Abstract
Background
The role of preoperative neoadjuvant chemotherapy (NAC) in patients with resectable colorectal liver metastases (CRLM) remains undetermined. This study aimed to assess the efficacy of NAC in patients with resectable CRLM, especially in high-risk subgroups for recurrence, with special reference to synchronicity and the CRLM grade in the Japanese classification system.
Methods
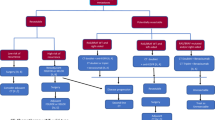
A retrospective analysis of a multi-institutional cohort who was diagnosed with resectable CRLM was performed. CRLM was classified into three grades (A, B, and C) according to the combination of H stage (H1: ≤ 4 lesions and ≤ 5 cm, H2: ≥ 5 lesions or > 5 cm, H3: ≥ 5 lesions and > 5 cm), nodal status of the primary tumor (pN0/1: ≤ 3 metastases, pN2: ≥ 4 metastases), and the presence of resectable extrahepatic metastases.
Results
Among 222 patients with resectable CRLM, 97 (43.7%) had synchronous CRLM. The surgical failure-free survival (SF-FS) of patients with synchronous CRLM (without NAC) was significantly worse than that of patients with metachronous CRLM (P = 0.0264). The SF-FS of patients with Grade B/C was also significantly worse than that of Grade A (P = 0.0058). Among the 53 patients with synchronous and Grade B/C CRLM, 31 were assigned to NAC, and all of them underwent liver surgery. In this high-risk subgroup, the SF-FS and OS in the NAC group were significantly better than those in the upfront surgery group (P < 0.0001 and P = 0.0004, respectively).
Conclusions
Patients with synchronous and Grade B/C CRLM could be good candidates for indication of NAC.




Similar content being viewed by others
References
Hallet J, Sa Cunha A, Adam R et al (2016) Factors influencing recurrence following initial hepatectomy for colorectal liver metastases. Br J Surg 103:1366–1376. https://doi.org/10.1002/bjs.10191
Primrose J, Falk S, Finch-Jones M et al (2014) Systemic chemotherapy with or without cetuximab in patients with resectable colorectal liver metastasis: the new EPOC randomised controlled trial. Lancet Oncol 15:601–611. https://doi.org/10.1016/S1470-2045(14)70105-6
Kopetz S, Chang GJ, Overman MJ et al (2009) Improved survival in metastatic colorectal cancer is associated with adoption of hepatic resection and improved chemotherapy. J Clin Oncol 27:3677–3683. https://doi.org/10.1200/JCO.2008.20.5278
Saiura A, Yamamoto J, Hasegawa K et al (2012) Liver resection for multiple colorectal liver metastases with surgery up-front approach: bi-institutional analysis of 736 consecutive cases. World J Surg 36:2171–2178. https://doi.org/10.1007/s00268-012-1616-y
Hebbar M, Pruvot FR, Romano O et al (2009) Integration of neoadjuvant and adjuvant chemotherapy in patients with resectable liver metastases from colorectal cancer. Cancer Treat Rev 35:668–675. https://doi.org/10.1016/j.ctrv.2009.08.005
Folprecht G, Gruenberger T, Bechstein WO et al (2010) Tumour response and secondary resectability of colorectal liver metastases following neoadjuvant chemotherapy with cetuximab: the CELIM randomised phase 2 trial. Lancet Oncol 11:38–47. https://doi.org/10.1016/S1470-2045(09)70330-4
Beppu T, Emi Y, Tokunaga S et al (2014) Liver resectability of advanced liver-limited colorectal liver metastases following mFOLFOX6 with bevacizumab (KSCC0802 study). Anticancer Res 34:6655–6662
Oki E, Emi Y, Yamanaka T et al (2019) Randomised phase II trial of mFOLFOX6 plus bevacizumab versus mFOLFOX6 plus cetuximab as first-line treatment for colorectal liver metastasis (ATOM trial). Br J Cancer 121:222–229. https://doi.org/10.1038/s41416-019-0518-2
Wang ZM, Chen YY, Chen FF et al (2015) Peri-operative chemotherapy for patients with resectable colorectal hepatic metastasis: a meta-analysis. Eur J Surg Oncol 41:1197–1203. https://doi.org/10.1016/j.ejso.2015.05.020
Bonney GK, Coldham C, Adam R et al (2015) Role of neoadjuvant chemotherapy in resectable synchronous colorectal liver metastasis; an international multi-center data analysis using LiverMetSurvey. J Surg Oncol 111:716–724. https://doi.org/10.1002/jso.23899
Zhu D, Zhong Y, Wei Y et al (2014) Effect of neoadjuvant chemotherapy in patients with resectable colorectal liver metastases. PLoS ONE 9:1–6. https://doi.org/10.1371/journal.pone.0086543
Hirokawa F, Asakuma M, Komeda K et al (2019) Is neoadjuvant chemotherapy appropriate for patients with resectable liver metastases from colorectal cancer? Surg Today 49:82–89. https://doi.org/10.1007/s00595-018-1716-x
Nordlinger B, Sorbye H, Glimelius B et al (2008) Perioperative chemotherapy with FOLFOX4 and surgery versus surgery alone for resectable liver metastases from colorectal cancer (EORTC Intergroup trial 40983): a randomised controlled trial. Lancet 371:1007–1016. https://doi.org/10.1016/S0140-6736(08)60455-9
Nordlinger B, Sorbye H, Glimelius B et al (2013) Perioperative FOLFOX4 chemotherapy and surgery versus surgery alone for resectable liver metastases from colorectal cancer (EORTC 40983): long-term results of a randomised, controlled, phase 3 trial. Lancet Oncol 14:1208–1215. https://doi.org/10.1016/S1470-2045(13)70447-9
Ichida H, Mise Y, Ito H et al (2019) Optimal indication criteria for neoadjuvant chemotherapy in patients with resectable colorectal liver metastases. World J Surg Oncol 17:1–9. https://doi.org/10.1186/s12957-019-1641-5
Yamaguchi T, Mori T, Takahashi K et al (2008) A new classification system for liver metastases from colorectal cancer in Japanese multicenter analysis. Hepatogastroenterology 55:173–178
Shinto E, Takahashi K, Yamaguchi T et al (2015) Validation and modification of the Japanese Classification System for liver metastases from colorectal cancer: a multi-institutional study. Ann Surg Oncol 22:3888–3895. https://doi.org/10.1245/s10434-015-4470-y
Yamashita K, Watanabe M, Mine S et al (2018) The impact of the Charlson comorbidity index on the prognosis of esophageal cancer patients who underwent esophagectomy with curative intent. Surg Today 48:632–639. https://doi.org/10.1007/s00595-018-1630-2
Hwang M, Jayakrishnan TT, Green DE et al (2014) Systematic review of outcomes of patients undergoing resection for colorectal liver metastases in the setting of extra hepatic disease. Eur J Cancer 50:1747–1757. https://doi.org/10.1016/j.ejca.2014.03.277
Oba M, Hasegawa K, Shindoh J et al (2016) Survival benefit of repeat resection of successive recurrences after the initial hepatic resection for colorectal liver metastases. Surgery 159:632–640. https://doi.org/10.1016/j.surg.2015.09.003
Oba M, Hasegawa K, Matsuyama Y et al (2014) Discrepancy between recurrence-free survival and overall survival in patients with resectable colorectal liver metastases: a potential surrogate endpoint for time to surgical failure. Ann Surg Oncol 21:1817–1824. https://doi.org/10.1245/s10434-014-3504-1
Allard MA, Nishioka Y, Beghdadi N et al (2019) Multicentre study of perioperative versus adjuvant chemotherapy for resectable colorectal liver metastases. BJS open 3:678–686. https://doi.org/10.1002/bjs5.50174
Ratti F, Fuks D, Cipriani F et al (2019) Timing of perioperative chemotherapy does not influence long-term outcome of patients undergoing combined laparoscopic colorectal and liver resection in selected upfront resectable synchronous liver metastases. World J Surg 43:3110–3119. https://doi.org/10.1007/s00268-019-05142-4
Hewes JC, Dighe S, Morris RW et al (2007) Preoperative chemotherapy and the outcome of liver resection for colorectal metastases. World J Surg 31:353–364. https://doi.org/10.1007/s00268-006-0103-8
Nishioka Y, Shindoh J, Yoshioka R et al (2017) Clinical impact of preoperative chemotherapy on microscopic cancer spread surrounding colorectal liver metastases. Ann Surg Oncol 24:2326–2333. https://doi.org/10.1245/s10434-017-5845-z
Beppu T, Sakamoto Y, Hasegawa K et al (2012) A nomogram predicting disease-free survival in patients with colorectal liver metastases treated with hepatic resection: multicenter data collection as a project study for hepatic surgery of the Japanese Society of Hepato-Biliary-Pancreatic Surgery. J Hepatobiliary Pancreat Sci 19:72–84. https://doi.org/10.1007/s00534-011-0460-z
Okuno M, Hatano E, Seo S et al (2014) Indication for neoadjuvant chemotherapy in patients with colorectal liver metastases based on a nomogram that predicts disease-free survival. J Hepatobiliary Pancreat Sci 21:881–888. https://doi.org/10.1002/jhbp.149
Ayez N, van der Stok EP, de Wilt H et al (2015) Neo-adjuvant chemotherapy followed by surgery versus surgery alone in high-risk patients with resectable colorectal liver metastases: the CHARISMA randomized multicenter clinical trial. BMC Cancer 15:1–7. https://doi.org/10.1186/s12885-015-1199-8
Acknowledgements
We thank all the patients and the investigators involved in this study.
Funding
This study received no financial support.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no conflict of interests for this article.
Ethical approval
This study was approved by the Institutional Review Board in each institution (approval number: 789, 2019–9-7 and 204).
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.

10147_2021_2024_MOESM1_ESM.jpg
Supplementary file1 Supplementary Figure 1. Kaplan-Meier curves of the SF-FS in patients with (A) synchronous Grade A CRLM, (B) metachronous Grade A CRLM, (C) metachronous Grade B/C CRLM. Comparison between the NAC and Upfront surgery groups. SF-FS, surgical failure-free survival; NAC, neoadjuvant chemotherapy (JPG 1200 KB)

10147_2021_2024_MOESM2_ESM.jpg
Supplementary file2 Supplementary Figure 2. Kaplan-Meier curves of the SF-FS in patients with Grade B subgroups. Comparison between H2 and pN0/1 subgroup and H1 and pN2 subgroup in synchronous (A) and metachronous (B) CRLM patients, and comparison between NAC and Upfront surgery group in H1 and pN2 subgroup (C) and H2 and pN0/1 subgroup (D). SF-FS, surgical failure-free survival; NAC, neoadjuvant chemotherapy. (JPG 941 KB)
About this article
Cite this article
Ninomiya, M., Emi, Y., Motomura, T. et al. Efficacy of neoadjuvant chemotherapy in patients with high-risk resectable colorectal liver metastases. Int J Clin Oncol 26, 2255–2264 (2021). https://doi.org/10.1007/s10147-021-02024-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10147-021-02024-5