Abstract
A lack of comprehensive mapping of ganglionic inputs into the pancreas and of technology for the modulation of the activity of specific pancreatic nerves has hindered the study of how they regulate metabolic processes. Here we show that the pancreas-innervating neurons in sympathetic, parasympathetic and sensory ganglia can be mapped in detail by using tissue clearing and retrograde tracing (the tracing of neural connections from the synapse to the cell body), and that genetic payloads can be delivered via intrapancreatic injection to target sites in efferent pancreatic nerves in live mice through optimized adeno-associated viruses and neural-tissue-specific promoters. We also show that, in male mice, the targeted activation of parasympathetic cholinergic intrapancreatic ganglia and neurons doubled plasma-insulin levels and improved glucose tolerance, and that tolerance was impaired by stimulating pancreas-projecting sympathetic neurons. The ability to map the peripheral ganglia innervating the pancreas and to deliver transgenes to specific pancreas-projecting neurons will facilitate the examination of ganglionic inputs and the study of the roles of pancreatic efferent innervation in glucose metabolism.
This is a preview of subscription content, access via your institution
Access options
Access Nature and 54 other Nature Portfolio journals
Get Nature+, our best-value online-access subscription
$29.99 / 30 days
cancel any time
Subscribe to this journal
Receive 12 digital issues and online access to articles
$99.00 per year
only $8.25 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout








Similar content being viewed by others
Data availability
The main data supporting the results in this study are available within the paper and its Supplementary Information. The raw and analysed datasets generated during the study are too large to be publicly shared, yet they are available for research purposes from the corresponding author on reasonable request.
References
Grapin-Botton, A. Ductal cells of the pancreas. Int. J. Biochem. Cell Biol. 37, 504–510 (2005).
Röder, P. V., Wu, B., Liu, Y. & Han, W. Pancreatic regulation of glucose homeostasis. Exp. Mol. Med. 48, e219 (2016).
Guenat, E. et al. Counterregulatory responses to hypoglycemia in patients with glucokinase gene mutations. Diabetes Metab. 26, 377–384 (2000).
Thorens, B. Neural regulation of pancreatic islet cell mass and function. Diabetes Obes. Metab. 16, 87–95 (2014).
Yamamoto, H., Nagai, K. & Nakagawa, H. Bilateral lesions of the SCN abolish lipolytic and hyperphagic responses to 2DG. Physiol. Behav. 32, 1017–1020 (1984).
Begg, D. P. & Woods, S. C. Interactions between the central nervous system and pancreatic islet secretions: a historical perspective. Adv. Physiol. Educ. 37, 53–60 (2013).
Holst, J. J. Neural regulation of pancreatic hormone secretion. Clin. Physiol. 5, 34–42 (1985).
Tang, S. C. et al. Human pancreatic neuro-insular network in health and fatty infiltration. Diabetologia 61, 168–181 (2018).
Butterworth, E. et al. High resolution 3D imaging of the human pancreas neuro-insular network. J. Vis. Exp. 2018, 56859 (2018).
Alvarsson, A. et al. A 3D atlas of the dynamic and regional variation of pancreatic innervation in diabetes. Sci. Adv. 6, eaaz9124 (2020).
Lindsay, T. H. et al. A quantitative analysis of the sensory and sympathetic innervation of the mouse pancreas. Neuroscience 137, 1417–1426 (2006).
Fasanella, K. E., Christianson, J. A., Chanthaphavong, R. S. & Davis, B. M. Distribution and neurochemical identification of pancreatic afferents in the mouse. J. Comp. Neurol. 509, 42–52 (2008).
Bou Karam, J. et al. TRPV1 neurons regulate β-cell function in a sex-dependent manner. Mol. Metab. 18, 60–67 (2018).
Quinson, N., Robbins, H. L., Clark, M. J. & Furness, J. B. Locations and innervation of cell bodies of sympathetic neurons projecting to the gastrointestinal tract in the rat. Arch. Histol. Cytol. 64, 281–294 (2001).
Stagner, J. I. & Samols, E. Role of intrapancreatic ganglia in regulation of periodic insular secretions. Am. J. Physiol. 248, E522–E530 (1985).
De Giorgio, R. et al. Patterns of innervation of vasoactive intestinal polypeptide, neuropeptide Y, and gastrin-releasing peptide immunoreactive nerves in the feline pancreas. Pancreas 7, 376–384 (1992).
Hoyes, A. D. & Barber, P. Ultrastructure of the perivascular nerve plexuses of the rat pancreas. Acta Anat. 108, 79–88 (1980).
Kirchgessner, A. L. & Gershon, M. D. Innervation of the pancreas by neurons in the gut. J. Neurosci. 10, 1626–1642 (1990).
Kirchgessner, A. L. & Pintar, J. E. Guinea pig pancreatic ganglia: projections, transmitter content, and the type-specific localization of monoamine oxidase. J. Comp. Neurol. 305, 613–631 (1991).
Li, C. et al. Anatomical and functional characterization of a duodeno-pancreatic neural reflex that can induce acute pancreatitis. Am. J. Physiol. Gastrointest. Liver Physiol. 304, 490–500 (2013).
Renier, N. et al. iDISCO: a simple, rapid method to immunolabel large tissue samples for volume imaging. Cell 159, 896–910 (2014).
Payne, S. C. et al. Differential effects of vagus nerve stimulation strategies on glycemia and pancreatic secretions. Physiol. Rep. 8, 1–11 (2020).
Andersson, P. O., Holst, J. & Järhult, J. Effects of adrenergic blockade on the release of insulin, glucagon and somatostatin from the pancreas in response to splanchnic nerve stimulation in cats. Acta Physiol. Scand. 116, 403–409 (1982).
Ahrén, B., Veith, R. C. & Taborsky, G. J. J. Sympathetic nerve stimulation versus pancreatic norepinephrine infusion in the dog: 1). Effects on basal release of insulin and glucagon. Endocrinology 121, 323–331 (1987).
Barlow, T. E., Greenwell, J. R., Harper, A. A. & Scratcherd, T. The influence of the splanchnic nerves on the external secretion, blood flow and electrical conductance of the cat pancreas. J. Physiol. 236, 421–433 (1974).
Fraser, K. A. & Lee, S. S. Autonomic regulation of splanchnic circulation. Can. J. Gastroenterol. 5, 949037 (1991).
Kaneto, A., Kajinuma, H. & Kosaka, K. Effect of splanchnic nerve stimulation on glucagon and insulin output in the dog. Endocrinology 96, 143–150 (1975).
Roy, M. W., Lee, K. C., Jones, M. S. & Miller, R. E. Neural control of pancreatic insulin and somatostatin secretion. Endocrinology 115, 770–775 (1984).
Meyers, E. E., Kronemberger, A., Lira, V., Rahmouni, K. & Stauss, H. M. Contrasting effects of afferent and efferent vagal nerve stimulation on insulin secretion and blood glucose regulation. Physiol. Rep. 4, e12718 (2016).
Rodriguez-Diaz, R. et al. Noninvasive in vivo model demonstrating the effects of autonomic innervation on pancreatic islet function. Proc. Natl Acad. Sci. USA 109, 21456–21461 (2012).
Stauss, H. M., Stangl, H., Clark, K. C., Kwitek, A. E. & Lira, V. A. Cervical vagal nerve stimulation impairs glucose tolerance and suppresses insulin release in conscious rats. Physiol. Rep. 6, e13953 (2018).
Lindskov, J., Amtorp, O. & Rohl Larsen, H. The effects of highly selective vagotomy on exocrine pancreatic function in man. Gastroenterology 70, 545–549 (1976).
Smith, R. B., Edwards, J. P. & Johnston, D. Effect of vagotomy on exocrine pancreatic and biliary secretion in man. Am. J. Surg. 141, 40–47 (1981).
Fabris, S. E., Thorburn, A., Litchfield, A. & Proietto, J. Effect of parasympathetic denervation of liver and pancreas on glucose kinetics in man. Metabolism 45, 987–991 (1996).
Demir, I. E., Friess, H. & Ceyhan, G. O. Neural plasticity in pancreatitis and pancreatic cancer. Nat. Rev. Gastroenterol. Hepatol. 12, 649–659 (2015).
Karlsson, S., Sundler, F. & Ahrén, B. Neonatal capsaicin-treatment in mice: effects on pancreatic peptidergic nerves and 2-deoxy-d-glucose-induced insulin and glucagon secretion. J. Auton. Nerv. Syst. 39, 51–59 (1992).
Kirkwood, K. S. et al. Substance P inhibits pancreatic exocrine secretion via a neural mechanism. Am. J. Physiol. 277, G314–G320 (1999).
Mason, M. R. J. et al. Comparison of AAV serotypes for gene delivery to dorsal root ganglion neurons. Mol. Ther. https://doi.org/10.1038/mt.2010.19 (2010).
Srivastava, A. In vivo tissue-tropism of adeno-associated viral vectors. Curr. Opin. Virol. 21, 75–80 (2016).
Watson, Z. L. et al. Adeno-associated virus vectors efficiently transduce mouse and rabbit sensory neurons coinfected with herpes simplex virus 1 following peripheral inoculation. J. Virol. 90, 7894–7901 (2016).
Aviello, G. & D’Agostino, G. Tools for controlling activity of neural circuits can boost gastrointestinal research. Front. Pharmacol. 7, https://doi.org/10.3389/fphar.2016.00043 (2016).
Suzuki, H. et al. Characterization of sensory neurons in the dorsal root ganglia of Bax-deficient mice. Brain Res. 1362, 23–31 (2010).
Dang, C. H. et al. In vivo dynamics of AAV-mediated gene delivery to sensory neurons of the trigeminal ganglia. Sci. Rep. https://doi.org/10.1038/s41598-017-01004-y (2017).
Mason, M. R. J. et al. Comparison of AAV serotypes for gene delivery to dorsal root ganglion neurons. Mol. Ther. 18, 715–724 (2010).
Geenen, K., Nauwynck, H. J., De Regge, N., Braeckmans, K. & Favoreel, H. W. Brn-3a suppresses pseudorabies virus-induced cell death in sensory neurons. J. Gen. Virol. 88, 743–747 (2007).
Jooss, K. & Chirmule, N. Immunity to adenovirus and adeno-associated viral vectors: implications for gene therapy. Gene Ther. 10, 955–963 (2003).
Xiao, X. et al. Pancreatic cell tracing, lineage tagging and targeted genetic manipulations in multiple cell types using pancreatic ductal infusion of adeno-associated viral vectors and/or cell-tagging dyes. Nat. Protoc. 9, 2719–2724 (2014).
Isgrò, M. A., Bottoni, P. & Scatena, R. Neuron-specific enolase as a biomarker: biochemical and clinical aspects. Adv. Exp. Med. Biol. 867, 125–143 (2015).
Kim, J., Adam, R. M., Solomon, K. R. & Freeman, M. R. Involvement of cholesterol-rich lipid rafts in interleukin-6-induced neuroendocrine differentiation of LNCaP prostate cancer cells. Endocrinology 145, 613–619 (2004).
Tornoe, J., Kusk, P., Johansen, T. E. & Jensen, P. R. Generation of a synthetic mammalian promoter library by modification of sequences spacing transcription factor binding sites. Gene 297, 21–32 (2002).
Lagos-Quintana, M. et al. Identification of tissue-specific microRNAs from mouse. Curr. Biol. 12, 735–739 (2002).
Brown, B. D. et al. Endogenous microRNA can be broadly exploited to regulate transgene expression according to tissue, lineage and differentiation state. Nat. Biotechnol. 25, 1457–1467 (2007).
Gilon, P. & Henquin, J. C. Mechanisms and physiological significance of the cholinergic control of pancreatic beta-cell function. Endocr. Rev. 22, 565–604 (2001).
Brunicardi, F. C. et al. Splanchnic neural regulation of insulin and glucagon secretion in the isolated perfused human pancreas. Am. J. Surg. 153, 34–40 (1987).
Bloom, S. R. & Edwards, A. V. The release of pancreatic glucagon and inhibition of insulin in response to stimulation of the sympathetic innervation. J. Physiol. 253, 157–173 (1975).
Waxenbaum, J. A. & Varacallo, M. In StatPearls (StatPearls Publishing, 2019).
Makhmutova, M. et al. Pancreatic β-cells communicate with vagal sensory neurons. Gastroenterology 160, 875–888.e11 (2021).
Rajendran, P. S. et al. Identification of peripheral neural circuits that regulate heart rate using optogenetic and viral vector strategies. Nat. Commun. 10, 1944 (2019).
Han, W. et al. A neural circuit for gut-induced reward. Cell 175, 887–888 (2018).
Lundberg, M. et al. The density of parasympathetic axons is reduced in the exocrine pancreas of individuals recently diagnosed with type 1 diabetes. PLoS ONE 12, e0179911 (2017).
Saloman, J. L. et al. Ablation of sensory neurons in a genetic model of pancreatic ductal adenocarcinoma slows initiation and progression of cancer. Proc. Natl Acad. Sci. USA 113, 3078–3083 (2016).
Gallaher, Z. R. & Steward, O. Modest enhancement of sensory axon regeneration in the sciatic nerve with conditional co-deletion of PTEN and SOCS3 in the dorsal root ganglia of adult mice. Exp. Neurol. 303, 120–133 (2018).
Elmallah, M. K. et al. Sustained correction of motoneuron histopathology following intramuscular delivery of AAV in pompe mice. Mol. Ther. 22, 702–712 (2014).
Zheng, H. et al. Efficient retrograde transport of adeno-associated virus type 8 to spinal cord and dorsal root ganglion after vector delivery in muscle. Hum. Gene Ther. 21, 87–97 (2010).
Niu, X. et al. Mapping of extrinsic innervation of the gastrointestinal tract in the mouse embryo. J. Neurosci. 40, 6691–6708 (2020).
Wee, N. K. Y., Lorenz, M. R., Bekirov, Y., Jacquin, M. F. & Scheller, E. L. Shared autonomic pathways connect bone marrow and peripheral adipose tissues across the central neuraxis. Front. Endocrinol. 10, https://doi.org/10.3389/fendo.2019.00668 (2019).
Mickle, A. D. & Gereau, R. W. A bright future? Optogenetics in the periphery for pain research and therapy. Pain 159, S65–S73 (2018).
Davis, A. S. et al. Rational design and engineering of a modified adeno-associated virus (AAV1)-based vector system for enhanced retrograde gene delivery. Neurosurgery 76, 216–225 (2015).
Chakrabarti, S. et al. Intraarticular adeno-associated virus serotype AAV-PHP.S-mediated chemogenetic targeting of knee-innervating dorsal root ganglion neurons alleviates inflammatory pain in mice. Arthritis Rheumatol. 72, 1749–1758 (2020).
Shifrin, A. L., Auricchio, A., Yu, Q.-C., Wilson, J. & Raper, S. E. Adenoviral vector-mediated insulin gene transfer in the mouse pancreas corrects streptozotocin-induced hyperglycemia. Gene Ther. 8, 1480–1489 (2001).
Li, J. H. et al. A novel experimental strategy to assess the metabolic effects of selective activation of a Gq-coupled receptor in hepatocytes in vivo. Endocrinology 154, 3539–3551 (2013).
Hu, J. et al. A G protein-biased designer G protein-coupled receptor useful for studying the physiological relevance of G q/11-dependent signaling pathways. J. Biol. Chem. 291, 7809–7820 (2016).
Nathwani, A. C. et al. Long-term safety and efficacy of factor IX gene therapy in hemophilia B. N. Engl. J. Med. 371, 1994–2004 (2014).
Bustos, R. et al. Synapsin I is expressed in epithelial cells: localization to a unique trans-Golgi compartment. J. Cell Sci. 114, 3695–3704 (2001).
Rolland, A.-S., Kareva, T., Kholodilov, N. & Burke, R. E. A quantitative evaluation of a 2.5-kb rat tyrosine hydroxylase promoter to target expression in ventral mesencephalic dopamine neurons in vivo. Neuroscience 346, 126–134 (2017).
Bandiera, S., Pfeffer, S., Baumert, T. F. & Zeisel, M. B. miR-122–a key factor and therapeutic target in liver disease. J. Hepatol. 62, 448–457 (2015).
Qiao, C. et al. Liver-specific microRNA-122 target sequences incorporated in AAV vectors efficiently inhibits transgene expression in the liver. Gene Ther. 18, 403–410 (2011).
Mcmaster, M. L., Kristinsson, S. Y., Turesson, I., Bjorkholm, M. & Landgren, O. Preferential labeling of inhibitory and excitatory cortical neurons by endogenous tropism of AAV and lentiviral vectors. Clin. Lymphoma 9, 19–22 (2010).
Powell, S. K., Samulski, R. J. & McCown, T. J. AAV capsid-promoter interactions determine CNS cell-selective gene expression in vivo. Mol. Ther. 28, 1373–1380 (2020).
Chiu, Y.-C., Hua, T.-E., Fu, Y.-Y., Pasricha, P. J. & Tang, S.-C. 3-D imaging and illustration of the perfusive mouse islet sympathetic innervation and its remodelling in injury. Diabetologia 55, 3252–3261 (2012).
Klein, E., Salinas, A., Shemesh, E. & Dreiling, D. A. Effects of autonomic denervation on canine exocrine pancreatic secretion and blood flow. Int. J. Pancreatol. 3, 165–170 (1988).
RICHINS, C. A. Effect of sympathetic nerve stimulation on blood flow and secretion in the pancreas of the cat. Am. J. Physiol. 173, 467–470 (1953).
Mei, Q., Mundinger, T. O., Lernmark, K. & Taborsky, G. J. J. Increased galanin expression in the celiac ganglion of BB diabetic rats. Neuropeptides 40, 1–10 (2006).
Zeng, W. et al. Sympathetic neuro-adipose connections mediate leptin-driven lipolysis. Cell 163, 84–94 (2015).
Spencer, N. J. et al. Identification of a rhythmic firing pattern in the enteric nervous system that generates rhythmic electrical activity in smooth muscle. J. Neurosci. 38, 5507–5522 (2018).
Bloom, S. R., Edwards, A. V. & Vaughan, N. J. The role of the autonomic innervation in the control of glucagon release during hypoglycaemia in the calf. J. Physiol. 236, 611–623 (1974).
Tang, S.-C., Peng, S.-J. & Chien, H.-J. Imaging of the islet neural network. Diabetes Obes. Metab. 16, 77–86 (2014).
Rodriguez-Diaz, R. et al. Innervation patterns of autonomic axons in the human endocrine pancreas. Cell Metab. 14, 45–54 (2011).
Banarer, S., McGregor, V. P. & Cryer, P. E. Intraislet hyperinsulinemia prevents the glucagon response to hypoglycemia despite an intact autonomic response. Diabetes 51, 958–965 (2002).
Teff, K. L. & Townsend, R. R. Prolonged mild hyperglycemia induces vagally mediated compensatory increase in C-peptide secretion in humans. J. Clin. Endocrinol. Metab. 89, 5606–5613 (2004).
Ahrén, B., Stern, J. S., Gingerich, R. L., Curry, D. L. & Havel, P. J. Glucagon secretory response to hypoglycaemia, adrenaline and carbachol in streptozotocin-diabetic rats. Acta Physiol. Scand. 155, 215–221 (1995).
Ahrén, B., Wierup, N. & Sundler, F. Neuropeptides and the regulation of islet function. Diabetes 55, S98–S107 (2006).
Khasar, S. G. et al. Gender and gonadal hormone effects on vagal modulation of tonic nociception. J. Pain. 2, 91–100 (2001).
Du, X. J., Dart, A. M. & Riemersma, R. A. Sex differences in the parasympathetic nerve control of rat heart. Clin. Exp. Pharmacol. Physiol. 21, 485–493 (1994).
Saleh, T. M. & Connell, B. J. 17β-Estradiol modulates baroreflex sensitivity and autonomic tone of female rats. J. Auton. Nerv. Syst. 80, 148–161 (2000).
Teff, K. L. How neural mediation of anticipatory and compensatory insulin release helps us tolerate food. Physiol. Behav. 103, 44–50 (2011).
Teff, K. L. & Townsend, R. R. Early phase insulin infusion and muscarinic blockade in obese and lean subjects. Am. J. Physiol. 277, R198–208 (1999).
Rodriguez-Diaz, R. et al. Alpha cells secrete acetylcholine as a non-neuronal paracrine signal priming beta cell function in humans. Nat. Med. 17, 888–892 (2011).
Johnston, N. R. et al. Beta cell hubs dictate pancreatic islet responses to glucose. Cell Metab. 24, 389–401 (2016).
Morgenstern, P. F., Marongiu, R., Musatov, S. A. & Kaplitt, M. G. Adeno-associated viral gene delivery in neurodegenerative disease. Methods Mol. Biol. 793, 443–455 (2011).
Marongiu, R. et al. Gene therapy blockade of dorsal striatal p11 improves motor function and dyskinesia in parkinsonian mice. Proc. Natl Acad. Sci. USA 113, 1423–1428 (2016).
Smith, B. N. et al. Pseudorabies virus expressing enhanced green fluorescent protein: a tool for in vitro electrophysiological analysis of transsynaptically labeled neurons in identified central nervous system circuits. Proc. Natl Acad. Sci. USA 97, 9264–9269 (2000).
Schneider, C. A., Rasband, W. S. & Eliceiri, K. W. NIH Image to ImageJ: 25 years of image analysis. Nat. Methods 9, 671–675 (2012).
Capozzi, M. E. et al. The limited role of glucagon for ketogenesis during fasting or in response to SGLT2 inhibition. Diabetes 69, 882–892 (2020).
Wewer Albrechtsen, N. J. et al. Dynamics of glucagon secretion in mice and rats revealed using a validated sandwich ELISA for small sample volumes. Am. J. Physiol. Endocrinol. Metab. 311, E302–E309 (2016).
Acknowledgements
We thank J. Friedman for critical comments; N. Tzavaras, E. Agullo-Pascual and D. Benson from the Bioimaging Resource Center for assistance and support; G. Gittes and members of the Gittes lab for assistance with intraductal pancreatic surgeries and A. Caicedo and members of the Caicedo lab for advice on intraductal pancreatic surgeries. A.A. was supported by a senior postdoctoral fellowship from the Charles H. Revson Foundation (Grant No. 18-25) and a postdoctoral scholarship from the Swedish Society for Medical Research (SSMF). R.F.H. was supported in part by NIH Training Grant T32GM007280 and F31DK129016. M.J.-G. was supported in part by the Naomi Berries Diabetes Center Russell Berrie Foundation Award. This work was supported by the American Diabetes Association Pathway to Stop Diabetes Grant ADA No. 1-17-ACE-31 and in part by grants from the National Institutes of Health (R01NS097184, OT2OD024912, R01DK124461), the Department of Defense (W81XWH-20-1-0345 and Discovery Award No. W81XWH-20-1-0156) and by funding to M.G.K. from the JPB Foundation. We also thank the NIDDK-supported Einstein-Sinai Diabetes Research Center (DRC) (P-30 DK020541).
Author information
Authors and Affiliations
Contributions
M.J.-G., R.L. and L.E.P. performed experiments, analysed data and contributed to the writing of the manuscript. A.A., R.M. and R.F.H. performed experiments and reviewed the manuscript. M.G.K., R.C.V. and G.J.S. provided experimental and intellectual expertise. S.A.S. performed experiments, analysed data and wrote the manuscript. M.J.-G., R.L., L.E.P. and S.A.S. designed the studies. All authors discussed the results and edited the manuscript.
Corresponding author
Ethics declarations
Competing interests
S.A.S is a named inventor of the patent ‘Compositions and methods to modulate cell activity’ (US9399063B2). S.A.S. and M.G.K. are co-founders of Redpin Therapeutics, and consult for and have equity in the company. M.G.K. also consults for Meira GTx. All other authors declare no competing interests.
Peer review
Peer review information
Nature Biomedical Engineering thanks Philipe Blancou, Gordon Weir and the other, anonymous, reviewer(s) for their contribution to the peer review of this work.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Extended data
Extended Data Fig. 1 Distribution of CTβ + pancreas-innervating neurons across ganglia.
a) Distribution of CTβ + pancreas-innervating neurons between ganglia (number of CTβ + pancreas-innervating neurons in specified ganglia/total number of CTβ + pancreas-innervating neurons in all ganglia) using intrapancreatic injection (IP, grey bars, upper panel) and comparison with intraductal infusion (ID, blue bars). N = 3 mice/ ganglia. b) Size distribution of CTβ + pancreas-innervating neurons in ganglia. Statistical analyses are described in Supplementary Table 3.
Extended Data Fig. 2 Off-target expression after intrapancreatic delivery of AAV.
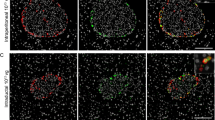
a) Off-target mCherry expression in kidney, muscle and heart, 4 weeks after intrapancreatic AAV8-hSyn-mCherry injection. Scale bars: 50 µm. b) Expression of mCherry 4 weeks after intrapancreatic injection of AAV8-hSyn-mCherry injection (serotypes 6, 8, 9 and rg). c) Images of mCherry and Synapsin in enteric nerves (duodenum). Scale bars: 100 µm. Quantification of viral expression as mCherry+ volume within Synapsin+ volume (bottom panel). n = 4 mice/group. d) Images of mCherry and Synapsin in mesenteric fibers. Scale bars: 50 µm. Quantification of mCherry+ volume within Synapsin+ volume in mesentery (bottom panel). n = 3 mice/group. e) Images of hindbrain stained for mCherry. Scale bars: 100 µm. Right panel: mCherry+ expression as percentage (upper) and total number (lower), n = 5 mice/group. f) Images of mCherry in liver. Scale bars: 50 µm. Right panel: expression of mCherry+ cells as percentage (upper) and total number (lower), n = 5 mice/group. g) Images of mCherry in spleen. Scale bars: 50 µm. Right: expression of mCherry+ cells as percentage (upper) and total number (lower), n = 5 mice/group. h) Quantification of mCherry+ neurons in CG, 4 (N = 6 mice) and 12 (N = 5 mice) weeks after intrapancreatic injection of AAV8-hSyn-mCherry, 1*1011 vg. i) Confocal images (left) and 3D volume segmentation analysis (right) of mCherry + /NF200 + intrapancreatic ganglia after intrapancreatic delivery of AAV8-hsyn-mCherry. N = 88 ganglia from 20 mice in 5 independent studies. Scale bar: 30 µm. Statistical analyses are described in Supplementary Table 3.
Extended Data Fig. 3 Neuronal specific promoters for gene delivery into pancreatic innervation.
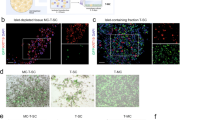
a) Schematic representation of AAV plasmid constructs. b) Immunofluorescence images of HEK293T and Neuro2A cells after transfection with pJeT-mCherry, phSyn-mCherry and pNSE-mCherry. Scale bars: 50 µm. c) Percentage of total cells (left) or percentage of relative to JeT-mcherry expressing mCherry+ cells in HEK293T and N2A after transfection with pJet-mCherry, phSyn-mCherry and pNSE-mCherry. N = 3 independent experiments. d) Fluorescence intensity of mCherry + (left) or relative to JeT-mCherry in HEK293T and N2A after transfection with pJet-mCherry, phSyn-mCherry and pNSE-mCherry. N = 3 independent experiments. e) Quantification of mCherry expression in primary DRG neurons after transfection with phSyn-mCherry and pNSE-mCherry (left panel) and fluorescence/transmitted light images (middle and right panels) showing mCherry (red). Scale bar: 25 µm. N = 3 independent experiments. f) Percentage of CG neurons expressing mCherry+ after intrapancreatic injection of AAV8-hSyn-mCherry and AAV8-NSE-mCherry (left panel) and corresponding images of iDISCO+ cleared CG (middle and right panels). Scale bars: 100 µm. N = 6 samples/group. g) Immunofluorescence image of mCherry expression in liver after intrapancreatic injection of AAV8-NSE-mCherry. Scale bars: 50 µm. Statistical analyses are described in Supplementary Table 3.
Extended Data Fig. 4 CNO does not affect GTT in wild-type (WT) mice and female ChAT-IRES-cre/AAV8-Syn-DIO-hM3D(Gq)-mCherry.
a) GTT in WT mice with CNO (ip, 3 mg/kg) or vehicle (10%DMSO). Right: Cumulative blood glucose change (AUC, 0′ to 120′). N = 10. Blood glucose in male ChAT-IRES-cre/AAV8-Syn-DIO-hM3D(Gq)-mCherry (N = 5) and ChAT-IRES-cre/AAV8-hSyn-DIO-mCherry (N = 8). b) After 6 h fasted with CNO treatment (3 mg/kg ip) over 240 mins. Right: cumulative blood glucose change (AUC, 0′ to 240′). c) During GTT after 6 h fast (vehicle at -30min, glucose 2 mg/kg at 0 min). Right: cumulative blood glucose change (AUC, 0′ to 120′). d) During GTT after 6 h fast (CNO at -180min, glucose 2 mg/kg at 0 min). Right: cumulative blood glucose change (AUC, 0′ to 120′). Blood glucose in female CNO-treated ChAT-IRES-cre/AAV8-hSyn-DIO-hM3D(Gq)-mCherry (N = 5) and ChAT-IRES-cre/AAV8-hSyn-DIO-mCherry (n = 7) mice (CNO: 3 mg/kg, intraperitoneal). e) After 6 h fast. Right: cumulative blood glucose change (AUC, 0′ to 120′). f) During ITT (CNO at -30min, Insulin 0.25U/kg i.p. at 0 min). g) During GTT after 6 h fast (CNO at -30min, glucose 2 mg/kg at 0 min). h) During GTT with atropine methyl nitrate (2 mg/kg, i.p.). i) During GTT after 6 h fast (CNO at -180min, glucose 2 mg/kg at 0 min). j) Cumulative blood glucose change (AUC, 0′ to 120′) during GTT. k) Cumulative blood glucose change (AUC, 0′ to 120′) during GTT with atropine. l) Cumulative blood glucose change (AUC, 0′ to 120′) during GTT 180 mins after CNO. m) Plasma insulin during GTT at -30, 0, and 10 mins. n) Plasma glucagon during GTT at -30, 0, 10, 30, 60 and 90 mins. o) Plasma glucagon during ITT at -30, 0, 10, 30, and 60 mins. Statistical analyses are described in Supplementary Table 3.
Supplementary information
Main Supplementary Information
Supplementary methods, figures, tables and video captions.
Supplementary Video 1
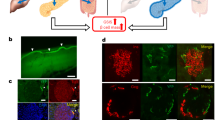
Light-sheet microscopy images of iDISCO+ mouse pancreatic samples immunostained for insulin and vesicular acetylcholine transporter.
Supplementary Video 2
Light-sheet microscopy images of iDISCO+ mouse pancreatic samples immunostained for insulin and tyrosine hydroxylase.
Supplementary Video 3
Confocal microscopy images of pancreas-innervating neurons in coeliac ganglia cleared with iDISCO+.
Rights and permissions
About this article
Cite this article
Jimenez-Gonzalez, M., Li, R., Pomeranz, L.E. et al. Mapping and targeted viral activation of pancreatic nerves in mice reveal their roles in the regulation of glucose metabolism. Nat. Biomed. Eng 6, 1298–1316 (2022). https://doi.org/10.1038/s41551-022-00909-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41551-022-00909-y
This article is cited by
-
O-GlcNAc of STING mediates antiviral innate immunity
Cell Communication and Signaling (2024)
-
Optogenetic control of β cell function
Nature Biomedical Engineering (2023)
-
Optogenetic stimulation of vagal nerves for enhanced glucose-stimulated insulin secretion and β cell proliferation
Nature Biomedical Engineering (2023)