Abstract
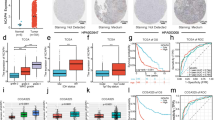
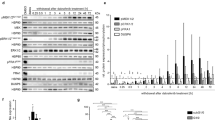
Since few reports have mentioned the role of FOSL1 in the radiotherapy sensitivity of glioma, this study would dig deep into this aspect. Cancer stem cells (CSCs) isolated by magnetic bead assay were identified by microscopy, qRT-PCR and western blot. The number of apoptotic cells was counted 72 h after X-ray irradiation to evaluate the sensitivity of cancer cells to radiotherapy. The effects of radiotherapy, FOSL1 and miR-27a-5p on basic cell functions were detected by functional experiments. The expressions of FOSL1, apoptosis-related genes and miR-27a-5p were detected by qRT-PCR and western blot as needed. The differential expression of FOSL1 and the effect of miR-27a-5p on survival rate were analyzed using GEPIA and UALCAN, respectively. FOSL1 was found highly expressed in glioma cells and patients. The appearance of spherical cells and high expressions of CSC-related markers indicated the successful isolation of CSC-like cells. The increment of X-ray dose enhanced the sensitivity of cancer cells to radiotherapy. Radiotherapy down-regulated cell viability and the expressions of FOSL1 and Bcl-2, but up-regulated cell apoptosis and the expressions of cleaved caspase-3 and Bax, which could be partially reversed by overexpressed FOSL1 or further enhanced by shFOSL1. MiR-27a-5p was highly expressed in in patients with glioma, which was associated with poor prognosis, while shFOSL1-inhibited miR-27a-5p expression enhanced the sensitivity of glioma stem cells to radiotherapy. In vivo experiments further verified the results obtained from in vitro experiments. Silent FOSL1 strengthened the radiosensitivity of glioma by down-regulating miR-27a-5p.
















Similar content being viewed by others
Data Availability
The analyzed data sets generated during the study are available from the corresponding author on reasonable request.
References
Allen C, Her S, Jaffray DA (2017) Radiotherapy for cancer: present and future. Adv Drug Deliv Rev 109:1–2. https://doi.org/10.1016/j.addr.2017.01.004
Baek SJ et al (2015) Cancer stem cells: The potential of carbon ion beam radiation and new radiosensitizers (Review). Oncol Rep 34:2233–2237. https://doi.org/10.3892/or.2015.4236
Barros-Silva D et al (2018) MicroRNA-27a-5p regulation by promoter methylation and MYC signaling in prostate carcinogenesis. Cell Death Dis 9:167. https://doi.org/10.1038/s41419-017-0241-y
Baskar R, Lee KA, Yeo R, Yeoh KW (2012) Cancer and radiation therapy: current advances and future directions. Int J Med Sci 9:193–199. https://doi.org/10.7150/ijms.3635
Bradshaw A, Wickremsekera A, Tan ST, Peng L, Davis PF, Itinteang T (2016) Cancer stem cell hierarchy in glioblastoma multiforme. Front Surg 3:21. https://doi.org/10.3389/fsurg.2016.00021
Chari NS et al (2020) Disruption of TP63-miR-27a* feedback loop by mutant TP53 in head and neck cancer. J National Cancer Inst 112:266–277. https://doi.org/10.1093/jnci/djz097
Cho DY et al (2011) The role of cancer stem cells (CD133(+)) in malignant gliomas. Cell Transplant 20:121–125. https://doi.org/10.3727/096368910x532774
Colak S, Medema JP (2014) Cancer stem cells–important players in tumor therapy resistance. FEBS J 281:4779–4791. https://doi.org/10.1111/febs.13023
Dawood S, Austin L, Cristofanilli M (2014) Cancer stem cells: implications for cancer therapy. Oncology (Williston Park) 28(1101–1107):1110
Duan L et al (2020) Down-regulation of FOS-like antigen 1 enhances drug sensitivity in breast cancer. Int J Clin Exp Pathol 13:2092–2099
Dutton JW 3rd, Artwohl JE, Huang X, Fortman JD (2019) Assessment of Pain Associated with the Injection of Sodium Pentobarbital in Laboratory Mice (Mus musculus). J Am Assoc Lab Anim Sci 58:373–379. https://doi.org/10.30802/aalas-jaalas-18-000094
Fiscon G, Conte F, Paci P (2018) SWIM tool application to expression data of glioblastoma stem-like cell lines, corresponding primary tumors and conventional glioma cell lines. BMC Bioinform 19:436. https://doi.org/10.1186/s12859-018-2421-x
Huynh TT et al (2015) Pterostilbene suppressed irradiation-resistant glioma stem cells by modulating GRP78/miR-205 axis. J Nutrit Biochem 26:466–475. https://doi.org/10.1016/j.jnutbio.2014.11.015
Jarosz-Biej M, Smolarczyk R, Cichoń T, Kułach N (2019) Tumor microenvironment as A “Game Changer” in cancer radiotherapy. Int J Mol Sci. https://doi.org/10.3390/ijms20133212
Jiang X, Xie H, Dou Y, Yuan J, Zeng D, Xiao S (2020) Expression and function of FRA1 protein in tumors. Mol Biol Rep 47:737–752. https://doi.org/10.1007/s11033-019-05123-9
Kastan MB, Schlaffer E, Russo JE, Colvin OM, Civin CI, Hilton J (1990) Direct demonstration of elevated aldehyde dehydrogenase in human hematopoietic progenitor cells. Blood 75:1947–1950
Kim B (2017) Western blot techniques. Methods Mol Biol (Clifton, NJ) 1606:133–139. https://doi.org/10.1007/978-1-4939-6990-6_9
Kong L, Wu Q, Zhao L, Ye J, Li N, Yang H (2019) Effect of microRNA-27a-5p on apoptosis and inflammatory response of pancreatic acinar cells in acute pancreatitis by targeting PTEN. J Cell Biochem 120:15844–15850. https://doi.org/10.1002/jcb.28855
Lapointe S, Perry A, Butowski NA (2018) Primary brain tumours in adults. Lancet (London, England) 392:432–446. https://doi.org/10.1016/s0140-6736(18)30990-5
Lawrie TA et al (2019) Long-term neurocognitive and other side effects of radiotherapy, with or without chemotherapy, for glioma. Cochrane Database Syst Rev 8:Cd013047. https://doi.org/10.1002/14651858.CD013047.pub2
Mishra S, Yadav T, Rani V (2016) Exploring miRNA based approaches in cancer diagnostics and therapeutics. Crit Rev Oncol Hematol 98:12–23. https://doi.org/10.1016/j.critrevonc.2015.10.003
Mizuno K et al (2017) The microRNA expression signature of small cell lung cancer: tumor suppressors of miR-27a-5p and miR-34b-3p and their targeted oncogenes. J Hum Genet 62:671–678. https://doi.org/10.1038/jhg.2017.27
Mueller AK, Lindner K, Hummel R, Haier J, Watson DI, Hussey DJ (2016) MicroRNAs and their impact on radiotherapy for cancer. Radiat Res 185:668–677. https://doi.org/10.1667/rr14370.1
Nassar D, Blanpain C (2016) Cancer stem cells: basic concepts and therapeutic implications. Annu Rev Pathol 11:47–76. https://doi.org/10.1146/annurev-pathol-012615-044438
Ogawa D, Ansari K, Nowicki MO, Salińska E, Bronisz A, Godlewski J (2019) MicroRNA-451 inhibits migration of glioblastoma while making it more susceptible to conventional therapy. Non-coding RNA. https://doi.org/10.3390/ncrna5010025
Ostrom QT et al (2014) The epidemiology of glioma in adults: a “state of the science” review. Neuro Oncol 16:896–913. https://doi.org/10.1093/neuonc/nou087
Peitzsch C, Kurth I, Kunz-Schughart L, Baumann M, Dubrovska A (2013) Discovery of the cancer stem cell related determinants of radioresistance. Radiother Oncol 108:378–387. https://doi.org/10.1016/j.radonc.2013.06.003
Schmittgen TD, Livak KJ (2008) Analyzing real-time PCR data by the comparative C(T) method. Nat Protoc 3:1101–1108. https://doi.org/10.1038/nprot.2008.73
Thon N et al (2010) Presence of pluripotent CD133+ cells correlates with malignancy of gliomas. Mol Cell Neurosci 43:51–59. https://doi.org/10.1016/j.mcn.2008.07.022
Tsang J, Zhu J, van Oudenaarden A (2007) MicroRNA-mediated feedback and feedforward loops are recurrent network motifs in mammals. Mol Cell 26:753–767. https://doi.org/10.1016/j.molcel.2007.05.018
Vlashi E, Pajonk F (2015) Cancer stem cells, cancer cell plasticity and radiation therapy. Seminars Cancer Biol 31:28–35. https://doi.org/10.1016/j.semcancer.2014.07.001
Wan Y et al (2021) A super-enhancer driven by FOSL1 controls miR-21–5p expression in head and neck squamous cell carcinoma. Front Oncol 11:656628. https://doi.org/10.3389/fonc.2021.656628
Xing Y et al (2018) MiR-27a-5p regulates apoptosis of liver ischemia-reperfusion injury in mice by targeting Bach1. J Cell Biochem 119:10376–10383. https://doi.org/10.1002/jcb.27383
Xu JF, Fang J, Shen Y, Zhang JM, Liu WG, Shen H (2011) Should we reoperate for recurrent high-grade astrocytoma? J Neurooncol 105:291–299. https://doi.org/10.1007/s11060-011-0585-6
Yang YP et al (2012) Inhibition of cancer stem cell-like properties and reduced chemoradioresistance of glioblastoma using microRNA145 with cationic polyurethane-short branch PEI. Biomaterials 33:1462–1476. https://doi.org/10.1016/j.biomaterials.2011.10.071
Zhou L et al (2016) MiR-27a-3p functions as an oncogene in gastric cancer by targeting BTG2. Oncotarget 7:51943–51954. https://doi.org/10.18632/oncotarget.10460
Zhu J, Zhao YP, Zhang YQ (2020) Low expression of FOSL1 is associated with favorable prognosis and sensitivity to radiation/pharmaceutical therapy in lower grade glioma. Neurol Res 42:522–527. https://doi.org/10.1080/01616412.2020.1748323
Acknowledgements
Not applicable.
Funding
Not applicable.
Author information
Authors and Affiliations
Contributions
RL: Substantial contributions to conception and design. WC, NL, SD, ZS, LY: Data acquisition, data analysis and interpretation. RL: Drafting the article or critically revising it for important intellectual content. RL, WC, NL, SD, ZS, LY: Final approval of the version to be published. RL, WC, NL, SD, ZS, LY: Agreement to be accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of the work are appropriately investigated and resolved.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no conflicts of interest.
Consent for Publication
Not applicable.
Ethical Approval
Animal experiments involved in this study were approved by the Animal Experiment Ethics Committee of the First Affiliated Hospital, Guangzhou Medical University (FG201907010NWK).
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Li, R., Che, W., Liang, N. et al. Silent FOSL1 Enhances the Radiosensitivity of Glioma Stem Cells by Down-Regulating miR-27a-5p. Neurochem Res 46, 3222–3246 (2021). https://doi.org/10.1007/s11064-021-03427-6
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11064-021-03427-6