Abstract
Purpose
The role of oxidative stress in the pathogenesis of pterygium is still unclear. However, abnormal thiol disulfide homeostasis levels are involved in the pathogenesis of various systemic or ocular diseases. We aim to analyze dynamic thiol disulphide homeostasis in patients suffering from conjunctival pterygium using a contemporary technique.
Methods
Thirty-eight subjects suffering from pterygium and 35 age-gender matched healthy volunteers were recruited for the study. For each case, total thiol, disulfide and native thiol levels in blood were obtained. Additionally, the ratio of disulfide over total thiol, native thiol over total thiol and disulfide over native thiol were computed.
Results
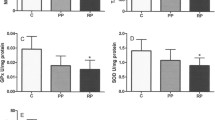
The level of median native thiol was lower in pterygium group (318.2 µmol/L vs. 333.4 µmol/L) and median disulfide was slightly higher in pterygium group (24.3 µmol/L vs. 22.8 µmol/L) compared to control group. Both disulfide over total thiol and disulfide over native thiol ratios were higher in pterygium group, ratio of native thiol over total thiol was found to be higher in control group. Nevertheless, none of those differences were statistically significant at 95% confidence level. Notably, correlation test pointed to a negative correlation both between pterygium grade and native thiol and between total thiol and pterygium grade in pterygium group (P = 0.03 and 0.02, respectively).
Conclusion
A negative correlation hinting that slightly weakened dynamic thiol disulphide homeostasis in subjects with pterygium, a local ocular disease. Further studies with larger sample sizes may shed light on this potential relationship and justify systemic antioxidant therapies in these cases.
Similar content being viewed by others
Data availability
The datasets generated and/or analyzed during the present study are not publicly available (obtained from Duzce University Hospital, Duzce repository), but are available from the corresponding author upon reasonable request.
References
Malozhen SA, Trufanov SV, Krakhmaleva DA (2017) Pterygium: etiology, pathogenesis, treatment. Vestn Oftalmol 133(5):76–83. https://doi.org/10.17116/oftalma2017133576-83
Wanzeler ACV, Barbosa IAF, Duarte B, Borges D, Barbosa EB, Kamiji D, Huarachi DRG, Melo MB, Alves M (2019) Mechanisms and biomarker candidates in pterygium development. Arq Bras Oftalmol 82(6):528–536. https://doi.org/10.5935/0004-2749.20190103
Chui J, Di Girolamo N, Wakefield D, Coroneo MT (2008) The pathogenesis of pterygium: current concepts and their therapeutic implications. Ocul Surf 6(1):24–43. https://doi.org/10.1016/s1542-0124(12)70103-9
Comini MA (2016) Measurement and meaning of cellular thiol:disufhide redox status. Free Radic Res 50(2):246–271. https://doi.org/10.3109/10715762.2015.1110241
Moriarty-Craige SE, Jones DP (2004) Extracellular thiols and thiol/disulfide redox in metabolism. Annu Rev Nutr 24:481–509. https://doi.org/10.1146/annurev.nutr.24.012003.132208
Sen CK (2000) Cellular thiols and redox-regulated signal transduction. Curr Top Cell Regul 36:1–30. https://doi.org/10.1016/s0070-2137(01)80001-7
Deneke SM (2000) Thiol-based antioxidants. Curr Top Cell Regul 36:151–180. https://doi.org/10.1016/s0070-2137(01)80007-8
Tetikoğlu M, Aktas S, Sağdik HM, Özcura F, Uçar F, Koçak H, Neşelioğlu S, Erel Ö (2017) Thiol disulfide homeostasis in pseudoexfoliation syndrome. Curr Eye Res 42(6):876–879. https://doi.org/10.1080/02713683.2016.1256412
Gulpamuk B, Elgin U, Sen E, Yilmazbas P, Neselioglu S, Erel O (2020) Evaluation of dynamic thiol-disulfide homeostasis in glaucoma patients and the correlation with retinal nerve fiber layer analysis. Eur J Ophthalmol 30(4):690–699. https://doi.org/10.1177/1120672119839582
Gulpamuk B, Koç M, Karatepe MS, Yildiz A, Erel O, Neselioglu S, Yilmazbas P (2017) Novel assay assessment of oxidative stress biomarkers in patients with keratoconus: thiol-disulfide homeostasis. Curr Eye Res 42(9):1215–1219. https://doi.org/10.1080/02713683.2017.1302592
Elbay A, Ozer OF, Altinisik M, Elbay AE, Sezer T, Bayraktar H, Ozdemir H (2017) A novel tool reflecting the role of oxidative stress in the cataracts: thiol/disulfide homeostasis. Scand J Clin Lab Invest 77(3):223–227. https://doi.org/10.1080/00365513.2017.1292539
Turkoglu EB, Dikci S, Çelik E, Erel Ö, Neselioglu S, Alışık M, Koca C (2016) Thiol/disulfide homeostasis in patients with central serous chorioretinopathy. Curr Eye Res 41(11):1489–1491. https://doi.org/10.3109/02713683.2015.1127390
ArıkanYorgun M, Toklu Y, Altınkaynak H, Tanrıverdi B, Ergin M, Biçer C (2016) A novel tool for the assessment oxidative stress in age-related macular degeneration: thiol/disulfide homeostasis revisited. Curr Eye Res 41(12):1584–1589. https://doi.org/10.3109/02713683.2016.1141965
Tan DT, Chee SP, Dear KB, Lim AS (1997) Effect of pterygium morphology on pterygium recurrence in a controlled trial comparing conjunctival autografting with bare sclera excision. Arch Ophthalmol 115(10):1235–1240. https://doi.org/10.1001/archopht.1997.01100160405001
Erel O, Neselioglu S (2014) A novel and automated assay for thiol/disulphide homeostasis. Clin Biochem 47(18):326–332. https://doi.org/10.1016/j.clinbiochem.2014.09.026
Kormanovski A, Parra F, Jarillo-Luna A, Lara-Padilla E, Pacheco-Yépez J, Campos-Rodriguez R (2014) Oxidant/antioxidant state in tissue of primary and recurrent pterygium. BMC Ophthalmol 14:149. https://doi.org/10.1186/1471-2415-14-149
Perra MT, Maxia C, Corbu A, Minerba L, Demurtas P, Colombari R, Murtas D, Bravo S, Piras F, Sirigu P (2006) Oxidative stress in pterygium: relationship between p53 and 8-hydroxydeoxyguanosine. Mol Vis 12:1136–1142 (PMID: 17093398)
Sun N, Zhang H (2018) Pyroptosis in pterygium pathogenesis. Biosci Rep 38(3):BSR20180282. 10.1042/BSR20180282
Peiretti E, Mandas A, Cocco P, Norfo C, Abete C, Angius F, Pani A, Vascellari S, Del Fiacco G, Cannas D, Diaz G, Dessì S, Fossarello M (2010) Glucose-6-phosphate-dehydrogenase deficiency as a risk factor for pterygium. Invest Ophthalmol Vis Sci 51(6):2928–2935. https://doi.org/10.1167/iovs.09-4426
Ahmad A, Ahsan H (2020) Biomarkers of inflammation and oxidative stress in ophthalmic disorders. J Immunoassay Immunochem 41(3):257–271. https://doi.org/10.1080/15321819.2020.1726774
Dogru M, Kojima T, Simsek C, Tsubota K (2018). Potential role of oxidative stress in ocular surface inflammation and dry eye disease. Invest Ophthalmol Vis Sci 59(14): DES163-DES168. https://doi.org/10.1167/iovs.17-23402
Longstreth J, de Gruijl FR, Kripke ML, Abseck S, Arnold F, Slaper HI, Velders G, Takizawa Y, van der Leun JC (1998) Health risks. J Photochem Photobiol B 46(1–3):20–39. https://doi.org/10.1016/s1011-1344(98)00183-3
Balci M, Sahin S, Mutlu FM, Yağci R, Karanci P, Yildiz M (2011) Investigation of oxidative stress in pterygium tissue. Mol Vis 17:443–447 (PMID: 21321673)
Kurtul BE, Kabatas EU, Ozates S (2019) The correlation of routine hematological indices with pterygium. Ther Adv Ophthalmol 11:2515841419848922. https://doi.org/10.1177/2515841419848922
Rasool M, Malik A, Abdul Basit Ashraf M, Arooj M, Kiran A, Waquar S, Ayyaz U, Zahid A, Zaheer A, Jabbar A, Zain M, Raza A, Mehmood A, BatoolQaisrani T, Mirza Z, Hussein Al-Qahtani M, Karim S, Haque A (2018) Role of diagnostic factors associated with antioxidative status and expression of matrix metalloproteinases (MMPs) in patients with cancer therapy induced ocular disorders. Saudi J Biol Sci 25(8):1724–1728. https://doi.org/10.1016/j.sjbs.2018.08.009
Kilic-Toprak E, Toprak I, Caliskan S, Ozdemir Y, Demirtas O, Altintas F, Kucukatay V (2019) Oxidative stress and genotoxicity in pterygium: a systemic investigation. Eye Contact Lens 45(6):399–404. https://doi.org/10.1097/ICL.0000000000000620
Erel Ö, Erdoğan S (2020), Thiol-disulfide homeostasis: an integrated approach with biochemical and clinical aspects. Turk J Med Sci, 50(SI-2): 1728–1738. https://doi.org/10.3906/sag-2003-64
Erenler AK, Yardan T (2017) Clinical utility of thiol/disulfide homeostasis. Clin Lab 63(5):867–870. https://doi.org/10.7754/Clin.Lab.2017.161117
Acknowledgements
All biochemical tests within the study were carried out at the biochemistry laboratory of Ankara Yıldırım Beyazıt University School of Medicine. The authors are thankful for the amazing assistance of Ozcan Erel’s research fellows.
Funding
This research did not receive any specific grants from funding agencies in the public, commercial, or not-for-profit sectors.
Author information
Authors and Affiliations
Contributions
HTA-Primary consultant to do the procedure, data acquisition, data interpretation, statistical analysis, manuscript submission, and coordination; OE-performing laboratory tests, data acquisition, supervision, data, and manuscript editing.
Corresponding author
Ethics declarations
Conflict of interest
The author declared that there is no conflict of interest.
Ethics approval
The Institutional Review Board of the Duzce University, Duzce, Turkey approved this study (IRB: 2019/152). All procedures adhered to the Declaration of Helsinki and HIPAA rules and were conducted in accordance with the approved protocol.
Animal Research
This article does not contain any studies with animals performed by any of the authors.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Consent to participate
Yes, obtained.
Consent to Publish
Yes, obtained.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Akcam, H.T., Erel, O. Dynamic thiol disulphide homeostasis in patients with surfer’s eye: a case–control study. Int Ophthalmol 42, 653–659 (2022). https://doi.org/10.1007/s10792-021-02125-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10792-021-02125-0