Abstract
Background
Patients with amnestic mild cognitive impairment (aMCI) present gait disturbances including slower speed and higher variability when compared to cognitively healthy individuals (CHI). Brain neuroimaging could explore higher levels of motor control. Our purpose was to look for an association between morphometrics and gait parameters in each group. We hypothesized that the relation between morphological cerebral alteration and gait speed are different following the group.
Methods
Fifty-three participants (30 with aMCI and 23 CHI) were recruited in this French cross-sectional study (mean 72 ± 5 years, 38% female). Gait speed and gait variability (coefficients of variation of stride time (STV) and stride length (SLV)) were measured using GAITrite® system. CAT12 software was used to analyse volume and surface morphometry like gray matter volume (GMV) and cortical thickness (CT). Age, gender and education level were used as potential cofounders.
Results
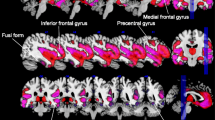
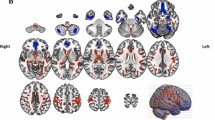
aMCI had slower gait speed and higher STV when compared to CHI. In aMCI the full adjusted linear regression model showed that lower gait speed was associated with decreased GMV and lower CT in bilateral superior temporal gyri (p < 0.36). In CHI, no association was found between gait speed and brain structure. Higher SLV was correlated with reduced GMV in spread regions (p < 0.05) and thinner cortex in the middle right frontal gyrus (p = 0.001) in aMCI. In CHI, higher SLV was associated with reduced GMV in 1 cluster: the left lingual (p = 0.041).
Conclusions
These findings indicate that lower gait speed is associated with specific brain structural changes as reduced GMV and CT during aMCI.



Similar content being viewed by others
References
Ali, P., Labriffe, M., Navasiolava, N., Custaud, M., Dinomais, M., Annweiler, C., & the SAM group. (2020). Vitamin D concentration and focal brain atrophy in older adults: A voxel-based morphometric study. Annals of Clinical Translational Neurology, 7, 554–558. https://doi.org/10.1002/acn3.50997
Allali, G., Montembeault, M., Brambati, S. M., Bherer, L., Blumen, H. M., Launay, C. P., Liu-Ambrose, T., Helbostad, J. L., Verghese, J., & Beauchet, O. (2019a). Brain structure covariance associated with gait control in aging. Journal of Gerontology Series A, 74, 705–713. https://doi.org/10.1093/gerona/gly123
Allali G, Montembeault M, Saj A, Wong CH, Cooper-Brown LA, Bherer L, Beauchet O (2019b) Structural brain volume covariance associated with gait speed in patients with amnestic and non-amnestic mild cognitive impairment: A double dissociation.Journal of Alzheimer's Disease, 1–11.https://doi.org/10.3233/JAD-190038.
Alzheimer’s Disease Neuroimaging Initiative (ADNI), Nho, K., Risacher, S. L., Crane, P. K., DeCarli, C., Glymour, M. M., Habeck, C., Kim, S., Lee, G. J., Mormino, E., Mukherjee, S., Shen, L., West, J. D., & Saykin, A. J. (2012). Voxel and surface-based topography of memory and executive deficits in mild cognitive impairment and Alzheimer’s disease. Brain Imaging and Behavior, 6, 551–567. https://doi.org/10.1007/s11682-012-9203-2
Annweiler, C., Beauchet, O., Bartha, R., & Montero-Odasso, M. (2013a). Slow gait in MCI is associated with ventricular enlargement: Results from the gait and brain study. Journal of Neural Transmission, 120, 1083–1092. https://doi.org/10.1007/s00702-012-0926-4
Annweiler, C., Beauchet, O., Bartha, R., Wells, J. L., Borrie, M. J., Hachinski, V., & Montero-Odasso, M. (2013b). Motor cortex and gait in mild cognitive impairment: A magnetic resonance spectroscopy and volumetric imaging study. Brain, 136, 859–871. https://doi.org/10.1093/brain/aws373
Ashburner, J. (2007). A fast diffeomorphic image registration algorithm. NeuroImage, 38, 95–113. https://doi.org/10.1016/j.neuroimage.2007.07.007
Ashburner, J., & Friston, K. J. (2000). Voxel-based morphometry—the methods. NeuroImage, 11, 805–821. https://doi.org/10.1006/nimg.2000.0582
Beauchet, O., Allali, G., Annweiler, C., Bridenbaugh, S., Assal, F., Kressig, R. W., & Herrmann, F. R. (2009). Gait variability among healthy adults: Low and high stride-to-stride variability are both a reflection of gait stability. Gerontology, 55, 702–706. https://doi.org/10.1159/000235905
Beauchet, O., Allali, G., Launay, C., Herrmann, F. R., & Annweiler, C. (2013). Gait variability at fast-pace walking speed: A biomarker of mild cognitive impairment? The Journal of Nutrition, Health & Aging, 17, 235–239. https://doi.org/10.1007/s12603-012-0394-4
Beauchet, O., Allali, G., Montero-Odasso, M., Sejdić, E., Fantino, B., & Annweiler, C. (2014). Motor phenotype of decline in cognitive performance among community-dwellers without dementia: Population-based study and meta-analysis. PLoS ONE, 9, e99318. https://doi.org/10.1371/journal.pone.0099318
Beauchet, O., Launay, C. P., Annweiler, C., & Allali, G. (2015). Hippocampal volume, early cognitive decline and gait variability: Which association? Experimental Gerontology, 61, 98–104. https://doi.org/10.1016/j.exger.2014.11.002
Beauchet, O., Montembeault, M., Barden, J. M., Szturm, T., Bherer, L., Liu-Ambrose, T., Chester, V. L., Li, K., Helbostad, J. L., & Allali, G. (2019). Brain gray matter volume associations with gait speed and related structural covariance networks in cognitively healthy individuals and in patients with mild cognitive impairment: A cross-sectional study. Experimental Gerontology, 122, 116–122. https://doi.org/10.1016/j.exger.2019.05.001
Beaudart, C., Rolland, Y., Cruz-Jentoft, A. J., Bauer, J. M., Sieber, C., Cooper, C., Al-Daghri, N., Araujo de Carvalho, I., Bautmans, I., Bernabei, R., Bruyère, O., Cesari, M., Cherubini, A., Dawson-Hughes, B., Kanis, J. A., Kaufman, J.-M., Landi, F., Maggi, S., McCloskey, E., … Fielding, R. A. (2019). Assessment of muscle function and physical performance in daily clinical practice : A position paper endorsed by the European Society for Clinical and Economic Aspects of Osteoporosis, Osteoarthritis and Musculoskeletal Diseases (ESCEO). Calcified Tissue International, 105, 1–14. https://doi.org/10.1007/s00223-019-00545-w
Bell-McGinty, S., Lopez, O. L., Meltzer, C. C., Scanlon, J. M., Whyte, E. M., Dekosky, S. T., & Becker, J. T. (2005). Differential cortical atrophy in subgroups of mild cognitive impairment. Archives of Neurology, 62, 1393–1397. https://doi.org/10.1001/archneur.62.9.1393
Castrillo, A., Olmos, L. M. G., Rodríguez, F., & Duarte, J. (2016). Gait disorder in a cohort of patients with mild and moderate Alzheimer’s disease. American Journal of Alzheimer’s Disease & Other Dementiasr, 31, 257–262. https://doi.org/10.1177/1533317515603113
Cavanna, A. E., & Trimble, M. R. (2006). The precuneus: A review of its functional anatomy and behavioural correlates. Brain, 129, 564–583. https://doi.org/10.1093/brain/awl004
Dahnke, R., Yotter, R. A., & Gaser, C. (2013). Cortical thickness and central surface estimation. NeuroImage, 65, 336–348. https://doi.org/10.1016/j.neuroimage.2012.09.050
Desikan, R. S., Ségonne, F., Fischl, B., Quinn, B. T., Dickerson, B. C., Blacker, D., Buckner, R. L., Dale, A. M., Maguire, R. P., Hyman, B. T., Albert, M. S., & Killiany, R. J. (2006). An automated labeling system for subdividing the human cerebral cortex on MRI scans into gyral based regions of interest. NeuroImage, 31, 968–980. https://doi.org/10.1016/j.neuroimage.2006.01.021
Doi, T., Blumen, H. M., Verghese, J., Shimada, H., Makizako, H., Tsutsumimoto, K., Hotta, R., Nakakubo, S., & Suzuki, T. (2017). Gray matter volume and dual-task gait performance in mild cognitive impairment. Brain Imaging and Behavior, 11, 887–898. https://doi.org/10.1007/s11682-016-9562-1
European GAITRite® Network Group, Kressig, R. W., & Beauchet, O. (2006). Guidelines for clinical applications of spatio-temporal gait analysis in older adults. Aging Clinical and Experimental Research, 18, 174–176. https://doi.org/10.1007/BF03327437
Hausdorff, J. M. (2005). Gait variability: Methods, modeling and meaning. Journal of Neuroengineering and Rehabilitation, 2, 19. https://doi.org/10.1186/1743-0003-2-19
Hirjak, D., Wolf, R. C., Pfeifer, B., Kubera, K. M., Thomann, A. K., Seidl, U., Maier-Hein, K. H., Schröder, J., & Thomann, P. A. (2017). Cortical signature of clock drawing performance in Alzheimer’s disease and mild cognitive impairment. Journal of Psychiatric Research, 90, 133–142. https://doi.org/10.1016/j.jpsychires.2017.02.019
Karas, G. B., Scheltens, P., Rombouts, S. A. R. B., Visser, P. J., van Schijndel, R. A., Fox, N. C., & Barkhof, F. (2004). Global and local gray matter loss in mild cognitive impairment and Alzheimer’s disease. NeuroImage, 23, 708–716. https://doi.org/10.1016/j.neuroimage.2004.07.006
Labriffe, M., Annweiler, C., Amirova, L. E., Gauquelin-Koch, G., Ter Minassian, A., Leiber, L.-M., Beauchet, O., Custaud, M.-A., & Dinomais, M. (2017). Brain activity during mental imagery of gait versus gait-like plantar stimulation: A novel combined functional MRI paradigm to better understand cerebral gait control. Frontiers in Human Neuroscience, 11, 106. https://doi.org/10.3389/fnhum.2017.00106
Liu, T., Sachdev, P. S., Lipnicki, D. M., Jiang, J., Cui, Y., Kochan, N. A., Reppermund, S., Trollor, J. N., Brodaty, H., & Wen, W. (2013). Longitudinal changes in sulcal morphology associated with late-life aging and MCI. NeuroImage, 74, 337–342. https://doi.org/10.1016/j.neuroimage.2013.02.047
Montero-Odasso, M., Casas, A., Hansen, K. T., Bilski, P., Gutmanis, I., Wells, J. L., & Borrie, M. J. (2009). Quantitative gait analysis under dual-task in older people with mild cognitive impairment: A reliability study. J. Neuroengineering Rehabil., 6, 35. https://doi.org/10.1186/1743-0003-6-35
Montero-Odasso, M., Muir, S. W., & Speechley, M. (2012a). Dual-task complexity affects gait in people with mild cognitive impairment: The interplay between gait variability, dual tasking, and risk of falls. Archives of Physical Medicine and Rehabilitation, 93, 293–299. https://doi.org/10.1016/j.apmr.2011.08.026
Montero-Odasso, M., Verghese, J., Beauchet, O., & Hausdorff, J. M. (2012b). Gait and cognition: A complementary approach to understanding brain function and the risk of falling. Journal of the American Geriatrics Society, 60, 2127–2136. https://doi.org/10.1111/j.1532-5415.2012.04209.x
Pennanen, C., Testa, C., Laakso, M., Hallikainen, M., Helkala, E., Hanninen, T., Kivipelto, M., Kononen, M., Nissinen, A., Tervo, S., Vanhanen, M., Vanninen, R., Frisoni, G., & Soininen, H. (2005). A voxel based morphometry study on mild cognitive impairment. Journal of Neurology, Neurosurgery and Psychiatry, 76, 11–14. https://doi.org/10.1136/jnnp.2004.035600
Perera, S., Mody, S. H., Woodman, R. C., & Studenski, S. A. (2006). Meaningful change and responsiveness in common physical performance measures in older adults: Meaningful change and performance. Journal of the American Geriatrics Society, 54, 743–749. https://doi.org/10.1111/j.1532-5415.2006.00701.x
Seiger, R., Ganger, S., Kranz, G. S., Hahn, A., & Lanzenberger, R. (2018). Cortical thickness estimations of freesurfer and the CAT12 toolbox in patients with Alzheimer’s disease and healthy controls. Journal of Neuroimaging: Official Journal of the American Society of Neuroimaging, 28, 515–523. https://doi.org/10.1111/jon.12521
Tomadesso, C., Perrotin, A., Mutlu, J., Mézenge, F., Landeau, B., Egret, S., de la Sayette, V., Jonin, P.-Y., Eustache, F., Desgranges, B., & Chételat, G. (2015). Brain structural, functional, and cognitive correlates of recent versus remote autobiographical memories in amnestic mild cognitive impairment. NeuroImage: Clinical, 8, 473–482. https://doi.org/10.1016/j.nicl.2015.05.010
Verghese, J., Robbins, M., Holtzer, R., Zimmerman, M., Wang, C., Xue, X., & Lipton, R. B. (2008a). Gait dysfunction in mild cognitive impairment syndromes: GAIT AND MCI. Journal of the American Geriatrics Society, 56, 1244–1251. https://doi.org/10.1111/j.1532-5415.2008.01758.x
Verghese, J., Robbins, M., Holtzer, R., Zimmerman, M., Wang, C., Xue, X., & Lipton, R. B. (2008b). Gait dysfunction in mild cognitive impairment syndromes. Journal of the American Geriatrics Society, 56, 1244–1251. https://doi.org/10.1111/j.1532-5415.2008.01758.x
Verghese, J., Wang, C., Lipton, R. B., & Holtzer, R. (2013). Motoric cognitive risk syndrome and the risk of dementia. Journals of Gerontology Series A, Biological Sciences and Medical Sciences, 68, 412–418. https://doi.org/10.1093/gerona/gls191
Viljanen, A., Kaprio, J., Pyykkö, I., Sorri, M., Koskenvuo, M., & Rantanen, T. (2009). Hearing acuity as a predictor of walking difficulties in older women. Journal of the American Geriatrics Society, 57, 2282–2286. https://doi.org/10.1111/j.1532-5415.2009.02553.x
Zimmerman, M. E., Lipton, R. B., Pan, J. W., Hetherington, H. P., & Verghese, J. (2009). MRI- and MRS-derived hippocampal correlates of quantitative locomotor function in older adults. Brain Research, 1291, 73–81. https://doi.org/10.1016/j.brainres.2009.07.043
Funding
The research was supported by the University hospital of Angers, France (eudract number 2014 – A01593 – 44). The funder had no role in study design, data collection and analysis, decision to publish, or preparation of the manuscript.
The study was conducted in accordance with the ethical standards set forth in the Helsinki Declaration (1983). The entire study protocol was approved by the Angers Ethical Review Committee (Comité de protection des personnes, CPP ouest II, Angers, France, n° A.C D 2014-A01593-44, n° CPP: 2014/32). Written informed consent was obtained at enrolment.
Author information
Authors and Affiliations
Contributions
Conceptualization; Data curation; MD and CA.
Methodology and writing: PA and MD.
Supervision: PP, CA and MD.
Corresponding author
Ethics declarations
Conflict of interest
C. Annweiler serves as an editor for Maturitas. All authors declare they do not have any other financial and personal conflicts of interest with this manuscript.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Ali, P., Labriffe, M., Paisant, P. et al. Associations between gait speed and brain structure in amnestic mild cognitive impairment: a quantitative neuroimaging study. Brain Imaging and Behavior 16, 228–238 (2022). https://doi.org/10.1007/s11682-021-00496-7
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11682-021-00496-7