Abstract
Introduction
Even treated, myasthenia gravis (MG) continues to represent a significant burden and might continuously affect patients’ quality of life (QoL). The aim of our longitudinal study was to analyze QoL in a large cohort of MG patients after a 10-year follow-up period.
Methods
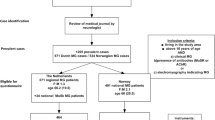
This study comprised 78 MG patients (60% females, 50 ± 16 years old at baseline, 70% AchR positive) who were retested after 10 years. Disease severity was evaluated by MGFA classification. QoL was assessed using SF-36 questionnaire and Myasthenia Gravis-specific Questionnaire (MGQ). Hamilton rating scales for depression and anxiety (HDRS and HARS), Multidimensional Scale of Perceived Social Support (MSPSS) and Acceptance of Illness Scale (AIS) were also used.
Results
Similar percentage of patients was in remission at both time points (42% and 45%). However, at baseline all patients were treated, while 32% were treatment-free at follow-up. SF-36, MGQ, MSPSS and AIS scores were similar at baseline and retest. Mean HDRS and HARS scores worsened during time (p < 0.05), although percentage of patients with depression and anxiety did not change significantly. Significant predictors of worse SF-36 score at retest were depression (β = − 0.45, p < 0.01), poor disease acceptance (β = − 0.44, p < 0.01) and older age (β = − 0.30, p < 0.01). Significant predictors of worse MGQ score at retest were poor disease acceptance (β = − 0.40, p < 0.01), retirement (β = − 0.36, p < 0.01), lower education (β = 0.25, p < 0.01), and depression (β = − 0.18, p < 0.05).
Conclusions
Although after 10 years, a significant number of MG patients were in remission, their QoL was still reduced. Neurologists should be aware that patients’ perception of poor QoL may persist even if MG is well treated from a physician’s perspective.
Similar content being viewed by others
Availability of data and material
The data that support the findings of this study are available on request from the corresponding author. The data are not publicly available due to privacy and ethical restrictions.
Code availability
Not applicable.
References
Szczudlik P, Sobieszczuk E, Szyluk B et al (2020) Determinants of Quality of Life in Myasthenia Gravis Patients. Front Neurol 11:553626. https://doi.org/10.3389/fneur.2020.553626
Boldingh MI, Dekker L, Maniaol AH, Brunborg C et al (2015) An up-date on health-related quality of life in myasthenia gravis - results from population based cohorts. Health Qual Life Outcomes 13:115. https://doi.org/10.1186/s12955-015-0298-1
Mourão AM, Gomez RS, Barbosa LSM et al (2016) Determinants of quality of life in Brazilian patients with myasthenia gravis. Clinics (Sao Paulo) 71(7):370–374. https://doi.org/10.6061/clinics/2016(07)03
Osserman KE, Genkins G (1971) Studies in myasthenia gravis: review of twenty-year experience in over 1200 patients. Mt Sinai J Med 38(497–537):20
Stalberg E (1980) Clinical electrophysiology in myasthenia gravis. J Neurol Neurosurg Psychiatry 43:622–633. https://doi.org/10.1136/jnnp.43.7.622
Jeretzki A, Barohn RJ, Ernstoff RM et al (2000) Myasthenia gravis: recommendations for clinical research standards. Task Force of the Medical Scientific Advisory Board of the Myasthenia Gravis Foundation of America. Neurology 55:16–23. https://doi.org/10.1016/s0003-4975(00)01595-2
Basta I, Pekmezovic T, Peric S et al (2012) Assessment of health-related quality of life in patients with myasthenia gravis in Belgrade (Serbia). Neurol Sci 33(6):1375–1381. https://doi.org/10.1007/s10072-012-1170-2
Felton BJ, Revenson TA (1984) Coping with chronic illness: a study of illness controllability and influence of coping strategies on psychological adjustment. J Consult Clin Psychol 2:343–353. https://doi.org/10.1037//0022-006x.52.3.343
Zimet GD, Powell SS, Farley GK et al (1990) Psychometric characteristics of the Multidimensional Scale of Perceived Social Support. J Pers Assess 55:610–617. https://doi.org/10.1080/00223891.1990.9674095
Bozovic I, Kacar A, Peric S et al (2017) Quality of life predictors in patients with chronic inflammatory demyelinating polyradiculoneuropathy. J Neurol 264(12):2481–2486. https://doi.org/10.1007/s00415-017-8658-x
Basta I, Pekmezovic T, Padua L et al (2010) Validation of Serbian version of the disease-specific myasthenia gravis questionnaire. Acta Neurol Scand 122(2):110–114. https://doi.org/10.1111/j.1600-0404.2009.01269.x
Salins S, Teter B, Kavak K et al (2016) Low-dose medication and long-term outcome in myasthenia gravis. J Clin Neuromusc Dis 18:61–66. https://doi.org/10.1097/CND.0000000000000122
Utsugisawa K, Nagane Y, Akaishi T et al (2017) Early fast-acting treatment strategy against generalised myasthenia gravis. Muscle Nerve 55:794–801. https://doi.org/10.1002/mus.25397
Andersen JB, Gilhus NE, Sanders DB (2016) Factors affecting outcome in myasthenia gravis. Muscle Nerve 54:1041–1049. https://doi.org/10.1002/mus.25205
Wolfe G, Kaminski H, Aban I et al (2019) Long-term effect of thymectomy in patients with non-thymomatous myasthenia gravis treated with prednisone: 2-year extension of the MGTX randomised trial. Lancet Neurol 18(3):259–268. https://doi.org/10.1016/S1474-4422(18)30392-2
Gilhus NE (2016) Myasthenia gravis. N Engl J Med 375:2570–2581. https://doi.org/10.1056/NEJMra1602678
Grob D, Brunner N, Namba T et al (2008) Lifetime course of myasthenia gravis. Muscle Nerve 37:141–149. https://doi.org/10.1002/mus.20950
Kupersmit M (2009) Ocular myasthenia gravis: treatment successes and failures in patients with long-term follow-up. J Neurol 256(8):1314–1320. https://doi.org/10.1007/s00415-009-5120-8
Redmond AC, Burns J, Ouvrier RA (2008) Factors that influence health-related quality of life in Australian adults with Charcot–Marie–Tooth disease. Neuromuscul Disord 18(8):619–625. https://doi.org/10.1016/j.nmd.2008.05.015
Carrozzino D, Patierno C, Fava G et al (2020) The hamilton rating scales for depression: A critical review of clinimetric properties of different versions. Psychother Psychosom 89:133–150. https://doi.org/10.1159/000506879
Law C, Flaherty CV, Bandyopadhyay S (2020) A review of psychiatric comorbidity in myasthenia gravis. Cureus 12(7):e9184. https://doi.org/10.7759/cureus.9184
Jeong A, Min JH, Kang YK (2018) Factors associated with quality of life of people with Myasthenia Gravis. PLoS ONE 13(11):e0206754. https://doi.org/10.1371/journal.pone.0206754
Padua L, Evoli A, Aprile I et al (2001) Health-related quality of life in patients with myasthenia gravis and the relationship between patient-oriented assessment and conventional measurements. Neurol Sci 22:363–369. https://doi.org/10.1007/s100720100066
Twork S, Wiesmeth S, Klewer J et al (2010) Quality of life and life circumstances in German myasthenia gravis patients. Health Qual Life Outcomes 8:129. https://doi.org/10.1186/1477-7525-8-129
Winter Y, Schepelmann K, Spottke AE et al (2010) Health-related quality of life in ALS, myasthenia gravis and facioscapulohumeral muscular dystrophy. J Neurol 257:1473–1481. https://doi.org/10.1007/s00415-010-5549-9
Harding KE, Wardle M, Carruthers R et al (2019) Socioeconomic status and disability progression in multiple sclerosis: a multinational study. Neurology 92(13):e1497–e1506. https://doi.org/10.1212/WNL.0000000000007190
Smith GD, Hart C, Blane D et al (1998) Adverse socioeconomic conditions in childhood and cause specific adult mortality: prospective observational study. BMJ 316:1631–1635. https://doi.org/10.1136/bmj.316.7145.1631
Goulden R, Ibrahim T, Wolfson C (2015) Is high socioeconomic status a risk factor for multiple sclerosis? A systematic review. Eur J Neurol 22:899–911. https://doi.org/10.1111/ene.12586
Goulden R, Riise T, Myhr KM et al (2016) Does low socioeconomic status in early life protect against multiple sclerosis? A multinational, case-control study. Eur J Neurol 23:168–174. https://doi.org/10.1111/ene.12830
Funding
This study was supported by the Ministry of Education, Science and Technological Development of Serbia (grant #175083).
Author information
Authors and Affiliations
Contributions
All authors contributed to the study conception and design. Material preparation, data collection and analysis were performed by JIZ, IB, MK, VI and SP. The first draft of the manuscript was written by IB and SP, and all authors have commented on previous versions of the manuscript. The whole research was conceptualized and supervised by IB, DL and SP. All authors have read and approved the final manuscript.
Corresponding author
Ethics declarations
Conflicts of interest/Competing interests
The authors declare that they have no conflict of interest.
Ethics approval
This research was approved by the Ethical Committee of the Faculty of Medicine, University of Belgrade (decision 2650/x-11).
Consent to participate
Informed consent was obtained from all individual participants included in the study.
Consent for publication
Each author has read and approved the final manuscript version for submission.
Rights and permissions
About this article
Cite this article
Bozovic, I., Ilic Zivojinovic, J., Peric , S. et al. Long-term outcome in patients with myasthenia gravis: one decade longitudinal study. J Neurol 269, 2039–2045 (2022). https://doi.org/10.1007/s00415-021-10759-4
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00415-021-10759-4