Abstract
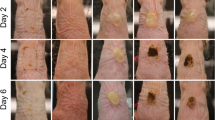
The overuse of antibiotics in medicine has led to concerns over management of wound infections where antibiotic-resistant bacteria are involved. Wound infections exhibit both acquired and biofilm-associated antibiotic resistance; innovative non-antibiotic therapeutic and preventive treatments are needed to limit emergence of conventional antimicrobial resistance and to address biofilm-associated resistance. Toward this goal, natural antibacterial clays have been identified that are effective at killing drug-resistant human pathogens in planktonic and biofilm states, in vitro. To move toward clinical testing of antibacterial clays, the present study was conducted to evaluate the topical application of a natural antibacterial clay to wounds in mice experimentally infected with methicillin-resistant Staphylococcus aureus (MRSA). Five preliminary animal trials were conducted to test various methods of applying hydrated antibacterial clay to infected wounds. None of the experiments yielded significantly reduced MRSA infection in vivo, compared to controls. Several hypotheses were tested to explore the diminished clay antibacterial activity in vivo including: (1) pH and Eh of mineral-bacterial suspensions may differ in wound fluids compared to growth media; (2) antibacterial reactants may complex with components of the wound; (3) hydrated clays may dry out in the wound; and (4) limited dissolved oxygen may reduce Fenton reactions. Ancillary in vitro tests were performed to explore these hypotheses. Results indicate that the clay application to wounds may require enhanced oxidation and possibly a longer treatment regimen. The experimental results foster understanding of the natural clay–bacterial interactions in wounds and may improve designs for medicinal applications.












Similar content being viewed by others
REFERENCES
Behroozian, S., Svensson, S. L., Li, L. Y., & Davies, J. E. (2020). Broad-spectrum antimicrobial and antibiofilm activity of a natural clay mineral from British Columbia. Canada. mBio, 11, e02350–e02320. https://doi.org/10.1128/mBio.02350-20
Caflisch, K.M., Schmidt-Malan, S.M., Mandrekar, J.N., Karau, M.J., Nicklas, J.P., Williams, L.B., & Patel, R. (2018). Antibacterial activity of reduced iron clay against pathogenic bacteria from wound infections. International Journal of Antimicrobial Agents, 52, 692–696.
Cervini-Silva, J., Nieto-Camacho, A., Ramirez-Apan, M. T., Gomez-Vidales, V., Palacios, E., Montoya, A., & Ronquillo de Jesus, E. (2015). Anti-inflammatory, anti-bacterial and cytotoxic activity of fibrous clays. Colloids and Surfaces B: Biointerfaces, 129, 1–6.
Darder, M., Colilla, M., & Ruiz-Hitzky, E. (2003). Biopolymer-clay nanocomposites based on chitosan intercalated in montmorillonite. Chemical Materials, 15, 3774–3780.
Dong, H. (2012). Clay–microbe interactions and implications for environmental mitigation. Elements, 8, 113–118.
Eberl, D.D. (2007). User’s guide to RockJock: A program for determining quantitative mineralogy from powder X-ray diffraction data. U.S. Geological Survey, Open-file report 03–78. 48 pp.
Fomina, M., & Skorochod, I. (2020). Microbial interaction with clay minerals and its environmental and biotechnological implications. Minerals, 10, 861. https://doi.org/10.3390/min10100861
Garcia-Villén, F., Souza, I. M. S., Barbosa, R. M., Borrego-Sánchez, A., Sámcjez-Espejo, R., Ojeda-Riascos, S., & Iborra, C. V. (2020). Natural inorganic ingredients in wound healing. Current Pharmaceutical Design, 26, 621–641.
Gomes, C., Rautureau, M., Niel, J., & Gomes, J. (2021). Clay and clay mineral benefits and risks on human health from ancestral to current time: A synoptic overview. Clays and Clay Minerals (in press).
Haque, S., Nasar, A., & Inamuddin, A. M. A. (2018). Montmorillonite clay nanocomposites for drug delivery. In A. M. A. Inamuddin & M. Ali (Eds.), Applications of Nanocomposite Materials in Drug Delivery. Woodhead Publishing Series in Biomaterials. https://doi.org/10.1016/B978-0-12-813741-3.00039-X
Haydel, S. E., Remenih, C. M., & Williams, L. B. (2008). Broad-spectrum in vitro antibacterial activities of clay minerals against antibiotic-susceptible and antibiotic-resistant bacterial pathogens. Journal of Antimicrobial Chemotherapy, 61353–61361.
Imlay, J. A. (2019). Where in the world do bacteria experience oxidative stress? Environmental Microbiology, 21(2), 521–530.
Jaisi, D. P., Dong, H., Kim, J. W., He, Z., & Morton, J. P. (2007). Nontronite particle aggregation induced by microbial Fe (III). reduction and exopolysaccharide production. Clays and Clay Minerals, 55, 96–107.
Kim, C. K., Karau, M. J., Greenwood-Quaintance, K. E., Tilahun, A. Y., Krogman, A., David, C. S., Pritt, B. S., Patel, R., & Rajagopalan, G. (2015). Superantigen-producing Staphylococcus aureus elicits systemic immune activation in a murine wound colonization model. Toxins (Basel), 7, 5308–5319 PMCID: PMC 4690136.
Komadel, P., Madejová, J., & Stucki, J. W. (1999). Partial stabilization of Fe (II) in reduced ferruginous smectite by Li fixation. Clays and Clay Minerals, 47, 458–465.
Li, G. L., Zhou, C. H., Fiore, S., & Yu, W. H. (2019). Interactions between microorganisms and clay minerals: New insights and broader applications. Applied Clay Science, 177, 91–113.
Londoño, S. C., & Williams, L. B. (2016). Unraveling the antibacterial mode of action of a clay from the Colombian Amazon. Environmental Geochemistry and Health, 38(2), 363–379. https://doi.org/10.1007/s10653-015-9723-y
Londoño, S. C., Hartnett, H., & Williams, L. B. (2017). The antibacterial activity of aluminum in clay from the Colombian Amazon. Environmental Science and Technology, 51, 2401–2408. https://doi.org/10.1021/acs.est.6b04670
Marks, H., Bucknor, A., Roussakis, E., Nowell, N., Kamali, P., Cascales, J. P., Kazei, D., Lin, S. J., & Evans, C. L. (2020). A paintable phosphorescent bandage for postoperative tissue oxygen assessment in DIEP flap reconstruction. Science Advances, 6, eabd1061.
Miller, M. B., & Bassler, B. L. (2001). Quorum sensing in bacteria. Annual Review of Microbiology, 55, 165–199. https://doi.org/10.1146/annurev.micro.55.1.165
Moore, D. M., & Reynolds, R. C. (1997). X-ray Diffraction and the Identification and Analysis of Clay Minerals (2nd ed.). Oxford University Press.
Morrison, K. D., Underwood, J. C., Metge, D. W., Eberl, D. D., & Williams, L. B. (2014). Mineralogical variables that control the antibacterial effectiveness of a natural clay deposit. Environmental Geochemistry and Health, 36(4), 613–631.
Morrison, K. D., Misra, R., & Williams, L. B. (2016). Unearthing the antibacterial mechanism of medicinal clay: A geochemical approach to combating antibiotic resistance. Nature Scientific Reports, 5, 19043. https://doi.org/10.1038/srep19043
Morrison, K. D., Williams, S. N., & Williams, L. B. (2017). The anatomy of an antibacterial clay deposit: A new economic geology. Economic Geology, 112(7), 1551–1570. https://doi.org/10.5382/econgeo.2017.4521
Müller, B. (2015). Experimental interactions between clay minerals and bacteria: A review. Pedosphere, 25(6), 799–810.
Naik, S. P., Sjolin, J., Ching, S., Chi, F., & Herpfer, M. (2018). Quorum sensing disruption in Vibrio harveyi bacteria by clay minerals. Journal of Agricultural and Food Chemistry, 66, 40–44.
Naylor, N. R., Atun, R., Zhu, N., Kulasabanathan, K., Silva, S., Chatterjee, A., Knight, G. M., & Robotham, J. V. (2018). Estimating the burden of antimicrobial resistance: A systematic literature review. Antimicrobial Resistance and Infection Control, 7, 58. https://doi.org/10.1186/s13756-018-0336-y
Ochoa, M., Rahimi, R., Zhou, J., & many others. (2020). Integrated sensing and delivery of oxygen for next-generation smart wound dressings. Microsystems & Nanoengineering, 6, 46. https://doi.org/10.1038/s41378-020-0141-7
Otto, C. C., Kilbourne, J., & Haydel, S. E. (2016). Natural and ion-exchanged illite clays reduce bacterial burden and inflammation in cutaneous methicillin-resistant Staphylococcus aureus infections in mice. Journal of Medical Microbiology, 65, 19–27.
Photos-Jones, E., & Hall, A. J. (2011). Lemnian Earth and the earths of the Aegean, an archaeological guide to medicines, pigments and washing powders (p. 129). Potingair Press, Glasgow, UK
Silhavy, T. J., Kahne, D., & Walker, S. (2010). The bacterial cell envelope. Cold Springs Harbor. Perspectives in Biology, 2010(2), a000414.
Sirvio, L. M., & Grussing, D. M. (1989). The effect of gas permeability of film dressings on wound environment and healing. The Journal of Investigative Dermatology, 93(4), 528–531. https://doi.org/10.1016/B978-1-78242-456-7.00019-2
Valko, M., Morris, H., & Cronin, M. T. D. (2005). Metals, toxicity, and oxidative stress. Current Medicinal Chemistry, 12, 1161–1208.
Wang, X., Dong, H., Zeng, Q., Xia, Q., Zhang, L., & Zhou, Z. (2017). Reduced iron-containing clay minerals as antibacterial agents. Environmental Science and Technology, 51, 7639–7647.
Werthén, M., Henriksson, L., Jensen, P., Sternberg, C., Givskov, M., & Bjarnholt, T. (2010). An in vitro model of bacterial infections in wounds and other soft tissues. Journal of Pathology, Microbiology and Immunology, 118, 156164. https://doi.org/10.1111/j.1600-0463.2009.02580.x
WHO (World Health Organization). (2019). IACG Interagency Coordination Group on Antimicrobial Resistance report to the Secretary General of the United Nations, No time to wait: Securing the future from drug-resistant infections. 25pp. https://www.who.int/antimicrobial-resistance/interagency-coordination-group/final-report/en/
Williams, L. B. (2019). Natural antibacterial clays: Historical uses and modern advances. Clays and Clay Minerals, 67, 7–24.
Williams, L. B. (2021). Antibacterial Clays: Scientific investigation of their practical applications in medicine. Chapter 20. In R. Finkelman, M. Seigel, & O. Selinus (Eds.), Practical Applications of Medical Geology (pp. 671–696. ISBN 978-3-030-53892-7). Springer. https://doi.org/10.1007/978-3-030-53893-4_20
Williams, L. B., & Haydel, S. E. (2010). Evaluation of the medicinal use of clay minerals as antibacterial agents. International Geology Review, 52(7/8), 745–770.
Williams, L. B., Holland, M., Eberl, D. D., Brunet, T., & Brunet de Courssou, L. (2004). Killer Clays! Natural antibacterial clay minerals. Mineralogical Society Bulletin, 139, 3–8.
Williams, L. B., Haydel, S. E., Giese, R. F., & Eberl, D. D. (2008). Chemical and mineralogical characteristics of French green clays used for healing. Clays and Clay Minerals, 56, 437–452.
Williams, L. B., Haydel, S. E., & Ferrell, R. E. (2009). Bentonites, bandaids and borborygmi. Elements, 5(2), 99–102.
Williams, L. B., Metge, D. W., Eberl, D. D., Harvey, R. W., Turner, A. G., Prapaipong, P., & Poret-Peterson, A. T. (2011). What makes natural clays antibacterial? Environmental Science and Technology, 45, 3768–3773.
Winterbourn, C. C. (2008). Reconciling the chemistry and biology of reactive oxygen species. Nature Chemical Biology, 4, 278–286.
Xia, Q., Wang, X., Zeng, Q., Guo, D., Zhu, Z., Chen, H., & Dong, H. (2020). Mechanisms of enhanced antibacterial activity by reduced chitosan-intercalated nontronite. Environmental Science and Technology, 54, 5207–5217.
Yuan, G., & Xiong, Y. (2017). Characterizing the surface charge of clay minerals with Atomic Force Microscopy (AFM). AIMS Materials Science, 4(3), 582–593. https://doi.org/10.3934/matersci.2017.3.582
Zhao, H., Bhattacharjee, S., Chow, R., Wallace, D., Maslinyah, J. H., & Xu, Z. (2008). Probing surface charge potentials of clay basal planes and edges by direct force measurements. Langmuir, 24, 12899–12910. https://doi.org/10.1021/la802112h
ACKNOWLEDGMENTS
The authors acknowledge Oregon Mineral Technologies Inc., for permission to study their clay deposit and thank Susan Selkirk at ASU for figure-drafting assistance. This work was funded by the U.S. National Science Foundation grant EAR-1719325 and by an ASU/Mayo seed grant for in vivo testing.
Funding
Funding sources are as stated in the Acknowledgments.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
The authors declare that they have no conflict of interest.
Additional information
(Received 12 May 2021; revised 7 October 2021; AE: Jin-Ho Choy)
This paper belongs to a special issue on Clay Minerals in Health Applications
Rights and permissions
About this article
Cite this article
Williams, L.B., Schmidt-Malan, S.M. & Patel, R. Preliminary Evaluation of Natural Antibacterial Clays for Treating Wound Infections. Clays Clay Miner. 69, 589–602 (2021). https://doi.org/10.1007/s42860-021-00164-3
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s42860-021-00164-3