Abstract
Summary
In Japanese patients who experienced an osteoporotic fracture, 10.8% and 18.6% had a subsequent fracture within 1 and 2 years of follow-up, respectively. Although the burden of hip and vertebral fractures has been reported widely, we found that patients with non-hip non-vertebral (NHNV) fractures had a 26% higher risk of subsequent fracture than patients with hip fractures; therefore, NHNV fractures should also be considered an important risk factor for subsequent fracture.
Introduction
To investigate imminent risk and odds of subsequent osteoporotic fractures and associated risk factors in patients who experienced an initial osteoporotic fracture.
Methods
Patients aged ≥ 50 years with ≥ 1 osteoporotic fracture were analyzed from Japan’s Medical Data Vision (MDV) database of claims from acute-care hospitals (January 2012–January 2017). Multivariable models were constructed to explore the impact of key comorbidities and medications on the subsequent fracture risk: Cox proportional hazards model for time to subsequent fracture and logistic regression models for odds of subsequent fracture within 1 and 2 years from index fracture.
Results
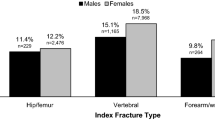
In total, 32,926 patients were eligible with a median follow-up duration of 12.3 months. The percentage of patients experiencing subsequent fractures was 14.1% across the study duration, and 10.8% and 18.6% in patients with 1 and 2 years of follow-up, respectively. In the Cox proportional hazards model, patients with vertebral or NHNV index fractures had a higher subsequent fracture risk than patients with a hip index fracture (adjusted hazard ratio [aHR] 1.11 and 1.26, respectively); subsequent fracture risk was lower in males than females (aHR 0.89). Patients with baseline claims for tranquilizers and glucocorticoids had a higher subsequent fracture risk than those without (aHR 1.14 and 1.08, respectively). Additionally, baseline claims for anti-Parkinson’s medications, alcoholism, and stage 4/5 chronic kidney disease were significantly associated with higher odds of subsequent fracture in the logistic regression models.
Conclusion
Several clinical and demographic factors were associated with a higher risk and odds of subsequent fracture. This may help to identify patients who should be prioritized for osteoporosis treatment.



Similar content being viewed by others
Data sharing statement
The data-sets analyzed in this study can be purchased from MDV. However, the authors cannot share the data with any third parties or make the data publicly available due to protections around the sharing of private health data.
Code availability
Analysis code is not publicly available; however, the authors are happy to provide further details of any aspects of the methodology on request.
References
Orimo H, Nakamura T, Hosoi T et al (2012) Japanese 2011 guidelines for prevention and treatment of osteoporosis–executive summary. Arch Osteoporos 7:3–20. https://doi.org/10.1007/s11657-012-0109-9
Committee of Japanese Guidelines for the Prevention and Treatment of Osteoporosis (2015) Japanese guidelines for the prevention and treatment of osteoporosis, 2015th edn. Life Science Publishing, Tokyo, Japan, pp 2–3 (in Japanese)
International Osteoporosis Foundation (n.d.) Fragility fractures epidemiology. https://www.osteoporosis.foundation/health-professionals/fragility-fractures/epidemiology. Accessed 2 June 2021
Kanis JA, Johnell O, De Laet C et al (2004) A meta-analysis of previous fracture and subsequent fracture risk. Bone 35:375–382. https://doi.org/10.1016/j.bone.2004.03.024
Klotzbuecher CM, Ross PD, Landsman PB, Abbott TA 3rd, Berger M (2000) Patients with prior fractures have an increased risk of future fractures: a summary of the literature and statistical synthesis. J Bone Miner Res 15:721–739. https://doi.org/10.1359/jbmr.2000.15.4.721
van Geel TA, van Helden S, Geusens PP, Winkens B, Dinant GJ (2009) Clinical subsequent fractures cluster in time after first fractures. Ann Rheum Dis 68:99–102. https://doi.org/10.1136/ard.2008.092775
Johansson H, Siggeirsdóttir K, Harvey NC, Odén A, Gudnason V, McCloskey E, Sigurdsson G, Kanis JA (2017) Imminent risk of fracture after fracture. Osteoporos Int 28:775–780. https://doi.org/10.1007/s00198-016-3868-0
Eisman JA, Bogoch ER, Dell R, Harrington JT, McKinney RE Jr, McLellan A, Mitchell PJ, Silverman S, Singleton R, Siris E (2012) Making the first fracture the last fracture: ASBMR task force report on secondary fracture prevention. J Bone Miner Res 27:2039–2046. https://doi.org/10.1002/jbmr.1698
Åkesson K, Marsh D, Mitchell PJ, McLellan A, Stenmark J, Pierroz D, Kyer C, Cooper C (2013) Capture the fracture: a best practice framework and global campaign to break the fragility fracture cycle. Osteoporos Int 24:2135–2152. https://doi.org/10.1007/s00198-013-2348-z
Li N, Hiligsmann M, Boonen A, van Oostwaard M, de Bot R, Wyers C, Bours S, van den Bergh J (2021) The impact of fracture liaison services on subsequent fractures and mortality: a systematic literature review and meta-analysis. Osteoporos Int 32:1517–1530
University of Sheffield Centre for Metabolic Bone Diseases (2008) FRAX® Fracture risk assessment tool. https://www.sheffield.ac.uk/FRAX/. Accessed 11 Nov 2019
Sobue T, Fukuda H, Matsumoto T, Lee B, Ito S, Iwata S (2021) The background occurrence of selected clinical conditions prior to the start of an extensive national vaccination program in Japan. PLoS ONE 16:e0256379. https://doi.org/10.1371/journal.pone.0256379
Medical Data Vision Co. (2017) Press release - overview of database. https://www.mdv.co.jp/press/2017/detail_728.html. Accessed 25 Feb 2021
Taguchi Y, Inoue Y, Kido T, Arai N (2018) Treatment costs and cost drivers among osteoporotic fracture patients in Japan: a retrospective database analysis. Arch Osteoporos 13:45. https://doi.org/10.1007/s11657-018-0456-2
Imai K, Petigara T, Kohn MA, Nakashima K, Aoshima M, Shito A, Kanazu S (2018) Risk of pneumococcal diseases in adults with underlying medical conditions: a retrospective, cohort study using two Japanese healthcare databases. BMJ Open 8:e018553. https://doi.org/10.1136/bmjopen-2017-018553
Nakamura M (2016) Utilization of MDV data and data quality control. Japan Pharmacoepidemiol 21:23–25. https://doi.org/10.3820/jjpe.21.23
Hagino H, Sawaguchi T, Endo N, Ito Y, Nakano T, Watanabe Y (2011) The risk of a second hip fracture in patients after their first hip fracture. Calcif Tissue Int 90:14–21. https://doi.org/10.1007/s00223-011-9545-6
Barron RL, Oster G, Grauer A, Crittenden DB, Weycker D (2020) Determinants of imminent fracture risk in postmenopausal women with osteoporosis. Osteoporos Int 31:2103–2111. https://doi.org/10.1007/s00198-020-05294-3
Balasubramanian A, Zhang J, Chen L, Wenkert D, Daigle SG, Grauer A, Curtis JR (2019) Risk of subsequent fracture after prior fracture among older women. Osteoporos Int 30:79–92. https://doi.org/10.1007/s00198-018-4732-1
Kanis JA, Johansson H, Odén A, Harvey NC, Gudnason V, Sanders KM, Sigurdsson G, Siggeirsdottir K, Fitzpatrick LA, Borgström F (2018) Characteristics of recurrent fractures. Osteoporos Int 29:1747–1757. https://doi.org/10.1007/s00198-018-4502-0
Park JA, Nam JH, Hong SH, Shim YB, Jeong J, Shin JY (2020) Economic burden of subsequent fracture in osteoporosis patients in South Korea. J Med Econ 23:1598–1605. https://doi.org/10.1080/13696998.2020.1831517
Khalid S, Pineda-Moncusí M, El-Hussein L, Delmestri A, Ernst M, Smith C, Libanati C, Toth E, Javaid MK, Cooper C (2021) Predicting imminent fractures in patients with a recent fracture or starting oral bisphosphonate therapy: development and international validation of prognostic models. J Bone Miner Res 36:2162–2176
Iconaru L, Charles A, Baleanu F, Surquin M, Benoit F, Mugisha A, Moreau M, Paesmans M, Karmali R, Rubinstein M (2022) Prediction of an imminent fracture after an index fracture–models derived from the Frisbee cohort. J Bone Miner Res 37:59–67
Rubin KH, Möller S, Holmberg T, Bliddal M, Søndergaard J, Abrahamsen B (2018) A new fracture risk assessment tool (FREM) based on public health registries. J Bone Miner Res 33:1967–1979
Möller S, Skjødt MK, Yan L, Abrahamsen B, Lix LM, McCloskey EV, Johansson H, Harvey NC, Kanis JA, Rubin KH (2022) Prediction of imminent fracture risk in Canadian women and men aged 45 years or older: external validation of the Fracture Risk Evaluation Model (FREM). Osteoporos Int 33:57–66
Cawthon PM (2011) Gender differences in osteoporosis and fractures. Clin Orthop Relat Res 469:1900–1905. https://doi.org/10.1007/s11999-011-1780-7
Toth E, Banefelt J, Åkesson K, Spångeus A, Ortsäter G, Libanati C (2020) History of previous fracture and imminent fracture risk in Swedish women aged 55 to 90 years presenting with a fragility fracture. J Bone Miner Res 35:861–868. https://doi.org/10.1002/jbmr.3953
Ji MX, Yu Q (2015) Primary osteoporosis in postmenopausal women. Chronic Dis Transl Med 1:9–13. https://doi.org/10.1016/j.cdtm.2015.02.006
Söreskog E, Ström O, Spångéus A, Åkesson KE, Borgström F, Banefelt J, Toth E, Libanati C, Charokopou M (2020) Risk of major osteoporotic fracture after first, second and third fracture in Swedish women aged 50 years and older. Bone 134:115286. https://doi.org/10.1016/j.bone.2020.115286
Briot K, Roux C (2015) Glucocorticoid-induced osteoporosis. RMD Open 1:e000014. https://doi.org/10.1136/rmdopen-2014-000014
Pereira RM, Carvalho JF, Canalis E (2010) Glucocorticoid-induced osteoporosis in rheumatic diseases. Clin (Sao Paulo) 65:1197–1205. https://doi.org/10.1590/s1807-59322010001100024
de Jong MR, Van der Elst M, Hartholt KA (2013) Drug-related falls in older patients: implicated drugs, consequences, and possible prevention strategies. Ther Adv Drug Saf 4:147–154. https://doi.org/10.1177/2042098613486829
American Geriatrics Society (2019) Updated AGS Beers Criteria® for potentially inappropriate medication use in older adults. J Am Geriatr Soc 67:674–694. https://doi.org/10.1111/jgs.15767
Allen NE, Schwarzel AK, Canning CG (2013) Recurrent falls in Parkinson’s disease: a systematic review. Parkinsons Dis 2013:906274. https://doi.org/10.1155/2013/906274
Kalilani L, Asgharnejad M, Palokangas T, Durgin T (2016) Comparing the incidence of falls/fractures in Parkinson’s disease patients in the US population. PLoS ONE 11:e0161689. https://doi.org/10.1371/journal.pone.0161689
Zhao DM, Cheng P, Zhu B (2016) Epilepsy and fracture risk: a meta-analysis. Int J Clin Exp Med 9:564–569
Camicioli R, Licis L (2004) Motor impairment predicts falls in specialized Alzheimer care units. Alzheimer Dis Assoc Disord 18:214–218
Qunibi WY (2020) Overview of chronic kidney disease-mineral and bone disorder (CKD-MBD). UpToDate. https://www.uptodate.com/contents/overview-of-chronic-kidney-disease-mineral-and-bone-disorder-ckd-mbd. Accessed 2 Mar 2021
Dawson-Hughes B (2021) Vitamin D deficiency in adults: definition, clinical manifestations, and treatment. UpToDate. https://www.uptodate.com/contents/vitamin-d-deficiency-in-adults-definition-clinical-manifestations-and-treatment. Accessed 22 Mar 2021
Avenell A, Mak JC, O'Connell D (2014) Vitamin D and vitamin D analogues for preventing fractures in post-menopausal women and older men. Cochrane Database Syst Rev. 2014:CD000227. https://doi.org/10.1002/14651858.CD000227.pub4
Shikari M, Kushida K, Yamazaki K, Nagai T, Inoue T, Orimo H (1996) Effects of 2 years’ treatment of osteoporosis with 1 alpha-hydroxy vitamin D3 on bone mineral density and incidence of fracture: a placebo-controlled, double-blind prospective study. Endocr J 43:211–220. https://doi.org/10.1507/endocrj.43.211
Richy F, Deroisy R, Lecart MP, Hanssens L, Mawet A, Reginster JY (2005) D-hormone analog alfacalcidol: an update on its role in post-menopausal osteoporosis and rheumatoid arthritis management. Aging Clin Exp Res 17:133–142. https://doi.org/10.1007/bf03324586
Xu Z, Fan C, Zhao X, Tao H (2016) Treatment of osteoporosis with eldecalcitol, a new vitamin D analog: a comprehensive review and meta-analysis of randomized clinical trials. Drug Des Devel Ther 10:509–517. https://doi.org/10.2147/dddt.S84264
Gaddini GW, Turner RT, Grant KA, Iwaniec UT (2016) Alcohol: a simple nutrient with complex actions on bone in the adult skeleton. Alcohol Clin Exp Res 40:657–671. https://doi.org/10.1111/acer.13000
Nishimura R, Kato H, Kisanuki K, Oh A, Hiroi S, Onishi Y, Guelfucci F, Shimasaki Y (2019) Treatment patterns, persistence and adherence rates in patients with type 2 diabetes mellitus in Japan: a claims-based cohort study. BMJ Open 9:e025806. https://doi.org/10.1136/bmjopen-2018-025806
Kawachi I, Okamoto S, Sakamoto M, Ohta H, Nakamura Y, Iwasaki K, Yoshida M, Hiroi S, Ogino M (2019) Recent transition of medical cost and relapse rate of multiple sclerosis in Japan based on analysis of a health insurance claims database. BMC Neurol 19:1–10. https://doi.org/10.1186/s12883-019-1534-9
ClinRisk Ltd (2016) QFracture Risk Calculator. https://qfracture.org/. Accessed 22 Mar 2021
Heinze G, Wallisch C, Dunkler D (2018) Variable selection–a review and recommendations for the practicing statistician. Biom J 60:431–449. https://doi.org/10.1002/bimj.201700067
Acknowledgements
The authors thank Rebecca Costa for her support with data analysis and Choy Jian Yi for the medical writing and editorial services for this manuscript.
Funding
This study was sponsored by Amgen K.K. and Astellas Pharma Inc. Support for third-party writing assistance for this article, provided by Choy Jian Yi, BSc, Costello Medical, Singapore, was funded by Amgen K.K. and Astellas Pharma Inc. in accordance with Good Publication Practice (GPP3) guidelines (http://www.ismpp.org/gpp3).
Author information
Authors and Affiliations
Contributions
Substantial contributions to study conception and design: All; substantial contributions to analysis and interpretation of the data: All; drafting the article or revising it critically for important intellectual content: All; final approval of the version of the article to be published: All.
Corresponding author
Ethics declarations
Ethics approval and consent to participate
Patient data are de-identified at the hospital level before being incorporated into the MDV database, and the medical claims data retrieved from the database for this study were unlinkable to individual patients. Furthermore, as there was no active enrolment, follow-up, or direct data collection from individuals, ethics committee approval for this study was not necessary. Formal consent from patients for participation and publication was not required for this study.
Conflicts of interest
Saeko Fujiwara received consultation fees from Teijin Pharma Co. Amy Buchanan-Hughes, Alvin Ng and Jennifer Page are employees of Costello Medical, which was funded by Amgen to provide data analysis, research, writing and editorial services for this manuscript. Kenji Adachi is an employee of Amgen, and Hong Li was an employee of Amgen at the time of study conduct and manuscript development.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Fujiwara, S., Buchanan-Hughes, A., Ng, A. et al. Real-world evaluation of osteoporotic fractures using the Japan Medical Data Vision database. Osteoporos Int 33, 2205–2216 (2022). https://doi.org/10.1007/s00198-022-06472-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00198-022-06472-1