Abstract
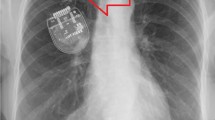
Twiddler’s syndrome (TS) is a hardware-related complication of deep brain stimulation which has not been well documented and is probably underreported. The objective of this study is to comprehensively describe TS by systematically reviewing the related literature. The methods include selecting the eligible studies based on the inclusion and exclusion criteria. Data about studies and TS were collected. A descriptive statistical analysis of the extracted data was performed. We found 18 eligible studies describing 23 patients with TS. The mean age of the 23 patients was 61.4 ± 15.9 years (range, 16–79 years.). The percentage of TS in the female population was 91.3% (females: 21/23). The incidence of postoperative TS was 1.4% (6 out of 437) per patient and 1.1% (8 out of 709) per extension wire. The mean time to clinical presentation was 9.9 ± 10.3 months (range, 0.5–36 months). Nineteen of the twenty-three patients presented with a rebound of previous symptoms. Twelve of the twenty-three patients had high impedance at the postoperative checkup of the DBS system. A plain X-ray indicated twisted extension wires in almost all these patients. All patients meeting the definition of postoperative device-related TS underwent revision surgery. TS is more prevalent in females. Based on the typical clinical symptoms (rebound of the previous symptoms, high impedance, and X-ray demonstration), the differential diagnosis can often be straightforward. TS should thus be taken into consideration when attempting to explain or rule out hardware malfunction. The timely recognition and proper revision of TS can prevent further serious damage.




Similar content being viewed by others
Data availability
Not applicable.
Code availability
Not applicable.
References
Bayliss C, Beanlands D, Baird R (1968) The pacemaker-twiddler’s syndrome: a new complication of implantable transvenous pacemakers. Can Med Assoc J 99(8):371–373
Sobstyl M, Ząbek M, Brzuszkiewicz-Kuźmicka G, Pasterski T (2017) Dual anchor internal pulse generator technique may lower risk of Twiddler’s syndrome: a case series and literature review. Neuromodulation 20(6):606–612. https://doi.org/10.1111/ner.12581
Khalilullah M, Khanna SK, Gupta U, Padmavati S (1979) Pacemaker twiddler’s syndrome: a note on its mechanism. J Cardiovasc Surg (Torino) 20(1):95–100
Mohammad R, Pervaiz A et al (2018) Reel syndrome: an atypical cause for inappropriate shocks in a patient with automated implantable cardioverter defibrillator (AICD). Cureus 10(2):e2237. https://doi.org/10.7759/cureus.2237
Iftikhar H, Saleem M, Nadeem M, Caplan J, Kaji A (2019) A presentation of Twiddler’s syndrome with underlying ratchet mechanism. Cureus 11(2):e4060. https://doi.org/10.7759/cureus.4060
Carrizo AG, Hong PS, Amit G, Healey JS (2016) Double twiddle trouble, a new variant of twiddler syndrome. J Arrhythm 32(3):236–237. https://doi.org/10.1016/j.joa.2016.02.008
Geissinger G, Neal J (2007) Spontaneous twiddler’s syndrome in a patient with a deep brain stimulator. Surg Neurol 68(4):454–456. https://doi.org/10.1016/j.surneu.2006.10.062 (discussion 456)
Machado A, Hiremath G, Salazar F, Rezai A (2005) Fracture of subthalamic nucleus deep brain stimulation hardware as a result of compulsive manipulation: case report. Neurosurgery 57(6):E1318–E1318. https://doi.org/10.1227/01.neu.0000187566.01731.51
Gelabert-Gonzalez M, Relova-Quinteiro J, Castro-García A (2010) “Twiddler syndrome” in two patients with deep brain stimulation. Acta Neurochir (Wien) 152(3):489–491. https://doi.org/10.1007/s00701-009-0366-6
Goyal V, Vaishya S, Shukla G, Singh S, Behari M (2009) Unusual complication of deep brain stimulation in Parkinson’s disease. Mov Disord 24(8):1251–1252. https://doi.org/10.1002/mds.21876
Astradsson A, Schweder P, Joint C, Green A, Aziz T (2011) Twiddler’s syndrome in a patient with a deep brain stimulation device for generalized dystonia. J Clin Neurosci 18(7):970–972. https://doi.org/10.1016/j.jocn.2010.11.012
Burdick A, Okun M et al (2010) Prevalence of Twiddler’s syndrome as a cause of deep brain stimulation hardware failure. Stereotact Funct Neurosurg 88(6):353–359. https://doi.org/10.1159/000319039
Dobson R (2007) Neurosurgeons told to watch for signs of “twiddler’s syndrome.” BMJ 335(7611):114–115. https://doi.org/10.1136/bmj.39279.395787.BE
Franzini A, Ranieri R, Gambini O, Messina G (2018) Manipulating an internal pulse generator until twiddler’s syndrome in a patient treated with deep brain stimulation for obsessive-compulsive disorder. Acta Neurochir (Wien) 160(2):389–392. https://doi.org/10.1007/s00701-017-3412-9
Garg A, Mohan A, Garell P (2010) Placement of the internal pulse generator for deep brain stimulation in the upper back to prevent fracture of the extension wire due to generator rotation: case report. Parkinsons Dis. https://doi.org/10.4061/2010/189371
Ghanchi H, Taka T, Bernstein J, Kashyap S, Ananda A (2020) The unsuccessful twiddler: a case of twiddler’s syndrome without deep brain stimulator lead breakage. Cureus 12(4):e7786. https://doi.org/10.7759/cureus.7786
Israel Z, Spivak A (2008) A tremulous twiddler. Stereotact Funct Neurosurg 86(5):297–299. https://doi.org/10.1159/000155231
Jackowiak E, Patil P, Chou K (2019) The deep brain stimulation “Twiddler syndrome.” JAMA Neurol 76(5):620. https://doi.org/10.1001/jamaneurol.2019.0691
Menghetti C, Zekaj E, Saleh C, Porta M, Servello D (2014) How to avoid Twiddler’s syndrome in deep brain stimulation for dystonia? Neuromodulation 17(2):198–199. https://doi.org/10.1111/ner.12067
Moliz N, Katati M et al (2015) Twiddler’s syndrome in a patient with obsessive-compulsive disorder treated with deep brain stimulation. Neurocirugia 26(4):196–199. https://doi.org/10.1016/j.neucir.2014.11.001
Morishita T, Foote K et al (2010) Identification and management of deep brain stimulation intra- and postoperative urgencies and emergencies. Parkinsonism Relat Disord 16(3):153–162. https://doi.org/10.1016/j.parkreldis.2009.10.003
Morishita T, Hilliard J et al (2017) Postoperative lead migration in deep brain stimulation surgery: Incidence, risk factors, and clinical impact. PLoS ONE 12(9):e0183711. https://doi.org/10.1371/journal.pone.0183711
Penn D, Wu C, Skidmore C, Sperling M, Sharan A (2012) Twiddler’s syndrome in a patient with epilepsy treated with deep brain stimulation. Epilepsia 53(7):e119-121. https://doi.org/10.1111/j.1528-1167.2012.03489.x
Pourfar M, Budman C, Mogilner A (2015) A case of deep brain stimulation for Tourette’s complicated by Twiddler’s syndrome. Mov Disord Clin Pract 2(2):192–193. https://doi.org/10.1002/mdc3.12132
Silva P, Chamadoira C et al (2014) Twiddler (or Not) Syndrome: Questioning etiology for an uncommon form of hardware malfunction in deep brain stimulation. Surg Neurol Int 5(Suppl 8):S410–S412. https://doi.org/10.4103/2152-7806.140201
Sobstyl M, Ząbek M, Górecki W, Brzuszkiewicz-Kuźmicka G (2015) Twiddler syndrome in a patient with tremor dominant Parkinson's disease. A case report and literature review. Neurologia neurochirurgia polska 49(6): 467–471. https://doi.org/10.1016/j.pjnns.2015.10.004
Tymchak Z, Vitali A (2017) What’s the twist? Twiddler’s syndrome in deep brain stimulation. Can J Neurol Sci 44(6):726–727. https://doi.org/10.1017/cjn.2017.230
Okun M, Rodriguez R et al (2008) A case-based review of troubleshooting deep brain stimulator issues in movement and neuropsychiatric disorders. Parkinsonism Relat Disord 14(7):532–538. https://doi.org/10.1016/j.parkreldis.2008.01.001
Jitkritsadakul O, Bhidayasiri R et al (2017) Systematic review of hardware-related complications of deep brain stimulation: do new indications pose an increased risk? Brain Stimul 10(5):967–976. https://doi.org/10.1016/j.brs.2017.07.003
Herschman Y, Fellig Y, Israel Z (2019) Deep brain stimulation and bowstringing: case report and pathological correlation. Interdisciplinary Neurosurgery 17:104–106. https://doi.org/10.1016/j.inat.2019.04.003
Miller PM, Gross RE (2009) Wire tethering or “bowstringing” as a long-term hardware-related complication of deep brain stimulation. Stereotact Funct Neurosurg 87(6):353–359. https://doi.org/10.1159/000236369
Baizabal Carvallo JF, Simpson R, Jankovic J (2011) Diagnosis and treatment of complications related to deep brain stimulation hardware. Mov Disord 26(8):1398–1406. https://doi.org/10.1002/mds.23800
Author information
Authors and Affiliations
Contributions
Wei wang had the idea for the article; Xiaowei Liu and Siyu Li performed the literature search; Xiaowei Liu and Yangyang Xu performed the literature screening and data extraction; Xiaowei Liu analyzed data and drafted the work; Hagai Bergman critically revised the manuscript.
Corresponding author
Ethics declarations
Ethics approval
Not applicable.
Consent to participate
Not applicable.
Consent for publication
Not applicable.
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Liu, X., Xu, Y., Bergman, H. et al. A systematic review of Twiddler’s syndrome: a hardware-related complication of deep brain stimulation. Neurosurg Rev 45, 951–963 (2022). https://doi.org/10.1007/s10143-021-01636-9
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10143-021-01636-9