Abstract
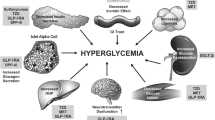
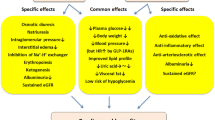
Sodium-glucose co-transporter 2 inhibitors (SGLT2i) have emerged as a promising therapeutic option for hyperglycemia and its complications. However, metformin remains the first-line pharmacological treatment in most algorithms for type 2 diabetes (T2D). Although metformin is generally believed to exert positive effects on cardiovascular (CV) outcomes, relevant data are mainly observational and potentially overinterpreted. Yet, it exerts numerous pleiotropic actions that favorably affect metabolism and diabetes comorbidities. CV outcome trials have demonstrated cardiorenal protection with SGLT2i among people at high CV risk and mostly on concomitant metformin therapy. However, post hoc analyses of these trials suggest that the cardiorenal effects of gliflozins are independent of background treatment and consistent across the full spectrum of CV risk. Considering the importance of addressing hyperglycemia as a means of preventing diabetic complications and significant knowledge gaps, particularly regarding the cost-effectiveness of SGLT2i in drug-naïve populations with T2D, the position of metformin in the management of people with diabetes at low CV risk remains solid for the moment. On the other hand, available evidence—despite its limitations—suggests that specific groups of people with T2D, particularly those with heart failure and kidney disease, could probably benefit more from treatment with SGLT2i. This narrative mini-review aims to discuss whether current evidence justifies the use of SGLT2i as the first-line treatment for T2D.

Similar content being viewed by others
References
Saeedi P, Petersohn I, Salpea P, Malanda B, Karuranga S, Unwin N, et al. Global and regional diabetes prevalence estimates for 2019 and projections for 2030 and 2045: Results from the International Diabetes Federation Diabetes Atlas, 9th edition. Diabetes Res Clin Pract. 2019;157:107843.
Buse JB, Wexler DJ, Tsapas A, Rossing P, Mingrone G, Mathieu C, et al. 2019 Update to: Management of Hyperglycemia in Type 2 Diabetes, 2018. A Consensus Report by the American Diabetes Association (ADA) and the European Association for the Study of Diabetes (EASD). Diabetes Care. 2020;43(2):487–93.
Cosentino F, Grant PJ, Aboyans V, Bailey CJ, Ceriello A, Delgado V, et al. ESC Guidelines on diabetes, pre-diabetes, and cardiovascular diseases developed in collaboration with the EASD. Eur Heart J. 2020;41(2):255–323.
Spain CV, Wright JJ, Hahn RM, Wivel A, Martin AA. Self-reported Barriers to Adherence and Persistence to Treatment With Injectable Medications for Type 2 Diabetes. Clin Ther. 2016;38(7):1653–64.
LaMoia TE, Shulman GI. Cellular and molecular mechanisms of metformin action. Endocr Rev. 2021;42(1):77–96.
Grammatiki M, Sagar R, Ajjan RA. Metformin: is it still the first line in type 2 diabetes management algorithm? Curr Pharm Des. 2021;27(8):1061–7.
Buse JB, DeFronzo RA, Rosenstock J, Kim T, Burns C, Skare S, et al. the primary glucose-lowering effect of metformin resides in the gut, not the circulation: results from short-term pharmacokinetic and 12-week dose-ranging studies. Diabetes Care. 2016;39(2):198–205.
Prattichizzo F, Giuliani A, Mensà E, Sabbatinelli J, De Nigris V, Rippo MR, et al. Pleiotropic effects of metformin: Shaping the microbiome to manage type 2 diabetes and postpone ageing. Ageing Res Rev. 2018;48:87–98.
Pan Q, Lu X, Zhao C, Liao S, Chen X, Guo F, et al. Metformin: the updated protective property in kidney disease. Aging (Albany NY). 2020;12(9):8742–59.
Cheng YY, Leu HB, Chen TJ, Chen CL, Kuo CH, Lee SD, et al. Metformin-inclusive therapy reduces the risk of stroke in patients with diabetes: a 4-year follow-up study. J Stroke Cerebrovasc Dis. 2014;23(2):e99-105.
McGuire DK, Shih WJ, Cosentino F, Charbonnel B, Cherney DZI, Dagogo-Jack S, et al. Association of SGLT2 Inhibitors with cardiovascular and kidney outcomes in patients with type 2 diabetes: a meta-analysis. JAMA Cardiol. 2021;6(2):148–58.
Koufakis T, Mustafa OG, Ajjan RA, Garcia-Moll X, Zebekakis P, Dimitriadis G, et al. The use of sodium-glucose co-transporter 2 inhibitors in the inpatient setting: is the risk worth taking? J Clin Pharm Ther. 2020;45(5):883–91.
Jitraknatee J, Ruengorn C, Nochaiwong S. Prevalence and risk factors of chronic kidney disease among type 2 diabetes patients: a cross-sectional study in primary care practice. Sci Rep. 2020;10(1):6205.
UK Prospective Diabetes Study (UKPDS) Group. Effect of intensive blood-glucose control with metformin on complications in overweight patients with type 2 diabetes (UKPDS 34). Lancet. 1998;352(9131):854–65.
Li X, Celotto S, Pizzol D, Gasevic D, Ji MM, Barnini T, et al. Metformin and health outcomes: An umbrella review of systematic reviews with meta-analyses. Eur J Clin Invest. 2021;51(7):e13536.
Koufakis T, Dimitriadis G, Kotsa K. A lion in the room: Has the CAROLINA trial definitely resolved the issue of the cardiovascular safety of sulfonylureas? J Diabetes. 2020;12(7):499–502.
Investigation of metformin in pre-diabetes on atherosclerotic cardiovascular outcomes (VA-IMPACT). https://clinicaltrials.gov/ct2/show/NCT02915198. Accessed on August 9, 2021.
Targher G, Byrne CD. Treatment algorithm in patients with type 2 diabetes and atherosclerotic cardiovascular disease or high/very high cardiovascular risk. Eur Heart J. 2020;41(2):331.
Szczech LA, Stewart RC, Su HL, DeLoskey RJ, Astor BC, Fox CH, et al. Primary care detection of chronic kidney disease in adults with type-2 diabetes: the ADD-CKD Study (awareness, detection and drug therapy in type 2 diabetes and chronic kidney disease). PLoS One. 2014;9(11):e110535.
Cahn A, Raz I, Leiter LA, Mosenzon O, Murphy SA, Goodrich EL, et al. Cardiovascular, renal, and metabolic outcomes of dapagliflozin versus placebo in a primary cardiovascular prevention cohort: Analyses From DECLARE-TIMI 58. Diabetes Care. 2021;44(5):1159–67.
Zaccardi F, Khunti K, Marx N, Davies MJ. First-line treatment for type 2 diabetes: is it too early to abandon metformin? Lancet. 2020;396(10264):1705–7.
Chen TH, Li YR, Chen SW, Lin YS, Sun CC, Chen DY, et al. Sodium-glucose cotransporter 2 inhibitor versus metformin as first-line therapy in patients with type 2 diabetes mellitus: a multi-institution database study. Cardiovasc Diabetol. 2020;19(1):189.
Singh AK, Singh R. Does background metformin therapy influence the cardiovascular outcomes with SGLT-2 inhibitors in type 2 diabetes? Diabetes Res Clin Pract. 2021;172:108536.
Packer M. Does metformin interfere with the cardiovascular benefits of sglt2 inhibitors? Questions about its role as the cornerstone of diabetes treatment. Am J Med. 2020;133(7):781–2.
Packer M. Are the benefits of SGLT2 inhibitors in heart failure and a reduced ejection fraction influenced by background therapy? Expectations and realities of a new standard of care. Eur Heart J. 2020;41(25):2393–6.
Papazafiropoulou AK, Melidonis A, Antonopoulos S. Effects of glucagon-like peptide-1 receptor agonists and sodium-glucose cotransporter 2 inhibitors on cardiorenal and metabolic outcomes in people without diabetes. Curr Pharm Des. 2021;27(8):1035–42.
Inzucchi SE, Zinman B, Fitchett D, Wanner C, Ferrannini E, Schumacher M, et al. How does empagliflozin reduce cardiovascular mortality? Insights from a mediation analysis of the EMPA-REG OUTCOME Trial. Diabetes Care. 2018;41(2):356–63.
Koufakis T, Papanas N, Dimitriadis G, Zebekakis P, Kotsa K. Interpreting the results of the VERTIS-CV trial: Is this the end of the “class effect” perspective? J Diabetes. 2020;12(12):942–5.
Koufakis T, Mustafa OG, Tsimihodimos V, Ajjan RA, Kotsa K. Insights into the results of sotagliflozin cardiovascular outcome trials: is dual inhibition the cherry on the cake of cardiorenal protection? Drugs. 2021;81(12):1365–71.
Ayele AA, Tegegn HG, Ayele TA, Ayalew MB. Medication regimen complexity and its impact on medication adherence and glycemic control among patients with type 2 diabetes mellitus in an Ethiopian general hospital. BMJ Open Diabetes Res Care. 2019;7(1):e000685.
Christofides EA. Practical insights into improving adherence to metformin therapy in patients with type 2 diabetes. Clin Diabetes. 2019;37(3):234–41.
Ofori-Asenso R, Liew D, Lalic S, Mazidi M, Magliano DJ, Ademi Z, et al. Adherence, persistence, and switching among people prescribed sodium glucose co-transporter 2 inhibitors: a nationwide retrospective cohort study. Adv Ther. 2019;36(11):3265–78.
Kartoun U, Iglay K, Shankar RR, Beam A, Radican L, Chatterjee A, et al. Factors associated with clinical inertia in type 2 diabetes mellitus patients treated with metformin monotherapy. Curr Med Res Opin. 2019;35(12):2063–70.
Hinton W, Feher MD, Munro N, oy M, de Lusignan S. Prescribing sodium-glucose co-transporter-2 inhibitors for type 2 diabetes in primary care: influence of renal function and heart failure diagnosis. Cardiovasc Diabetol. 2021;20(1):130.
Paul SK, Klein K, Thorsted BL, Wolden ML, Khunti K. Delay in treatment intensification increases the risks of cardiovascular events in patients with type 2 diabetes. Cardiovasc Diabetol. 2015;14:100.
Bhatt DL, Szarek M, Steg PG, Cannon CP, Leiter LA, McGuire DK, et al. Sotagliflozin in patients with diabetes and recent worsening heart failure. N Engl J Med. 2021;384(2):117–28.
Mosenzon O, Del Prato S, Schechter M, Leiter LA, Ceriello A, DeFronzo RA, et al. From glucose lowering agents to disease/diabetes modifying drugs: a “SIMPLE” approach for the treatment of type 2 diabetes. Cardiovasc Diabetol. 2021;20(1):92.
Bajpai S, Wong-Jacobson S, Liu D, Mitchell B, Haynes G, Syring K, et al. Health care resource utilization and cost of severe hypoglycemia treatment in insulin-treated patients with diabetes in the United States. J Manag Care Spec Pharm. 2021;27(3):385–91.
Gourzoulidis G, Tzanetakos C, Ioannidis I, Tsapas A, Kourlaba G, Papageorgiou G, et al. Cost-effectiveness of empagliflozin for the treatment of patients with type 2 diabetes mellitus at increased cardiovascular risk in Greece. Clin Drug Investig. 2018;38(5):417–26.
Koufakis T, Papanas N, Zebekakis P, Kotsa K. Treatment options following metformin in primary prevention populations with type 2 diabetes: which is the right road to take? Expert Rev Clin Pharmacol. 2021:1–4.
Zinman B, Wanner C, Lachin JM, Fitchett D, Bluhmki E, Hantel S, et al. Empagliflozin, cardiovascular outcomes, and mortality in type 2 diabetes. N Engl J Med. 2015;373(22):2117–28.
Rena G, Mordi IR, Lang CC. Metformin: still the sweet spot for CV protection in diabetes? Curr Opin Pharmacol. 2020;54:202–8.
Funding
No external funds were used in the preparation of this manuscript.
Author information
Authors and Affiliations
Contributions
TK reviewed the literature and drafted the first version of the manuscript. AP, KM, and KK reviewed the literature and edited the manuscript. All authors have read and approved the final version of the manuscript.
Corresponding author
Ethics declarations
Ethics Approval and Consent to Participate
Not applicable.
Consent for Publication
Not applicable.
Availability of Data and Materials
Not applicable.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Koufakis, T., Papazafiropoulou, A., Makrilakis, K. et al. Sodium-Glucose Co-transporter 2 Inhibitors Versus Metformin as the First-Line Treatment for Type 2 Diabetes: Is It Time for a Revolution?. Cardiovasc Drugs Ther 37, 315–321 (2023). https://doi.org/10.1007/s10557-021-07249-0
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10557-021-07249-0