Abstract
Purpose
To investigate if comorbidity predicts mortality and functional impairment in middle-aged individuals with cancer (50–64 years) as compared to older individuals.
Methods
A prospective cohort study. Outcomes were mortality and functional impairment at 5 years follow-up. Comorbidity was assessed using adjusted Charlson comorbidity index and polypharmacy (≥ 5 drugs) as surrogate for comorbidity. Multivariate Cox-proportional hazards and binary logit models were used to assess the risk of 5-year mortality and functional impairment respectively.
Results
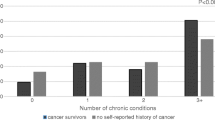
We included 477 middle-aged (50–64 years) and 563 older (65 + years) individuals with cancer. The prevalence of comorbidity (at least one disease in addition to cancer) was 29% for middle-aged and 45% for older individuals, with polypharmacy observed in 15% and 31% respectively. Presence of ≥ 3 comorbidities was associated with nearly three times as high a risk of mortality in middle-aged individuals (HR 2.97, 95% CI: 1.43–6.16). In older individuals, the HR was 1.7 (95% CI 1.1–2.8). Polypharmacy was associated with a higher risk of mortality in middle-aged (HR 2.35, 95% CI 1.32–4.16) but not in older individuals (HR 1.2, 95% CI 0.9–1.8). Polypharmacy was associated with the four time the risk of functional impairment in middle-aged (OR 4.0, 95% CI 1.59–10.06) and older individuals (OR 4.4, 95% CI 1.6–11.7).
Conclusion
This study of middle-aged and older adults with cancer shows that comorbid disease is common in younger and older individuals with cancer and are associated with inferior outcomes. Assessment and management of comorbidity should be a priority for cancer care across all age groups.



Similar content being viewed by others
Data availability
Data are available on reasonable request.
Code availability
Code is available upon request.
References
Sarfati D, Koczwara B, Jackson C (2016) The impact of comorbidity on cancer and its treatment. CA Cancer J Clin 66(4):337–350. https://doi.org/10.3322/caac.21342
Ng HS, Koczwara B, Roder D, Vitry A (2018) Changes in the prevalence of comorbidity in the Australian population with cancer, 2007–2014. Cancer Epidemiol 54:56–62. https://doi.org/10.1016/j.canep.2018.03.010
Ritchie CS, Kvale E, Fisch MJ (2011) Multimorbidity: an Issue of Growing Importance for Oncologists. J Oncol Pract 7(6):371–374. https://doi.org/10.1200/JOP.2011.000460
Jack E, Maskrey N, Byng R (2018) SHERPA: a new model for clinical decision making in patients with multimorbidity. Lancet 392:1397–1399. https://doi.org/10.1016/S0140-6736(18)31371-0
Webster S, Lawn S, Chan R et al (2020) The role of comorbidity assessment in guiding treatment decision-making for women with early breast cancer: a systematic literature review. Support Care Cancer 28:1041–1050. https://doi.org/10.1007/s00520-019-05218-w
Li D, Sun C-L, Kim H, Chung V, Koczywas M, Fakih M et al (2020) Geriatric assessment-driven intervention (GAIN) on chemotherapy toxicity in older adults with cancer: a randomized controlled trial. J Clin Oncol 38(15_suppl):12010. https://doi.org/10.1200/JCO.2020.38.15_suppl.12010
Extermann M, Boler I, Reich R, Lyman GH, Brown RH, DeFelice J et al (2010) The Chemotherapy Risk Assessment Scale for High-Age Patients (CRASH) score: design and validation. J Clin Oncol 28(15_suppl):9000. https://doi.org/10.1200/jco.2010.28.15_suppl.9000
Wildiers H, Heeren P, Puts M, Topinkova E, Janssen-Heijnen MLG, Extermann M et al (2014) International Society of Geriatric Oncology Consensus on Geriatric Assessment in Older Patients With Cancer. J Clin Oncol 32(24):2595–603. https://doi.org/10.1200/JCO.2013.54.8347
Yancik R, Wesley MN, Ries LA, Havlik RJ, Edwards BK, Yates JW (2001) Effect of age and comorbidity in postmenopausal breast cancer patients aged 55 years and older. JAMA 285(7):885–92. https://doi.org/10.1001/jama.285.7.885
Hanlon P, Nicholl BI, Jani BD et al (2018) Frailty and pre-frailty in middle-aged and older adults and its association with multimorbidity and mortality: a prospective analysis of 493 737 UK Biobank participants. Lancet Public Health 3:e323-32. https://doi.org/10.1016/S2468-2667(18)30091-4
de Vries S, Schaapveld M, Janus CPM et al (2021) Long-term cause-specific mortality in hodgkin lymphoma patients. J Natl Cancer Inst 113(6):760–769. https://doi.org/10.1093/jnci/djaa194
Deckx L, van Abbema D, Nelissen K et al (2011) Study protocol of KLIMOP: a cohort study on the wellbeing of older cancer patients in Belgium and the Netherlands. BMC Public Health 11:825. https://doi.org/10.1186/1471-2458-11-825
Charlson ME, Pompei P, Ales KL, MacKenzie CR (1987) A new method of classification of prognostic comorbidity for longitudinal studies: development and validation. J Chronic Dis 40(5):373–383. https://doi.org/10.1016/0021-9681(87)90171-8
Masnoon N, Shakib S, Kalisch-Ellett L, Caughey GE (2017) What is polypharmacy? A systematic review of definitions. BMC Geriatr 10;17(1):230. https://doi.org/10.1186/s12877-017-0621-2
Katz S (1983) Assessing self-maintenance: activities of daily living, mobility and instrumental activities of daily living. J Am Geriatr Soc 31(12):721–726. https://doi.org/10.1111/j.1532-5415.1983.tb03391.x
Lawton MP, Brody EM (1969) Assessment of older people: self-maintaining and instrumental activities of daily living. Gerontologist 9(3):179–186
Deckx L, van Abbema DL, van den Akker M et al (2015) A cohort study on the evolution of psychosocial problems in older patients with breast or colorectal cancer: comparison with younger cancer patients and older primary care patients without cancer. BMC Geriatr 15:79
Deckx L, van den Akker M, Daniels L et al (2015) Geriatric screening tools are of limited value to predict decline in functional status and quality of life: results of a cohort study. BMC Fam Pract 16:30
Fowler H, Belot A, Ellis L et al (2020) Comorbidity prevalence among cancer patients: a population-based cohort study of four cancers. BMC Cancer 20:2. https://doi.org/10.1186/s12885-019-6472-9
Luque-Fernandez MA, Redondo Sánchez D, Rodriguez-Barranco M, CarmonaGarcia MC, Marcos-Gragera R, Sanchez-Perez MJ (2020) Multimorbidity by patient and tumor factors and time-to-surgery among colorectal cancer patients in Spain: a population-based study. Clin Epidemiol 12(31–40):20. https://doi.org/10.2147/CLEP.S229935
Sarfati D, Gurney J, Lim BT, Bagheri N, Simpson A, Koea J et al (2016) Identifying important comorbidity among cancer populations using administrative data: prevalence and impact on survival. Asia Pac J Clin Oncol 12(1):e47-56. https://doi.org/10.1111/ajco.12130
Barnett K, Mercer SW, Norbury M, Watt G, Wyke S, Guthrie B (2012) Epidemiology of multimorbidity and implications for health care, research, and medical education: a cross-sectional study. Lancet 380:37–43. https://doi.org/10.1016/S0140-6736(12)60240-2
Schenker Y, Park SY, Jeong K et al (2019) Associations between polypharmacy, symptom burden, and quality of life in patients with advanced, life-limiting illness. J Gen Intern Med 34(4):559–566
Overcash J, Cope DG, Van Cleave JH (2018) (2018) Frailty in Older Adults: Assessment, Support, and Treatment Implications in Patients With Cancer. Clin J Oncol Nurs 22(6):8–18. https://doi.org/10.1188/18.CJON.S2.8-18.10.1188/18.CJON.S2.8-18
Mohile SG, Dale W, Sommerfield MR et al (2018) (2018) Practical Assessment and Management of Vulnerabilities in Older Patients Receiving Chemotherapy: ASCO Guideline for Geriatric Oncology. J Clin Onc 36(22):2326–2347. https://doi.org/10.1200/JCO.2018.78.8687
Cupit-Link MC, Kirkland JL, Ness KK, Armstrong GT, Tchkonia T, LeBrasseur NK, Armenian SH, Ruddy KJ, Hashmi SK (2017) Biology of premature ageing in survivors of cancer. ESMO Open 2(5):e000250. https://doi.org/10.1136/esmoopen-2017-000250
Funding
This study is funded by the European Union/Interreg IV Grensregio Vlaanderen-Nederland (IVA-VLANED-3.46) and Kom op tegen Kanker (Stand up to Cancer–the Flemish cancer league) (10482)).
Author information
Authors and Affiliations
Contributions
All authors contributed to the conceptualization, formal analysis, methodology, and writing.
Corresponding author
Ethics declarations
Ethics approval
The Ethical Review Board of KU Leuven and UZ Leuven (S52097–ML6279) and the Maastricht University Medical Centre (NL31414.068.10) approved the study protocol.
Consent to participate
All individuals signed informed consent.
Consent for publication
All authors granted the consent to publish the manuscript.
Conflict of interest
Laura Deckx is currently employed by Kom op tegen Kanker who partially funded this study. However, at the time of the data collection, Laura was not employed at Kom op tegen Kanker and was not the investigator on the original grant.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Koczwara, B., Deckx, L., Ullah, S. et al. Impact of comorbidities on physical function and survival of middle-aged, as compared to older, individuals with cancer. Support Care Cancer 30, 1625–1632 (2022). https://doi.org/10.1007/s00520-021-06567-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00520-021-06567-1