Abstract
Objectives
To propose multiparametric MRI-based machine learning models and assess their ability to preoperatively predict rectal adenoma with canceration.
Materials and methods
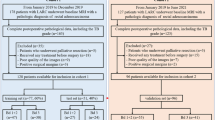
A total of 53 patients with postoperative pathology confirming rectal adenoma (n = 29) and adenoma with canceration (n = 24) were enrolled in this retrospective study. All patients were divided into a training cohort (n = 42) and a test cohort (n = 11). All patients underwent preoperative pelvic MR examination, including high-resolution T2-weighted imaging (HR-T2WI) and diffusion-weighted imaging (DWI). A total of 1396 radiomics features were extracted from the HR-T2WI and DWI sequences, respectively. The least absolute shrinkage and selection operator (LASSO) was utilized for feature selection from the radiomics feature sets from the HR-T2WI and DWI sequences and from the combined feature set with 2792 radiomics features incorporating two sequences. Five-fold cross-validation and two machine learning algorithms (logistic regression, LR; support vector machine, SVM) were utilized for model construction in the training cohort. The diagnostic performance of the models was evaluated by sensitivity, specificity and area under the curve (AUC) and compared with the Delong’s test.
Results
Ten, 8, and 25 optimal features were selected from 1396 HR-T2WI, 1396 DWI and 2792 combined features, respectively. Three group models were constructed using the selected features from HR-T2WI (ModelT2), DWI (ModelDWI) and the two sequences combined (Modelcombined). Modelcombined showed better prediction performance than ModelT2 and ModelDWI. In Modelcombined, there was no significant difference between the LR and SVM algorithms (p = 0.4795), with AUCs in the test cohort of 0.867 and 0.900, respectively.
Conclusions
Multiparametric MRI-based machine learning models have the potential to predict rectal adenoma with canceration. Compared with ModelT2 and ModelDWI, Modelcombined showed the best performance. Moreover, both LR and SVM have equal excellent performance for model construction.




Similar content being viewed by others
Abbreviations
- MRI :
-
Magnetic resonance imaging
- HR-T2WI:
-
High-resolution T2-weighted imaging
- DWI:
-
Diffusion-weighted imaging
- LASSO:
-
Least absolute shrinkage and selection operator
- LR:
-
Logistic regression
- SVM:
-
Support vector machine
- AUC:
-
Area under the curve
- CRC:
-
Colorectal cancer
- EMR:
-
Endoscopic mucosal resection
- ESD:
-
Endoscopic submucosal dissection
- ERC:
-
Early rectal cancer
- MP:
-
Muscularis propria
- TE:
-
Echo time
- TR:
-
Repetition time
- FOV:
-
Field of view
- ROI:
-
Region of interest
- GLCM:
-
Gray-level co-occurrence matrix
- GLRLM:
-
Gray-level run-length matrix
- GLSZM:
-
Gray-level size zone matrix
- GLDM:
-
Gray-level dependence matrix
- NGTDM:
-
Neighbouring gray-tone difference matrix
- ICC:
-
Interclass correlation coefficient
- SMOTE:
-
Synthetic minority over-sampling Technique
- ROC:
-
Receiver operating characteristic
- CEA:
-
Carcinoembryonic antigen
- CA199:
-
Carbohydrate antigen 19–9
- CA724:
-
Carbohydrate antigen 724
- FPR :
-
False-positive rate
- FNR :
-
False-negative rate
- SD:
-
Standard deviation
- Sen :
-
Sensitivity
- Spe :
-
Specificity
- MSE :
-
Mean-square error
- NM:
-
Normal mucosa
References
Ferlay J, Colombet M, Soerjomataram I et al (2019) Estimating the global cancer incidence and mortality in 2018: GLOBOCAN sources and methods. Int J Cancer 144(8):1941–1953
Ferlay J, Soerjomataram I, Dikshit R et al (2015) Cancer incidence and mortality worldwide: sources, methods and major patterns in GLOBOCAN 2012. Int J Cancer 136(5):E359–E386
Pasha HF, Radwan MI, Yehia AM (2019) Circulating methylated RUNX3 and SFRP1 genes as a noninvasive panel for early detection of colorectal cancer. Eur J Gastroenterol Hepatol 31(11):1342–1349
Wang X, Kuang YY (2014) Advances in epigenetic biomarker research in colorectal cancer. World J Gastroenterol 20(15):4276–4287
Xue VW, Cheung MT, Chan PT et al (2019) Non-invasive potential circulating mRNA markers for colorectal adenoma using targeted sequencing. Sci Rep 9(1):12943
Soto Y, Limia CM, González L et al (2016) Molecular evidence of high-risk human papillomavirus infection in colorectal tumours from Cuban patients. Mem Inst Oswaldo Cruz 111(12):731–736
Enquist IB, Good Z, Jubb AM et al (2014) Lymph node-independent liver metastasis in a model of metastatic colorectal cancer. Nat Commun 5:3530
Yin Y, Song M, Gu B et al (2016) Systematic analysis of key miRNAs and related signaling pathways in colorectal tumorigenesis. Gene 578(2):177–184
Rutter MD, Chattree A, Barbour JA et al (2015) British Society of Gastroenterology/Association of Coloproctologists of Great Britain and Ireland guidelines for the management of large nonpedunculated colorectal polyps. Gut 64(12):1847–1873
Saunders BP, Tsiamoulos ZP (2016) Endoscopic mucosal resection and endoscopic submucosal dissection of large colonic polyps. Nat Rev Gastroenterol Hepatol 13(8):486–496
Moss A, Williams SJ, Hourigan LF et al (2015) Long-term adenoma recurrence following wide-field endoscopic mucosal resection (WF-EMR) for advanced colonic mucosal neoplasia is infrequent: results and risk factors in 1000 cases from the Australian Colonic EMR (ACE) study. Gut 64(1):57–65
Jin Y, Yao L, Zhou P et al (2018) Risk analysis of the canceration of colorectal large polyps. Zhonghua Wei Chang Wai Ke Za Zhi 21(10):1161–1166
Balyasnikova S, Read J, Wotherspoon A et al (2017) Diagnostic accuracy of high-resolution MRI as a method to predict potentially safe endoscopic and surgical planes in patients with early rectal cancer. BMJ Open Gastroenterol 4(1):e000151
Çolakoğlu Er H, Peker E, Erden A et al (2018) Rectal cancer confined to the bowel wall: the role of 3 Tesla phased-array MR imaging in T categorization. Br J Radiol 91(1082):20170581
Kudou M, Nakanishi M, Kuriu Y et al (2020) Value of intra-tumor heterogeneity evaluated by diffusion-weighted MRI for predicting pathological stages and therapeutic responses to chemoradiotherapy in lower rectal cancer. J Cancer 11(1):168–176
Huang YQ, Liang CH, He L et al (2016) Development and validation of a radiomics nomogram for preoperative prediction of lymph node metastasis in colorectal cancer. J Clin Oncol 34:2157–2164
Nie K, Shi L, Chen Q et al (2016) Rectal cancer: assessment of neoadjuvant chemoradiation outcome based on radiomics of multiparametric MRI. Clin Cancer Res 22(21):5256–5264
Gillies RJ, Kinahan PE (2016) Radiomics: images are more than pictures, they are data. Radiology 278(2):563–577
Liang C, Huang Y, He L et al (2016) The development and validation of a CT-based radiomics signature for the preoperative discrimination of stage I–II and stage III–IV colorectal cancer. Oncotarget 7(21):31401–31412
Yang L, Dong D, Fang M et al (2018) Can CT-based radiomics signature predict KRAS/NRAS/BRAF mutations in colorectal cancer? Eur Radiol 28(5):2058–2067
Meng X, Xia W, Xie P et al (2019) Preoperative radiomic signature based on multiparametric magnetic resonance imaging for noninvasive evaluation of biological characteristics in rectal cancer. Eur Radiol 29(6):3200–3209
Liu Z, Zhang XY, Shi YJ et al (2017) Radiomics analysis for evaluation of pathological complete response to neoadjuvant chemoradiotherapy in locally advanced rectal cancer. Clin Cancer Res 23(23):7253–7262
Golia Pernicka JS, Gagniere J, Chakraborty J et al (2019) Radiomics-based prediction of microsatellite instability in colorectal cancer at initial computed tomography evaluation. Abdom Radiol (NY) 44(11):3755–3763
Liu G (2019) Role of miRNA in transformation from normal tissue to colorectal adenoma and cancer. J Cancer Res Ther 15:278–285
Levin B, Lieberman DA, McFarland B, Andrews KS, Brooks D, Bond J, American Cancer Society Colorectal Cancer Advisory Group, US Multi-Society Task Force, American College of Radiology Colon Cancer Committee (2008) Screening and surveillance for the early detection of colorectal cancer and adenomatous polyps, 2008: a joint guideline from the American Cancer Society, the US multi-society taskforce on colorectal cancer, and the American College of Radiology. Gastroenterology 134:1570–1595
Lambin P, Rios-Velazquez E, Leijenaar R et al (2012) Radiomics: extracting more information from medical images using advanced feature analysis. Eur J Cancer (Oxford, England: 1990) 48(4):441–446
Kumar V, Gu Y, Basu S et al (2012) Radiomics: the process and the challenges. Magn Reson Imaging 30(9):1234–1248
Liang M, Cai Z, Zhang H et al (2019) Machine learning-based analysis of rectal cancer MRI radiomics for prediction of metachronous liver metastasis. Acad Radiol 26(11):1495–1504
Lubner MG, Stabo N, Lubner SJ et al (2015) CT textural analysis of hepatic metastatic colorectal cancer: pre-treatment tumor heterogeneity correlates with pathology and clinical outcomes[J]. Abdom Imag 40(7):2331–2337
Huang Y, He L, Dong D et al (2018) Individualized prediction of perineural invasion in colorectal cancer: development and validation of a radiomics prediction model. Chin J Cancer Res 30(1):40–50
Author information
Authors and Affiliations
Contributions
PL: analysis and interpretation of the data, drafting of the manuscript; AL: study conception and design; HL: acquisition of the data; RW: acquisition of the data; GS: critical revision; RZ: analysis and interpretation of the data; and PZ: analysis and interpretation of the data.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflicts of interest.
Ethical approval
All procedures performed in studies involving human participants were approved by the Ethics Commission of the Shandong Provincial Qianfoshan Hospital of Shandong University.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Li, P., Song, G., Wu, R. et al. Multiparametric MRI-based machine learning models for preoperatively predicting rectal adenoma with canceration. Magn Reson Mater Phy 34, 707–716 (2021). https://doi.org/10.1007/s10334-021-00915-2
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10334-021-00915-2