Abstract
Summary
The aim of this study was to investigate the relationship between prevalence and risks of osteoporosis or osteoporotic fracture and NAFLD. Patients with NAFLD should be monitored regularly for bone mineral density and bone metabolism indicators to prevent osteoporosis or osteoporotic fractures.
Objectives
The aim of this meta-analysis was to investigate the relationship between prevalence and risks of osteoporosis or osteoporotic fracture and non-alcoholic fatty liver disease (NAFLD).
Methods
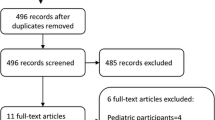
Five databases, including PubMed, Web of Science, Embase, Scopus and Cochrane Library, were searched since the conception of these databases until December 2021. The cohort studies, cross-sectional analyses or case–control studies evaluating the relationship between osteoporosis or osteoporotic fracture and NAFLD were retrieved from these databases. Relevant data were extracted from the included studies, and a meta-analysis was performed.
Results
A total of seven studies were included. The prevalence of osteoporosis or osteoporotic fractures was higher in the NAFLD group than in the non-NAFLD group [OR = 1.17, 95%CI(1.04,1.31)], while the prevalence of osteoporosis was higher in the NAFLD group than in the non-NAFLD group [OR = 1.46, 95%CI (1.21,1.77) and OR = 1.48, 95%CI (1.31,1.68), respectively] in men and women. The risk of osteoporosis or osteoporotic fractures was higher in the NAFLD group than in the non-NAFLD group [OR = 1.33,95%CI (1.24,1.44) and OR = 1.57,95%CI (1.08,2.29), respectively]. The risk of osteoporosis or osteoporotic fractures was higher in male and female NAFLD groups than that in the non-NAFLD group [OR = 1.29, 95%CI(1.14,1.47) and OR = 1.36, 95%CI (1.25,1.48), respectively]. After parameter adjustment, the risk of osteoporosis or osteoporotic fracture was higher in the male NAFLD group than in the non-NAFLD group [OR = 2.10, 95%CI(1.36,3.25)], while no significant difference was found among women [OR = 1.13, 95%CI (0.86,1.48)].
Conclusions
The prevalence and risk of osteoporosis or osteoporotic fractures were significantly associated with NAFLD in men and women.
Trial registration: PROSPERO 2022 CRD42022304708





Similar content being viewed by others
References
Cobbina E, Akhlaghi F (2017)Non-alcoholic fatty liver disease (NAFLD) - pathogenesis, classification, and effect on drug metabolizing enzymes and transporters. Drug Metab Rev 49(2):197–211. https://doi.org/10.1080/03602532.2017.1293683
Mundi MS, Velapati S, Patel J, Kellogg TA, Abu Dayyeh BK, Hurt RT (2020) Evolution of NAFLD and Its Management. Nutr Clin Pract 35(1):72–84. https://doi.org/10.1002/ncp.10449
Michelotti GA, Machado MV, Diehl AM (2013) NAFLD, NASH and liver cancer. Nat Rev Gastroenterol Hepatol 10(11):656–665. https://doi.org/10.1038/nrgastro.2013.183
Patel N, Sharma B, Samant H (2021) Cryptogenic Cirrhosis. StatPearls Publishing, In StatPearls
Dai G, Liu P, Li X, Zhou X, He S (2019) Association between PNPLA3 rs738409 polymorphism and nonalcoholic fatty liver disease (NAFLD) susceptibility and severity: A meta-analysis. Medicine 98(7):e14324. https://doi.org/10.1097/MD.0000000000014324
Hotta K, Yoneda M, Hetal H (2010) Association of the rs738409 polymorphism in PNPLA3 with liver damage and the development of nonalcoholic fatty liver disease. BMC Med Genet 11:172. https://doi.org/10.1186/1471-2350-11-172
Trépo E, Valenti L (2020) Update on NAFLD genetics: From new variants to the clinic. J Hepatol 72(6):1196–1209. https://doi.org/10.1016/j.jhep.2020.02.020
Carlsson B, Lindén D, Brolén G et al (2020) Review article: the emerging role of genetics in precision medicine for patients with non-alcoholic steatohepatitis. Aliment PharmacolTher 51(12):1305–1320. https://doi.org/10.1111/apt.15738
Fatty Liver and Alcoholic Liver Disease Group of the Chinese Medical Association, Fatty Liver Disease Expert Committee of the Chinese Medical Association (2018) Guidelines of prevention and treatment for nonalcoholic fatty liver disease:a 2018 update [J].J Pract Hepatol 177–186. https://doi.org/10.3969/j.issn.1672-5069.2018.02.007
Qadir A, Liang S, Zetal Wu (2020) Senile Osteoporosis: The Involvement of Differentiation and Senescence of Bone Marrow Stromal Cells. Int J Mol Sci 21(1):349. https://doi.org/10.3390/ijms21010349
Kiernan J, Davies JE, Stanford WL (2017) Concise Review: Musculoskeletal Stem Cells to Treat Age-Related Osteoporosis. Stem Cells Transl Med 6(10):1930–1939. https://doi.org/10.1002/sctm.17-0054
Florencio-Silva R, Sasso GR, Sasso-Cerri E et al (2015) Biology of Bone Tissue: Structure, Function, and Factors That Influence Bone Cells. Biomed Res Int 2015:421746. https://doi.org/10.1155/2015/421746
Li X, Kordsmeier J, Xiong J (2021) New Advances in Osteocyte Mechanotransduction. CurrOsteoporos Rep 19(1):101–106. https://doi.org/10.1007/s11914-020-00650-y
Clynes MA, Harvey NC, Curtis EM et al (2020) The epidemiology of osteoporosis. Br Med Bull 133(1):105–117. https://doi.org/10.1093/bmb/ldaa005
Anam AK, Insogna K (2021) Update on Osteoporosis Screening and Management. Med Clin North Am 105(6):1117–1134. https://doi.org/10.1016/j.mcna.2021.05.016
Yang YJ, Kim DJ (2021) An Overview of the Molecular Mechanisms Contributing to Musculoskeletal Disorders in Chronic Liver Disease: Osteoporosis, Sarcopenia, and Osteoporotic Sarcopenia. Int J Mol Sci 22(5):2604. https://doi.org/10.3390/ijms22052604
Locatelli V, Bianchi VE (2014) Effect of GH/IGF-1 on Bone Metabolism and Osteoporsosis. Int J Endocrinol 2014:235060. https://doi.org/10.1155/2014/235060
Mantovani A, Dauriz M, Gatti D et al (2019) Systematic review with meta-analysis: non-alcoholic fatty liver disease is associated with a history of osteoporotic fractures but not with low bone mineral density. Aliment Pharmacol Ther 49(4):375–388. https://doi.org/10.1111/apt.15087
Xie R, Liu M (2022) Relationship Between Non-Alcoholic Fatty Liver Disease and Degree of Hepatic Steatosis and Bone Mineral Density. Front Endocrinol 13:857110. https://doi.org/10.3389/fendo.2022.857110
Shen Z, Cen L, Chen X, Pan J, Li Y, Chen W, Yu C (2020) Increased risk of low bone mineral density in patients with non-alcoholic fatty liver disease: a cohort study. Eur J Endocrinol 182(2):157–164. https://doi.org/10.1530/EJE-19-0699
Upala S, Jaruvongvanich V, Wijarnpreecha K, Sanguankeo A (2017) Nonalcoholic fatty liver disease and osteoporosis: a systematic review and meta-analysis. J Bone Miner Metab 35(6):685–693. https://doi.org/10.1007/s00774-016-0807-2
Stang A (2010) Critical evaluation of the Newcastle-Ottawa scale for the assessment of the quality of nonrandomized studies in meta-analyses. Eur J Epidemiol 25(9):603–605. https://doi.org/10.1007/s10654-010-9491-z
Li M, Xu Y, Metal Xu (2012) Association between nonalcoholic fatty liver disease (NAFLD) and osteoporotic fracture in middle-aged and elderly Chinese. J Clin Endocrinol Metab 97(6):2033–2038. https://doi.org/10.1210/jc.2011-3010
Lee SH, Yun JM, Kim SH et al (2016) Association between bone mineral density and nonalcoholic fatty liver disease in Korean adults. J Endocrinol Invest 39(11):1329–1336. https://doi.org/10.1007/s40618-016-0528-3
Kim G, Kim KJ, Rhee Y, Lim SK (2017) Significant liver fibrosis assessed using liver transient elastography is independently associated with low bone mineral density in patients with non-alcoholic fatty liver disease. PLoS ONE 12(7):e0182202. https://doi.org/10.1371/journal.pone.0182202
Chen HJ, Yang HY, Hsueh KC et al (2018) Increased risk of osteoporosis in patients with nonalcoholic fatty liver disease: A population-based retrospective cohort study. Medicine (Baltimore) 97(42): e12835. https://doi.org/10.1097/MD.0000000000012835
Wang Y, Wen G, Retal Z (2018) Association of Nonalcoholic Fatty Liver Disease With Osteoporotic Fractures: A Cross-Sectional Retrospective Study of Chinese Individuals. Front Endocrinol (Lausanne) 9:408. https://doi.org/10.3389/fendo.2018.00408
Lee HJ, Lee DC, Kim CO (2021) Association Between 10-Year Fracture Probability and Nonalcoholic Fatty Liver Disease With or Without Sarcopenia in Korean Men: A Nationwide Population-Based Cross-Sectional Study. Front Endocrinol (Lausanne) 12:599339. https://doi.org/10.3389/fendo.2021.599339
Loosen SH, Roderburg C, Metal D (2021) Non-alcoholic fatty liver disease (NAFLD) is associated with an increased incidence of osteoporosis and bone fractures. Z Gastroenterol. https://doi.org/10.1055/a-1482-9236.10.1055/a-1482-9236
Wáng Y, Lentle BC (2020) Radiographic osteoporotic vertebral fractures in elderly men: a brief review focusing on differences between the sexes. Quant Imaging Med Surg 10(9):1863–1876. https://doi.org/10.21037/qims-2020-21
Wang D, Liu N, Gao Y, Li P, Tian M (2014) Association between metabolic syndrome and osteoporotic fracture in middle-aged and elderly Chinese peoples. Cell Biochem Biophys 70(2):1297–1303. https://doi.org/10.1007/s12013-014-0054-x
Lee J, Yoon K, Ryu S, Chang Y, Kim HR (2017) High-normal levels of hs-CRP predict the development of non-alcoholic fatty liver in healthy men. PLoS ONE 12(2):e0172666. https://doi.org/10.1371/journal.pone.0172666
Noh JY, Yang Y, Jung H (2020) Molecular Mechanisms and Emerging Therapeutics for Osteoporosis. Int J Mol Sci 21(20):7623. https://doi.org/10.3390/ijms21207623
Laurent MR, Dedeyne L, Dupont J, Mellaerts B, Dejaeger M, Gielen E (2019) Age-related bone loss and sarcopenia in men. Maturitas 122:51–56. https://doi.org/10.1016/j.maturitas.2019.01.006
Jähn-Rickert K, Zimmermann EA (2021) Potential Role of Perilacunar Remodeling in the Progression of Osteoporosis and Implications on Age-Related Decline in Fracture Resistance of Bone. Curr Osteoporos Rep 19(4):391–402. https://doi.org/10.1007/s11914-021-00686-8
Aydın MM, Akçalı KC (2018) Liver fibrosis. Turk J Gastroenterol 29(1):14–21. https://doi.org/10.5152/tjg.2018.17330
Povero D, Feldstein AE (2016) Novel Molecular Mechanisms in the Development of Non-Alcoholic Steatohepatitis. Diabetes Metab J 40(1):1–11. https://doi.org/10.4093/dmj.2016.40.1.1
Yang L, Yang CQ (2021) Liver cirrhosis and secondary osteoporosis. Chin J Hepatol 29(3):204–208. https://doi.org/10.3760/cma.j.cn501113-20210208-00078
Filip R, Radzki RP, Bieńko M (2018) Novel insights into the relationship between nonalcoholic fatty liver disease and osteoporosis. Clin Interv Aging 13:1879–1891. https://doi.org/10.2147/CIA.S170533:1879-1891
Xian L, Wu X, Pang L et al (2012) Matrix IGF-1 maintains bone mass by activation of mTOR in mesenchymal stem cells. Nat Med 18(7):1095–1101. https://doi.org/10.1038/nm.2793
Wang Y, Dai J, Zhong W, Hu C, Lu S, Chai Y (2018) Association between Serum Cholesterol Level and Osteoporotic Fractures. Front Endocrinol (Lausanne) 9:30. https://doi.org/10.3389/fendo.2018.00030
An T, Hao J, Sun S et al (2017) Efficacy of statins for osteoporosis: a systematic review and meta-analysis. Osteoporos Int 28(1):47–57. https://doi.org/10.1007/s00198-016-3844-8
Zhang Z, Thorne JL, Moore JB (2019) Vitamin D and nonalcoholic fatty liver disease. CurrOpin Clin NutrMetab Care 22(6):449–458. https://doi.org/10.1097/MCO.0000000000000605
Barchetta I, Cimini FA, Cavallo MG (2017) Vitamin D Supplementation and Non-Alcoholic Fatty Liver Disease: Present and Future. Nutrients 9(9):1015. https://doi.org/10.3390/nu9091015
Erem S, Atfi A, Razzaque MS (2019) Anabolic effects of vitamin D and magnesium in aging bone. J Steroid Biochem Mol Biol 193:105400. https://doi.org/10.1016/j.jsbmb.2019.105400
Acknowledgements
Not applicable.
Funding
This study was funded by National Natural Science Foundation of China (No.81960155), Natural Science Foundation of Gansu Province (20JR10RA690) and Health industry scientific research project of Gansu Province (No.GSWSKY-2019–07).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Data Sharing
The data that support the findings of this study are available from the corresponding author upon reasonable request.
Consent to participate
Not applicable.
Conflicts of interest
Binjing Pan, Jing Cai, Pingping Zhao, Jingfang Liu, Gaojing Jing, QianglongNiu, and Qiong Li declare that they have no competing interests.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Pan, B., Cai, J., Zhao, P. et al. Relationship between prevalence and risk of osteoporosis or osteoporotic fracture with non-alcoholic fatty liver disease: A systematic review and meta-analysis. Osteoporos Int 33, 2275–2286 (2022). https://doi.org/10.1007/s00198-022-06459-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00198-022-06459-y