Abstract
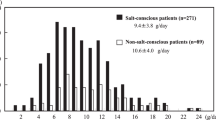
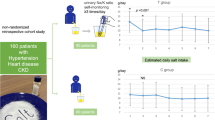
Reducing salt and increasing potassium intake are recommended lifestyle modifications for patients with hypertension. The estimated 24-h urinary salt excretion value from spot urine using Tanaka’s formula and the salt check-sheet scores, questionnaire-based scores of salt intake, are practical indices of daily salt intake. However, few studies have evaluated salt intake with these methods in hypertensive outpatients. We examined salt and potassium intake with the spot urine method and the salt check-sheet scores of hypertensive outpatients in a multi-facility, real-world setting and examined whether the salt or potassium intake evaluated with these methods related to inadequate blood pressure control. Hypertensive outpatients from 12 medical facilities in the Okinawa prefecture were enrolled from November 2011 to April 2014 (n = 1559, mean age 63.9 years, 46% women). The mean blood pressure, urinary salt excretion value, urinary potassium excretion value, and total score on the salt check-sheet were 129/75 mmHg, 8.7 g/day, 1.6 g/day, and 10.4 points, respectively. The urinary salt excretion value and total score on the salt check-sheet but not urinary potassium excretion value were associated with inadequate blood pressure control (≥140/90 mmHg). Higher body mass index, estimated glomerular filtration rate, urinary potassium excretion value, total score on the salt check-sheet, and presence of inadequate blood pressure control were associated with high urinary salt excretion (≥10.2 g/day). In conclusion, hypertensive outpatients with high urinary salt excretion values estimated using Tanaka’s formula or with high scores on the salt check sheet may be candidates for more intensive salt reduction guidance.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout


Similar content being viewed by others
Change history
31 August 2021
A Correction to this paper has been published: https://doi.org/10.1038/s41440-021-00742-x
References
Ministry of Health Labour and Welfare of Japan. Summary of results of National Health and Nutrition Survey in 2018. Ministry of Health Labour and Welfare of Japan; 2020.
Umemura S, Arima H, Arima S, Asayama K, Dohi Y, Hirooka Y, et al. The Japanese society of hypertension guidelines for the management of hypertension (JSH 2019). Hypertens Res. 2019;42:1235–481.
Tanaka T, Okamura T, Miura K, Kadowaki T, Ueshima H, Nakagawa H, et al. A simple method to estimate populational 24-h urinary sodium and potassium excretion using a casual urine specimen. J Hum Hypertens. 2002;16:97–103.
Kawano Y, Tsuchihashi T, Matsuura H, Ando K, Fujita T, Ueshima H. Working group for dietary salt reduction of the Japanese society of hypertension. Report of the working group for dietary salt reduction of the Japanese Society of Hypertension: (2) Assessment of salt intake in the management of hypertension. Hypertens Res. 2007;30:887–93.
Ministry of Health Labour and Welfare of Japan. Summary of results of National Health and Nutrition Survey in 2016. Ministry of Health Labour and Welfare of Japan; 2017.
Todoriki H, Willcox DC, Willcox BJ. The effects of post-war dietary change on longevity and health in Okinawa. Okinawan J Am Stud. 2004;1:52–61.
Yasutake K, Miyoshi E, Kajiyama T, Umeki Y, Misumi Y, Horita N, et al. Comparison of a salt check sheet with 24-h urinary salt excretion measurement in local residents. Hypertens Res. 2016;39:879–85.
Sakata S, Tsuchihashi T, Oniki H, Tominaga M, Arakawa K, Sakaki M, et al. Relationship between salt intake as estimated by a brief self-administered diet-history questionnaire (BDHQ) and 24-h urinary salt excretion in hypertensive patients. Hypertens Res. 2015;38:560–3.
Sasaki S, Yanagibori R, Amano K. Self-administered diet history questionnaire developed for health education: a relative validation of the test-version by comparison with 3-day diet record in women. J Epidemiol. 1998;8:203–15.
Ohe K, Yasutake K, Murata Y, Tsuchihashi T, Enjoji M. Assessment of dietary salt and sodium intake: from device to questionnaire. Qual Prim Care. 2017;25:101–8.
Ministry of Health Labour and Welfare of Japan. Overview of dietary reference intakes for Japanese. Tokyo, Japan: Ministry of Health Labour and Welfare of Japan; 2020.
Miyagawa N, Okuda N, Nakagawa H, Takezaki T, Nishi N, Takashima N, et al. Socioeconomic status associated with urinary sodium and potassium excretion in Japan: NIPPON DATA2010. J Epidemiol. 2018;28:S29–S34.
Iseki K, Iseki C, Itoh K, Uezono K, Sanefuji M, Ikemiya Y, et al. Urinary excretion of sodium and potassium in a screened cohort in Okinawa, Japan. Hypertens Res. 2002;25:731–6.
Kawasaki T, Itoh K, Uezono K, Sasaki H. A simple method for estimating 24 h urinary sodium and potassium excretion from second morning voiding urine specimen in adults. Clin Exp Pharmacol Physiol. 1993;20:7–14.
Ito S, Asakura K, Sugiyama K, Takakura M, Todoriki H. Salt and potassium intake estimated from spot urine in elementary school children and their mothers in Okinawa. Jpn J Health Hum Ecol. 2020;86:76–82.
Intersalt Cooperative Research Group. Intersalt: an international study of electrolyte excretion and blood pressure. Results for 24h urinary sodium and potassium excretion. BMJ. 1988;297:319–28.
Mente A, O’Donnell MJ, Rangarajan S, McQueen MJ, Poirier P, Wielgosz A, et al. PURE Investigators. Association of urinary sodium and potassium excretion with blood pressure. N. Engl J Med. 2014;371:601–11.
Cook NR, Appel LJ, Whelton PK. Sodium intake and all-cause mortality over 20 years in the trials of hypertension prevention. J Am Coll Cardiol. 2016;68:1609–17.
O’Donnell M, Mente A, Rangarajan S, McQueen MJ, Wang X, Liu L, et al. PURE Investigators. Urinary sodium and potassium excretion, mortality, and cardiovascular events. N Engl J Med. 2014;371:612–23.
Yasutake K, Miyoshi E, Misumi Y, Kajiyama T, Fukuda T, Ishii T, et al. Self-monitoring of urinary salt excretion as a method of salt-reduction education: a parallel, randomized trial involving two groups. Public Health Nutr. 2018;21:2164–73.
Ohta Y, Tsuchihashi T, Onaka U, Miyata E. Long-term compliance of salt restriction and blood pressure control status in hypertensive outpatients. Clin Exp Hypertens. 2010;32:234–8.
Isaka Y, Moriyama T, Kanda K. The SONG (Salt intake and OrigiN from General foods) Study - A Large-scale Survey of the Eating Habits and Dietary Salt Intake in the Working-age Population. Intern Med. 2017;56:2423–30.
Whelton PK, He J, Cutler JA, Brancati FL, Appel LJ, Follmann D, et al. Effects of oral potassium on blood pressure. Meta-analysis of randomized controlled clinical trials. JAMA. 1997;277:1624–32.
Aburto NJ, Hanson S, Gutierrez H, Hooper L, Elliott P, Cappuccio FP. Effect of increased potassium intake on cardiovascular risk factors and disease: systematic review and meta-analyses. BMJ. 2013;346:f1378.
WHO. Guideline: potassium intake for adults and children. Geneva: World Health Organization; 2009.
Tuekpe MK, Todoriki H, Sasaki S, Zheng KC, Ariizumi M. Potassium excretion in healthy Japanese women was increased by a dietary intervention utilizing home-parcel delivery of Okinawan vegetables. Hypertens Res. 2006;29:389–96.
Mano R, Ishida A, Ohya Y, Todoriki H, Takishita S. Dietary intervention with Okinawan vegetables increased circulating endothelial progenitor cells in healthy young women. Atherosclerosis. 2009;204:544–8.
Willcox DC, Scapagnini G, Willcox BJ. Healthy aging diets other than the Mediterranean: a focus on the Okinawan diet. Mech Ageing Dev. 2014;136-7:148–62.
Iwahori T, Ueshima H, Miyagawa N, Ohgami N, Yamashita H, Ohkubo T, et al. Six random specimens of daytime casual urine on different days are sufficient to estimate daily sodium/potassium ratio in comparison to 7-day 24-h urine collections. Hypertens Res. 2014;37:765–71.
Iwahori T, Ueshima H, Torii S, Saito Y, Fujiyoshi A, Ohkubo T, et al. Four to seven random casual urine specimens are sufficient to estimate 24-h urinary sodium/potassium ratio in individuals with high blood pressure. J Hum Hypertens. 2016;30:328–34.
Iwahori T, Ueshima H, Torii S, Saito Y, Kondo K, Tanaka-Mizuno S, et al. Diurnal variation of urinary sodium-to-potassium ratio in free-living Japanese individuals. Hypertens Res. 2017;40:658–64.
Acknowledgements
The authors are grateful for the cooperation from the staff of the collaborating medical facilities, particularly doctors T. Kikumura, N. Nagayoshi, M. Tomori, C. Imai, M. Matsuoka, and Y. Shinzato. The authors are also grateful to our clinical research coordinators, particularly M. Kobayashi and M. Nakahodo for retrieving data from the facilities and F. Aniya and K. Kohama for their excellent assistance as nutritionists.
Funding
This work was partly supported by the Grants-in-Aid for Scientific Research from the Japan Society for the Promotion of Science (grant number 2530891).
Author information
Authors and Affiliations
Contributions
MY, AS, and OY were involved in the conception and design of this article. MY, AS, AI, KK, TM, TT, YN, and OY were involved in planning and MY, AS, TT, MT, YH, TN, YN, and OY supervised the project at respective facilities. MY drafted and revised the manuscript. All authors discussed the results and contributed to the final manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
The original online version of this article was revised: " plus the same explanatory text of the problem as in the erratum/correction article
Supplementary information
Rights and permissions
About this article
Cite this article
Yamazato, M., Sakima, A., Ishida, A. et al. Salt and potassium intake evaluated with spot urine and brief questionnaires in combination with blood pressure control status in hypertensive outpatients in a real-world setting. Hypertens Res 44, 1316–1325 (2021). https://doi.org/10.1038/s41440-021-00707-0
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41440-021-00707-0
Keywords
This article is cited by
-
Associations between estimation of salt intake and salt-restriction spoons and hypertension status in patients with poorly controlled hypertension: a community-based study from Huzhou City, Eastern China
Nutrition Journal (2024)
-
Achievement rate of target blood pressure in patients with hypertension treated by hypertension specialists and non-specialists in a real-world setting
Hypertension Research (2023)
-
STEP to estimate cardiovascular events by home blood pressure in the era of digital hypertension
Hypertension Research (2022)