Abstract
Objectives
Inflammatory bowel disease (IBD) is a chronic and idiopathic gastrointestinal pathology whose bi-directional relation with psychological variables (e.g., quality of life, fatigue, and stress) has been studied in depth. Dispositional mindfulness has been related to a better quality of life and health in chronic diseases. The present study aims to examine the potential mediator influence of dispositional mindfulness in the association between disease severity and health-related quality of life, stress, and fatigue in IBD patients.
Methods
In a cross-sectional study, 152 patients diagnosed with IBD were recruited from the digestive unit of Sagunt Hospital (Spain) where they were receiving treatment. Dispositional mindfulness, fatigue, perceived stress, health-related quality of life, and illness severity were measured. Subsequently, descriptive statistical analyses, Pearson product-moment correlations, multivariate analysis of variance, and mediation analyses were performed.
Results
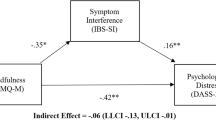
Dispositional mindfulness facets were positively associated with quality of life, lower fatigue, and lower perceived stress levels (except for the observe subscale). Mediation analyses showed that IBD severity (moderate vs. mild patients) indirectly influenced quality of life (ab = −6.16, 95% CI [−13.46, −0.76]), perceived stress (ab = 2.23, 95% CI [0.41, 4.24]), and fatigue (ab = 3.24, 95% CI [0.48, 6.66]) through its effect on the dispositional mindfulness facet “acting with awareness.”
Conclusions
Dispositional mindful awareness seems to be a protective factor in addition to a promising intervention target in IBD patients, whose severity only influences quality of life, perceived stress, and fatigue through it.

Similar content being viewed by others
References
Armuzzi, A., Tarallo, M., Bargo, D., Lucas, J., Bluff, D., Hoskin, B., Salese, L., Cappelleri, J., Kayhan, C., & DiBonaventura, M. (2019). Perceived disease severity and treatment satisfaction among patients with ulcerative colitis in Europe. Journal of Crohn’s and Colitis, 13, 224–225.
Baer, R. A., Smith, G. T., Hopkins, J., Krietemeyer, J., & Toney, L. (2006). Using self-report assessment methods to explore facets of mindfulness. Assessment, 13(1), 27–45.
Baer, R. A., Smith, G. T., Lykins, E., Button, D., Krietemeyer, J., Sauer, S., Walsh, E., Duggan, D., & Williams, J. M. G. (2008). Construct validity of the five facet mindfulness questionnaire in meditating and nonmeditating samples. Assessment, 15(3), 329–342.
Ballou, S., & Keefer, L. (2017). Psychological interventions for irritable bowel syndrome and inflammatory bowel diseases. Clinical and Translational Gastroenterology, 8(1), e214.
Bernstein, C. N. (2016). Psychological stress and depression: Risk factors for IBD? Digestive Diseases, 34(1-2), 58–63.
Bishop, S. R., Lau, M., Shapiro, S., Carlson, L., Anderson, N. D., Carmody, J., Segal, Z. V., Abbey, S., Speca, M., & Velting, D. (2004). Mindfulness: A proposed operational definition. Clinical Psychology: Science and Practice, 11(3), 230–241.
Böhmig, M. (2019). Mechanisms of disease, etiology and clinical manifestations. In A. Sturm & L. White (Eds.), Inflammatory bowel disease nursing manual (pp. 15–24). Springer.
Bränström, R., Kvillemo, P., Brandberg, Y., & Moskowitz, J. T. (2010). Self-report mindfulness as a mediator of psychological well-being in a stress reduction intervention for cancer patients—A randomized study. Annals of Behavioral Medicine, 39(2), 151–161.
Castillo-Cejas, M. D., Robles, V., Borruel, N., Torrejón, A., Navarro, E., Peláez, A., & Casellas, F. (2013). Questionnaires for measuring fatigue and its impact on health perception in inflammatory bowel disease. Revista Española De Enfermedades Digestivas, 105(3), 144–153.
Cebolla, A., Garcia-Palacios, A., Soler, J., Guillén, V., Baños, R., & Botella, C. (2012). Psychometric properties of the Spanish validation of the five facets of mindfulness questionnaire (FFMQ). The European Journal of Psychiatry, 26(2), 118–126.
Cohen, S., Kamarck, T., & Mermelstein, R. (1983). A global measure of perceived stress. Journal of Health and Social Behavior, 24, 385–396.
Davidson, R. J. (2010). Empirical explorations of mindfulness: Conceptual and methodological conundrums. Emotion, 10(1), 8–11. https://doi.org/10.1037/a0018480.
De Souza, H. S., & Fiocchi, C. (2016). Immunopathogenesis of IBD: Current state of the art. Nature Reviews Gastroenterology & Hepatology, 13(1), 13-27.
Ewais, T., Begun, J., Kenny, M., Rickett, K., Hay, K., Ajilchi, B., & Kisely, S. (2019). A systematic review and meta-analysis of mindfulness based interventions and yoga in inflammatory bowel disease. Journal of Psychosomatic Research, 116, 44–53.
Garland, E. L., Gaylord, S. A., Palsson, O., Faurot, K., Mann, J. D., & Whitehead, W. E. (2012). Therapeutic mechanisms of a mindfulness-based treatment for IBS: Effects on visceral sensitivity, catastrophizing, and affective processing of pain sensations. Journal of Behavioral Medicine, 35(6), 591–602.
Gracie, D. J., Irvine, A. J., Sood, R., Mikocka-Walus, A., Hamlin, P. J., & Ford, A. C. (2017). Effect of psychological therapy on disease activity, psychological comorbidity, and quality of life in inflammatory bowel disease: A systematic review and meta-analysis. The Lancet Gastroenterology & Hepatology, 2(3), 189–199.
Guyatt, G., Mitchell, A., Irvine, E. J., Singer, J., Williams, N., Goodacre, R., & Tompkins, C. (1989). A new measure of health status for clinical trials in inflammatory bowel disease. Gastroenterology, 96(2), 804–810.
Hayes, A. F. (2017). Introduction to mediation, moderation, and conditional process analysis: A regression-based approach (2nd ed.). Guilford publications.
Hood, M. M., & Jedel, S. (2017). Mindfulness-based interventions in inflammatory bowel disease. Gastroenterology Clinics, 46(4), 859–874.
Jedel, S., Merriman, P., Hoffman, A., Swanson, B., Fogg, L. F., & Keshavarzian, A. (2013). Relationship of mindfulness, quality of life, and psychiatric symptoms among patients with ulcerative colitis. Mindfulness, 4(4), 296–300.
Kabat-Zinn, J. (1990). Full catastrophe living: Using the wisdom of your mind to face stress, pain and illness. New York: Dell.
Kappelman, M. D., Long, M. D., Martin, C., DeWalt, D. A., Kinneer, P. M., Chen, W., Lewis, J. D., & Sandler, R. S. (2014). Evaluation of the patient-reported outcomes measurement information system in a large cohort of patients with inflammatory bowel diseases. Clinical Gastroenterology and Hepatology, 12(8), 1315–1323.
Kiken, L. G., Garland, E. L., Bluth, K., Palsson, O. S., & Gaylord, S. A. (2015). From a state to a trait: Trajectories of state mindfulness in meditation during intervention predict changes in trait mindfulness. Personality and Individual Differences, 81, 41–46.
Knowles, S. R., Graff, L. A., Wilding, H., Hewitt, C., Keefer, L., & Mikocka-Walus, A. (2018a). Quality of life in inflammatory bowel disease: A systematic review and meta-analyses—part I. Inflammatory Bowel Diseases, 24(4), 742–751.
Knowles, S. R., Keefer, L., Wilding, H., Hewitt, C., Graff, L. A., & Mikocka-Walus, A. (2018b). Quality of life in inflammatory bowel disease: A systematic review and meta-analyses—part II. Inflammatory Bowel Diseases, 24(5), 966–976.
Krupp, L. B., LaRocca, N. G., Muir-Nash, J., & Steinberg, A. D. (1989). The fatigue severity scale: Application to patients with multiple sclerosis and systemic lupus erythematosus. Archives of Neurology, 46(10), 1121–1123.
Lecuona, O., García-Garzón, E., García-Rubio, C., & Rodríguez-Carvajal, R. (2019). A psychometric review and conceptual replication study of the Five Facets Mindfulness Questionnaire latent structure. Assessment, 27(5), 859–872.
Luo, H., Sun, Y., Li, Y., Lv, H., Sheng, L., Wang, L., & Qian, J. (2018). Perceived stress and inappropriate coping behaviors associated with poorer quality of life and prognosis in patients with ulcerative colitis. Journal of Psychosomatic Research, 113, 66–71.
Maaser, C., Sturm, A., Vavricka, S. R., Kucharzik, T., Fiorino, G., Annese, V., Calabrese, E., Baumgart, D. C., Bettenworth, D., & Borralho Nunes, P. (2019). ECCO-ESGAR Guideline for Diagnostic Assessment in IBD Part 1: Initial diagnosis, monitoring of known IBD, detection of complications. Journal of Crohn’s and Colitis, 13(2), 144–164.
MacKinnon, D. P., & Fairchild, A. J. (2009). Current directions in mediation analysis. Current Directions in Psychological Science, 18(1), 16–20.
Masachs, M., Casellas, F., & Malagelada, J. R. (2007). Traducción, adaptación y validación al español del cuestionario de calidad de vida de 32 ítems (IBDQ-32) de la enfermedad inflamatoria intestinal. Revista Española de Enfermedades Digestivas, 99(9), 511–519.
Maxwell, S. E., & Cole, D. A. (2007). Bias in cross-sectional analyses of longitudinal mediation. Psychological Methods, 12(1), 23-44.
Moskowitz, J. T., Duncan, L. G., Moran, P. J., Acree, M., Epel, E. S., Kemeny, M. E., Hecht, F. M., & Folkman, S. (2015). Dispositional mindfulness in people with HIV: Associations with psychological and physical health. Personality and Individual Differences, 86, 88–93.
Mun, C. J., Okun, M. A., & Karoly, P. (2014). Trait mindfulness and catastrophizing as mediators of the association between pain severity and pain-related impairment. Personality and Individual Differences, 66, 68–73.
Murphy, M. J., Mermelstein, L. C., Edwards, K. M., & Gidycz, C. A. (2012). The benefits of dispositional mindfulness in physical health: A longitudinal study of female college students. Journal of American College Health, 60(5), 341–348.
Naliboff, B. D., Kim, S. E., Bolus, R., Bernstein, C. N., Mayer, E. A., & Chang, L. (2012). Gastrointestinal and psychological mediators of health-related quality of life in IBS and IBD: A structural equation modeling analysis. The American Journal of Gastroenterology, 107(3), 451-459.
Neuendorf, R., Harding, A., Stello, N., Hanes, D., & Wahbeh, H. (2016). Depression and anxiety in patients with inflammatory bowel disease: A systematic review. Journal of Psychosomatic Research, 87, 70–80.
Pagnini, F., Cavalera, C., Rovaris, M., Mendozzi, L., Molinari, E., Phillips, D., & Langer, E. (2019). Longitudinal associations between mindfulness and well-being in people with multiple sclerosis. International Journal of Clinical and Health Psychology, 19(1), 22–30.
Pariente, B., Cosnes, J., Danese, S., Sandborn, W. J., Lewin, M., Fletcher, J. G., Chowers, Y., D’Haens, G., Feagan, B. G., Hibi, T., Hommes, D. W., Irvine, J. E., Kamm, M. A., Loftus, E. V., Jr, Louis, E., Michetti, P., Munkholm, P., Oresland, T., Panés, J., … Lémann, M. (2011). Development of the Crohn’s disease digestive damage score, the Lémann score. Inflammatory Bowel Diseases, 17(6), 1415-1422. https://doi.org/10.1002/ibd.21506.
Pedrero-Pérez, E., Ruiz Sánchez de León, J., Lozoya-Delgado, P., Gloria, R. M., Llanero, M., & Puerta-García, C. (2015). The Perceived Stress Scale: An unrestricted approach to its psychometric properties in non-clinical population and treated substance-addicts. Behavioral Psychology/Psicologia Conductual, 23, 305–324.
Pekow, J. (2015). Do I have Crohn’s disease or ulcerative colitis? Identifying factors that distinguish CD from UC and indeterminate colitis. In D. J. Stein & R. Shaker (Eds.) Inflammatory bowel disease: A point of care clinical guide (pp. 29–33). Springer International Publishing. https://doi.org/10.1007/978-3-319-14072-8_5.
Peyrin-Biroulet, L., Sandborn, W., Sands, B. E., Reinisch, W., Bemelman, W., Bryant, R. V., D’Haens, G., Dotan, I., Dubinsky, M., Feagan, B., Fiorino, G., Gearry, R., Krishnareddy, S., Lakatos, P. L., Loftus, E. V. J., Marteau, P., Munkholm, P., Murdoch, T. B., Ordás, I., … Colombel, J.-F. (2015). Selecting therapeutic targets in inflammatory bowel disease (stride): Determining therapeutic goals for treat-to-target. Official Journal of the American College of Gastroenterology, 110(9), 1324-1338. https://doi.org/10.1038/ajg.2015.233
Pleman, B., Park, M., Han, X., Price, L. L., Bannuru, R. R., Harvey, W. F., Driban, J. B., & Wang, C. (2019). Mindfulness is associated with psychological health and moderates the impact of fibromyalgia. Clinical Rheumatology, 38(6), 1737–1745. https://doi.org/10.1007/s10067-019-04436-1.
Podsakoff, P. M., MacKenzie, S. B., Lee, J.-Y., & Podsakoff, N. P. (2003). Common method biases in behavioral research: A critical review of the literature and recommended remedies. Journal of Applied Psychology, 88(5), 879–903. https://doi.org/10.1037/0021-9010.88.5.879.
Raimundo, K., Montagut, T. R., Flores, N. M., & Low, J. (2018). The impact of inflammatory bowel disease severity on health-related quality of life. Gastroenterology, 154(1), S109. https://doi.org/10.1053/j.gastro.2017.11.256.
Rau, H. K., & Williams, P. G. (2016). Dispositional mindfulness: A critical review of construct validation research. Personality and Individual Differences, 93, 32–43. https://doi.org/10.1016/j.paid.2015.09.035.
Salmoirago-Blotcher, E., Crawford, S., Carmody, J., Rosenthal, L., & Ockene, I. (2011). Characteristics of dispositional mindfulness in patients with severe cardiac disease. Journal of Evidence-Based Complementary & Alternative Medicine, 16(3), 218–225. https://doi.org/10.1177/2156587211405525.
Schirda, B., Nicholas, J. A., & Prakash, R. S. (2015). Examining trait mindfulness, emotion dysregulation, and quality of life in multiple sclerosis. Health Psychology, 34(11), 1107–1115. https://doi.org/10.1037/hea0000215.
Schoultz, M., Beattie, M., Gorely, T., & Leung, J. (2020). Assessment of causal link between psychological factors and symptom exacerbation in inflammatory bowel disease: A systematic review utilising Bradford Hill criteria and meta-analysis of prospective cohort studies. Systematic Reviews, 9(1), 169. https://doi.org/10.1186/s13643-020-01426-2.
Schreiber, S., Panés, J., Louis, E., Holley, D., Buch, M., & Paridaens, K. (2012). Perception gaps between patients with ulcerative colitis and healthcare professionals: An online survey. BMC Gastroenterology, 12(1), 108. https://doi.org/10.1186/1471-230X-12-108.
Senders, A., Bourdette, D., Hanes, D., Yadav, V., & Shinto, L. (2014). Perceived stress in multiple sclerosis: the potential role of mindfulness in health and well-being. Journal of Evidence-Based Complementary & Alternative Medicine, 19(2), 104–111. https://doi.org/10.1177/2156587214523291.
Thoguluva, V., & Venu, N. (2015). So what is Crohn’s disease and ulcerative colitis? Pathophysiology of Crohn’s disease and ulcerative colitis. In D. J. Stein & R. Shaker (Eds.), Inflammatory bowel disease: A point of care clinical guide (pp. 15-23). Springer International Publishing. https://doi.org/10.1007/978-3-319-14072-8_3.
Thomas, E. A., & Garland, E. L. (2017). Mindfulness is associated with increased hedonic capacity among chronic pain patients receiving extended opioid pharmacotherapy. The Clinical Journal of Pain, 33(2), 166–173. https://doi.org/10.1097/AJP.0000000000000379.
Timmer, A., Preiss, J. C., Motschall, E., Rücker, G., Jantschek, G., & Moser, G. (2011). Psychological interventions for treatment of inflammatory bowel disease. Cochrane Database of Systematic Reviews, 2, CD006913. https://doi.org/10.1002/14651858.CD006913.pub2.
Tran, U. S., Cebolla, A., Glück, T. M., Soler, J., Garcia-Campayo, J., & von Moy, T. (2014). The serenity of the meditating mind: a cross-cultural psychometric study on a two-factor higher order structure of mindfulness, its effects, and mechanisms related to mental health among experienced meditators. PLoS ONE, 9(10), e110192. https://doi.org/10.1371/journal.pone.0110192.
Trindade, I. A., Ferreira, C., & Pinto-Gouveia, J. (2016). Inflammatory bowel disease: The harmful mechanism of experiential avoidance for patients’ quality of life. Journal of Health Psychology, 21(12), 2882–2892. https://doi.org/10.1177/1359105315587142.
Truelove, S. C., & Witts, L. J. (1955). Cortisone in ulcerative colitis; final report on a therapeutic trial. British Medical Journal, 2(4947), 1041–1048. https://doi.org/10.1136/bmj.2.4947.1041.
Ungaro, R., Mehandru, S., Allen, P. B., Peyrin-Biroulet, L., & Colombel, J.-F. (2017). Ulcerative colitis. The Lancet, 389(10080), 1756–1770. https://doi.org/10.1016/S0140-6736(16)32126-2.
Whitaker, R. C., Dearth-Wesley, T., Gooze, R. A., Becker, B. D., Gallagher, K. C., & McEwen, B. S. (2014). Adverse childhood experiences, dispositional mindfulness, and adult health. Preventive Medicine, 67, 147–153. https://doi.org/10.1016/j.ypmed.2014.07.029.
Whitaker, R. C., Herman, A. N., Dearth-Wesley, T., Hubbell, K., Huff, R., Heneghan, L. J., & Rowe, P. C. (2019). The association of fatigue with dispositional mindfulness: Relationships by levels of depressive symptoms, sleep quality, childhood adversity, and chronic medical conditions. Preventive Medicine, 129, 105873. https://doi.org/10.1016/j.ypmed.2019.105873.
Zhang, M., Hong, L., Zhang, T., Lin, Y., Zheng, S., Zhou, X., Fan, R., Wang, Z., Zhang, C., & Zhong, J. (2016). Illness perceptions and stress: Mediators between disease severity and psychological well-being and quality of life among patients with Crohn’s disease. Patient preference and adherence, 10, 2387–2396. https://doi.org/10.2147/PPA.S118413.
Funding
This work was supported by CIBEROBN, an initiative of the ISCIII (ISC III CB06 03/0052) and Ministerio de Economía y Competitividad (Spain) under AMABLE-VR (RTI2018-097835-A-I00).
Author information
Authors and Affiliations
Contributions
JN and XC performed the recruitment. JN conducted the formal analyses and wrote the results section. JN, AC, and RMB wrote the original draft. RG-M, JFL, JMS, and XC collaborated in the writing and editing of the final manuscript. All author approved the final version of the manuscript for submission.
Corresponding author
Ethics declarations
Conflict of Interest
The authors declare no competing interests.
Ethics Approval
This cross-sectional study was approved by the Human Ethics Committee at the University Hospital of Sagunto (Spain).
Informed Consent
Freely given, informed consent to participate in the study was obtained from participants.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Navarrete, J., González-Moret, R., Cortés, X. et al. Dispositional Mindfulness and Inflammatory Bowel Disease: Mindful Awareness Mediates the Relation Between Severity and Quality of Life, Stress, and Fatigue. Mindfulness 12, 1524–1533 (2021). https://doi.org/10.1007/s12671-021-01620-w
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12671-021-01620-w