Abstract
Feedback delivery and training have not been characterized in the context of academic cancer centres. The purpose of this study was to assess the feasibility and utility of a microlearning course based on the R2C2 (Relationship, Reaction, Content, Coaching) feedback model and characterize multidisciplinary healthcare provider (HCP) perspectives on existing feedback practices in an academic cancer centre. Five HCP (two radiation oncologists, one medical oncologist, and two allied health professionals) with supervisory roles were selected by purposive sampling to participate in a prospective longitudinal qualitative study. Each participant completed a web-based multimedia course. Semi-structured one-on-one interviews were conducted with each participant at four time points: pre- and immediately post-course, and at one- and three-months post course. All participants found the course to be time feasible and completed it in 10–20 min. Participants expressed that the course fulfilled their need for feedback training and that its adoption may normalize a feedback culture in the cancer centre. Three themes were identified regarding perceptions of existing feedback practices: (1) hierarchical and interdisciplinary relationships modulate feedback delivery, (2) interest in feedback delivery varies by duration of the supervisory relationship, and (3) the transactionality of supervisor-trainee relationships influences feedback delivery. This study demonstrates the perceived feasibility and utility of a digital microlearning approach for development of feedback competencies in an academic cancer centre, perceptions of cultural barriers to feedback delivery, and the need for organizational commitment to developing a feedback culture.

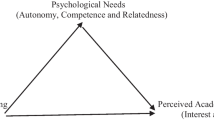
Adapted from work by Sargeant et al. [4]

Similar content being viewed by others
References
Sender Liberman A, Liberman M, Steiner Y, McLeod P, Meterissian S (2005) Surgery residents and attending surgeons have different perceptions of feedback. Med Teach 27(5):470–472. https://doi.org/10.1080/0142590500129183
Bing-You RG, Trowbridge RL (2009) Why medical educators may be failing at feedback. JAMA 302(12):1330–1331. https://doi.org/10.1001/jama.2009.1393
Bing-You RG, Varaklis K, Hayes V, Trowbridge R, Kemp H, McKelvey D (2018) The feedback tango: an integrative review and analysis of the content of the teacher-learner feedback exchange. Acad Med 93(4):657–663. https://doi.org/10.1097/ACM.0000000000001927
Sargeant J, Armson H, Driessen E, Holmboe E, Könings K, Lockyer J, Lynn L, Mann K, Ross K, Silver I, Soklaridis S, Warren A, Zetkulic M, Boudreau M, Shearer C (2016) Evidence-informed facilitated feedback: The R2C2 feedback model. MedEDPORTAL 12:10387. https://doi.org/10.15766/mep_2374-8265.10387
Lockyer J, Armson H, Könings K, Lee-Krueger RCW, des Ordons AR, Ramani S, Trier J, Zetkulic M, Sargeant J (2020) In-the-moment feedback and coaching: improving R2C2 for a new context. J Grad Med Educ 12(1):27–35. https://doi.org/10.4300/JGME-D-19-00508.1
Ruiz JG, Mintzer MJ, Leipzig RM (2006) The impact of E-learning in medical education. Acad Med 81(3):207–212. https://doi.org/10.1097/00001888-200603000-00002
Axley L (2008) The integration of technology into nursing curricula: supporting faculty via the technology fellowship program. Online J Issues Nurs 13(3). https://doi.org/10.3912/OJIN.Vol13No03PPT01
Skiba DJ, Connors HR, Jeffries PR (2008) Information technologies and the transformation of nursing education. Nurs Outlook 56(5):225–330. https://doi.org/10.1016/j.outlook.2008.06.012
Kogan JR, Hatala R, Hauer KE, Holmboe E (2017) The do’s, don’ts and don’t knows of direct observation of clinical skills in medical education. Perspect Med Educ 6(5):286–305. https://doi.org/10.1007/s40037-017-0376-7
Calman L, Brunton L, Molassiotis A (2013) Developing longitudinal qualitative designs: lessons learned and recommendations for health services research. BMC Med Res Methodol 13:14. https://doi.org/10.1186/1471-2288-13-14
Patton MQ (2002) Qualitative research and evaluation methods. SAGE Publications, Thousand Oaks, CA
Flick U (2018) The SAGE Handbook of Qualitative Data Collection. SAGE Publications, London
Colonna S, Sweetenham J, Burgon TB, Buys SS, Lynch R, Au T, Johnson E, Kubal T, Paculdo D, Acelajado MC, Peabody JW (2019) A better pathway? Building consensus and engaging providers with feedback to improve and standardize cancer care. Clin Breast Cancer 19(2):e376–e384. https://doi.org/10.1016/j.clbc.2018.12.010
Tanvetyanon T, Lee J-H, Fulp WJ, Schreiber F, Brown RH, Levine RM, Cartwright TH, Abesada-Terk G Jr, Kim GP, Alemany C, Faig D, Sharp PV, Markham MJ, Malafa M, Jacobsen PB (2014) Changes in the care of non-small cell lung cancer after audit and feedback: The Florida Initiative for Quality Cancer Care. J Oncol Pract 10(4):e247–e254. https://doi.org/10.1200/JOP.2013.001275
Ramani S, Könings KV, Mann KD, Pisarski EE, van der Vleuten CPM (2018) About politeness, face, and feedback: exploring resident and faculty perceptions of how institutional feedback culture influences feedback practices. Acad Med 93(9):1348–1358. https://doi.org/10.1097/ACM.0000000000002193
Areemit RS, Cooper CM, Wirasorn K, Paopongsawan P, Panthongviriyakul C, Ramani S (2020) Hierarchy, “Kreng Jai” and feedback: a grounded theory study exploring perspectives of clinical faculty and medical students in Thailand. Teach Learn Med 1-10https://doi.org/10.1080/10401334.20201.1813584
Krugman RD, Jones MD Jr, Lowenstein SR (2014) Can we learn civility? Reflections on the challenge of changing culture. Acad Med 89(12):1586–1588. https://doi.org/10.1097/ACM.0000000000000429
Ramani S, Post SE, Könings K, Mann K, Katz JT, van der Vleuten C (2017) “It’s just not the culture”: A qualitative study exploring residents’ perceptions of the impact of institutional culture on feedback. Teach Learn Med 29(2):153–161. https://doi.org/10.1080/10401334.2016.1244014
Kirkpatrick JD, Kirkpatrick WK (2016) Kirkpatrick’s four levels of training evaluation. Association for Talent Development Press, Alexandria
Funding
This study was funded by the CBME Residency Education Implementation Award (Postgraduate Medical Education, University of Toronto).
Author information
Authors and Affiliations
Contributions
All authors contributed to the study conception and design. Material preparation, data collection, and analysis were performed by Amir H. Safavi, Janet Papadakos, Tina Papadakos, Karen Lawrie, and Meredith E. Giuliani. The first draft of the manuscript was written by Amir H. Safavi and all authors commented on previous versions of the manuscript. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Ethics approval, consent to participate, and consent for publication
This protocol was reviewed by the Institutional Research Ethics Board and ethics approval was obtained (UHN REB #19–5981). Informed consent for participation and publication was obtained from all participants.
Conflict of interest
MG has received funding from Bristol-Myers Sqiubb, AstraZeneca, and Eli Lilly. AHS, JP, TP, NKQ, KL, EK, SS, JC, BAM, RJ, and AB declare no conflicts of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Safavi, A.H., Papadakos, J., Papadakos, T. et al. Feedback Delivery in an Academic Cancer Centre: Reflections From an R2C2-based Microlearning Course. J Canc Educ 37, 1790–1797 (2022). https://doi.org/10.1007/s13187-021-02028-9
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13187-021-02028-9