiological responses to hypoglycemia 2 days after antecedent hypoglycemia in patients with IDDM. Diabetes Care 20:1293–1298. https://doi.org/10.2337/DIACARE.20.8.1293
Jones TW, Borg WP, Borg MA et al (1997) Resistance to neuroglycopenia: an adaptive response during intensive insulin treatment of diabetes. J Clin Endocrinol Metab 82:1713–1718. https://doi.org/10.1210/JCEM.82.6.3993
Cranston I, Lomas J, Amiel SA et al (1994) Restoration of hypoglycaemia awareness in patients with long-duration insulin-dependent diabetes. Lancet 344:283–287. https://doi.org/10.1016/S0140-6736(94)91336-6
Kanc K, Janssen MMJ, Keulen ETP et al (1998) Substitution of night-time continuous subcutaneous insulin infusion therapy for bedtime NPH insulin in a multiple injection regimen improves counterregulatory hormonal responses and warning symptoms of hypoglycaemia in IDDM. Diabetologia 41:322–329. https://doi.org/10.1007/S001250050910
De Galan BE, Tack CJ, Lenders JW et al (2002) Theophylline improves hypoglycemia unawareness in type 1 diabetes. Diabetes 51:790–796. https://doi.org/10.2337/DIABETES.51.3.790
Kinsley BT, Widom B, Utzschneider K, Simonson DC (1994) Stimulus specificity of defects in counterregulatory hormone secretion in insulin-dependent diabetes mellitus: effect of glycemic control. J Clin Endocrinol Metab 79:1383–1389. https://doi.org/10.1210/JCEM.79.5.7962332
Ovalle F, Fanelli CG, Paramore DS et al (1998) Brief twice-weekly episodes of hypoglycemia reduce detection of clinical hypoglycemia in type 1 diabetes mellitus. Diabetes 47:1472–1479. https://doi.org/10.2337/DIABETES.47.9.1472
Boyle PJ, Schwartz NS, Shah SD et al (1988) Plasma Glucose Concentrations at the Onset of Hypoglycemic Symptoms in Patients with Poorly Controlled Diabetes and in Nondiabetics. N Engl J Med 318:1487–1492. https://doi.org/10.1056/nejm198806093182302
Leelarathna L, Little SA, Walkinshaw E et al (2013) Restoration of self-awareness of hypoglycemia in adultswith long-standing type 1 diabetes: Hyperinsulinemic-hypoglycemic clamp substudy results from the HypoCOMPaSS trial. Diabetes Care 36:4063–4070. https://doi.org/10.2337/dc13-1004
Carey M, Gospin R, Goyal A et al (2017) Opioid Receptor Activation Impairs Hypoglycemic Counterregulation in Humans. Diabetes 66:2764–2773. https://doi.org/10.2337/DB16-1478
ter Braak EWMT, Appelman AMMF, van der Tweel I et al (2002) The sulfonylurea glyburide induces impairment of glucagon and growth hormone responses during mild insulin-induced hypoglycemia. Diabetes Care 25:107–112. https://doi.org/10.2337/diacare.25.1.107
Gabriely I, Shamoon H (2005) Fructose normalizes specific counterregulatory responses to hypoglycemia in patients with type 1 diabetes. Diabetes 54:609–616. https://doi.org/10.2337/DIABETES.54.3.609
Kim HS (2016) Blood glucose measurement: Is serum equal to plasma? Diabetes Metab J 40:365–366. https://doi.org/10.4093/dmj.2016.40.5.365
Rodrigues AS, Calsavara VF, Silva FIB et al (2018) Use of interval-censored survival data as an alternative to Kaplan-Meier survival curves: studies of oral lesion occurrence in liver transplants and cancer recurrence. Appl Cancer Res 381(38):1–10. https://doi.org/10.1186/S41241-018-0067-7
Santiago JV, Clarke WL, Shah SD, Cryer PE (1980) Epinephrine, norepinephrine, glucagon, and growth hormone release in association with physiological decrements in the plasma glucose concentration in normal and diabetic man. J Clin Endocrinol Metab 51:877–883. https://doi.org/10.1210/jcem-51-4-877
Yosten GLC (2018) Alpha cell dysfunction in type 1 diabetes. Peptides 100:54–60. https://doi.org/10.1016/j.peptides.2017.12.001
Bolli G, de Feo P, Compagnucci P et al (1983) Abnormal glucose counterregulation in insulin-dependent diabetes mellitus. Interaction of anti-insulin antibodies and impaired glucagon and epinephrine secretion. Diabetes 32:134–141. https://doi.org/10.2337/diab.32.2.134
Group TDR (1998) Effect of intensive therapy on residual β-cell function in patients with type 1 diabetes in the diabetes control and complications trial: A randomized, controlled trial. Ann Intern Med 128:517–523. https://doi.org/10.7326/0003-4819-128-7-199804010-00001
Hilsted J, Christensen NJ (1992) Dual effect of insulin on plasma volume and transcapillary albumin transport. Diabetologia 35:99–103. https://doi.org/10.1007/BF00402539
Workgroup on Hypoglycemia, American Diabetes Association (2005) Defining and reporting hypoglycemia in diabetes: a report from the American Diabetes Association Workgroup on Hypoglycemia. Diabetes Care 28:1245–1249. https://doi.org/10.2337/diacare.28.5.1245
IHSG (2017) Glucose concentrations of less than 3.0 mmol/L (54 mg/dL) should be reported in clinical trials: A joint position statement of the American diabetes association and the European association for the study of diabetes. Diabetes Care 40:155–157. https://doi.org/10.2337/dc16-2215
Acknowledgements
The authors would like to acknowledge the support of J. Meelby (Information Specialist, Library and Information Services at Nordsjællands Hospital, Denmark) for her assistance with the systematic search strategy.
Authors’ relationships and activities
PLK has received lecture fees from AstraZeneca, Sanofi and Novo Nordisk. CJT has received research support from AstraZeneca, served on advisory boards for Bayer, Boehringer-Ingelheim, MSD and Novo Nordisk, and has received lecture fees from AstraZeneca and Novo Nordisk. RJM has served on advisory boards for Novo Nordisk and Sanofi and has received lecture fees from Novo Nordisk and Sanofi. SRH has served on advisory boards for Sanofi-Aventis, Eli Lilly, Novo Nordisk, Zealand Pharma and has received lecture fees from Novo Nordisk and AstraZeneca. MLE has received speakers/writers’ fees, acted on advisory board, and/or had research collaborations with/acted as a triallist for Eli Lilly, Novo Nordisk, Sanofi, Medtronic, Dexcom, Roche, Astra Zeneca, Zucara, Abbott Diabetes Care, Pila Pharma, Imcyse, Ypsomed and Provention. SAA has served on advisory boards for Medtronic and Novo Nordisk in the last year and given a lecture at a Sanofi-sponsored educational meeting. UP-B has served on advisory boards for AstraZeneca, Bristol-Myers Squibb, Sanofi-Aventis, Novo Nordisk and Zealand Pharma and has received lecture fees from AstraZeneca, Bristol-Myers Squibb, Sanofi-Aventis and Novo Nordisk. BDG has received research support from Novo Nordisk. UP-B and BDG are both associate editors for Diabetologia but were not involved in the handling of the manuscript during the editorial process. All other authors declare that there are no relationships or activities that might bias, or be perceived to bias, their work.
Contribution statement
TWF, CV, UP-B and BDG designed the study. TWF and CV selected the articles, appraised the articles and extracted data for the review. TWF analysed the data. TWF and CV wrote the first version of the manuscript with input from UP-B and BDG. All other authors contributed to interpretation of the data, critical reading and providing comments and edits to the manuscript for important intellectual content. All authors gave final approval of the version to be published. TWF and CV are guarantors of the work.
Funding
This article has received funding from the Innovative Medicines Initiative 2 Joint Undertaking (JU) under grant agreement no. 777460. The JU receives support from the European Union’s Horizon 2020 research and innovation program and EFPIA and T1D Exchange, JDRF, International Diabetes Federation (IDF) and The Leona M. and Harry B. Helmsley Charitable Trust.
Author information
Authors and Affiliations
Consortia
Corresponding authors
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Clementine E. M. Verhulst and Therese W. Fabricius share first authorship. Ulrik Pedersen-Bjergaard and Bastiaan E. de Galan share last authorship.
Supplementary Information
ESM 1
(PDF 851 kb)
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Verhulst, C.E.M., Fabricius, T.W., Teerenstra, S. et al. Glycaemic thresholds for counterregulatory hormone and symptom responses to hypoglycaemia in people with and without type 1 diabetes: a systematic review. Diabetologia 65, 1601–1612 (2022). https://doi.org/10.1007/s00125-022-05749-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00125-022-05749-8