Abstract
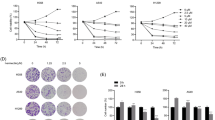
Cholangiocarcinoma (CCA) is an aggressive bile duct cancer. Opisthorchis viverrini (O. viverrini) infection is a significant cause of CCA in the Greater Mekong subregion. Currently, there is no standard chemotherapeutic regimen for CCA. A unique hamster carcinogenesis model of O. viverrini–associated CCA was established. Molecular targets identified from the hamster CCA-comparative model are valuable for target identification and validation. Hamster CCA was induced by the administration of O. viverrini metacercariae and N-nitrosodimethylamine. Hamster-derived cancer cells were isolated and continuously cultured for more than 6 months. Ham-2 cell line was established and characterized in vitro and in vivo. Ham-2 exhibited chromosome hyperploidy. A comparative study with previously established cell line, Ham-1, demonstrated that Ham-2 acquired slower growth, higher adhesion, higher migration, and resistance to doxorubicin and 5-fluorouracil (5-FU). In BALB/c Rag-2/Jak3 double-deficient (BRJ) mice, Ham-2 subcutaneous transplantation formed mucin-producing cancers, which morphologically resemble human tubular cholangiocarcinoma. Intravenous-injected Ham-2 established the metastatic nodules in the lungs and livers of BRJ mice. Altogether, a new hamster cholangiocarcinoma cell line, Ham-2, which acquired more aggressive phenotypes in vitro and in vivo, was established. This cell line might be a valuable tool for comparative drug target identification and validation.





Similar content being viewed by others
References
Abou-Rebyeh H, Al-Abadi H, Jonas S, Rotter I, Bechstein WO, Neuhaus P (2002) DNA analysis of cholangiocarcinoma cells: prognostic and clinical importance. Cancer Detect Prev 26:313–319
Baldus SE, Engelmann K, Hanisch FG (2004) MUC1 and the MUCs: a family of human mucins with impact in cancer biology. Crit Rev Clin Lab Sci 41:189–231
Banales JM, Cardinale V, Carpino G, Marzioni M, Andersen JB, Invernizzi P, Lind GE, Folseraas T, Forbes SJ, Fouassier L, Geier A, Calvisi DF, Mertens JC, Trauner M, Benedetti A, Maroni L, Vaquero J, Macias RI, Raggi C, Perugorria MJ, Gaudio E, Boberg KM, Marin JJ, Alvaro D (2016) Expert consensus document: cholangiocarcinoma: current knowledge and future perspectives consensus statement from the European Network for the Study of Cholangiocarcinoma (ENS-CCA). Nat Rev Gastroenterol Hepatol 13:261–280
Banales JM, Marin JJG, Lamarca A, Rodrigues PM, Khan SA, Roberts LR, Cardinale V, Carpino G, Andersen JB, Braconi C, Calvisi DF, Perugorria MJ, Fabris L, Boulter L, Macias RIR, Gaudio E, Alvaro D, Gradilone SA, Strazzabosco M, Marzioni M, Coulouarn C, Fouassier L, Raggi C, Invernizzi P, Mertens JC, Moncsek A, Rizvi S, Heimbach J, Koerkamp BG, Bruix J, Forner A, Bridgewater J, Valle JW, Gores GJ (2020) Cholangiocarcinoma 2020: the next horizon in mechanisms and management. Nat Rev Gastroenterol Hepatol 17:557–588
Blechacz B (2017) Cholangiocarcinoma: current knowledge and new developments. Gut Liver 11:13–26
Boonjaraspinyo S, Wu Z, Boonmars T, Kaewkes S, Loilome W, Sithithaworn P, Nagano I, Takahashi Y, Yongvanit P, Bhudhisawasdi V (2012) Overexpression of PDGFA and its receptor during carcinogenesis of Opisthorchis viverrini-associated cholangiocarcinoma. Parasitol Int 61:145–150
Boonla C, Wongkham S, Sheehan JK, Wongkham C, Bhudhisawasdi V, Tepsiri N, Pairojkul C (2003) Prognostic value of serum MUC5AC mucin in patients with cholangiocarcinoma. Cancer 98:1438–1443
Dana P, Kariya R, Vaeteewoottacharn K, Sawanyawisuth K, Seubwai W, Matsuda K, Okada S, Wongkham S (2017) Upregulation of CD147 promotes metastasis of cholangiocarcinoma by modulating the epithelial-to-mesenchymal transitional process. Oncol Res 25:1047–1059
Danese E, Ruzzenente A, Montagnana M, Lievens PM (2018) Current and future roles of mucins in cholangiocarcinoma-recent evidences for a possible interplay with bile acids. Ann Transl Med 6:333
Hall PA, Coates PJ, Goodlad RA, Hart IR, lane DP, (1994) Proliferating cell nuclear antigen expression in non-cycling cells may be induced by growth factors in vivo. Br J Cancer 70:244–247
Hollingsworth MA, Swanson BJ (2004) Mucins in cancer: protection and control of the cell surface. Nat Rev Cancer 4:45–60
Ikenoue T, Terakado Y, Nakagawa H, Hikiba Y, Fujii T, Matsubara D, Noguchi R, Zhu C, Yamamoto K, Kudo Y, Asaoka Y, Yamaguchi K, Ijichi H, Tateishi K, Fukushima N, Maeda S, Koike K, Furukawa Y (2016) A novel mouse model of intrahepatic cholangiocarcinoma induced by liver-specific Kras activation and Pten deletion. Sci Rep 6:23899
Jonckheere N, Skrypek N, Van Seuningen I (2014) Mucins and tumor resistance to chemotherapeutic drugs. Biochim Biophys Acta 1846:142–151
Kamphues C, Al-Abadi N, Bova R, Rademacher S, Al-Abadi H, Klauschen F, Bahra M, Neuhaus P, Pratschke J, Seehofer D (2015) The DNA index as a prognostic tool in hilar cholangiocarcinoma. J Surg Oncol 112:214–218
Kubota K, Nakanuma Y, Kondo F, Hachiya H, Miyazaki M, Nagino M, Yamamoto M, Isayama H, Tabata M, Kinoshita H, Kamisawa T, Inui K (2014) Clinicopathological features and prognosis of mucin-producing bile duct tumor and mucinous cystic tumor of the liver: a multi-institutional study by the Japan Biliary Association. J Hepatobiliary Pancreat Sci 21:176–185
Maga G, Hubscher U (2003) Proliferating cell nuclear antigen (PCNA): a dancer with many partners. J Cell Sci 116:3051–3060
Mall AS, Tyler MG, Ho SB, Krige JE, Kahn D, Spearman W, Myer L, Govender D (2010) The expression of MUC mucin in cholangiocarcinoma. Pathol Res Pract 206:805–809
Ono A, Hattori S, Kariya R, Iwanaga S, Taura M, Harada H, Suzu S, Okada S (2011) Comparative study of human hematopoietic cell engraftment into BALB/c and C57BL/6 strain of rag-2/jak3 double-deficient mice. J Biomed Biotechnol 2011:539748
Phoomak C, Vaeteewoottacharn K, Sawanyawisuth K, Seubwai W, Wongkham C, Silsirivanit A, Wongkham S (2016) Mechanistic insights of O-GlcNAcylation that promote progression of cholangiocarcinoma cells via nuclear translocation of NF-kappaB. Sci Rep 6:27853
Prakobwong S, Khoontawad J, Yongvanit P, Pairojkul C, Hiraku Y, Sithithaworn P, Pinlaor P, Aggarwal BB, Pinlaor S (2011) Curcumin decreases cholangiocarcinogenesis in hamsters by suppressing inflammation-mediated molecular events related to multistep carcinogenesis. Int J Cancer 129:88–100
Puthdee N, Vaeteewoottacharn K, Seubwai W, Wonkchalee O, Kaewkong W, Juasook A, Pinlaor S, Pairojkul C, Wongkham C, Okada S, Boonmars T, Wongkham S (2013) Establishment of an allo-transplantable hamster cholangiocarcinoma cell line and its application for in vivo screening of anti-cancer drugs. Korean J Parasitol 51:711–717
Rizvi S, Fischbach SR, Bronk SF, Hirsova P, Krishnan A, Dhanasekaran R, Smadbeck JB, Smoot RL, Vasmatzis G, Gores GJ (2018) YAP-associated chromosomal instability and cholangiocarcinoma in mice. Oncotarget 9:5892–5905
Saranaruk P, Kariya R, Sittithumcharee G, Boueroy P, Boonmars T, Sawanyawisuth K, Wongkham C, Wongkham S, Okada S, Vaeteewoottacharn K (2020) Chromomycin A3 suppresses cholangiocarcinoma growth by induction of S phase cell cycle arrest and suppression of Sp1related antiapoptotic proteins. Int J Mol Med 45:1005–1016
Sirica AE, Zhang Z, Lai GH, Asano T, Shen XN, Ward DJ, Mahatme A, Dewitt JL (2008) A novel “patient-like” model of cholangiocarcinoma progression based on bile duct inoculation of tumorigenic rat cholangiocyte cell lines. Hepatology 47:1178–1190
Sirisinha S, Tengchaisri T, Boonpucknavig S, Prempracha N, Ratanarapee S, Pausawasdi A (1991) Establishment and characterization of a cholangiocarcinoma cell line from a Thai patient with intrahepatic bile duct cancer. Asian Pac J Allergy Immunol 9:153–157
Sripa B, Leungwattanawanit S, Nitta T, Wongkham C, Bhudhisawasdi V, Puapairoj A, Sripa C, Miwa M (2005) Establishment and characterization of an opisthorchiasis-associated cholangiocarcinoma cell line (KKU-100). World J Gastroenterol 11:3392–3397
Sripa B, Seubwai W, Vaeteewoottacharn K, Sawanyawisuth K, Silsirivanit A, Kaewkong W, Muisuk K, Dana P, Phoomak C, Lert-Itthiporn W, Luvira V, Pairojkul C, Teh BT, Wongkham S, Okada S, Chamgramol Y (2020) Functional and genetic characterization of three cell lines derived from a single tumor of an Opisthorchis viverrini-associated cholangiocarcinoma patient. Hum Cell 33:695–708
Stadinski BD, Huseby ES (2020) How to prevent yourself from seeing double. Cytometry A 97:1102–1104
Tengchaisri T, Prempracha N, Thamavit W, Boonpucknavig S, Sriurairatana S, Sirisinha S (1995) Establishment and characterization of cell lines from liver fluke-associated cholangiocarcinoma induced in a hamster model. Southeast Asian J Trop Med Public Health 26:231–239
Thamavit W, Bhamarapravati N, Sahaphong S, Vajrasthira S, Angsubhakorn S (1978) Effects of dimethylnitrosamine on induction of cholangiocarcinoma in Opisthorchis viverrini-infected Syrian golden hamsters. Cancer Res 38:4634–4639
Umemura T, Kai S, Hasegawa R, Kanki K, Kitamura Y, Nishikawa A, Hirose M (2003) Prevention of dual promoting effects of pentachlorophenol, an environmental pollutant, on diethylnitrosamine-induced hepato- and cholangiocarcinogenesis in mice by green tea infusion. Carcinogenesis 24:1105–1109
Vaeteewoottacharn K, Kariya R, Pothipan P, Fujikawa S, Pairojkul C, Waraasawapati S, Kuwahara K, Wongkham C, Wongkham S, Okada S (2019a) Attenuation of CD47-SIRPalpha signal in cholangiocarcinoma potentiates tumor-associated macrophage-mediated phagocytosis and suppresses intrahepatic metastasis. Transl Oncol 12:217–225
Vaeteewoottacharn K, Pairojkul C, Kariya R, Muisuk K, Imtawil K, Chamgramol Y, Bhudhisawasdi V, Khuntikeo N, Pugkhem A, Saeseow OT, Silsirivanit A, Wongkham C, Wongkham S, Okada S (2019b) Establishment of highly transplantable cholangiocarcinoma cell lines from a patient-derived xenograft mouse model. Cells 8:496
Vaeteewoottacharn K, Seubwai W, Bhudhisawasdi V, Okada S, Wongkham S (2014) Potential targeted therapy for liver fluke associated cholangiocarcinoma. J Hepatobiliary Pancreat Sci 21:362–370
Wersto RP, Chrest FJ, Leary JF, Morris C, Stetler-Stevenson MA, Gabrielson E (2001) Doublet discrimination in DNA cell-cycle analysis. Cytometry 46:296–306
Wu Z, Boonmars T, Boonjaraspinyo S, Nagano I, Pinlaor S, Puapairoj A, Yongvanit P, Takahashi Y (2011) Candidate genes involving in tumorigenesis of cholangiocarcinoma induced by Opisthorchis viverrini infection. Parasitol Res 109:657–673
Xu X, Kobayashi S, Qiao W, Li C, Xiao C, Radaeva S, Stiles B, Wang RH, Ohara N, Yoshino T, LeRoith D, Torbenson MS, Gores GJ, Wu H, Gao B, Deng CX (2006) Induction of intrahepatic cholangiocellular carcinoma by liver-specific disruption of Smad4 and Pten in mice. J Clin Investig 116:1843–1852
Yongvanit P, Pinlaor S, Bartsch H (2012) Oxidative and nitrative DNA damage: key events in opisthorchiasis-induced carcinogenesis. Parasitol Int 61:130–135
Funding
This work was supported in part by e-ASIA Joint Research Program from Japan Agency for Medical Research and Development (AMED), Japan (Grant Number: 20jm0210062h0003 to SO) and from the National Science and Technology Development Agency, Thailand (Grant Number: FDA-CO-2562–9172-TH to KV). KV was partly supported by the Thailand Research Fund (Grant Number: RSA6180068).
Author information
Authors and Affiliations
Contributions
KV and SO conceived and designed the experiments. PB, KV, RK, and SF performed the experiments. PB. and RK. analyzed the data. PB, KV, and SO wrote the paper. All authors carefully read and approved the final version of the manuscript.
Corresponding authors
Ethics declarations
Conflict of interest
The authors declare no conflict of interest.
Supplementary Information
Below is the link to the electronic supplementary material.
11626_2021_608_MOESM1_ESM.tif
Figure S1 Cell cycle analysis of multinucleated Ham-1 and Ham-2 cells. Cells were stained with PI and were gated as shown from left to right. The multinucleated cells were the cells that have DNA content higher than G2 (> 4N) (tif 113 kb)
Rights and permissions
About this article
Cite this article
Boonnate, P., Vaeteewoottacharn, K., Kariya, R. et al. Mucin-producing hamster cholangiocarcinoma cell line, Ham-2, possesses the aggressive cancer phenotypes with liver and lung metastases. In Vitro Cell.Dev.Biol.-Animal 57, 825–834 (2021). https://doi.org/10.1007/s11626-021-00608-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11626-021-00608-z