Abstract
Objectives
Acute cholecystitis is a complication in critically ill patients. However, a few studies have described its incidence, risk factors, and mortality in patients who underwent cardiovascular surgery. We investigated the incidence, perioperative predictors, and clinical features of acute cholecystitis after cardiovascular surgery.
Methods
This retrospective cohort study examined 7013 patients who underwent cardiovascular surgery between October 2000 and March 2019 at a tertiary care hospital. We collected preoperative, intraoperative, and postoperative data from our database and electronic medical records. The primary outcome was the incidence of postoperative cholecystitis until hospital discharge. A multivariable logistic regression analysis to estimate perioperative predictors of acute cholecystitis was conducted. We described the clinical characteristics of patients complicated with acute cholecystitis.
Results
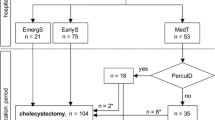
Among the 7013 patients, 51 (0.7%) developed acute cholecystitis. Logistic regression analysis found that circulatory arrest (odds ratio [OR] 1.97; 95% confidence interval [CI] 1.04–3.74; P = 0.037) and intraoperative massive transfusion (OR 2.03; 95% CI 1.03–4.01; P = 0.041) were associated with the incidences of cholecystitis. In-hospital mortality was significantly higher in the cholecystitis group than in the non-cholecystitis group (13.7% vs 3.9%, P = 0.004). Aortic disease was more frequent in the cholecystitis group (54.9% vs 38.6%, P = 0.021). The median time of acute cholecystitis onset from surgery was 12.5 days (interquartile range 7.0–27.75). Twenty-six patients (51.0%) developed asymptomatic cholecystitis.
Conclusions
Approximately 1% of patients who underwent cardiovascular surgery developed postoperative cholecystitis; half of them were asymptomatic. Since cholecystitis is associated with high mortality, it is a complication after cardiovascular surgery that needs to be considered.

Similar content being viewed by others
References
Laurila J, Syrjala H, Laurila PA, Saarnio J, Ala-Kokko TI. Acute acalculous cholecystitis in critically ill patients. Acta Anaesthesiol Scand. 2004;48(8):986–91.
Pelinka LE, Schmidhammer R, Hamid L, Mauritz W, Redl H. Acute acalculous cholecystitis after trauma: a prospective study. J Trauma. 2003;55(2):323–9.
Walsh K, Goutos I, Dheansa B. Acute acalculous cholecystitis in burns: a review. J Burn Care Res. 2018;39(5):724–8.
Inoue T, Mishima Y. Postoperative acute cholecystitis: a collective review of 494 cases in Japan. Jpn J Surg. 1988;18(1):35–42.
Huffman JL, Schenker S. Acute acalculous cholecystitis: a review. Clin Gastroenterol Hepatol. 2010;8(1):15–22.
Kalliafas S, Ziegler DW, Flancbaum L, Choban PS. Acute acalculous cholecystitis: incidence, risk factors, diagnosis, and outcome. Am Surg. 1998;64(5):471–5.
McChesney JA, Northup PG, Bickston SJ. Acute acalculous cholecystitis associated with systemic sepsis and visceral arterial hypoperfusion: a case series and review of pathophysiology. Dig Dis Sci. 2003;48(10):1960–7.
Orlando R 3rd, Gleason E, Drezner AD. Acute acalculous cholecystitis in the critically ill patient. Am J Surg. 1983;145(4):472–6.
Rady MY, Kodavatiganti R, Ryan T. Perioperative predictors of acute cholecystitis after cardiovascular surgery. Chest. 1998;114(1):76–84.
Passage J, Joshi P, Mullany DV. Acute cholecystitis complicating cardiac surgery: case series involving more than 16,000 patients. Ann Thorac Surg. 2007;83(3):1096–101.
Karkouti K, O’Farrell R, Yau TM, Beattie WS, Reducing Bleeding in Cardiac Surgery Research G. Prediction of massive blood transfusion in cardiac surgery. Can J Anaesth. 2006;53(8):781–94.
Delaney M, Stark PC, Suh M, Triulzi DJ, Hess JR, Steiner ME, et al. Massive transfusion in cardiac surgery: the impact of blood component ratios on clinical outcomes and survival. Anesth Analg. 2017;124(6):1777–82.
Yokoe M, Hata J, Takada T, Strasberg SM, Asbun HJ, Wakabayashi G, et al. Tokyo guidelines 2018: diagnostic criteria and severity grading of acute cholecystitis (with videos). J Hepatobiliary Pancreat Sci. 2018;25(1):41–54.
Ansaloni L, Pisano M, Coccolini F, Peitzmann AB, Fingerhut A, Catena F, et al. 2016 WSES guidelines on acute calculous cholecystitis. World J Emerg Surg. 2016;11:25.
Trowbridge RL, Rutkowski NK, Shojania KG. Does this patient have acute cholecystitis? JAMA. 2003;289(1):80–6.
Fuks D, Mouly C, Robert B, Hajji H, Yzet T, Regimbeau JM. Acute cholecystitis: preoperative CT can help the surgeon consider conversion from laparoscopic to open cholecystectomy. Radiology. 2012;263(1):128–38.
Maekawa Y, Abe S, Yoshimura Y, Uchida T, Kim C, Kuroda Y, et al. Clinical characteristics of biliary tract infection and acalculous cholecystitis after cardiovascular surgery. Kyobu Geka. 2014;67(12):1039–43 (discussion 43–6).
Laurila JJ, Ala-Kokko TI, Laurila PA, Saarnio J, Koivukangas V, Syrjala H, et al. Histopathology of acute acalculous cholecystitis in critically ill patients. Histopathology. 2005;47(5):485–92.
Andersson B, Nilsson J, Brandt J, Hoglund P, Andersson R. Gastrointestinal complications after cardiac surgery. Br J Surg. 2005;92(3):326-33.
Filsoufi F, Rahmanian PB, Castillo JG, Scurlock C, Legnani PE, Adams DH. Predictors and outcome of gastrointestinal complications in patients undergoing cardiac surgery. Ann Surg. 2007;246(2):323-9.
Kumral E, Yuksel M, Buket S, Yagdi T, Atay Y, Guzelant A. Neurologic complications after deep hypothermic circulatory arrest: types, predictors, and timing. Tex Heart Inst J. 2001;28(2):83–8.
Zanardo G, Michielon P, Paccagnella A, Rosi P, Calo M, Salandin V, et al. Acute renal failure in the patient undergoing cardiac operation. Prevalence, mortality rate, and main risk factors. J Thorac Cardiovasc Surg. 1994;107(6):1489–95.
Cooper WA, Duarte IG, Thourani VH, Nakamura M, Wang NP, Brown WM 3rd, et al. Hypothermic circulatory arrest causes multisystem vascular endothelial dysfunction and apoptosis. Ann Thorac Surg. 2000;69(3):696–702 (discussion 3).
Croome KP, Kiaii B, Fox S, Quantz M, McKenzie N, Novick RJ. Comparison of gastrointestinal complications in on-pump versus off-pump coronary artery bypass grafting. Can J Surg. 2009;52(2):125–8.
De Backer D, Dubois MJ, Schmartz D, Koch M, Ducart A, Barvais L, et al. Microcirculatory alterations in cardiac surgery: effects of cardiopulmonary bypass and anesthesia. Ann Thorac Surg. 2009;88(5):1396–403.
Lindberg EF, Grinnan GL, Smith L. Acalculous cholecystitis in Viet Nam casualties. Ann Surg. 1970;171(1):152–7.
Toursarkissian B, Kearney PA, Holley DT, Cheung R, Fried A, Strodel WE. Biliary sludging in critically ill trauma patients. South Med J. 1995;88(4):420–4.
Petersen SR, Sheldon GF. Acute acalculous cholecystitis: a complication of hyperalimentation. Am J Surg. 1979;138(6):814–7.
Guglielmi FW, Regano N, Mazzuoli S, Fregnan S, Leogrande G, Guglielmi A, et al. Cholestasis induced by total parenteral nutrition. Clin Liver Dis. 2008;12(1):97–110 (viii).
Saito A, Shirai Y, Ohzeki H, Hayashi J, Eguchi S. Acute acalculous cholecystitis after cardiovascular surgery. Surg Today. 1997;27(10):907–9.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
None.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Kamei, J., Kuriyama, A., Shimamoto, T. et al. Incidence and risk factors of acute cholecystitis after cardiovascular surgery. Gen Thorac Cardiovasc Surg 70, 611–618 (2022). https://doi.org/10.1007/s11748-021-01751-w
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11748-021-01751-w