Abstract
The therapeutic value of mesenchymal stromal cells (MSCs) for various regenerative medicine applications, including hematopoietic stem cell transplantations (HSCT), has been well-established. Owing to their small numbers in vivo, it becomes necessary to expand them in vitro, which leads to a gradual loss of their regenerative capacity. Stress-induced mitogen-activated protein kinase p38 (p38 MAPK) signaling has been shown to compromise the MSC functions. Therefore, we investigated whether pharmacological inhibition of p38 MAPK signaling rejuvenates the cultured MSCs and boosts their functionality. Indeed, we found that the ex vivo expanded MSCs show activated p38 MAPK signaling and exhibit increased oxidative stress. These MSCs show a decreased ability to secrete salutary niche factors, thereby compromising their ability to support hematopoietic stem cell (HSC) self-renewal, proliferation, and differentiation. We, therefore, attempted to rejuvenate the cultured MSCs by pharmacological inhibition of p38 MAPK – a strategy broadly known as “priming of MSCs”. We demonstrate that priming of MSCs with a p-38 MAPK inhibitor, PD169316, boosts their niche-supportive functions via upregulation of various HSC-supportive transcription factors. These primed MSCs expand multipotent HSCs having superior homing and long-term reconstitution ability. These findings shed light on the significance of non-cell-autonomous mechanisms operative in the hematopoietic niche and point towards the possible use of pharmacological compounds for rejuvenation of ex vivo cultured MSCs. Such approaches could improve the outcome of regenerative therapies involving in vitro cultured MSCs.
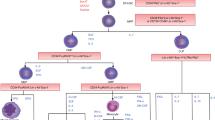
Graphical abstract






Similar content being viewed by others
Data Availability
The article and its supplementary information files contain all data generated or analyzed during this study.
References
Jayaraman, P., Lim, R., Ng, J., & Vemuri, M. C. (2021). Acceleration of translational mesenchymal stromal cell therapy through consistent quality GMP manufacturing. Frontiers in Cell and Developmental Biology, 9, 648472. https://doi.org/10.3389/fcell.2021.648472
Budgude, P., Kale, V., & Vaidya, A. (2020). Mesenchymal stromal cell-derived extracellular vesicles as cell-free biologics for the ex vivo expansion of Hematopoietic stem cells. Cell Biology International, 44(5), 1078–1102. https://doi.org/10.1002/cbin.11313
Allan, D., Tieu, A., Lalu, M., & Burger, D. (2020). Mesenchymal stromal cell-derived extracellular vesicles for regenerative therapy and immune modulation: Progress and challenges toward clinical application. Stem Cells Translational Medicine, 9(1), 39–46. https://doi.org/10.1002/sctm.19-0114
Fajardo-Orduña, G. R., Mayani, H., & Montesinos, J. J. (2015). Hematopoietic support capacity of mesenchymal stem cells: Biology and clinical potential. Archives of Medical Research, 46(8),589–596. https://doi.org/10.1016/j.arcmed.2015.10.001
Kumar, S., & Geiger, H. (2017). HSC niche biology and HSC expansion ex vivo. Trends in Molecular Medicine, 23(9), 799–819. https://doi.org/10.1016/j.molmed.2017.07.003
Man, Y., Yao, X., Yang, T., & Wang, Y. (2021). Hematopoietic stem cell niche during homeostasis, malignancy, and bone marrow transplantation. Frontiers in Cell and Developmental Biology, 9, 14. https://doi.org/10.3389/fcell.2021.621214
Fernandez-Rebollo, E., Franzen, J., Goetzke, R., Hollmann, J., Ostrowska, A., Oliverio, M., … Wagner, W. (2020). Senescence-associated metabolomic phenotype in primary and iPSC-derived mesenchymal stromal cells. Stem cell reports, 14(2), 201–209. https://doi.org/10.1016/j.stemcr.2019.12.012
Andrzejewska, A., Catar, R., Schoon, J., Qazi, T. H., Sass, F. A., Jacobi, D., … Streitz, M. (2019). Multi-parameter analysis of biobanked human bone marrow stromal cells shows little influence for donor age and mild comorbidities on phenotypic and functional properties. Frontiers in Immunology, 10, 2474. https://doi.org/10.3389/fimmu.2019.02474
Yin, J. Q., Zhu, J., & Ankrum, J. A. (2019). Manufacturing of primed mesenchymal stromal cells for therapy. Nature Biomedical Engineering, 3, 90–104. https://doi.org/10.1038/s41551-018-0325-8
Turinetto, V., Vitale, E., & Giachino, C. (2016). Senescence in human mesenchymal stem cells: Functional changes and implications in stem cell-based therapy. International Journal of Molecular Sciences, 17(7), 1164. https://doi.org/10.3390/ijms17071164
Kim, M., Kim, C., Choi, Y. S., Kim, M., Park, C., & Suh, Y. (2012). Age-related alterations in mesenchymal stem cells related to shift in differentiation from osteogenic to adipogenic potential: Implication to age-associated bone diseases and defects. Mechanisms of Ageing and Development, 133(5), 215–225. https://doi.org/10.1016/j.mad.2012.03.014
Hu, C., Zhao, L., Peng, C., & Li, L. (2018). Regulation of the mitochondrial reactive oxygen species: Strategies to control mesenchymal stem cell fates ex vivo and in vivo. Journal of Cellular and Molecular Medicine, 22(11), 5196–5207. https://doi.org/10.1111/jcmm.13835
Nakahara, F., Borger, D. K., Wei, Q., Pinho, S., Maryanovich, M., Zahalka, A. H., … Xu, C. (2019). Engineering a haematopoietic stem cell niche by revitalizing mesenchymal stromal cells. Nature Cell Biology, 21(5), 560–567. https://doi.org/10.1038/s41556-019-0308-3
Singh, P., Kacena, M. A., Orschell, C. M., & Pelus, L. M. (2020). Aging-related reduced expression of CXCR4 on bone marrow mesenchymal stromal cells contributes to hematopoietic stem and progenitor cell defects. Stem Cell Reviews and Reports, 16, 684–692. https://doi.org/10.1007/s12015-020-09974-9
Fitzsimmons, R. E. B., Mazurek, M. S., Soos, A., & Simmons, C. A. (2018). Mesenchymal stromal/stem cells in regenerative medicine and tissue engineering. Stem Cells International, 2018, 1–16. https://doi.org/10.1155/2018/8031718
Singh, S., Moirangthem, R. D., Vaidya, A., Jalnapurkar, S., Limaye, L., & Kale, V. (2016). AKT signaling prevailing in mesenchymal stromal cells modulates the functionality of hematopoietic stem cells via intercellular communication. Stem Cells, 34(9), 2354–2367. https://doi.org/10.1002/stem.2409
Moirangthem, R. D., Singh, S., Adsul, A., Jalnapurkar, S., Limaye, L., & Kale, V. P. (2015). Hypoxic niche-mediated regeneration of hematopoiesis in the engraftment window is dominantly affected by oxygen tension in the milieu. Stem Cells and Development, 24(20), 2423–2436. https://doi.org/10.1089/scd.2015.0112
Kulkarni, R., Bajaj, M., Ghode, S., Jalnapurkar, S., Limaye, L., & Kale, V. P. (2018). Intercellular transfer of microvesicles from young mesenchymal stromal cells rejuvenates aged murine hematopoietic stem cells. Stem Cells, 36(3), 420–433. https://doi.org/10.1002/stem.2756
Jalnapurkar, S., Moirangthem, R. D., Singh, S., Limaye, L., & Kale, V. (2018). Microvesicles secreted by nitric oxide-primed mesenchymal stromal cells boost the engraftment potential of hematopoietic stem cells. Stem Cells, 37(1), 128–138. https://doi.org/10.1002/stem.2912
Maruyama, J., Naguro, I., Takeda, K., & Ichijo, H. (2009). Stress-activated MAP kinase cascades in cellular senescence. Current Medicinal Chemistry, 16(10), 1229–1235. https://doi.org/10.2174/092986709787846613
Yong, H.-Y., Koh, M.-S., & Moon, A. (2009). The p38 MAPK inhibitors for the treatment of inflammatory diseases and cancer. Expert Opinion on Investigational Drugs, 18(12), 1893–1905. https://doi.org/10.1517/13543780903321490
Anton, D. B., Ducati, R. G., Timmers, L. F. S. M., Laufer, S., & Goettert, M. I. (2021). A special view of what was almost forgotten: P38δ MAPK. Cancers, 13(9), 2077. https://doi.org/10.3390/cancers13092077
Ito, K., Hirao, A., Arai, F., Takubo, K., Matsuoka, S., Miyamoto, K., … Suda, T. (2006). Reactive oxygen species act through p38 MAPK to limit the lifespan of hematopoietic stem cells. Nature Medicine, 12(4), 446–451. https://doi.org/10.1038/nm1388
Wang, Y., Liu, L., & Zhou, D. (2011). Inhibition of p38 MAPK attenuates ionizing radiation-induced hematopoietic cell senescence and residual bone marrow injury. Radiation Research, 176(6), 743–752. https://doi.org/10.1667/rr2727.1
Zou, J., Zou, P., Lou, Y., Xiao, Y., Wang, J., & Liu, L. (2011). The cross-talk between ROS and p38MAPKα in the ex vivo expanded human umbilical cord blood CD133+ cells. Journal of Huazhong University of Science and Technology [Medical Sciences], 31(5), 591–595. https://doi.org/10.1007/s11596-011-0566-1
Li, D., Wang, Y., Wu, H., Lu, L., Zhang, H., Chang, J., … Meng, A. (2011). Mitigation of ionizing radiation-induced bone marrow suppression by p38 inhibition and G-CSF administration. Journal of Radiation Research, 52(6), 712–716. https://doi.org/10.1269/jrr.11007
Lu, L., Wang, Y. Y., Zhang, J. L., Li, D. G., & Meng, A. M. (2016). p38 MAPK inhibitor insufficiently attenuates HSC senescence administered long-term after 6 gy total body irradiation in mice. International Journal of Molecular Sciences, 17(6), 905. https://doi.org/10.3390/ijms17060905
Jung, H., Kim, D. O., Byun, J. E., Kim, W. S., Kim, M. J., Song, H. Y., … Choi, I. (2016). Thioredoxin-interacting protein regulates haematopoietic stem cell ageing and rejuvenation by inhibiting p38 kinase activity. Nature Communications, 7, 1–12. https://doi.org/10.1038/ncomms13674
Navas, T. A., Mohindru, M., Estes, M., Ma, J. Y., Sokol, L., Pahanish, P., … Collins, R. (2006). Inhibition of overactivated p38 MAPK can restore hematopoiesis in myelodysplastic syndrome progenitors. Blood, 108(13), 4170–4177. https://doi.org/10.1182/blood-2006-05-023093
Saadatzadeh, M. R., Bijangi-Vishehsaraei, K., Kapur, R., & Haneline, L. S. (2009). Distinct roles of stress-activated protein kinases in Fanconi anemia type C–deficient hematopoiesis. Blood, The Journal of the American Society of Hematology, 113(12), 2655–2660. https://doi.org/10.1182/blood-2008-09-181420
Kale, V. P. (2019). Application of “primed” mesenchymal stromal cells in hematopoietic stem cell transplantation: Current status and future prospects. Stem Cells and Development, 28(22), 1473–1479. https://doi.org/10.1089/scd.2019.0149
Budgude, P., Kale, V., & Vaidya, A. (2021). Cryopreservation of mesenchymal stromal cell-derived extracellular vesicles using trehalose maintains their ability to expand hematopoietic stem cells in vitro. Cryobiology, 98, 152–163. https://doi.org/10.1016/j.cryobiol.2020.11.009
Wu, K. K. (2021). Control of mesenchymal stromal cell senescence by tryptophan metabolites. International Journal of Molecular Sciences, 22(2), 697. https://doi.org/10.3390/ijms22020697
Borodkina, A. V., Shatrova, A. N., Nikolsky, N. N., & Burova, E. B. (2016). The role of p38 MAP-kinase in stress-induced senescence of human endometrium-derived mesenchymal stem cells. Cell and Tissue Biology, 10(5), 365–371. https://doi.org/10.1134/S1990519X16050023
Papaconstantinou, J. (2019). The role of signaling pathways of inflammation and oxidative stress in development of senescence and aging phenotypes in cardiovascular disease. Cells, 8(11), 1383. https://doi.org/10.3390/cells8111383
Mendelson, A., & Frenette, P. S. (2014). Hematopoietic stem cell niche maintenance during homeostasis and regeneration. Nature Medicine, 20(8), 833–846. https://doi.org/10.1038/nm.3647
Liu, H., Xia, X., & Li, B. (2015). Mesenchymal stem cell aging: Mechanisms and influences on skeletal and non-skeletal tissues. Experimental Biology and Medicine, 240(8), 1099–1106. https://doi.org/10.1177/1535370215591828
Han, L., Wang, B., Wang, R., Gong, S., Chen, G., & Xu, W. (2019). The shift in the balance between osteoblastogenesis and adipogenesis of mesenchymal stem cells mediated by glucocorticoid receptor. Stem Cell Research & Therapy, 10(1), 1–14. https://doi.org/10.1186/s13287-019-1498-0
Pinho, S., & Frenette, P. S. (2019). Haematopoietic stem cell activity and interactions with the niche. Nature Reviews Molecular Cell Biology, 20(5), 303–320. https://doi.org/10.1038/s41580-019-0103-9
Ali, M. A. E., Fuse, K., Tadokoro, Y., Hoshii, T., Ueno, M., Kobayashi, M., … Hegazy, A. M. (2017). Functional dissection of hematopoietic stem cell populations with a stemness-monitoring system based on NS-GFP transgene expression. Scientific Reports, 7(1), 1–12. https://doi.org/10.1038/s41598-017-11909-3
Peng, C., Chen, Y., Shan, Y., Zhang, H., Guo, Z., Li, D., & Li, S. (2012). LSK derived LSK–cells have a high apoptotic rate related to survival regulation of hematopoietic and leukemic stem cells. PLoS ONE, 7(6), e38614. https://doi.org/10.1371/journal.pone.0038614
Challen, G. A., Boles, N., Lin, K. K., & Goodell, M. A. (2009). Mouse hematopoietic stem cell identification and analysis. Cytometry Part A: The Journal of the International Society for Advancement of Cytometry, 75(1), 14–24. https://doi.org/10.1002/cyto.a.20674
Lu, Z., Hong, C. C., Kong, G., Assumpção, A. L. F. V, Ong, I. M., Bresnick, E. H., … Pan, X. (2018). Polycomb group protein YY1 is an essential regulator of hematopoietic stem cell quiescence. Cell Reports, 22(6), 1545–1559. https://doi.org/10.1016/j.celrep.2018.01.026
Jalnapurkar, S., Singh, S., Devi, M. R., Limaye, L., & Kale, V. (2016). Nitric oxide has contrasting age-dependent effects on the functionality of murine hematopoietic stem cells. Stem Cell Research and Therapy, 7, 171. https://doi.org/10.1186/s13287-016-0433-x
Hock, H., Hamblen, M. J., Rooke, H. M., Schindler, J. W., Saleque, S., Fujiwara, Y., & Orkin, S. H. (2004). Gfi-1 restricts proliferation and preserves functional integrity of haematopoietic stem cells. Nature, 431(7011), 1002–1007. https://doi.org/10.1038/nature02994
Zeng, H., Yücel, R., Kosan, C., Klein-Hitpass, L., & Möröy, T. (2004). Transcription factor Gfi1 regulates self-renewal and engraftment of hematopoietic stem cells. The EMBO Journal, 23(20), 4116–4125. https://doi.org/10.1038/sj.emboj.7600419
Laricchia-Robbio, L., & Nucifora, G. (2008). Significant increase of self-renewal in hematopoietic cells after forced expression of EVI1. Blood Cells, Molecules, and Diseases, 40(2), 141–147. https://doi.org/10.1016/j.bcmd.2007.07.012
Chang, V. Y., Fang, T., Pohl, K. A., Tran, E., Himburg, H. A., & Chute, J. P. (2018). Epidermal Growth Factor Rejuvenates Aging Hematopoietic Stem Cells. Blood, 132(Supplement 1), 1284. https://doi.org/10.1182/blood-2018-99-119929
Ahmadnejad, M., Amirizadeh, N., Mehrasa, R., Karkhah, A., Nikougoftar, M., & Oodi, A. (2017). Elevated expression of DNMT1 is associated with increased expansion and proliferation of hematopoietic stem cells co-cultured with human MSCs. Blood Research, 52(1), 25. https://doi.org/10.5045/br.2017.52.1.25
Piryani, S. O., Kam, A. Y. F., Kliassov, E. G., Chen, B. J., Spector, N. L., Chute, J. P., … Doan, P. L. (2018). Epidermal growth factor and granulocyte colony stimulating factor signaling are synergistic for hematopoietic regeneration. Stem Cells, 36(2), 252–264. https://doi.org/10.1002/stem.2731
Kataoka, K., Sato, T., Yoshimi, A., Goyama, S., Tsuruta, T., Kobayashi, H., … Imai, Y. (2011). Evi1 is essential for hematopoietic stem cell self-renewal, and its expression marks hematopoietic cells with long-term multilineage repopulating activity. Journal of Experimental Medicine, 208(12), 2403–2416. https://doi.org/10.1084/jem.20110447
Ma, Z., Xu, J., Wu, L., Wang, J., Lin, Q., Chowdhury, F. A., … Du, W. (2020). Hes1 deficiency causes hematopoietic stem cell exhaustion. Stem Cells, 38(6), 756–768. https://doi.org/10.1002/stem.3169
Zhu, J., & Emerson, S. G. (2002). Hematopoietic cytokines, transcription factors and lineage commitment. Oncogene, 21(21), 3295–3313. https://doi.org/10.1038/sj.onc.1205318
Sharma, M., Afrin, F., Satija, N., Tripathi, R. P., & Gangenahalli, G. U. (2011). Stromal-derived factor-1/CXCR4 signaling: Indispensable role in homing and engraftment of hematopoietic stem cells in bone marrow. Stem Cells and Development, 20(6), 933–946. https://doi.org/10.1089/scd.2010.0263
Borodkina, A., Shatrova, A., Abushik, P., Nikolsky, N., & Burova, E. (2014). Interaction between ROS dependent DNA damage, mitochondria and p38 MAPK underlies senescence of human adult stem cells. Aging (Albany NY), 6(6), 481. https://doi.org/10.18632/aging.100673
Zhou, X., Hong, Y., Zhang, H., & Li, X. (2020). Mesenchymal stem cell senescence and rejuvenation: Current status and challenges. Frontiers in Cell and Developmental Biology, 8, 364. https://doi.org/10.3389/fcell.2020.00364
Baxter, M. A., Wynn, R. F., Jowitt, S. N., Wraith, J. E., Fairbairn, L. J., & Bellantuono, I. (2004). Study of telomere length reveals rapid aging of human marrow stromal cells following in vitro expansion. Stem Cells, 22(5), 675–682. https://doi.org/10.1634/stemcells.22-5-675
Elmansi, A. M., Hussein, K. A., Herrero, S. M., Periyasamy-Thandavan, S., Aguilar-Pérez, A., Kondrikova, G., … Kaiser, H. (2020). Age-related increase of kynurenine enhances miR29b-1-5p to decrease both CXCL12 signaling and the epigenetic enzyme Hdac3 in bone marrow stromal cells. Bone Reports, 12, 100270. https://doi.org/10.1016/j.bonr.2020.100270
Singh, P., Kacena, M. A., Orschell, C. M., & Pelus, L. M. (2017). Attenuation of CXCR4/SDF-1 axis in bone marrow mesenchymal stromal cells impairs hematopoietic niche activity and promotes stem cell aging. Blood, 130(Supplement 1), 92. https://doi.org/10.1182/blood.V130.Suppl_1.92.92
Singh, P., Mohammad, K. S., & Pelus, L. M. (2020). CXCR4 expression in the bone marrow microenvironment is required for hematopoietic stem and progenitor cell maintenance and early hematopoietic regeneration after myeloablation. Stem Cells, 38(7), 849–859. https://doi.org/10.1002/stem.3174
Shao, H., Xu, Q., Wu, Q., Ma, Q., Salgueiro, L., Wang, J., … Yu, H. (2011). Defective CXCR4 expression in aged bone marrow cells impairs vascular regeneration. Journal of Cellular and Molecular Medicine, 15(10), 2046–2056. https://doi.org/10.1111/j.1582-4934.2010.01231.x
Li, H., Hao, L., Li, Y., & Wang, R. (2018). Reducing CXCR4 resulted in impairing proliferation and promoting aging. The Journal of Nutrition, Health & Aging, 22(7), 785–789. https://doi.org/10.1007/s12603-018-1013-9
Alicka, M., Kornicka-Garbowska, K., Kucharczyk, K., Kępska, M., Rӧcken, M., & Marycz, K. (2020). Age-dependent impairment of adipose-derived stem cells isolated from horses. Stem Cell Research & Therapy, 11(1), 1–20. https://doi.org/10.1186/s13287-019-1512-6
Li, J., Zuo, B., Zhang, L., Dai, L., & Zhang, X. (2018). Osteoblast versus adipocyte: Bone marrow microenvironment-guided epigenetic control. Case Reports in Orthopedic Research, 1(1), 2–18. https://doi.org/10.1159/000489053
Perucca, S., Di Palma, A., Piccaluga, P. P., Gemelli, C., Zoratti, E., Bassi, G., … Russo, D. (2017). Mesenchymal stromal cells (MSCs) induce ex vivo proliferation and erythroid commitment of cord blood haematopoietic stem cells (CB-CD34+ cells). PLoS ONE, 12(2), e0172430. https://doi.org/10.1371/journal.pone.0172430
Klamer, S. E., Dorland, Y. L., Kleijer, M., Geerts, D., Lento, W. E., van der Schoot, C. E., … Voermans, C. (2018). TGFBI expressed by bone marrow niche cells and hematopoietic stem and progenitor cells regulates hematopoiesis. Stem Cells and Development, 27(21), 1494–1506. https://doi.org/10.1089/scd.2018.0124
Frenette, P. S., Pinho, S., Lucas, D., & Scheiermann, C. (2013). Mesenchymal stem cell: Keystone of the hematopoietic stem cell niche and a stepping-stone for regenerative medicine. Annual Review of Immunology, 31, 285–316. https://doi.org/10.1146/annurev-immunol-032712-095919
Coulthard, L. R., White, D. E., Jones, D. L., McDermott, M. F., & Burchill, S. A. (2009). p38MAPK: Stress responses from molecular mechanisms to therapeutics. Trends in Molecular Medicine, 15(8), 369–379. https://doi.org/10.1016/j.molmed.2009.06.005
Leestemaker, Y., de Jong, A., Witting, K. F., Penning, R., Schuurman, K., Rodenko, B., … Heck, A. J. R. (2017). Proteasome activation by small molecules. Cell Chemical Biology, 24(6), 725–736. https://doi.org/10.1016/j.chembiol.2017.05.010
Zhang, Z., Wang, B., Wu, S., Wen, Y., Wang, X., Song, X., … Chen, W. (2017). PD169316, a specific p38 inhibitor, shows antiviral activity against Enterovirus71. Virology, 508, 150–158. https://doi.org/10.1016/j.virol.2017.05.012
Acknowledgements
The authors wish to thank Symbiosis Centre for Research & Innovation, Symbiosis International (Deemed University) for providing infrastructural support.
Funding
This study was funded by Department of Biotechnology (DBT), Ministry of Science & Technology, New Delhi, Government of India. P.B. was provided with Junior Research Fellowship (JRF) by DBT under this project (No.BT/PR23620/MED/31/368/2017).
Author information
Authors and Affiliations
Contributions
Pallavi Budgude: Investigation, Validation, Formal Analysis, Writing – original draft preparation; Vaijayanti Kale: Conceptualization, Methodology, Formal Analysis, Reviewing & Editing; Anuradha Vaidya: Conceptualization, Visualization, Methodology, Formal Analysis, Resources, Writing—Reviewing & Editing, Supervision, Project Administration, Funding Acquisition.
Corresponding author
Ethics declarations
Conflict of Interest
The authors declare no conflict of interest.
Ethics Approval
All the animal experiments were reviewed and approved by the Institutional Animal Ethics Committee (IAEC) of the Symbiosis School of Biological Sciences (SSBS) (Approval Number: SSBS/IAEC/09–2016).
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
12015_2021_10240_MOESM1_ESM.pdf
Supplementary file1 (PDF 1853 KB) Fig. S1: (A) The graph depicts the quantification of native p38 MAPK and p-p38 MAPK in naïve and primed MSCs as determined by densitometry of bands obtained in the blots. (B) The bar represents the ratio of phosphorylated p38 MAPK to native p38 MAPK protein. (C) The graph depicts percent cell viability of MSCs after treatment with DMSO and 10µM PD169316 for 24 and 48h, respectively (n=3). (D) A representative phase contrast image showing the morphology of ex vivo expanded MSCs when treated with DMSO and 10µM PD169316 for 24 and 48h. (10X magnification, scale = 20µm). (E) The frequency of DCF+ cells and (F) Mean Fluorescence Intensity (MFI) of DCF was measured using flow cytometry to determine the levels of intracellular ROS in naïve and primed MSCs. The data are represented as mean ± SD. ***p≤0.001
12015_2021_10240_MOESM2_ESM.pdf
Supplementary file2 (PDF 2173 KB) Fig. S2: Phase contrast images showing the ex vivo expansion of HSCs when they were co-cultured with (A) naïve and (B) primed MSCs (10X magnification), respectively. (C) The graph represents the total number of nucleated cells (TNCs) (n=25). (D-F) Flow panels depicting the frequency of HSC subsets such as (D) Lin- (upper panel), (E) LSK (middle panel), (F) LT-HSC and ST-HSC (lower panel) in HSCs co-cultured with naïve and primed MSCs. (G-I) Graphs depict the absolute numbers of (G) Lin-, (H) LSK, (I) LT-HSCs and ST-HSCs subsets in HSCs co-cultured with naïve and primed MSCs. The absolute number of each HSC subset was calculated from the total hematopoietic output and the percentage obtained in flow cytometry analysis (n=4). The data are represented as mean ± SD. * p≤0.05, ** p≤0.01, ***p≤0.001
12015_2021_10240_MOESM3_ESM.pdf
Supplementary file3 (PDF 329 KB) Fig. S3: Gating strategy used to determine the different HSC progenitors by flow cytometry is shown
12015_2021_10240_MOESM4_ESM.pdf
Supplementary file4 (PDF 541 KB) Fig. S4: (A-D) Flow panels depicting the frequency of HSC progenitors such as (A-B) CLPs (left panels) and (C-D) CMP, GMP and MEP (middle panels) in HSCs co-cultured with naïve and primed MSCs. (E-F) Flow panels depicting the frequency of CXCR4+ cells in naïve and primed LSK HSCs (right panels).
Rights and permissions
About this article
Cite this article
Budgude, P., Kale, V. & Vaidya, A. Pharmacological Inhibition of p38 MAPK Rejuvenates Bone Marrow Derived-Mesenchymal Stromal Cells and Boosts their Hematopoietic Stem Cell-Supportive Ability. Stem Cell Rev and Rep 17, 2210–2222 (2021). https://doi.org/10.1007/s12015-021-10240-9
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12015-021-10240-9