Abstract
Objectives
Metastasectomy is often the local treatment for pulmonary metastases arising from osteosarcoma or soft tissue sarcoma. However, there have been few investigations on the outcomes of patients who undergo this procedure. In this study, we identified prognostic factors in patients with pulmonary metastases arising from osteosarcoma and soft tissue sarcoma to determine more appropriate eligibility criteria for metastasectomy.
Methods
We retrospectively examined 37 patients who underwent metastasectomy of pulmonary nodules arising from osteosarcomas or soft tissue sarcomas at our institute between 2005 and 2020. Overall and recurrence-free survival intervals were determined using univariate and multivariate analyses.
Results
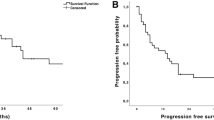
A tumor doubling time > 1 month and a primary tumor histological type of osteosarcoma were independent predictors of longer overall survival on multivariate analysis (hazard ratios: 3.618 and 2.979, p = 0.00986 and 0.0373, respectively). Moreover, a > 1-month tumor doubling time and > 10-cm diameter of the primary tumor were independent predictors of longer recurrence-free survival (hazard ratios: 3.293 and 2.67, p = 0.0121 and 0.0134, respectively). Patients who underwent repeat pulmonary metastasectomy after complete resection of sarcoma-derived pulmonary metastases had significantly longer overall survival than those who did not (median: 5.91 years vs. 0.81 years, p < 0.0001).
Conclusions
Tumor doubling time is a significant predictor of clinical outcomes in patients who undergo resection of pulmonary metastases originating from sarcomas. The surgical indication for this procedure should be decided carefully, particularly for patients with metastatic lesion doubling times ≤ 1 month.



Similar content being viewed by others
References
Digesu CS, Wiesel O, Vaporciyan AA, Colson YL. Management of sarcoma metastases to the lung. Surg Oncol Clin N Am. 2016;25:721–33.
Marulli G, Mammana M, Comacchio G, Rea F. Survival and prognostic factors following pulmonary metastasectomy for sarcoma. J Thorac Dis. 2017;9(Suppl 12):S1305–15.
Mizuno T, Taniguchi T, Ishikawa Y, Kawaguchi K, Fukui T, Ishiguro F, et al. Pulmonary metastasectomy for osteogenic and soft tissue sarcoma: who really benefits from surgical treatment? Eur J Cardiothoracic Surg. 2013;43:795–9.
Yamamoto Y, Kanzaki R, Kanou T, Ose N, Funaki S, Shintani Y, et al. Long-term outcomes and prognostic factors of pulmonary metastasectomy for osteosarcoma and soft tissue sarcoma. Int J Clin Oncol. 2019;24:863–70.
Wigge S, Heißner K, Steger V, Ladurner R, Traub F, Sipos B, et al. Impact of surgery in patients with metastatic soft tissue sarcoma: a monocentric retrospective analysis. J Surg Oncol. 2018;118:167–76.
Schwartz M. A biomathematical approach to clinical tumor growth. Cancer. 1961;14:1272–94.
Ozono S, Miyao N, Igarashi T, Marumo K, Nakazawa H, Fukuda M, et al. Tumor doubling time of renal cell carcinoma measured by CT: collaboration of Japanese society of renal cancer. Jpn J Clin Oncol. 2004;34:82–5.
Kanda Y. Investigation of the freely available easy-to-use software “EZR” for medical statistics. Bone Marrow Transplant. 2013;48:452–8.
Tomimaru Y, Noura S, Ohue M, Okami J, Oda K, Higashiyama M, et al. Metastatic tumor doubling time is an independent predictor of intrapulmonary recurrence after pulmonary resection of solitary pulmonary metastasis from colorectal cancer. Dig Surg. 2008;25:220–5.
Nakamura T, Matsumine A, Takao M, Nakatsuka A, Matsubara T, Asanuma K, et al. Impact of tumor volume doubling time on post-metastatic survival in bone or soft-tissue sarcoma patients treated with metastasectomy and/or radiofrequency ablation of the lung. Onco Targets Ther. 2017;10:559–64.
Lin AY, Kotova S, Yanagawa J, Elbuluk O, Wang G, Kar N, et al. Risk stratification of patients undergoing pulmonary metastasectomy for soft tissue and bone sarcomas. J Thorac Cardiovasc Surg. 2015;149:85–92.
Navarria P, Ascolese AM, Cozzi L, Tomatis S, D’Agostino G, De Rose F, et al. Stereotactic body radiation therapy for lung metastases from soft tissue sarcoma. Eur J Cancer. 2015;51:668–74.
Baumann BC, Nagda SN, Kolker JD, Levin WP, Weber KL, Berman AT, et al. Efficacy and safety of stereotactic body radiation therapy for the treatment of pulmonary metastases from sarcoma: a potential alternative to resection. J Surg Oncol. 2016;114:65–9.
Dhakal S, Corbin KS, Milano MT, Philip A, Sahasrabudhe D, Jones C, et al. Stereotactic body radiotherapy for pulmonary metastases from soft-tissue sarcomas: excellent local lesion control and improved patient survival. Int J Radiat Oncol Biol Phys. 2012;82:940–5.
Funding
No funding was received for this study.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
Akiisa Omura, Toru Kimura, Ryo Tanaka, Takashi Hiroshima, Tomohiro Maniwa, Satoshi Takenaka, Norifumi Naka, and Jiro Okami declare no conflicts of interest in association with the present study.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Omura, A., Kimura, T., Tanaka, R. et al. Surgical indication of pulmonary metastasis arising from osteosarcoma or soft tissue sarcoma. Gen Thorac Cardiovasc Surg 70, 273–279 (2022). https://doi.org/10.1007/s11748-021-01726-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11748-021-01726-x