Abstract
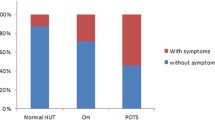
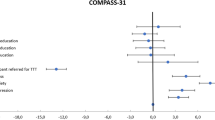
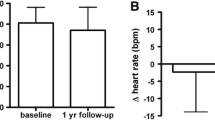
Chronic orthostatic intolerance (COI) is defined by changes in heart rate (HR), blood pressure (BP), respiration, symptoms of cerebral hypoperfusion and sympathetic overactivation. Postural tachycardia syndrome (POTS) is the most common form of COI in young adults and is defined by an orthostatic increase in heart rate (HR) of ≥ 30 bpm in the absence of orthostatic hypotension. However, some patients referred for evaluation of COI symptoms do not meet the orthostatic HR response criterion of POTS despite debilitating symptoms. Such patients are ill defined, posing diagnostic and therapeutic challenges. This study explored the relationship among cardiovascular autonomic control, the orthostatic HR response, EtCO2 and the severity of orthostatic symptoms and fatigue in patients referred for evaluation of COI. Patients (N = 108) performed standardized testing protocol of the Autonomic Reflex Screen and completed the Composite Autonomic Symptom Score (COMPASS-31) and the Fatigue Severity Scale (FSS). Greater severity of COI was associated with younger age, larger phase IV amplitude in the Valsalva maneuver and lower adrenal baroreflex sensitivity. Greater fatigue severity was associated with a larger reduction in ETCO2 during 10 min of head-up tilt (HUT) and reduced low-frequency (LF) power of heart rate variability. This study suggests that hemodynamic changes associated with the baroreflex response and changes in EtCO2 show a stronger association with the severity of orthostatic symptoms and fatigue than the overall orthostatic HR response in patients with COI.

Similar content being viewed by others
References
Anderson, G. W., Lambert, E. A., Sari, C. I., Dawood, T., Esler, M. D., Vaddadi, G., & Lambert, G. W. (2014). Cognitive dysfunction, health-related quality of life, and symptoms of depression and anxiety sensitivity are impaired in patients with the postural orthostatic tachycardia syndrome (POTS). Frontiers in Physiology, 5, 230. https://doi.org/10.3389/fphys.2014.00230
Arnold, A. C., Haman, K., Garland, E. M., Raj, V., Dupont, W. D., Biaggioni, I., Robertson, D., & Raj, S. R. (2015). Cognitive dysfunction in postural tachycardia syndrome. Clinical Science, 128, 39–45. https://doi.org/10.1042/CS20140251
Baker, J., Racosta, J. M., Balint, B., & Kimpinski, K. (2018). Utility of time and frequency domain parameters of heart rate variability in the context of autonomic disorders characterized by orthostatic dysfunction. Journal of Clinical Neurophysiology, 35, 123–129.
Ball, S., & Shekhar, A. (1997). Basilar artery response to hyperventilation in panic disorder. American Journal of Psychiatry, 154, 1603–1604. https://doi.org/10.1176/ajp.154.11.1603
Boris, J. R., Huang, J., & Bernadzikowski, T. (2020). Orthostatic heart rate does not predict symptomatic burden in pediatric patients with chronic orthostatic intolerance. Clinical Autonomic Research, 30, 19–28. https://doi.org/10.1007/s10286-019-00622-y
Bruce, B. K., Harrison, T. E., Bee, S. M., Luedtke, C. A., Porter, C. J., Fischer, P. R., Hayes, S. E., Allman, D. A., Ale, C. M., & Weiss, K. E. (2016). Improvement in functioning and psychological distress in adolescents with postural orthostatic tachycardia syndrome following interdisciplinary treatment. Clinical Pediatrics, 55, 1300–1304. https://doi.org/10.1177/0009922816638663
Custaud, M. A., de Souza Neto, E. P., Abry, P., Flandrin, P., Millet, C., Duvareille, M., Fortrat, J. O., & Gharib, C. (2002). Orthostatic tolerance and spontaneous baroreflex sensitivity in men versus women after 7 days of head-down bed rest. Autonomic Neuroscience: Basic & Clinical, 100, 66–76.
Dittner, A. J., Wessely, S. C., & Brown, R. G. (2004). The assessment of fatigue: A practical guide for clinicians and researchers. Journal of Psychosomatic Research, 56, 157–170. https://doi.org/10.1016/S0022-3999(03)00371-4
Farquhar, W. B., Taylor, J. A., Darling, S. E., Chase, K. P., & Freeman, R. (2000). Abnormal baroreflex responses in patients with idiopathic orthostatic intolerance. Circulation, 102, 2086–3091. https://doi.org/10.1161/01.cir.102.25.3086
Fisher, C. J., Katzan, I., Heinberg, L. J., Schuster, A. T., Thompson, N. R., & Wilson, R. (2020). Psychological correlates of patients with postural orthostatic tachycardia syndrome (POTS). Autonomic Neuroscience, 227, 102790. https://doi.org/10.1016/j.autneu.2020.102690
Fu, Q., & Levine, B. D. (2018). Exercise and non-pharmacological treatment of POTS. Autonomic Neuroscience: Basic and Clinical, 215, 20–27. https://doi.org/10.1016/j.autneu.2018.07.001
Galbreath, M. M., Shibata, S., VanGundy, T. B., Okazaki, K., Fu, Q., & Levine, B. D. (2011). Effects of exercise training on arterial-cardiac baroreflex function in POTS. Clinical Autonomic Research, 21, 73–80. https://doi.org/10.1007/s10286-010-0091-5
Gevirtz, R. (2013). The promise of heart rate variability biofeedback: Evidence-based application. Biofeedback, 41, 110–120. https://doi.org/10.5298/1081-5937-41.3.01
Gibbs, D. M. (1992). Hyperventilation-induced cerebral ischemia in panic disorder and effect of nimodipine. American Journal of Psychiatry, 149, 1589–1591. https://doi.org/10.1176/ajp.149.11.1589
Hewlett, S., Dures, E., & Almeida, C. (2011). Measures of fatigue: Bristol Rheumatoid Arthritis Fatigue Multi-Dimensional Questionnaire (BRAF MDQ), Bristol Rheumatoid Arthritis Fatigue Numerical Rating Scales (BRAF NRS) for Severity, Effect, and Coping, Chalder Fatigue Questionnaire (CFQ), Checklist Individual Strength (CIS20R and CIS8R), Fatigue Severity Scale (FSS), Functional Assessment Chronic Illness Therapy (Fatigue) (FACIT-F), Multi-Dimensional Assessment of Fatigue (MAF), Multi-Dimensional Fatigue Inventory (MFI), Pediatric Quality Of Life (PedsQL) Multi-Dimensional Fatigue Scale, Profile of Fatigue (ProF), Short Form 36 Vitality Subscale (SF-36 VT), and Visual Analog Scales (VAS). Arthritis Care & Research, 63, S263–S286. https://doi.org/10.1002/acr.20579
Huang, C.-C., Sandroni, P., Sletten, D. M., Weigand, S. D., & Low, P. A. (2007). Effect of age on adrenergic and vagal baroreflex sensitivity in normal subjects. Muscle & Nerve, 36, 637–642. https://doi.org/10.1002/mus.20853
Immink, R. V., Pott, F. C., Secher, N. H., & van Lieshout, J. J. (2014). Hyperventilation, cerebral perfusion, and syncope. Journal of Applied Physiology, 116, 844–851. https://doi.org/10.1152/japplphysiol.00637.2013
Jacob, G., Shannon, J. R., Black, B., Biaggioni, I., Mosqueda-Garcia, R., Robertson, R. M., & Robertson, D. (1997). Effects of volume loading and pressor agents in idiopathic orthostatic tachycardia. Circulation, 96, 575–580. https://doi.org/10.1161/01.cir.96.2.575
Khurana, R. K. (2006). Experimental induction of panic-like symptoms in patients with postural tachycardia syndrome. Clinical Autonomic Research, 16, 371–377. https://doi.org/10.1007/s10286-006-0365-0
Krupp, L. B., LaRocca, N. G., Muir-Nash, J., & Steinberg, A. D. (1989). The fatigue severity scale. Application to patients with multiple sclerosis and systemic lupus erythematosus. Archives of Neurology, 46, 1121–1123. https://doi.org/10.1001/archneur.1989.0050460115022
Lehrer, P. M., & Gevirtz, R. (2014). Heart rate variability biofeedback: How and why does it work? Frontiers in Psychology, 5, 756. https://doi.org/10.3389/fpsyg.2014.00756
Lehrer, P. M., Kaur, K., Sharma, A., Shah, K., Huseby, R., Bhavsar, J., Sgobba, P., & Zhang, Y. (2020). Heart rate variability biofeedback improves emotional and physical health and performance: A systematic review and meta analysis. Applied Psychophysiology and Biofeedback, 45, 109–129. https://doi.org/10.1007/s10484-020-09466-z
Low, P. A., Opfer-Gehrking, T. L., Textor, S. C., Benarroch, E. E., Shen, W. K., Schondorf, R., Suarez, G. A., & Rummans, T. A. (1995). Postural tachycardia syndrome (POTS). Neurology, 45, S19–S25.
Low, P. A., Sandroni, P., Joyner, M., & Shen, W.-K. (2009). Postural tachycardia syndrome (POTS). Journal of Cardiovascular Electrophysiology, 20, 352–358. https://doi.org/10.1111/j.1540-8167.2008.01407.x
Low, P.A., & Sletten, D.M. (2008). Laboratory evaluation of autonomic failure, In P.A. Low & E.E. Benarroch (Eds.), Clinical Autonomic Disorders (3rd ed., pp. 130–163). Lippincott Williams & Wilkins.
Mar, P. L., & Raj, S. R. (2020). Postural orthostatic tachycardia syndrome: Mechanisms and new therapies. Annual Review of Medicine, 71, 235–248. https://doi.org/10.1146/annurev-med-041818-011630
Masuki, S., Eisenach, J. H., Johnson, C. P., Dietz, N. M., Benrud-Larson, L. M., Schrage, W. G., Curry, T. B., Sandroni, P., Low, P. A., & Joyner, M. J. (2007). Excessive heart rate response to orthostatic stress in postural tachycardia syndrome is not caused by anxiety. Journal of Applied Physiology, 102, 896–903. https://doi.org/10.1152/japplphysiol.00927.2006
Moon, J., Kim, D.-Y., Byun, J.-I., Sunwoo, J.-S., Lim, J.-A., Kim, T.-J., Shin, J.-W., Lee, W.-J., Lee, H.-S., Jun, J. S., Park, K.-I., Jung, K.-H., Lee, S.-T., Jung, K.-Y., Chu, K., & Lee, S.-K. (2016). Orthostatic intolerance symptoms are associated with depression and diminished quality of life in patients with postural tachycardia syndrome. Health and Quality of Life Outcomes, 14, 144. https://doi.org/10.1186/s12955-016-0548-x
Mustafa, H.I., Raj, S.R., Diedrich, A., Black, B.K., Paranjape, S.Y., Dupont, W.D., Williams, G.H., Biaggioni, I., & Robertson, D. (2012). Altered systemic hemodynamic & baroreflex response to Angiotensin II in Postural Tachycardia Syndrome. Circulation: Arrhythmia and Electrophysiology, 5, 173–180. https://doi.org/10.1161/CIRCEP.111.965343
Norcliffe-Kaufmann, L., Galindo-Mendez, B., Garcia-Guarniz, A.-L., Villareal-Vitorica, E., & Novak, V. Transcranial doppler in autonomic testing: standards and clinical applications. Clinical Autonomic Research, 28, 187–202. https://doi.org/10.1007/s10286-017-0454-2
Novak, P. (2016a). Cerebral blood flow, heart rate, and blood pressure patterns during the tilt test in common orthostatic syndromes. Neuroscience Journal, 2016, 6127340. https://doi.org/10.1155/2016/6127340
Novak, P. (2016b). Orthostatic cerebral hypoperfusion syndrome. Frontiers in Aging Neuroscience, 8, 22. https://doi.org/10.3389/fnagi.2016.00022
Novak, P. (2018). Hypocapnic cerebral hypoperfusion: A biomarker of orthostatic intolerance. PLoS ONE, 13, e0204419. https://doi.org/10.1371/journal.pone.0204419
Novak, P. (2019). Autonomic testing. Oxford University Press.
Novak, V., Spies, J. M., Novak, P., McPhee, B. R., Rummans, T. A., & Low, P. A. (1998). Hypocapnia and cerebral hypoperfusion in orthostatic intolerance. Stroke, 29, 1876–1881. https://doi.org/10.1161/01.str.29.9.1876
Parsaik, A., Allison, T. G., Singer, W., Sletten, D. M., Joyner, M. J., Benarroch, E. E., Low, P. A., & Sandroni, P. (2012). Deconditioning in patients with orthostatic intolerance. Neurology, 79, 1435–1439. https://doi.org/10.1212/WNL.0b013e31826d5f95
Rahman, F., Pechnik, S., Gross, D., Sewell, L., & Goldstein, D. S. (2011). LF power reflects baroreflex function, not cardiac sympathetic innervation. Clinical Autonomic Research, 21, 133–141. https://doi.org/10.1007/s10286-010-0098-y
Raj, V., Haman, K.L., Raj, S.R., Byrne, D., Blakely, R.D., Biaggioni, I., Robertson, D., & Shelton, R.C. (2009). Psychiatric profile and attention deficits in postural tachycardia syndrome. Journal of Neurology, Neurosurgery, and Psychiatry, 80, 339–344.
Raj, V., Opie, M., & Arnold, A. C. (2018). Cognitive and psychological issues in posturaltachycardia syndrome. Autonomic Neuroscience, 215, 46–55. https://doi.org/10.1016/j.autneu.2018.03.004
Rea, N. A., Campbell, C. I., & Cortez, M. M. (2017). Quantitative assessment of autonomic symptom burden in Postural tachycardia syndrome (POTS). Journal of the Neurological Sciences, 377, 35–41. https://doi.org/10.1016/j.jns.2017.03.032
Robertson, D. (1999). The epidemic of orthostatic tachycardia and orthostatic intolerance. The American Journal of the Medical Sciences, 317, 75–77. https://doi.org/10.1097/00000441-199902000-00001
Ross, A. J., Medow, M. S., Rowe, P. C., & Stewart, J. M. (2013). What is brain fog? An evaluation of the symptom in postural tachycardia syndrome. Clinical Autonomic Research, 23, 305–311. https://doi.org/10.1007/s10286-013-0212-z
Sandroni, P., Benarroch, E. E., & Low, P. A. (1991). Pharmacological dissection of components of the Valsalva maneuver in adrenergic failure. Journal of Applied Physiology, 71, 1563–1567. https://doi.org/10.1152/jappl.1991.71.4.1563
Sandroni, P., Novak, V., Opfer-Gehrking, T. L., Huck, C. A., & Low, P. A. (2000). Mechanisms of blood pressure alterations in response to the Valsalva maneuver in postural tachycardia syndrome. Clinical Autonomic Research, 10, 1–5. https://doi.org/10.1007/bf02291382
Schondorf, R., & Low, P. A. (1993). Idiopathic postural orthostatic tachycardia syndrome: Attenuated form of acute pandysautonomia? Neurology, 43, 132–137. https://doi.org/10.1212/wnl.43.1_part_1.132
Schrezenmaier, C., Singer, W., Muenter Swift, N., Sletten, D., Tanabe, J., & Low, P. A. (2007). Adrenergic and vagal baroreflex sensitivity in autonomic failure. Archives of Neurology, 64, 381–386. https://doi.org/10.1001/archneur.64.3.381
Sheldon, R. S., Grubb, B. P., 2nd., Olshansky, B., Shen, W. K., Calkins, H., Brignole, M., Raj, S. R., Krahn, A. D., Morillo, C. A., Stewart, J. M., Sutton, R., Sandroni, P., Friday, K. J., Hachul, D. T., Cohen, M. I., Lau, D. H., Mayuga, K. A., Moak, J. P., Sandhu, R. K., & Kanjwal, K. (2015). Heart rhythm society expert consensus statement on the diagnosis and treatment of postural tachycardia syndrome, inappropriate sinus tachycardia, and vasovagal syncope. Heart Rhythm, 12, e41-63. https://doi.org/10.1016/j.hrthm.2015.03.029
Shibao, C., Arzubiaga, C., Roberts, L. J., 2nd., Raj, S., Black, B., Harris, P., & Biaggioni, I. (2005). Hyperadrenergic postural tachycardia syndrome in mast cell activation disorders. Hypertension, 45, 385–390. https://doi.org/10.1161/01.HYP.0000158259.68614.40
Shibata, S., Fu, Q., Bivens, T. B., Hastings, J. L., Wang, W., & Levine, B. D. (2012). Short-term exercise training improves the cardiovascular response to exercise in the postural orthostatic tachycardia syndrome. The Journal of Physiology, 590, 3495–3505. https://doi.org/10.1113/jphysiol.2012.233858
Shields, R. W. (2009). Heart rate variability with deep breathing as a clinical test of cardiovagal function. Cleveland Clinic Journal of Medicine, 76, S37–S40. https://doi.org/10.3949/ccjm.76s2.08
Sletten, D. M., Suarez, G. A., Low, P. A., Mandrekar, J., & Singer, W. (2012). COMPASS-31: A refined and abbreviated composite autonomic symptom score. Mayo Clinic Proceedings, 87, 1196–1201. https://doi.org/10.1016/j.mayocp.2012.10.013
Stewart, J. M. (2000). Autonomic nervous system dysfunction in adolescents with postural orthostatic tachycardia syndrome and chronic fatigue syndrome is characterized by attenuated vagal baroreflex and potentiated sympathetic vasomotion. Pediatric Research, 48, 218–226. https://doi.org/10.1203/00006450-200008000-00016
Stewart, J. M. (2013). Common syndromes of orthostatic intolerance. Pediatrics, 131, 968–980. https://doi.org/10.1542/peds.2012-2610
Stewart, J. M., Medow, M. S., Cherniack, N. S., & Natelson, B. H. (2006). Postural hypocapnic hyperventilation is associated with enhanced peripheral vasoconstriction in postural tachycardia syndrome with normal supine blood flow. American Journal of Physiology Heart and Circulatory Physiology, 291, H904–H913. https://doi.org/10.1152/ajpheart.01359.2005
Stewart, J. M., Medow, M. S., Montgomery, L. D., Glover, J. L., & Millonas, M. (2005). Splanchnic hyperemia and hypervolemia during Valsalva maneuver in postural tachycardia syndrome. American Journal of Physiology Heart and Circulatory Physiology, 289, H1951–H1959. https://doi.org/10.1152/ajpheart.00194.2005
Stewart, J. M., Pianosi, P., Shaban, M. A., Terilli, C., Svistunova, M., Visintainer, P., & Medow, M. S. (2018). Postural hyperventilation as a cause of postural tachycardia syndrome: Increased systemic vascular resistance and decreased cardiac output when upright in all postural tachycardia syndrome variants. Journal of the American Heart Association, 7, e008854. https://doi.org/10.1161/JAHA.118.008854
Task Force of the European Society of Cardiology and the North American Society of Pacing and Electrophysiology. (1996). Heart rate variability: Standards of measurement, physiological interpretation, and clinical use. Circulation, 93, 1043–1065.
Van De Borne, P., Mezzetti, S., Montano, N., Narkiewicz, K., Degaute, J. P., & Somers, V. K. (2000). Hyperventilation alters arterial baroreflex control of heart rate and muscle sympathetic activity. American Journal of Physiology Heart and Circulatory Physiology, 279, H436–H441. https://doi.org/10.1152/ajpheart.2000.279.2.H536
Acknowledgements
The authors thank Kathryn Dickson, RN and Taelor Getz for assistance in data analyses. This study is funded by Scripps Clinic Medical Group Research Fund and from the Hearst Endowment. The Scripps Clinic Medical Group Research Fund and the Hearst Endowment had no further role in study design; in the collection, analysis and interpretation of data; in the writing of the report; or in the decision to submit the paper for publication.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflicts of interests.
Informed Consent
All patients were over 18 years of age. The study was approved by the Scripps Health’s Institutional Review Board of the Office for the Protection of Research Subjects as a minimal risk study and written consent was waived.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Wheeler, C., Pacheco, J.M., Kim, A.C. et al. Cardiovascular Autonomic Regulation, ETCO2 and the Heart Rate Response to the Tilt Table Test in Patients with Orthostatic Intolerance. Appl Psychophysiol Biofeedback 47, 107–119 (2022). https://doi.org/10.1007/s10484-022-09536-4
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10484-022-09536-4