Abstract
Introduction
This study aimed to examine the medication prescriptions for hypertension in a class 1 and grade A hospital in Shanxi province to provide references for clinical rational drug use.
Methods
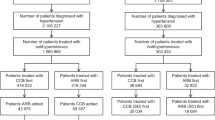
An inpatient medical record inquiry system was used to evaluate the use of antihypertensives in a hypertensive population (age ≥ 18 years old) who received a prescription for one or more antihypertensives between January 2017 and December 2019. The hypertensive population was categorized into grades (1, 2, and 3), age groups, and different comorbidities to analyze the medication prescriptions. Drug analysis included angiotensin-converting enzyme inhibitor (ACEI), angiotensin receptor antagonist (ARB), calcium channel blocker (CCB), diuretics, and beta-receptor blockers (B-RB). SPSS16.0 was used for statistical analysis, including one-way analysis of variance (ANOVA,) chi-squared test, and multifactor logistic regression analysis.
Results
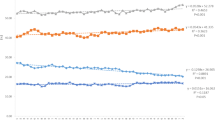
The overall control rate of blood pressure was 60.79%. The control rates of single, double, triple, and quadruple antihypertensives were 70.08%, 59.97%, 56.27%, and 45.23%, respectively. There were more cases of grade 3 than grades 1 and 2. The 18–65 years group was larger than the 66–79 years and ≥ 80 years groups. With the increase in grade, the prescription rate of the single drug decreased and the prescription rate of the combination drug increased, but this phenomenon was not obvious in different age groups. The most common drug prescribed for monotherapy was CCB; CCB combined with B-RB had the highest drug use in the double group by age or grade. Statistically significant differences were detected in the type of comorbidities between different age groups (P < 0.001), while only some differences were observed between different grades. Also, statistically significant differences were observed in the drugs prescribed for patients with hypertension with different comorbidities (P < 0.001). Factors influencing the efficiency of antihypertensives included sex, age, diabetes, heart failure, and usage of CCB and B-RB. The prescription rate of ARB combined with B-RB was relatively higher in grade 2 cases. B-RB was the primary drug for patients with diabetes, significantly increasing the blood glucose level.
Conclusions
The medication prescription of this hospital was in line with the requirements of China’s hypertension prevention and treatment guidelines. The pathophysiology of patients with hypertension in different age groups, increased use of combination drugs, and rational drug requirement should be considered when prescribing drugs.




Similar content being viewed by others
References
2018 Chinese Guidelines for the Management of Hypertension. Chin J Cardiovasc Med. 2019;24(01):24–56.
Lewington S, Clarke R, Qizilbash N, Peto R, Collins R, Prospective Studies Collaboration. Age-specific relevance of usual blood pressure to vascular mortality: a meta-analysis of individual data for one million adults in 61 prospective studies. Lancet. 2002;360(9349):1903–13.
Lu J, Lu Y, Wang X, et al. Prevalence, awareness, treatment, and control of hypertension in China: data from 17 million adults in a population based screening study (China PEACE Million Persons Project). Lancet. 2017;390(10112):2549–58.
Levey AS, Stevens LA, Schmid CH, et al. A new equation to estimate glomerular filtration rate. Ann Intern Med. 2009;150:604–12.
Peixoto MF, Cesaretti M, Hood SD, Tavares A. Effects of SSRI medication on heart rate and blood pressure in individuals with hypertension and depression. Clin Exp Hypertens. 2019;41(5):428–33.
Shen C, Zhou Z, Lai S, et al. Urban-rural-specific trend in prevalence of general and central obesity, and association with hypertension in Chinese adults, aged 18–65 years. BMC Public Health. 2019;19(1):661.
Wang Y, Zhou Q, Gao WH, et al. Association of plasma cyclooxygenase-2 levels and genetic polymorphisms with salt sensitivity, blood pressure changes and hypertension incidence in Chinese adults. J Hypertens. 2020;38(9):1745–54.
Zhang Y. The influence of community nursing intervention on the life quality of elderly patients with hypertension. Contin Med Educ. 2019;33(07):166–8.
Yang Y. The value of health education in the cognition and treatment of hypertension in elderly patients. Contemp Med. 2020;26(13):180–1.
Delgado J, Masoli JAH, Bowman K, et al. Outcomes of treated hypertension at age 80 and older: cohort analysis of 79,376 individuals. J Am Geriatr Soc. 2017;65(5):995–1003.
Derington CG, King JB, Herrick JS, et al. Trends in antihypertensive medication monotherapy and combination use among US adults, national health and nutrition examination survey 2005–2016. Hypertension. 2020;75:973–81.
Franklin SS, Lopez VA, Wong ND, et al. Single versus combined blood pressure components and risk for cardiovascular disease: the Framingham Heart Study. Circulation. 2009;119(2):243–50.
Zhang Y, Yang H, Wang R, et al. An analysis of medication prescriptions for hypertension in urban and rural residents in Tianjin. Adv Ther. 2020;37(10):4414–26.
Yamada Y, Miyajima E, Tochikubo O, Matsukawa T, Ishii M. Age-related changes in muscle sympathetic nerve activity in essential hypertension. Hypertension. 1989;13(6 Pt 2):870–7.
Collins KJ. Age-related changes in autonomic control: the use of beta blockers in the treatment of hypertension. Cardiovasc Drugs Ther. 1991;4(Suppl6):1257–62.
Shimamoto K, Ando K, Fujita T, et al. The Japanese Society of Hypertension Guidelines for the Management of Hypertension (JSH 2014). Hypertens Res. 2014;37:253–390.
Fonseca VA. Effects of beta-blockers on glucose and lipid metabolism. Curr Med Res Opin. 2010;26(3):615–29.
Hollenberg NK. The antihypertensive and lipid-lowering treatment to prevent heart attack trial (ALLHAT). Major outcomes in high-risk hypertensive patients randomized to angiotensin-converting enzyme inhibitor or calcium channel blocker vs diuretic. Curr Hypertens Rep. 2003;5(3):183–5.
Leenen FH, Nwachuku CE, Black HR, et al. Clinical events in high-risk hypertensive patients randomly assigned to calcium channel blocker versus angiotensin-converting enzyme inhibitor in the antihypertensive and lipid-lowering treatment to prevent heart attack trial. Hypertension. 2006;48(3):374–84.
Liu G, Zeng G, Hong X. Long-acting calcium antagonist is the best choice of antihypertensive therapy for Chinese hypertensive population. Chin Commun Dr. 2011;13(01):10–1.
Langrish JP, Mills NL, Bath LE, et al. Cardiovascular effects of physiological and standard sex steroid replacement regimens in premature ovarian failure. Hypertension. 2009;53(5):805–11.
William BW, Vladimir H, Vijay C, Bertram P. Effects of a new hormone therapy, drospirenone and 17-beta-estradiol, in postmenopausal women with hypertension. Hypertension. 2006;48(2):264–74.
Strong RK, Page HM, Teresa C-C, James R, William CS, Jeffrey RB. Estrogen stimulates heat shock protein 90 binding to endothelial nitric oxide synthase in human vascular endothelial cells. Effects on calcium sensitivity and NO release. J Biol Chem. 2000;275(7):5026–30.
Tazumi S, Yokota N, Kawakami M, Omoto S, Takamata A, Morimoto K. Effects of estrogen replacement on stress-induced cardiovascular responses via renin-angiotensin system in ovariectomized rats. Am J Physiol Regul Integr Comp Physiol. 2016;311(5):R898–905.
Lekontseva O, Chakrabarti S, Davidge ST. Endothelin in the female vasculature: a role in aging. Am J Physiol Regul Integr Comp Physiol. 2010;298(3):R509–16.
American College of Cardiology Foundation Board. ACCF/AHA 2011 Expert Consensus Document on Hypertension in the Elderly. JACC. 2011;57(20):1–78.
Schoenenberger AW, Erne P, Stuck AE. Die arterielle Hypertonie im Alter [Hypertension in the elderly]. Ther Umsch. 2012;69(5):299–304.
Ozawa M, Tamura K, Iwatsubo K, et al. Ambulatory blood pressure variability is increased in diabetic hypertensives. Clin Exp Hypertens. 2008;30(3–4):213–24.
Parati G, Ochoa JE, Salvi P, Lombardi C, Bilo G. Prognostic value of blood pressure variability andaverage blood pressure levels in patients with hypertension and diabetes. Diabetes Care. 2013;36(Supplement 2):S312–24.
Ruiz J, Monbaron D, Parati G, et al. Diabetic neuropathy is a more important determinant of baroreflex sensitivity than carotid elasticity in type 2 diabetes. Hypertension. 2005;46(1):162–7.
Frattola A, Parati G, Gamba P, et al. Time and frequency domain estimates of spontaneous baroreflex sensitivity provide early detection of autonomic dysfunction in diabetes mellitus. Diabetologia. 1997;40(12):1470–5.
Rothwell PM. Limitations of the usual blood pressure hypothesis and importance of variability, instability, and episodic hypertension. Lancet. 2010;375(9718):938–48.
Acknowledgements
Funding
The authors funded the study and the Journal’s rapid service fee.
Authorship
All named authors meet the International Committee of Medical Journal Editors (ICMJE) criteria for authorship for this article, take responsibility for the integrity of the work as a whole, and have given their approval for this version to be published.
Disclosures
Zhen Li, Siyang Wang, Tingting Zhi, Hongxia Wang, Yuanyuan Zhu, Jian Ren, Yanhui Wang, Zhiqing Yao, Huizi Zhang, Jinxin Feng, and Ruiqing Zhang have nothing to disclose.
Authorship Contributions
Zhen Li: Conceptualization-Equal, Data curation-Equal, Formal analysis-Equal, Writing original draft-Supporting, Writing review and editing-Supporting. Siyang Wang: Conceptualization-Equal, Formal analysis-Equal, Investigation-Equal, Writing original draft-Lead, Writing, review & editing*Lead. Tingting Zhi: Data curation-Equal; Hongxia Wang: Data curation-Equal; Jian Ren: Data curation-Equal, Writing original; Yuanyuan Zhu: Formal analysis-Equal, Supervision-Equal; Yanhui Wang: Data curation-Equal, Formal analysis-Equal; Zhiqing Yao: Data curation-Equal, Formal analysis-Equal; Huizi Zhang: Data curation-Equal; Jinxin Feng: Data curation-Equal;Ruiqin Zhang: Conceptualization-Equal, Formal analysis-Equal, Writing review & editing-Supporting.
Compliance with Ethics Guidelines
This study was performed in accordance with the Helsinki Declaration of 1964 and its later amendments and approved by the ethics committee of The Second Hospital of Shanxi Medical University with waiver of informed consent. Approval No. (2020) XY No. (170).
Data Availability
All data generated or analyzed during this study are included in this published article.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Li, Z., Wang, S., Ren, J. et al. Analysis of Medication Prescriptions for Hypertension in a Class 1 and Grade A Hospital in Shanxi Province. Adv Ther 38, 5100–5115 (2021). https://doi.org/10.1007/s12325-021-01869-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12325-021-01869-6