Abstract
Purpose
Schistosomiasis is one of the leading chronic parasitic diseases in Ethiopia. We aimed to summarize the prevalence of S. mansoni in human and Biomphalaria snails as well as risk factors in Ethiopia.
Methods
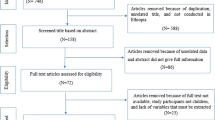
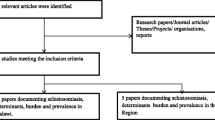
Literature search was carried out from Scopus, Google Scholar, Science Direct and PubMed which reported Schistosoma mansoni infection in human and Biomphalaria snails in Ethiopia. The overall prevalence was estimated by a random-effect model and heterogeneities among studies were assessed by I2 test.
Results
A total of 178,251 participants and 1,097 snails were tested for the presence of S. mansoni in the eligible studies. The pooled prevalence of S. mansoni was 32.5% (95% CI 28.0–37.0) and 15.9% (95% CI − 5.6–37.5) in human and Biomphalaria snails in Ethiopia, respectively. The highest pooled prevalence was 43.2% (95% CI 27.3–59.1) in South Nations and National Peoples region while the lowest pooled prevalence was 25% (95% CI 19.3–30.7) observed in the Afar region. Interestingly, the pooled prevalence of S. mansoni declined from 40.7% (95% CI 33–48.4) to 22.4% (95% CI 18.5–26.3) after the launching of mass drug administration (MDA). The analysis of risk factors showed that swimming habit (OR, 2.78; 95% CI 2.35–3.21) and participation in irrigation (OR, 2.69; 95% CI 1.45–3.73) were independent predictors for S. mansoni infection.
Conclusion
This study revealed that about one-third of human and nearly 16% of Biomphalaria snails were infected with S. mansoni in Ethiopia. This review indicated that the prevalence of S. mansoni declined after the implementation of MDA. This study highlights the importance of further integrated approaches for better control of schistosomiasis in Ethiopia.






Similar content being viewed by others
Data availability
All information is included with the manuscript.
Code availability
Not applicable.
Abbreviations
- CI:
-
Confidence interval
- DALYs:
-
Disability-adjusted life year
- EOTC:
-
Ethiopian Orthodox Tewahido Church
- I 2 :
-
Inverse variance index
- MDA:
-
Mass drug administration
- NOS:
-
Newcastle–Ottawa quality assessment scale
- NTD:
-
Neglected tropical disease
- OR:
-
Odd ratio
- PCR:
-
Polymerase chain reaction
- POC:
-
Point of care
- PRISMA:
-
Preferred reporting items for systematic reviews and meta-analysis
- WASH:
-
Water, sanitation and hygiene
References
Jejaw A, Zemene E, Alemu Y, Mengistie Z (2015) High prevalence of Schistosoma mansoni and other intestinal parasites among elementary school children in Southwest Ethiopia: a cross-sectional study. BMC Public Health 15(1):1–7. https://doi.org/10.1186/s12889-015-1952-6
Melman SD, Steinauer ML, Cunningham C, Kubatko LS, Mwangi IN et al (2009) Reduced susceptibility to praziquantel among naturally occurring Kenyan isolates of Schistosoma mansoni. PLoS NTDs 3(8):504. https://doi.org/10.1371/journal.pntd.0000504
Barry MA, Simon G, Mistry N, Hotez PJ (2013) Global trends in neglected tropical disease control and elimination: impact on child health. Arch Dis Child 98(8):635. https://doi.org/10.1136/archdischild-2012-302338
Adenowo AF, Oyinloye BE, Ogunyinka BI, Kappo AP (2015) Impact of human schistosomiasis in sub-Saharan Africa. Braz J Infect Dis 19(2):196–205. https://doi.org/10.1016/j.bjid.2014.11.004
Colley DG, Bustinduy AL, Secor WE, King CH (2014) Human schistosomiasis. Lancet 383(9936):2253–2264. https://doi.org/10.1016/s0140-6736(13)61949-2 (Epub 2014/04/01)
Gryseels B, Polman K, Clerinx J, Kestens L (2006) Human schistosomiasis. Lancet 368(9541):1106–1118. https://doi.org/10.1016/S0140-6736(06)69440-3
Blanton RE (2019) Population structure and dynamics of helminthic infection: schistosomiasis. Microbiol Spectr. https://doi.org/10.1128/microbiolspec.AME-0009-2019
Pinto-Almeida A, Mendes T, de Oliveira RN, Corrêa SDAP, Allegretti SM et al (2016) Morphological characteristics of Schistosoma mansoni PZQ-resistant and -susceptible strains are different in presence of praziquantel. Front Microbiol. https://doi.org/10.3389/fmicb.2016.00594
Gordon CA, Kurscheid J, Williams GM, Clements ACA, Li Y et al (2019) Asian schistosomiasis: current status and prospects for control leading to elimination. Trop Med Infect Dis 4:40. https://doi.org/10.3390/tropicalmed4010040
Negussu N, Mengistu B, Kebede B, Deribe K, Ejigu E et al (2017) Ethiopia schistosomiasis and soil-transmitted helminthes control programme: progress and prospects. Ethiop Med J 55(Suppl 1):75–80
Jember TH (2014) Challenges of schistosomiasis prevention and control in Ethiopia: literature review and current status. J Parasitol Vector Biol 6(6):80–86. https://doi.org/10.5897/JPVB2014.0155
Kloos H, Tsong Lo C, Birrie H, Ayele T, Tedla S et al (1988) Schistosomiasis in Ethiopia. Soc Sci Med 26(8):803–827. https://doi.org/10.1016/0277-9536(88)90174-8
Worku L, Damte D, Endris M, Tesfa H, Aemero M (2014) Schistosoma mansoni infection and associated determinant factors among school children in Sanja town Northwest Ethiopia. J Parasitol Res. https://doi.org/10.1155/2014/792536
Alebie G, Erko B, Aemero M, Petros B (2014) Epidemiological study on Schistosoma mansoni infection in Sanja area, Amhara region, Ethiopia. Parasit Vectors 7:15. https://doi.org/10.1186/1756-3305-7-15
Erko B, Fekede B, Demeke K (2006) The ecology of Biomphalaria sudanica in Lake Ziway, Ethiopia. Afr J Ecol 44(3):347–352. https://doi.org/10.1111/j.1365-2028.2006.00615.x
Aboelhadid SM, Thabet M, El-Basel D, Taha R (2016) Digenetic larvae in Schistosome snails from El Fayoum, Egypt with detection of Schistosoma mansoni in the snail by PCR. J Parasit Dis 40(3):730–734. https://doi.org/10.1007/s12639-014-0567-7
Lewis-Mikhael A-M, Bueno-Cavanillas A, Ofir Guiron T, Olmedo-Requena R, Delgado-Rodríguez M et al (2016) Occupational exposure to pesticides and prostate cancer: a systematic review and meta-analysis. Occup Environ Med 73(2):134. https://doi.org/10.1136/oemed-2014-102692
Higgins JPT, Thompson SG, Deeks JJ, Altman DG (2003) Measuring inconsistency in meta-analyses. BMJ 327(7414):557–560. https://doi.org/10.1136/bmj.327.7414.557
Melsen WG, Bootsma MCJ, Rovers MM, Bonten MJM (2014) The effects of clinical and statistical heterogeneity on the predictive values of results from meta-analyses. Clinl Microbiol Infect 20(2):123–129. https://doi.org/10.1111/1469-0691.12494
Erko B, Tedla S (1993) The incidence of schstosomiasis in Bahir-Dar, Ethiopia. Ethiop J Health Dev 7(1):17–20
Hailu T, Abera B, Mulu W, Alemu M, Yizengaw E et al (2018) Efficacy of single dose albendazole and praziquantel drugs among helminthinfected school children at Rural Bahir Dar, northwest Ethiopia. Trop Doct. https://doi.org/10.1177/0049475518786835
Dejenie T, Asmelash T (2010) Efficacy of praziquantel in treating Schistosoma Mansoni infected school children in Tumuga and Waja. N Ethiop MEJS 2(2):3–11. https://doi.org/10.4314/mejs.v2i2.57669
Alemu A, Atnafu A, Addis Z, Shiferaw Y, Teklu T et al (2011) Soil-transmitted helminths and Schistosoma mansoni infections among school children in zarima town, northwest Ethiopia. BMC Infect Dis 11:189. https://doi.org/10.1186/1471-2334-11-189
Abera B, Alem G, Yimer M, Herrador Z (2013) Epidemiology of soil-transmitted helminths, Schistosoma mansoni, and haematocrit values among schoolchildren in Ethiopia. J Infect Dev Ctries 7(3):253–260. https://doi.org/10.3855/jidc.2539
Essa T, Birhane Y, Endris M, Moges A, Moges F (2013) Current status of Schistosoma mansoni infections and associated risk factors among students in Gorgora Town. Northwest Ethiop ISRN Infect Dis 2013:7. https://doi.org/10.5402/2013/636103
Taddese K, Zein ZA (1988) Comparison between the efficacy of oxamniquine and praziquantel in the treatment of Schistosoma mansoni infections on a sugar estate in Ethiopia. Ann Trop Med Parasitol 82(2):175–180. https://doi.org/10.1080/00034983.1988.11812225
Workineh L, Yimer M, Gelaye W, Muleta D (2019) The magnitude of Schistosoma mansoni and its associated risk factors among Sebatamit primary school children rural Bahir Dar Northwest Ethiopia: a cross-sectional study. BMC Res Notes 12(1):447. https://doi.org/10.1186/s13104-019-4498-3
Desta H, Bugssa G, Demtsu B (2014) The Current status of schistosoma mansoni infection among school children around hizaty wedicheber microdam in Merebmieti, Ethiopia. J Bacteriol Parasitol. https://doi.org/10.4172/2155-9597.1000204
Worku L, Damte D, Endris M, Tesfa H, Aemero M (2014) Schistosoma mansoni Infection and associated determinant factors among school children in Sanja Town, Northwest Ethiopia. J Parasitol Res. https://doi.org/10.1155/2014/792536
Workineh L, Kiros T, Damtie S, Andualem T, Dessie B (2020) Prevalence of soil-transmitted helminth and Schistosoma mansoni infection and their associated factors among hiruy abaregawi primary school children, rural Debre Tabor, North West Ethiopia: a cross-sectional study. J Parasitol Res. https://doi.org/10.1155/2020/2521750
Andargie AA, Abera AS (2018) Determinants of Schistosoma mansoni in Sanja health center, north West Ethiopiah. BMC Public Health 18:620. https://doi.org/10.1186/s12889-018-5552-0
Feleke DG, Arega S, Tekleweini M, Kindie K, Gedefie A (2017) Schistosoma mansoni and other helminthes infections at Haike primary school children, North-East, Ethiopia: a cross-sectional study. BMC Res Notes 10:609. https://doi.org/10.1186/s13104-017-2942-9
Alemu A, Tegegne Y, Damte D, Melku M (2016) Schistosoma mansoni and soil-transmitted helminths among preschool-aged children in Chuahit, Dembia district, Northwest Ethiopia: prevalence, intensity of infection and associated risk factors. BMC Public Health 16:422. https://doi.org/10.1186/s12889-016-2864-9
Sitotaw B, Mekuriaw H, Damtie D (2019) Prevalence of intestinal parasitic infections and associated risk factors among Jawi primary school children, Jawi town, northwest Ethiopia. BMC Infect Dis 19:341. https://doi.org/10.1186/s12879-019-3971-x
Birre H, Ayele T, Tedla S, Abebe F (1993) Transmission of S. mansoni in three ecological settings in Ethiopia, an epidemiological aspects. Ethiop J Health Dev 7(2):63–69
Leta GT, French M, Dorny P, Vercruysse J, Levecke B (2018) Comparison of individual and pooled diagnostic examination strategies during the national mapping of soil-transmitted helminths and Schistosoma mansoni in Ethiopia. PLoS NTD 12(9):e0006723. https://doi.org/10.1371/journal.pntd.0006723
Amsalu G, Mekonnen Z, Erko B (2015) A new focus of Schistosomiasis mansoni in Hayk town, northeastern Ethiopia. BMC Res Notes 8:22. https://doi.org/10.1186/s13104-014-0965-z
Gashaw F, Aemero M, Legesse M, Petros B, Teklehaimanot T et al (2015) Prevalence of intestinal helminth infection among school children in Maksegnit and Enfranz Towns, northwestern Ethiopia, with emphasis on Schistosoma mansoni infection. Parasit Vectors 8:567. https://doi.org/10.1186/s13071-015-1178-6
Getie S, Wondimeneh Y, Getnet G, Workineh M, Worku L et al (2015) Prevalence and clinical correlates of Schistosoma mansoni co-infection among malaria infected patients, Northwest Ethiopia. BMC Res Notes 8(1):480. https://doi.org/10.1186/s13104-015-1468-2
Bitew AA, Bayeh A, Walle S, Endale B, Tibebu K et al (2016) Soil-transmitted helminths and Schistosoma mansoni infections in Ethiopian orthodox church students around Lake Tana, Northwest Ethiopia. PLoS ONE 11(5):155915. https://doi.org/10.1371/journal.pone.0155915
Yencneh H, Abebe F, Ameha M, Hailu B, Teklemariam A (1996) Praziquantel in the control of Schistosoma mansoni infection in Jiga, Northwestern Ethiopia. Ethiop J Health Dev 10(2):105–110
Birrie H, Berhe N, Tedla S, Gemeda N (1993) Schistosoma haematobium infection among Ethiopiam prisoners of war (1977–1988) returning from Somalia. Ethiop Med J 31(4):259–264
Hailu T, Yimer M (2014) Prevalence of Schistosoma mansoni and geo-helminthic infections among patients examined at Workemeda Health Center, Northwest Ethiopia. J Parasitol Vector Biol 6(5):75–79. https://doi.org/10.5897/JPVB2014.0149
Merem A, Endalkachew N, Abaineh M (2017) Prevalence of intestinal helminthic infections and malnutrition among schoolchildren of the Zegie Peninsula, northwestern Ethiopia. J Infect Public Health 10(1):84–92. https://doi.org/10.1016/j.jiph.2016.02.009
Sousa-Figueiredo JC, Betson M, Atuhaire A, Arinaitwe M, Navaratnam AMD et al (2012) Performance and safety of praziquantel for treatment of intestinal schistosomiasis in infants and preschool. PLoS Neg Trop Dis 6:e1864. https://doi.org/10.1371/journal.pntd.0001864
Jemaneh L (1999) Intestinal helminths infections in schoolchildren in Gondar Town and surrounding areas,Northwest Ethiopia. Ethiop J Sci 22(2):209–220
Hailu T, Mulu W, Abera B (2020) Effects of water source, sanitation and hygiene on the prevalence of Schistosoma mansoni among school age children in Jawe District, Northwest Ethiopia. Iran J Parasitol 15(1):124–129
Jemaneh L (2001) Soil-transmitted helminth infections and Schistosoma mansoni in school children from Chilga District, Northwest Ethiopia. Ethiop J Health Sci 11(2):79–87
Nute AW, Endeshaw T, Stewart AEP, Sata E, Bayissasse B et al (2018) Prevalence of soil-transmitted helminths and Schistosoma mansoni among a population-based sample of school-age children in Amhara region, Ethiopia. Parasit Vectors 11:431. https://doi.org/10.1186/s13071-018-3008-0
Wubet K, Damtie D (2020) Prevalence of Schistosoma mansoni infection and associated risk factors among school children in Jiga Town, Northwest-Ethiopia: a cross-sectional study. J Parasitol Res. https://doi.org/10.1155/2020/6903912
Tadesse G (2005) The prevalence of intestinal helminthic infections and associated risk factors among school children in Babile town, eastern Ethiopia. Ethiop J Health Dev 19(2):140–147
Erko B, Balcha F, Kifle D (2006) The ecology of Biomphalaria sudanica in Lake Ziway, Ethiopia. Afr J Ecol 44(3):347–352. https://doi.org/10.1111/j.1365-2028.2006.00615.x
Legesse M, Erko B (2007) Field-based evaluation of a reagent strip test for diagnosis of Schistosoma mansoni by detecting circulating cathodic antigen in urine before and after chemotherapy. Trans R Soc Trop Med Hyg 101:668–673. https://doi.org/10.1016/j.trstmh.2006.11.009
Kemal M, Tadesse G, Esmael A, Abay SM, Kebede T (2019) Schistosoma mansoni infection among preschool age children attending Erer Health Center, Ethiopia and the response rate to praziquantel. BMC Res Notes 12:211. https://doi.org/10.1186/s13104-019-4246-8
Bajiro M, Tesfaye S (2017) Schistosoma mansoni infection prevalence and associated determinant factors among school children in Mana District, Jimma Zone, Oromia Region, South West Ethiopia. J Bacteriol Parasitol 8:5. https://doi.org/10.4172/2155-9597.1000329
Tulu B, Taye S, Amsalu E (2014) Prevalence and its associated risk factors of intestinal parasitic infections among Yadot primary school children of Southeastern Ethiopia: a cross-sectional study. BMC Res Notes. https://doi.org/10.1186/1756-0500-7-848
Sitotaw B, Shiferaw W (2020) Prevalence of intestinal parasitic infections and associated risk factors among the first-cycle primary schoolchildren in Sasiga District, Southwest Ethiopia . J Parasitol Res. https://doi.org/10.1155/2020/8681247
Bajiro M, Gedamu S, Hamba N, Yonas A (2018) Prevalence, intensity of infection and associated risk factors for Schistosoma mansoni and soil transmitted helminthes among two primary school children at nearby Rivers in Jimma Town, South West Ethiopia. Ann Clin Pathol 6(4):1144. https://doi.org/10.1371/journal.pone.0228007
Bronzan RN, Dorkenoo AM, Agbo YM, Halatoko W, Layibo Y et al (2018) Impact of community-based integrated mass drug administration on schistosomiasis and soil-transmitted helminth prevalence in Togo. PLoS NTD 12(8):e0006551. https://doi.org/10.1371/journal.pntd.0006551
Mohammed J, Weldegebreal F, Teklemariam Z, Mitiku H (2018) Clinico-epidemiology, malacology and community awareness of Schistosoma mansoni in Haradenaba and Dertoramis kebeles in Bedeno district, eastern Ethiopia. Sage Open Med 6:1–11. https://doi.org/10.1177/2050312118786748
Nega B, Svein GG, Fekadu A, Hailu B, Girmay M et al (1999) Praziquantel side effects and efficacy related to Schistosoma mansoni egg loads and morbidity in primary school children in north-east Ethiopia. Acta Trop 72:53–63. https://doi.org/10.1016/s0001-706x(98)00084-9
Tefera A, Belay T, Bajiro M (2020) Epidemiology of Schistosoma mansoni infection and associated risk factors among school children attending primary schools nearby rivers in Jimma town, an urban setting, Southwest Ethiopia. PLoS ONE 15(2):228007. https://doi.org/10.1371/journal.pone.0228007
Tadesse K, Yohanis N, Berhanu E (2018) Schistosoma mansoni infection in human and nonhuman primates in selected areas of Oromia Regional State, Ethiopia. J Vector Borne Dis 55(2):116–121. https://doi.org/10.4103/0972-9062.242558
Dufera M, Petros B, Erko B, Berhe N, Gundersen SG (2014) Schistosoma mansoni infection in finchaa sugar estate: public health problem assessment based on clinical records and parasitological surveys, Western Ethiopia. Sci Technol Arts Res J 3(2):155–161. https://doi.org/10.4314/star.v3i2.20
Mekonnen Z, Meka S, Zeynudin A, Suleman S (2014) Schistosoma mansoni infection and undernutrition among school age children in Fincha’a sugar estate, rural part of West Ethiopia. BMC Res Notes 7:763. https://doi.org/10.1186/1756-0500-7-763
Teklemariam D, Legesse M, Degarege A, Liang S, Erko B (2018) Schistosoma mansoni and other intestinal parasitic infections in schoolchildren and vervet monkeys in Lake Ziway area, Ethiopia. BMC Res Notes 11:146. https://doi.org/10.1186/s13104-018-3248-2
Gebrehiwot Y, Degarege A, Erko B (2014) Prevalence of intestinal parasitic infections among children under five years of age with emphasis on Schistosoma mansoni in Wonji Shoa Sugar Estate, Ethiopia. PLoS ONE 9(10):109793. https://doi.org/10.1371/journal.pone.0109793
Caldeira RL, Jannotti-Passos LK, Dos Santos CO (2017) Use of molecular methods for the rapid mass detection of Schistosoma mansoni (Platyhelminthes: Trematoda) in Biomphalaria spp. (Gastropoda: Planorbidae). J Trop Med. https://doi.org/10.1155/2017/8628971
Ibrahim T, Zemene E, Asres Y, Seyoum D, Tiruneh A et al (2018) Epidemiology of soil-transmitted helminths and Schistosoma mansoni: a base line survey among schoolchildren, Ejaji Ethiopia. J Infect Dev Ctries 12(12):1134–1141. https://doi.org/10.3855/jidc.9665
Kure A, Mekonnen Z, Dana D, Bajiro M, Ayana M et al (2015) Comparison of individual and pooled stool samples for the assessment of intensity of Schistosoma mansoni and soil-transmitted helminth infections using the Kato-Katz technique. Parasit Vectors 8:489. https://doi.org/10.1186/s13071-015-1101-1
Ansha MG, Kuti KA, Girma E (2020) Prevalence of intestinal schistosomiasis and associated factors among school children in Wondo District, Ethiopia. J Trop Med. https://doi.org/10.1155/2020/9813743
Wodimagegnehu T, Birrie H, Yeneneh H (1997) Schistosomiasis and intestinal helminthc infections in Delo Awraja, Bale adminisstrative region south Ethiopia. Ethiop J Health Dev 11(3):183–188
Haile S, Golassa L, Mekonnen Z (2012) Prevalence of Schistosoma mansoni and effectiveness of Praziquantel in school children in Finchaa valley, Ethiopia. J Parasitol Vector Biol 4(3):25–30. https://doi.org/10.5897/JPVB12.013
Tadege B, Shimelis T (2017) Infections with Schistosoma mansoni and geohelminths among school children dwelling along the shore of the Lake Hawassa southern Ethiopia. PLoS ONE 12(7):e081547. https://doi.org/10.1371/journal.pone.0181547
Alemayehu B, Tomas Z (2015) Schistosoma mansoni infection prevalence and associated risk factors among schoolchildren in Demba Girara, damot Woide District of Wolaita Zone, Southern Ethiopia. Asian Pac J Trop Biomed 8(6):457–463. https://doi.org/10.1016/j.apjtm.2015.05.009
Menjetta T, Debalke S, Dana D (2019) Schistosoma mansoni infection and risk factors among the fishermen of Lake Hawassa, southern Ethiopia. J Biosoc Sci 51(6):817–826. https://doi.org/10.1017/S0021932019000075
Alemu M, Hailu A, Bugssa G (2014) Prevalence of intestinal schistosomiasis and soil transmitted helminthiasis among primary school children in Umolante district, South Ethiopia. Clin Med Res 3(6):174–180. https://doi.org/10.11648/j.cmr.20140306.14
Roma B, Worku S (1997) Magnitude of Schistosoma mansoni and intestinal helminthic infections among school children in Wondo-Genet Zuria, Southern Ethiopia. Ethiop J Health Dev 11(2):125–129
Tiruneh A, Kahase D, Zemene E, Tekalign E, Solomon A et al (2020) Identification of transmission foci of Schistosoma mansoni: narrowing the intervention target from district to transmission focus in Ethiopia. BMC Public Health 20:769. https://doi.org/10.1186/s12889-020-08904-1
Alemayehu B, Tomass Z, Wadilo F, Leja D, Liang S et al (2017) Epidemiology of intestinal helminthiasis among school children with emphasis on Schistosoma mansoni infection in Wolaita zone, Southern Ethiopia. BMC Public Health 17:587. https://doi.org/10.1186/s12889-017-4499-x
Mulu A, Legesse M, Erko B, Belyhun Y, Nugussie D et al (2013) Epidemiological and clinical correlates of malaria-helminth co-infections in southern Ethiopia. Malar J 12:227. https://doi.org/10.1186/1475-2875-12-227
Berhanu E, Degarege A, Tadesse K, Mathiwos A (2012) Efficacy and side effects of praziquantel in the treatment of Schistosoma mansoni in schoolchildren in Shesha Kekele Elementary School, Wondo Genet, Southern Ethiopia. Asian Pac J Trop Biomed 2(3):235–239. https://doi.org/10.1016/S2221-1691(12)60049-5
Assefa A, Dejenie T, Tomass Z (2013) Infection prevalence of Schistosoma mansoni and associated risk factors among schoolchildren in suburbs of Mekelle city, Tigray. Northern Ethiopia MEJS 5(1):174–188. https://doi.org/10.4314/mejs.v5i1.85339
Teshale T, Belay S, Tadesse D, Awala A, Teklay G (2018) Prevalence of intestinal helminths and associated factors among school children of Medebay Zana wereda; North Western Tigray, Ethiopia 2017. BMC Res Notes 11:444. https://doi.org/10.1186/s13104-018-3556-6
Mekonnen Z, Haileselassie H, Medhin G, Erko B, Berhe N (2012) Schistosoma mansoni focus in Mekele city, Northestern Ethiopia. Ethiop Med J 50(4):331–336
Abebe N, Erko B, Medhin G, Berhe N (2014) Clinico-epidemiological study of Schistosomiasis mansoni in Waja-Timuga, District of Alamata, northern Ethiopia. Parasit Vectors 7:158. https://doi.org/10.1186/1756-3305-7-158
Gebreyohanns A, Legese MH, Wolde M, Leta G, Tasew G (2018) Prevalence of intestinal parasites versus knowledge, attitude and practices (KAPs) with special emphasis to Schistosoma mansoni among individuals who have river water contact in Addiremets town, Western Tigray, Ethiopia. PLoS ONE 13(9):e0204259. https://doi.org/10.1371/journal.pone.0204259
Mahmud MA, Spigt M, Mulugeta Bezabih A, López Pavon I, Dinant G-J et al (2013) Risk factors for intestinal parasitosis, anaemia, and malnutrition among school children in Ethiopia. Pathog Glob Health 107(2):58–65. https://doi.org/10.1179/2047773213y.0000000074
Kariuki HC, Clennon JA, Brady MS, Kitron U, Sturrock RF et al (2004) Distribution patterns and cercarial shedding of Bulinus nasutus and other snails in the Msambweni area, Coast Province, Kenya. Am J Trop Med Hyg 70(4):449–456. https://doi.org/10.4269/ajtmh.2004.70.449
Asaye Mekonnen A, Legesse M, Belay M, Tadesse K, Torben W et al (2013) Efficacy of praziquantel against Schistosoma haematobium in Dulshatalo village, western Ethiopia. BMC Res Notes 6:392
Grimes JET, Tadesse G, Mekete K, Wuletaw Y, Gebretsadik A et al (2016) School water, sanitation, and hygiene, soil-transmitted helminths, and schistosomes: national mapping in Ethiopia. PLoS NTD 10(3):0004515. https://doi.org/10.1371/journal.pntd.0004515
Degarege A, Legesse M, Medhin G, Teklehaymanot T, Erko B (2014) Day-to-day fluctuation of point-of-care circulating cathodic antigen test scores and faecal egg counts in children infected with Schistosoma mansoni in Ethiopia. BMC Infect Dis 14:210. https://doi.org/10.1186/1471-2334-14-210
Berhe N, Myrvang B, Gundersen SG (2007) Intensity of Schistosoma Mansoni, hepatitis B, age, and sex predict levels of hepatic periportal thickening/fibrosis (PPT/F): a large-scale community-based study in Ethiopia. Am J Trop Med Hyg 77(6):1079–1086. https://doi.org/10.4269/AJTMH.2007.77.1079
Reta B, Erko B (2013) Efficacy and side effects of praziquantel in the treatment for Schistosoma mansoni infection in school children in Senbete Town, northeastern Ethiopia. Trop Med Int Health 18(11):1338–1343. https://doi.org/10.1111/tmi.12187
Kalinda C, Mutengo M, Chimbari M (2019) A meta-analysis of changes in schistosomiasis prevalence in Zambia: implications on the 2020 elimination target. Parasitol Res 119(1):1–10. https://doi.org/10.1007/s00436-019-06534-0
Casavechia MTG, Melo GdANd, Fernandes ACBdS, Castro KRRd, Pedroso RB et al (2018) Systematic review and meta-analysis on Schistosoma mansoni infection prevalence, and associated risk factors in Brazil. Parasitology 145(8):1000–1014. https://doi.org/10.1017/S0031182017002268
Asundi A, Beliavsky A, Liu XJ, Akaberi A, Schwarzer G et al (2019) Prevalence of strongyloidiasis and schistosomiasis among migrants: a systematic review and meta-analysis. Lancet Glob Health 7(2):e236–e248. https://doi.org/10.1016/s2214-109x(18)30490-x
Katz N, Chaves A, Pellegrino J (1972) A simple device for quantitative stool thick-smear technique in Schistosomiasis mansoni. Rev Inst Med Trop Sao Paulo 14(6):397–400
Lamberton PHL, Kabatereine NB, Oguttu DW, Fenwick A, Webster JP (2014) Sensitivity and specificity of multiple Kato-Katz thick smears and a circulating cathodic antigen test for Schistosoma mansoni diagnosis pre- and post-repeated-praziquantel treatment. PLoS NTD 8(9):3139. https://doi.org/10.1371/journal.pntd.0003139
Mazigo HD, Kepha S, Kinung’hi SM (2018) Sensitivity and specificity of point-of-care circulating Cathodic antigen test before and after praziquantel treatment in diagnosing Schistosoma mansoni infection in adult population co-infected with human immunodeficiency virus-1, North-Western Tanzania. Arch Public Health 76:29. https://doi.org/10.1186/s13690-018-0274-4
Kabatereine NB, Brooker S, Tukahebwa EM, Kazibwe F, Onapa AW (2004) Epidemiology and geography of Schistosoma mansoni in Uganda: implications for planning control. Trop Med Int Health 9(3):372–380. https://doi.org/10.1046/j.1365-3156.2003.01176.x
Taman A, El-Tantawy N, Besheer T, Taman S, Helal R (2014) Schistosoma mansoni infection in a fishermen community, the Lake Manzala region-Egypt. Asian Pac J Trop Dis 4(6):463–468. https://doi.org/10.1016/S2222-1808(14)60607-1
Grimes JET, Croll D, Harrison WE, Utzinger J, Freeman MC et al (2015) The roles of water, sanitation and hygiene in reducing schistosomiasis: a review. Parasit Vectors 8:156. https://doi.org/10.1186/s13071-015-0766-9
Campbell SJ, Savage GB, Gray DJ, Atkinson J-AM, Soares Magalhães RJ et al (2014) Water, Sanitation, and Hygiene (WASH): a critical component for sustainable soil-transmitted helminth and schistosomiasis control. PLoS NTD 8(4):e2651. https://doi.org/10.1371/journal.pntd.0002651
Bah YM, Paye J, Bah MS, Conteh A, Saffa S et al (2019) Schistosomiasis in school age children in sierra leone after 6 years of mass drug administration with praziquantel. Front Public Health. https://doi.org/10.3389/fpubh.2019.00001
Wang W, Liang Y (2014) Mass drug administration (MDA) for schistosomiasis. J Infect Dis 211(5):848–849. https://doi.org/10.1093/infdis/jiu506
Lemos QT, Andrade ZA (2001) Sequential histological changes in Biomphalaria glabrata during the course of Schistosoma mansoni infection. Mem Inst Oswaldo Cruz 96:719–721. https://doi.org/10.1590/s0074-02762001000500025
Farghaly A, Saleh AA, Mahdy S, Abd El-Khalik D, Abd El-Aal NF et al (2016) Molecular approach for detecting early prepatent Schistosoma mansoni infection in Biomphalaria alexandrina snail host. J Parasit Dis 40(3):805–812. https://doi.org/10.1007/s12639-014-0583-7 (Epub 2014/09/25)
Kabuyaya M, Chimbari MJ, Manyangadze T, Mukaratirwa S (2017) Schistosomiasis risk factors based on the infection status among school-going children in the Ndumo area, uMkhanyakude district, South Africa. S Afr J Infect Dis 32(2):67–72. https://doi.org/10.1080/23120053.2016.1266139
Matthys B, Tschannen AB, Tian-Bi NT, Comoé H, Diabaté S et al (2007) Risk factors for Schistosoma mansoni and hookworm in urban farming communities in western Côte d’Ivoire. Trop Med Int Health 12(6):709–723. https://doi.org/10.1111/j.1365-3156.2007.01841.x
Masaku J, Njomo DW, Njoka A, Okoyo C, Mutungi FM et al (2020) Soil-transmitted helminths and schistosomiasis among pre-school age children in a rural setting of Busia County, Western Kenya: a cross-sectional study of prevalence, and associated exposures. BMC Public Health 20(1):356. https://doi.org/10.1186/s12889-020-08485-z
Angora EK, Boissier J, Menan H, Rey O, Tuo K et al (2019) Prevalence and risk factors for schistosomiasis among schoolchildren in two settings of Côte d’Ivoire. Trop Med Infect Dis 4(3):110. https://doi.org/10.3390/tropicalmed4030110
Madinga J, Linsuke S, Mpabanzi L, Meurs L, Kanobana K et al (2015) Schistosomiasis in the democratic Republic of Congo: a literature review. Parasit Vectors 8(1):601. https://doi.org/10.1186/s13071-015-1206-6
Masaku J, Madigu N, Okoyo C, Njenga SM (2015) Current status of Schistosoma mansoni and the factors associated with infection two years following mass drug administration programme among primary school children in Mwea irrigation scheme: a cross-sectional study. BMC Public Health 15:739. https://doi.org/10.1186/s12889-015-1991-z
Acknowledgements
We are gratful to all authors whose articles are included in this systematic review and meta-analysis.
Funding
Not applicable.
Author information
Authors and Affiliations
Contributions
TH was involved in the design and conducted the review, data analysis, interpretation of the findings and drafting of the manuscript. EN and AM were involved in drafting the manuscript, reviewing and editing the manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors declared that there is no conflict of interest.
Ethical approval
Not applicable.
Consent to participate
Not applicable.
Consent for publication
Not applicable.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Hailegebriel, T., Nibret, E. & Munshea, A. Prevalence of Schistosoma mansoni and Associated Risk Factors in Human and Biomphalaria Snails in Ethiopia: A Systematic Review and Meta-analysis. Acta Parasit. 67, 31–48 (2022). https://doi.org/10.1007/s11686-021-00449-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11686-021-00449-6