Abstract
Purpose
We aimed to identify the joint associations of modifiable lifestyle and metabolic factors with the incidences of cardiovascular disease and all-cause mortality.
Methods
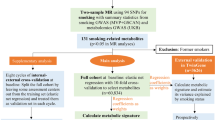
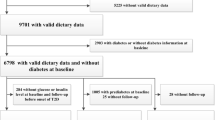
We recruited 94,831 participants (men, 79.76%; median age, 51.60 [43.47–58.87]) without a history of cardiovascular disease from the Kailuan study during 2006 and 2007 and followed them until a cardiovascular disease event, or death occurred, or until December 31, 2017. Baseline metabolic health status was assessed using Adult Treatment Panel III criteria, and details of the lifestyles of the participants were recorded using a self-reported questionnaire. We used Cox proportional hazards models to evaluate the joint associations.
Results
During a median follow-up of 11.03 years, we recorded 6590 cardiovascular disease events and 9218 all-cause mortality. Participants with the most metabolic risk components and the least healthy lifestyle had higher risk of cardiovascular disease (hazard ratio 2.06 [95% confidence interval (CI) 1.77–2.39]) and mortality (HR 1.53 [95% CI 1.31–1.78]), than participants with fewer metabolic risk components and the healthiest lifestyle. Compared with those in participants with the healthiest lifestyle, the HRs for cardiovascular disease in participants with the least healthy lifestyle were 1.26 (95% CI 1.17–1.37), 1.16 (95% CI 1.03–1.31), and 1.07 (95% CI 0.90–1.27) for those with low, medium, and high metabolic risk, respectively.
Conclusion
Healthy lifestyle is associated with a lower risk of cardiovascular disease and there is no significant interaction between metabolic risk and a healthy lifestyle. Therefore, a healthy lifestyle should be promoted, even for people with high metabolic risk.


Similar content being viewed by others
Data availability
Data are available to researchers on request for purposes of reproducing the results or replicating the procedure by directly contacting the corresponding author.
References
GBD 2017 Causes of Death Collaborators. Global, regional, and national age-sex-specific mortality for 282 causes of death in 195 countries and territories, 1980–2017: a systematic analysis for the Global Burden of Disease Study 2017. Lancet 392(10159), 1736–1788 (2018)
S.C. Cramer, W.J. Koroshetz, S.P. Finklestein, The case for modality-specific outcome measures in clinical trials of stroke recovery-promoting agents. Stroke 38(4), 1393–1395 (2007)
L.B. Goldstein, R. Adams, M.J. Alberts, L.J. Appel, L.M. Brass, C.D. Bushnell, A. Culebras, T.J. DeGraba, P.B. Gorelick, J.R. Guyton, R.G. Hart, G. Howard, M. Kelly-Hayes, J.V. Nixon, R.L. Sacco, Primary prevention of ischemic stroke: a guideline from the American Heart Association/American Stroke Association Stroke Council: cosponsored by the Atherosclerotic Peripheral Vascular Disease Interdisciplinary Working Group; Cardiovascular Nursing Council; Clinical Cardiology Council; Nutrition, Physical Activity, and Metabolism Council; and the Quality of Care and Outcomes Research Interdisciplinary Working Group. Circulation 113(24), e873–e923 (2006)
C.P. Wen, J.P. Wai, M.K. Tsai, Y.C. Yang, T.Y. Cheng, M.C. Lee, H.T. Chan, C.K. Tsao, S.P. Tsai, X. Wu, Minimum amount of physical activity for reduced mortality and extended life expectancy: a prospective cohort study. Lancet 378(9798), 1244–1253 (2011)
S.E. Chiuve, K.M. Rexrode, D. Spiegelman, G. Logroscino, J.E. Manson, E.B. Rimm, Primary prevention of stroke by healthy lifestyle. Circulation 118(9), 947–954 (2008)
T.T. van Sloten, M. Tafflet, M.C. Périer, A. Dugravot, R.E.D. Climie, A. Singh-Manoux, J.P. Empana, Association of change in cardiovascular risk factors with incident cardiovascular events. JAMA 320(17), 1793–1804 (2018)
M. Li, Y. Xu, Q. Wan, F. Shen, M. Xu, Individual and combined associations of modifiable lifestyle and metabolic health status with new-onset diabetes and major cardiovascular events: the China Cardiometabolic Disease and Cancer Cohort (4C) Study. Diabetes Care 43(8), 1929–1936 (2020)
A.S. Gami, B.J. Witt, D.E. Howard, P.J. Erwin, L.A. Gami, V.K. Somers, V.M. Montori, Metabolic syndrome and risk of incident cardiovascular events and death: a systematic review and meta-analysis of longitudinal studies. J. Am. Coll. Cardiol. 49(4), 403–414 (2007)
F.B. Hu, J.E. Manson, M.J. Stampfer, G. Colditz, S. Liu, C.G. Solomon, W.C. Willett, Diet, lifestyle, and the risk of type 2 diabetes mellitus in women. N. Engl. J. Med. 345(11), 790–797 (2001)
D. Mozaffarian, A. Kamineni, M. Carnethon, L. Djoussé, K.J. Mukamal, D. Siscovick, Lifestyle risk factors and new-onset diabetes mellitus in older adults: the cardiovascular health study. Arch. Intern. Med. 169(8), 798–807 (2009)
Y. Zhang, X.F. Pan, J. Chen, L. Xia, A. Cao, Y. Zhang, J. Wang, H. Li, K. Yang, K. Guo, M. He, A. Pan, Combined lifestyle factors and risk of incident type 2 diabetes and prognosis among individuals with type 2 diabetes: a systematic review and meta-analysis of prospective cohort studies. Diabetologia 63(1), 21–33 (2020)
X.F. Pan, Y. Li, O.H. Franco, J.M. Yuan, A. Pan, W.P. Koh, Impact of combined lifestyle factors on all-cause and cause-specific mortality and life expectancy in Chinese: the Singapore Chinese Health Study. J. Gerontol. Ser. A, Biol. Sci. Med. Sci 75(11), 2193-2199 (2019)
E.S. Horton, Effects of lifestyle changes to reduce risks of diabetes and associated cardiovascular risks: results from large scale efficacy trials. Obesity 17(Suppl 3), S43–S48 (2009)
S. Wu, Z. Huang, X. Yang, Y. Zhou, A. Wang, L. Chen, H. Zhao, C. Ruan, Y. Wu, A. Xin, K. Li, C. Jin, J. Cai, Prevalence of ideal cardiovascular health and its relationship with the 4-year cardiovascular events in a northern Chinese industrial city. Circ. Cardiovasc. Qual. Outcomes 5(4), 487–493 (2012)
A. Wang, Y. Sun, X. Liu, Z. Su, J. Li., Y. Luo, S. Chen, J. Wang, X. Li, Z. Zhao, H. Zhu, S. Wu, X. Guo, Changes in proteinuria and the risk of myocardial infarction in people with diabetes or pre-diabetes: a prospective cohort study. Cardiovasc Diabetol 16(1), 104 (2017)
C. Wang, Y. Yuan, M. Zheng, A. Pan, M. Wang, M. Zhao, Y. Li, S. Yao, S. Chen, S. Wu, H. Xue, Association of Age of onset of hypertension with cardiovascular diseases and mortality. J. Am. Coll. Cardiol. 75(23), 2921–2930 (2020)
S. Wu, Y. Song, S. Chen, M. Zheng, Y. Ma, L. Cui, J.B. Jonas, Blood pressure classification of 2017 associated with cardiovascular disease and mortality in young Chinese adults. Hypertension 76(1), 251–258 (2020)
C.E. Tan, S. Ma, D. Wai, S.K. Chew, E.S. Tai, Can we apply the National Cholesterol Education Program Adult Treatment Panel definition of the metabolic syndrome to Asians? Diabetes Care 27(5), 1182–1186 (2004)
X.Y. Li, X.L. Cai, P.D. Bian, L.R. Hu, High salt intake and stroke: meta-analysis of the epidemiologic evidence. CNS Neurosci. Ther. 18(8), 691–701 (2012)
D. Mozaffarian, S. Fahimi, G.M. Singh, R. Micha, S. Khatibzadeh, R.E. Engell, S. Lim, G. Danaei, M. Ezzati, J. Powles, Global sodium consumption and death from cardiovascular causes. N. Engl. J. Med. 371(7), 624–634 (2014)
S.M. El Dayem, A.A. Battah, M. El Bohy Ael, A. El Shehaby, El, E.A. Ghaffar, Relationship of plasma level of chemerin and vaspin to early atherosclerotic changes and cardiac autonomic neuropathy in adolescent type 1 diabetic patients. J. Pediatr. Endocrinol. Metab. 28(3–4), 265–273 (2015)
Y. Li, Z. Huang, C. Jin, A. Xing, Y. Liu, C. Huangfu, A.H. Lichtenstein, K.L. Tucker, S. Wu, X. Gao, Longitudinal change of perceived salt intake and stroke risk in a Chinese population. Stroke 49(6), 1332–1339 (2018)
S. Wu, S. An, W. Li, A.H. Lichtenstein, J. Gao, P.M. Kris-Etherton, Y. Wu, C. Jin, S. Huang, F.B. Hu, X. Gao, Association of trajectory of cardiovascular health score and incident cardiovascular disease. JAMA Netw. Open 2(5), e194758 (2019)
A. Wang, X. Liu, Z. Su, S. Chen, N. Zhang, Y. Wang, Y. Wang, S. Wu, Two-year changes in proteinuria and risk for myocardial infarction in patients with hypertension: a prospective cohort study. J. Hypertens. 35(11), 2295–2302 (2017)
World Health Organization. Recommendations on stroke prevention, diagnosis, and therapy. Report of the WHO Task Force on Stroke and other Cerebrovascular Disorders. Stroke 20(10), 1407–1431 (1989)
H. Tunstall-Pedoe, K. Kuulasmaa, P. Amouyel, D. Arveiler, A.M. Rajakangas, A. Pajak, Myocardial infarction and coronary deaths in the World Health Organization MONICA Project. Registration procedures, event rates, and case-fatality rates in 38 populations from 21 countries in four continents. Circulation 90(1), 583–612 (1994)
A. Towfighi, E.M. Cheng, V.A. Hill, F. Barry, M. Lee, N.P. Valle, B. Mittman, M. Ayala-Rivera, L. Moreno, A. Espinosa, H. Dombish, D. Wang, D. Ochoa, A. Chu, M. Atkins, B.G. Vickrey, Results of a pilot trial of a lifestyle intervention for stroke survivors: healthy eating and lifestyle after stroke. J. Stroke Cerebrovasc. Dis. 29(12), 105323 (2020)
J. Lv, C. Yu, Y. Guo, Z. Bian, L. Yang, Y. Chen, X. Hu, W. Hou, J. Chen, Z. Chen, L. Qi, L. Li, Adherence to a healthy lifestyle and the risk of type 2 diabetes in Chinese adults. Int. J. Epidemiol. 46(5), 1410–1420 (2017)
K.K. Teo, L. Liu, C.K. Chow, X. Wang, S. Islam, L. Jiang, J.E. Sanderson, S. Rangarajan, S. Yusuf, Potentially modifiable risk factors associated with myocardial infarction in China: the INTERHEART China study. Heart 95(22), 1857–1864 (2009)
R.J. Song, X.T. Nguyen, R. Quaden, Y.L. Ho, A.C. Justice, D.R. Gagnon, K. Cho, C.J. O’Donnell, J. Concato, J.M. Gaziano, L. Djoussé, Alcohol consumption and risk of coronary artery disease (from the Million Veteran Program). Am. J. Cardiol. 121(10), 1162–1168 (2018)
X.Y. Zhang, L. Shu, C.J. Si, X.L. Yu, D. Liao, W. Gao, L. Zhang, P.F. Zheng, Dietary patterns, alcohol consumption and risk of coronary heart disease in adults: a meta-analysis. Nutrients 7(8), 6582–6605 (2015)
Acknowledgements
The authors thank all study participants, their relatives, the members of the survey teams at the 11 regional hospitals of the Kailuan Medical Group, and the project development and management teams at the Beijing Tiantan Hospital and the Kailuan Group.
Funding
This study was funded by Beijing Municipal Administration of Hospitals Incubating Program (PX2020021), Beijing Excellent Talents Training Program (2018000021469G234), Young Elite Scientists Sponsorship Program by CAST (2018QNRC001), and National Key R&D Program of China (2018YFC1312400 and 2018YFC1312402).
Author information
Authors and Affiliations
Contributions
Y.Z. and H.L. wrote the manuscript. Y.Z., A.W., S.C., X.T., and H.L. collected the data. S.C. and X.T. researched data and contributed to discussion. S.W. and D.M. reviewed and edited the manuscript. A.W. contributed to the discussion and reviewed/edited the manuscript. All authors read and approved the final manuscript.
Corresponding authors
Ethics declarations
Conflict of interest
The authors declare no competing interests.
Ethical approval
The authors are accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved. The study was performed according to the guidelines of the Helsinki Declaration and was approved by the Ethics Committee of Kailuan General Hospital (approval number: 2006-05) and Beijing Tiantan Hospital (approval number: 2010-014-01). Written consents were obtained from all participants or their legal representatives.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
About this article
Cite this article
Zuo, Y., Li, H., Chen, S. et al. Joint association of modifiable lifestyle and metabolic health status with incidence of cardiovascular disease and all-cause mortality: a prospective cohort study. Endocrine 75, 82–91 (2022). https://doi.org/10.1007/s12020-021-02832-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12020-021-02832-9