Abstract
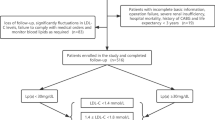
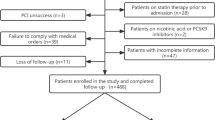
Low-density lipoprotein cholesterol (LDL-C) is a traditional and important risk factor for atherosclerotic cardiovascular disease (CVD). Recently, lipoprotein (a) (lp(a)) attracts considerable attention as a residual risk factor for CVD. However, the roles of lp(a) in acute coronary syndrome (ACS) patients with well-controlled LDL-C (≤1.8mmol/L) after percutaneous coronary intervention (PCI) remain unclear. Current study results demonstrated that occurrence of major adverse cardiovascular events (MACE) and recurrent myocardial infarction (MI) increased with the Lp(a) increasing in patients with LDL-C≤1.8mmol/L at 1-month follow-up. In relatively low-risk patients presented with ACS and underwent PCI (LDL-C ≤1.8mmol/L at 1-month follow-up), lp(a) is still independently related to adverse prognosis. Further researches of targeted therapy against lp(a) are warranted.



Similar content being viewed by others
References
Hu, X., Yang, X., Li, X., Luo, D., Zhou, Y., & Dong, H. (2020). Lipoprotein (a) as a residual risk factor for atherosclerotic renal artery stenosis in hypertensive patients: A hospital-based cross-sectional study. Lipids in Health and Disease, 19(1), 173.
Cai, A., Li, L., Zhang, Y., Mo, Y., Mai, W., & Zhou, Y. (2013). Lipoprotein(a): A promising marker for residual cardiovascular risk assessment. Disease Markers, 35(5), 551–559.
Mach, F., Baigent, C., Catapano, A., Koskinas, K., Casula, M., Badimon, L., et al. (2020). 2019 ESC/EAS Guidelines for the management of dyslipidaemias: Lipid modification to reduce cardiovascular risk. European Heart Journal, 41(1), 111–188.
Catapano, A., Graham, I., De Backer, G., Wiklund, O., Chapman, M., Drexel, H., et al. (2016). 2016 ESC/EAS Guidelines for the Management of Dyslipidaemias. European Heart Journal, 37(39), 2999–3058.
Campbell, C., Rivera, J., & Blumenthal, R. (2007). Residual risk in statin-treated patients: Future therapeutic options. Current Cardiology Reports, 9(6), 499–505.
Erqou, S., Kaptoge, S., Perry, P., Di Angelantonio, E., Thompson, A., White, I., et al. (2009). Lipoprotein(a) concentration and the risk of coronary heart disease, stroke, and nonvascular mortality. JAMA, 302(4), 412–423.
Nicholls, S., Tang, W., Scoffone, H., Brennan, D., Hartiala, J., Allayee, H., et al. (2010). Lipoprotein(a) levels and long-term cardiovascular risk in the contemporary era of statin therapy. Journal of Lipid Research, 51(10), 3055–3061.
Nielsen, L., Grønholdt, M., Schroeder, T., Stender, S., & Nordestgaard, B. (1997). In vivo transfer of lipoprotein(a) into human atherosclerotic carotid arterial intima. Arteriosclerosis, Thrombosis, and Vascular Biology, 17(5), 905–911.
Boffa, M., Marcovina, S., & Koschinsky, M. (2004). Lipoprotein(a) as a risk factor for atherosclerosis and thrombosis: Mechanistic insights from animal models. Clinical Biochemistry, 37(5), 333–343.
Poon, M., Zhang, X., Dunsky, K., Taubman, M., & Harpel, P. (1997). Apolipoprotein(a) induces monocyte chemotactic activity in human vascular endothelial cells. Circulation, 96(8), 2514–2519.
Nielsen, L., Juul, K., & Nordestgaard, B. (1998). Increased degradation of lipoprotein(a) in atherosclerotic compared with nonlesioned aortic intima-inner media of rabbits: In vivo evidence that lipoprotein(a) may contribute to foam cell formation. Arteriosclerosis, Thrombosis, and Vascular Biology, 18(4), 641–649.
Bennet, A., Di Angelantonio, E., Erqou, S., Eiriksdottir, G., Sigurdsson, G., Woodward, M., et al. (2008). Lipoprotein(a) levels and risk of future coronary heart disease: Large-scale prospective data. Archives of Internal Medicine, 168(6), 598–608.
Jørgensen, A., Frikke-Schmidt, R., West, A., Grande, P., Nordestgaard, B., & Tybjærg-Hansen, A. (2013). Genetically elevated non-fasting triglycerides and calculated remnant cholesterol as causal risk factors for myocardial infarction. European Heart Journal, 34(24), 1826–1833.
Suk Danik, J., Rifai, N., Buring, J., & Ridker, P. (2006). Lipoprotein(a), measured with an assay independent of apolipoprotein(a) isoform size, and risk of future cardiovascular events among initially healthy women. JAMA, 296(11), 1363–1370.
Liu, H., Cao, Y., Jin, J., Zhang, H., Hua, Q., Li, Y., et al. (2020). Association of lipoprotein(a) levels with recurrent events in patients with coronary artery disease. Heart (British Cardiac Society)., 106(16), 1228–1235.
Schwartz, G., Ballantyne, C., Barter, P., Kallend, D., Leiter, L., Leitersdorf, E., et al. (2018). Association of Lipoprotein(a) With Risk of Recurrent Ischemic Events Following Acute Coronary Syndrome: Analysis of the dal-Outcomes Randomized Clinical Trial. JAMA Cardiology, 3(2), 164–168.
Levine, G., Bates, E., Bittl, J., Brindis, R., Fihn, S., Fleisher, L., et al. (2016). 2016 ACC/AHA Guideline Focused Update on Duration of Dual Antiplatelet Therapy in Patients With Coronary Artery Disease: A Report of the American College of Cardiology/American Heart Association Task Force on Clinical Practice Guidelines: An Update of the 2011 ACCF/AHA/SCAI Guideline for Percutaneous Coronary Intervention, 2011 ACCF/AHA Guideline for Coronary Artery Bypass Graft Surgery, 2012 ACC/AHA/ACP/AATS/PCNA/SCAI/STS Guideline for the Diagnosis and Management of Patients With Stable Ischemic Heart Disease, 2013 ACCF/AHA Guideline for the Management of ST-Elevation Myocardial Infarction, 2014 AHA/ACC Guideline for the Management of Patients With Non-ST-Elevation Acute Coronary Syndromes, and 2014 ACC/AHA Guideline on Perioperative Cardiovascular Evaluation and Management of Patients Undergoing Noncardiac Surgery. Circulation, 134(10), e123-55.
Li, Z., Li, G., Zhou, Y., Chen, Z., Yang, J., Zhang, Y., et al. (2013). Lack of association between lipoprotein(a) genetic variants and subsequent cardiovascular events in Chinese Han patients with coronary artery disease after percutaneous coronary intervention. Lipids in health and disease, 12(127).
Nestel, P., Barnes, E., Tonkin, A., Simes, J., Fournier, M., White, H., et al. (2013). Plasma lipoprotein(a) concentration predicts future coronary and cardiovascular events in patients with stable coronary heart disease. Arteriosclerosis, Thrombosis, and Vascular Biology, 33(12), 2902–2908.
O'Donoghue, M., Morrow, D., Tsimikas, S., Sloan, S., Ren, A., Hoffman, E., et al. (2014). Lipoprotein(a) for risk assessment in patients with established coronary artery disease. Journal of the American College of Cardiology, 63(6), 520–527.
Holmer, S. R., Hengstenberg, C., Kraft, H. G., Mayer, B., Pöll, M., Kürzinger, S., et al. (2003). Association of polymorphisms of the apolipoprotein(a) gene with lipoprotein(a) levels and myocardial infarction. Circulation, 107(5), 696–701.
Giugliano, R., Pedersen, T., Park, J., De Ferrari, G., Gaciong, Z., Ceska, R., et al. (2017). Clinical efficacy and safety of achieving very low LDL-cholesterol concentrations with the PCSK9 inhibitor evolocumab: A prespecified secondary analysis of the FOURIER trial. Lancet (London, England), 390(10106), 1962–1971.
Raal, F. J., Giugliano, R. P., Sabatine, M. S., Koren, M. J., Blom, D., Seidah, N. G., et al. (2016). PCSK9 inhibition-mediated reduction in Lp(a) with evolocumab: an analysis of 10 clinical trials and the LDL receptor's role. Journal of Lipid Research, 57(6), 1086–1096.
Cai, A., Li, L., Zhang, Y., Mo, Y., Li, Z., Mai, W., et al. (2013). Baseline LDL-C and Lp(a) elevations portend a high risk of coronary revascularization in patients after stent placement. Disease Markers, 35(6), 857–862.
Liu, H. H., Cao, Y. X., Jin, J. L., Zhang, H. W., Hua, Q., Li, Y. F., et al. (2020). Predicting Cardiovascular Outcomes by Baseline Lipoprotein(a) Concentrations: A Large Cohort and Long-Term Follow-up Study on Real-World Patients Receiving Percutaneous Coronary Intervention. Journal of the American Heart Association, 9(3), e014581.
Acknowledgements
The authors would like to thank Yidu Cloud Technology Co., Ltd for their assistance in data searching, extraction, and processing.
Funding
This study was funded by Liaoning Province Natural Science Foundation ((20180550892) to Dr. Yin and (2019-ZD-0635) to Dr. Ren).
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Ethical Approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Informed Consent
Informed consent was obtained from all individual participants included in the study.
Conflict of Interest
All the authors declare no conflict of interest.
Additional information
Associate Editor Craig M. Stolen oversaw the review of this article
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Ren, Y., Pan, W., Li, X. et al. The Predictive Value of Lp(a) for Adverse Cardiovascular Event in ACS Patients With an Achieved LDL-C Target at Follow Up After PCI. J. of Cardiovasc. Trans. Res. 15, 67–74 (2022). https://doi.org/10.1007/s12265-021-10148-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12265-021-10148-2