Abstract
Purpose
Delineate retrospectively and prospectively the incidence and characteristics of transient ST-segment elevation during transseptal puncture.
Methods
The study retrospectively evaluated 307 patients from January 1, 2015, to December 31, 2017, and prospectively evaluated 231 patients from January 1, 2018, to July 31, 2019.
Results
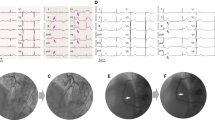
The presence of ST-segment elevation was significantly higher in the prospective sample than in the retrospective sample (5.2% vs. 1.3%, p < 0.05). Between the two groups, there was no significant difference in age, sex, comorbidities, left atrial volume index, and the etiology of atrial fibrillation among patients with ST-segment alteration. In all patients, the ST-segment elevation was observed in the inferior wall derivations, except for one patient with ST elevation in lead I, AVL, V1-V4 during the septal puncture, associated with sinus bradycardia and reversed hypotension with intravenous fluids. Comparative analysis of the systolic and diastolic arterial pressure and the minimum heart rate during the phenomenon demonstrated more severity in the retrospectively evaluated population than in the prospective population. There was a significant association between the occurrence of ST-segment elevation > 2 mm and the presence of symptoms. In these patients, coronary angiography showed no alterations. Atropine was administered to one patient who presented with junctional bradycardia after the puncture. This medication reversed the situation.
Conclusion
ST-segment elevation is a short-term phenomenon that can occur during transseptal catheterization without clinically evident symptoms. The catheter ablation procedure can be safely concluded despite the occurrence of the phenomenon.



Similar content being viewed by others
References
Haegeli LM, Wolber T, Ercin E, Altwegg L, Krasniqi N, Novak PG, et al. Double transseptal puncture for catheter ablation of atrial fibrillation: safety of the technique and its use in the outpatient setting. Cardiol Res Pract. 2010;1. https://doi.org/10.4061/2010/295297.
Arita T, Kubota S, Okamoto K, Kuma F, Nakasuga K, Koga H, et al. Bezold-Jarisch-like reflex during Brockenbrough’s procedure for radiofrequency catheter ablation of focal left atrial fibrillation: report of two cases. J Interv Card Electrophysiol. 2003;8:195–202. https://doi.org/10.1023/A:1023917221763.
Cheng YL, Dong JZ, Liu XP, Long DY, Fang DP, Yu RH, et al. Transient ST-segment elevation after transseptal puncture for atrial fibrillation ablation in two cases. Chin Med J (Engl). 2012;125:941–4. https://doi.org/10.3760/cma.j.issn.0366-6999.2012.05.037.
Salghetti F, Sieira J, Chierchia GB, Curnis A, de Asmundis C. Recognizing and reacting to complications of trans-septal puncture. Expert Rev Cardiovasc Ther. 2017. https://doi.org/10.1080/14779072.2017.1408411.
Calkins H, Kuck KH, Cappato R, Brugada J, Camm AJ, Chen SA, et al. HRS/EHRA/ECAS expert consensus statement on catheter and surgical ablation of atrial fibrillation: recommendations for patient selection, procedural techniques, patient management and follow-up, definitions, endpoints, and research trial design. Europace. 2012;14(2012):528–606. https://doi.org/10.1093/europace/eus027.
Risius T, Lewalter T, Lüderitz B, Schwab JO, Spitzer S, Schmitt C, et al. Transient ST-segment-elevation during pulmonary vein ablation using circumferential coiled microelectrodes in a prospective multi-centre study. Europace. 2006;8:178–81. https://doi.org/10.1093/europace/euj013.
Schwab JO, Burkhardt D, Yang A, Schrickel J, Lüderitz B, Lewalter T. ECG signs mimicking acute inferior wall myocardial infarction are associated with elevated myocardial enzymes during isolation of pulmonary vein for focal atrial fibrillation. Europace. 2004;6:111–5. https://doi.org/10.1016/j.eupc.2003.12.002.
Simon RDB, Gill JS. Coronary ischemia induced by radiofrequency ablation in the left atrium. J Cardiovasc Electrophysiol. 2003;14:186–90. https://doi.org/10.1046/j.1540-8167.2003.02474.x.
Tada H, Naito S, Oshima S, Taniguchi K. Vasospastic angina shortly after left atrial catheter ablation for atrial fibrillation. Hear Rhythm. 2005;2:867–70. https://doi.org/10.1016/j.hrthm.2005.05.009.
Tang RB, Dong JZ, Long DY, Yu RH, Liu XP, Cheng YL, et al. Incidence and clinical characteristics of transient ST-T elevation during transseptal catheterization for atrial fibrillation ablation. Europace. 2015;17:579–83. https://doi.org/10.1093/europace/euu278.
Ishigaki D, Arimoto T, Iwayama T, Kutsuzawa D, Yashiro Y, Nitobe J, et al. ST-segment elevation and ventricular fibrillation shortly after transseptal puncture for left atrial catheter ablation. J Arrhythmia. 2013;29:296–9. https://doi.org/10.1016/j.joa.2013.03.004.
Le BH, Black JN, Stephen Hung SK. Transient ST-segment elevation during transseptal catheterization for atrial fibrillation ablation. Texas Hear Inst J. 2010;37:717–21.
Campagna JA, Carter C. Clinical relevance of the Bezold-Jarisch reflex. Anesthesiology. 2003;98:1250–60. https://doi.org/10.1097/00000542-200305000-00030.
Mark AL. The Bezold-Jarisch reflex revisited: Clinical implications of inhibitory reflexes originating in the heart. J Am Coll Cardiol. 1983;1:90–102. https://doi.org/10.1016/S0735-1097(83)80014-X.
Morillo CA, Verma A, Connolly SJ, Kuck KH, Nair GM, Champagne J, et al. Radiofrequency ablation vs antiarrhythmic drugs as first-line treatment of paroxysmal atrial fibrillation (RAAFT-2) a randomized trial. JAMA - J Am Med Assoc. 2014;311:692–9. https://doi.org/10.1001/jama.2014.467.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Vale, P.D., Silva, L.T.M., de Oliveira, E.M.M. et al. Incidence and characteristics of transient St-segment elevation during transseptal puncture. J Interv Card Electrophysiol 63, 425–430 (2022). https://doi.org/10.1007/s10840-021-01022-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10840-021-01022-x



