Abstract
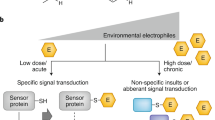
The aromatic hydrocarbon receptor (AhR) had been described as a molecular sensor to which many environmental pollutants, such as polycyclic aromatic hydrocarbons (PAHs) and halogenated aromatic hydrocarbons (HAHs) binds leading to many biological and toxic effects. Recently, it had been demonstrated that the differentiation of CD4+ T cells is influenced by AhR ligands present in the surrounding microenvironment of the cells. In this study, we assessed the immune environment of CD4+ T cells in a cohort of firefighters, a group of individuals more exposed to AhR ligands. Our results showed that in firefighters, Th17 and Treg cells were increased compared to our control group. Also, the microenvironment presents an increase in cytokines promoting the differentiation of these cells in firefighters. The presence of a large number of AhR ligands in the firefighters' sera had been observed. Finally, in vitro treatments of CD4+ T cells with AhR ligands (BaP and Kynurenine) had shown an ability to modulate Treg and Th17 cells' differentiation.







Similar content being viewed by others
Abbreviations
- AhR:
-
Aryl hydrocarbon receptor
- AhRR:
-
Aryl hydrocarbon receptor repressor
- ALD:
-
Alcohol dehydrogenase
- APC:
-
Antigen-presenting cell
- ARNT:
-
Aryl hydrocarbon receptor nuclear translocator
- BaP:
-
Benzo(a)pyrene
- BATF:
-
Basic leucine zipper transcription factor, ATF-like
- bHLH–PAS:
-
Basic helix-loop-helix Per-ARNT-Sim
- Bili:
-
Bilirubin
- CARS:
-
Compensatory anti-inflammatory response syndrome
- MHC:
-
Major histocompatibility complex
- CYP450:
-
Cytochrome P450
- DMBA:
-
7,12-Dimethylbenz(a)anthracene
- DRE:
-
Dioxin response element
- EGFR:
-
Epidermal growth factor receptor
- FBS:
-
Fetal bovine serum
- FICZ:
-
6-Formylindolo[3,2-b]carbazole
- Foxp3:
-
Forkhead box P3
- GATA-3:
-
GATA-3 binding protein
- GST:
-
Glutathione S-transferase
- GVH:
-
Graft versus host
- HAH:
-
Halogenated aromatic hydrocarbon
- PAH:
-
Polycyclic aromatic hydrocarbon
- Hsp90:
-
Heat shock protein 90
- I3C:
-
Indole-3-carbinol
- IFNγ:
-
Interferon gamma
- IL:
-
Interleukin
- IRF4:
-
Interferon regulatory factor 4
- Kyn:
-
Kynurenine
- KMO:
-
Kynurenine 3-monooxygenase
- LT:
-
T lymphocyte
- MODS:
-
Multiple organ dysfunction syndrome
- NES:
-
Nuclear export signal
- NF-κB:
-
Nuclear factor-kappa B
- NK:
-
Natural killer
- NLS:
-
Nuclear localization signal
- NQO:
-
NADH-quinone oxidoreductase
- PBMC:
-
Peripheral blood mononuclear cells
- RORγt:
-
RAR-related orphan receptor gamma
- SIRS:
-
Systemic inflammatory response syndrome
- T-bet:
-
T-box transcription factor
- TAD:
-
Trans-activating domain
- Tc:
-
Cytotoxic T cell
- TCDD:
-
2,3,7,8-Tétrachlorodibenzo-p-dioxin
- TGFβ:
-
Transforming growth factor beta
- Th:
-
T helper cell
- TNF:
-
Tumor necrosis factor
- Treg:
-
Regulatory T cell
- UGT:
-
Urdine triphosphate glucuronosyl transférase
- VAF347:
-
(4-(3-Chloro-phenyl)-pyrimidin-2-yl)-(4-trifluoromethyl-phenyl)-amine
- XRE:
-
Xenobiotic response element
References
Adeegbe DO, Nishikawa H (2013) Natural and induced T regulatory cells in cancer. Front Immunol 4:190. https://doi.org/10.3389/fimmu.2013.00190
Anderson DA, Harrison TR, Yang F, Wendorf Muhamad J, Morgan SE (2017) Firefighter perceptions of cancer risk: results of a qualitative study. Am J Ind Med 60(7):644–650. https://doi.org/10.1002/ajim.22726
Andersen MHG, Saber AT, Pedersen JE et al (2018) Assessment of polycyclic aromatic hydrocarbon exposure, lung function, systemic inflammation, and genotoxicity in peripheral blood mononuclear cells from firefighters before and after a work shift. Environ Mol Mutagen 59(6):539–548. https://doi.org/10.1002/em.22193
Bedoya SK, Lam B, Lau K, Larkin J 3rd (2013) Th17 cells in immunity and autoimmunity. Clin Dev Immunol 2013:986789. https://doi.org/10.1155/2013/986789
Bogdan C, Schleicher U (2006) Production of interferon-gamma by myeloid cells–fact or fancy? Trends Immunol 27(6):282–290. https://doi.org/10.1016/j.it.2006.04.004
Broere F, Apasov SG, Sitkovsky MV, van Eden W (2011) T cell subsets and T cell-mediated immunity. Principles of immunopharmacology. Springer, Cham, pp 15–27
Cella M, Fuchs A, Vermi W et al (2009) A human natural killer cell subset provides an innate source of IL-22 for mucosal immunity. Nature 457(7230):722–725. https://doi.org/10.1038/nature07537
Chen K, Kolls JK (2017) Interluekin-17A (IL17A). Gene. https://doi.org/10.1016/j.gene.2017.01.016
Dixon BR, Radin JN, Piazuelo MB, Contreras DC, Algood HM (2016) IL-17a and IL-22 induce expression of antimicrobials in gastrointestinal epithelial cells and may contribute to epithelial cell defense against helicobacter pylori. PLoS ONE 11(2):e0148514. https://doi.org/10.1371/journal.pone.0148514
Ehrlich AK, Pennington JM, Bisson WH, Kolluri SK, Kerkvliet NI (2018) TCDD, FICZ, and other high affinity AhR ligands dose-dependently determine the fate of CD4+ t cell differentiation. Toxicol Sci 161(2):310–320. https://doi.org/10.1093/toxsci/kfx215
Esser C, Rannug A, Stockinger B (2009) The aryl hydrocarbon receptor in immunity. Trends Immunol 30(9):447–454. https://doi.org/10.1016/j.it.2009.06.005
Fang D, Zhu J (2020) Molecular switches for regulating the differentiation of inflammatory and IL-10-producing anti-inflammatory T-helper cells. Cell Mol Life Sci 77(2):289–303. https://doi.org/10.1007/s00018-019-03277-0
Fent KW, Eisenberg J, Snawder J et al (2014) Systemic exposure to PAHs and benzene in firefighters suppressing controlled structure fires. Ann Occup Hyg 58(7):830–845. https://doi.org/10.1093/annhyg/meu036
Fent KW, Toennis C, Sammons D et al (2020) Firefighters’ absorption of PAHs and VOCs during controlled residential fires by job assignment and fire attack tactic. J Expo Sci Environ Epidemiol 30(2):338–349. https://doi.org/10.1038/s41370-019-0145-2
Flaveny CA, Perdew GH (2009) Transgenic humanized AHR mouse reveals differences between human and mouse AHR ligand selectivity. Mol Cell Pharmacol 1(3):119–123. https://doi.org/10.4255/mcpharmacol.09.15
Fossiez F, Djossou O, Chomarat P et al (1996) T cell interleukin-17 induces stromal cells to produce proinflammatory and hematopoietic cytokines. J Exp Med 183(6):2593–2603. https://doi.org/10.1084/jem.183.6.2593
Gasiewicz TA, Geiger LE, Rucci G, Neal RA (1983) Distribution, excretion, and metabolism of 2,3,7,8-tetrachlorodibenzo-p-dioxin in C57BL/6J, DBA/2J, and B6D2F1/J mice. Drug Metab Dispos 11(5):397–403
Guillon A, Le Ménach K, Flaud PM, Marchand N, Budzinski H, Villenave E (2013) Chemical characterization and stable carbon isotopic composition of particulate polycyclic aromatic hydrocarbons issued from combustion of 10 mediterranean woods. Atmos Chem Phys 13(5):2703–2719. https://doi.org/10.5194/acp-13-2703-2013
Hahn ME (2002) Aryl hydrocarbon receptors: diversity and evolution. Chem Biol Interact 141(1–2):131–160. https://doi.org/10.1016/s0009-2797(02)00070-4
Hayes MD, Ovcinnikovs V, Smith AG, Kimber I, Dearman RJ (2014) The aryl hydrocarbon receptor: differential contribution to T helper 17 and T cytotoxic 17 cell development. PLoS ONE 9(9):e106955. https://doi.org/10.1371/journal.pone.0106955
Hockley SL, Arlt VM, Brewer D et al (2007) AHR- and DNA-damage-mediated gene expression responses induced by benzo(a)pyrene in human cell lines. Chem Res Toxicol 20(12):1797–1810. https://doi.org/10.1021/tx700252n
Ifegwu OC, Anyakora C (2015) Polycyclic aromatic hydrocarbons: part I. Exposure. Adv Clin Chem 72:277–304. https://doi.org/10.1016/bs.acc.2015.08.001
Iwata S, Mikami Y, Sun HW et al (2017) The transcription factor T-bet limits amplification of type I IFN transcriptome and circuitry in T helper 1 cells. Immunity 46(6):983–991. https://doi.org/10.1016/j.immuni.2017.05.005
Jensen BA, Leeman RJ, Schlezinger JJ, Sherr DH (2003) Aryl hydrocarbon receptor (AhR) agonists suppress interleukin-6 expression by bone marrow stromal cells: an immunotoxicology study. Environ Health 2(1):16. https://doi.org/10.1186/1476-069X-2-16
Kourilsky P, Truffa-Bachi P (2001) Cytokine fields and the polarization of the immune response. Trends Immunol 22(9):502–509. https://doi.org/10.1016/s1471-4906(01)02012-9
Liu J, Zhang L, Winterroth LC et al (2013) Epigenetically mediated pathogenic effects of phenanthrene on regulatory T cells. J Toxicol 2013:967029. https://doi.org/10.1155/2013/967029
Lu L, Barbi J, Pan F (2017) The regulation of immune tolerance by FOXP3. Nat Rev Immunol 17(11):703–717. https://doi.org/10.1038/nri.2017.75
Luci C, Reynders A, Ivanov II et al (2009) Influence of the transcription factor RORgammat on the development of NKp46+ cell populations in gut and skin. Nat Immunol 10(1):75–82. https://doi.org/10.1038/ni.1681
Luzardo OP, Badea M, Zumbado M et al (2019) Body burden of organohalogenated pollutants and polycyclic aromatic hydrocarbons in Romanian population: influence of age, gender, body mass index, and habitat. Sci Total Environ 656:709–716. https://doi.org/10.1016/j.scitotenv.2018.11.404
Mezrich JD, Fechner JH, Zhang X, Johnson BP, Burlingham WJ, Bradfield CA (2010) An interaction between kynurenine and the aryl hydrocarbon receptor can generate regulatory T cells. J Immunol (Baltimore, Md: 1950) 185(6):3190–3198. https://doi.org/10.4049/jimmunol.0903670
Mukai M, Tischkau SA (2007) Effects of tryptophan photoproducts in the circadian timing system: searching for a physiological role for aryl hydrocarbon receptor. Toxicol Sci 95(1):172–181. https://doi.org/10.1093/toxsci/kfl126
Nebert DW (2017) Aryl hydrocarbon receptor (AHR): “pioneer member” of the basic-helix/loop/helix per-Arnt-sim (bHLH/PAS) family of “sensors” of foreign and endogenous signals. Prog Lipid Res 67:38–57. https://doi.org/10.1016/j.plipres.2017.06.001
Nguyen LP, Bradfield CA (2008) The search for endogenous activators of the aryl hydrocarbon receptor. Chem Res Toxicol 21(1):102–116. https://doi.org/10.1021/tx7001965
Nishikawa H (2014) Regulatory T cells in cancer immunotherapy. Rinsho Ketsueki 55(10):2183–2189
Ohtake F, Baba A, Fujii-Kuriyama Y, Kato S (2008) Intrinsic AhR function underlies cross-talk of dioxins with sex hormone signalings. Biochem Biophys Res Commun 370(4):541–546. https://doi.org/10.1016/j.bbrc.2008.03.054
Oreja-Guevara C, Ramos-Cejudo J, Aroeira LS, Chamorro B, Diez-Tejedor E (2012) TH1/TH2 cytokine profile in relapsing-remitting multiple sclerosis patients treated with glatiramer acetate or natalizumab. BMC Neurol 12:95. https://doi.org/10.1186/1471-2377-12-95
Ouyang B, Baxter CS, Lam HM et al (2012) Hypomethylation of dual specificity phosphatase 22 promoter correlates with duration of service in firefighters and is inducible by low-dose benzo[a]pyrene. J Occup Environ Med 54(7):774–780. https://doi.org/10.1097/JOM.0b013e31825296bc
Phelan D, Winter GM, Rogers WJ, Lam JC, Denison MS (1998) Activation of the Ah receptor signal transduction pathway by bilirubin and biliverdin. Arch Biochem Biophys 357(1):155–163. https://doi.org/10.1006/abbi.1998.0814
Quintana FJ, Basso AS, Iglesias AH et al (2008) Control of T(reg) and T(H)17 cell differentiation by the aryl hydrocarbon receptor. Nature 453(7191):65–71. https://doi.org/10.1038/nature06880
Rocuts F, Zhang X, Yan J et al (2010) Bilirubin promotes de novo generation of T regulatory cells. Cell Transplant 19(4):443–451. https://doi.org/10.3727/096368909X484680
Sakaguchi S, Yamaguchi T, Nomura T, Ono M (2008) Regulatory T cells and immune tolerance. Cell 133(5):775–787. https://doi.org/10.1016/j.cell.2008.05.009
Salimi Elizei S, Poormasjedi-Meibod MS, Wang X, Kheirandish M, Ghahary A (2017) Kynurenic acid downregulates IL-17/1L-23 axis in vitro. Mol Cell Biochem 431(1–2):55–65. https://doi.org/10.1007/s11010-017-2975-3
Sallusto F (2016) Heterogeneity of human CD4(+) T cells against microbes. Annu Rev Immunol 34:317–334. https://doi.org/10.1146/annurev-immunol-032414-112056
Schulze-Koops H, Kalden JR (2001) The balance of Th1/Th2 cytokines in rheumatoid arthritis. Best Pract Res Clin Rheumatol 15(5):677–691. https://doi.org/10.1053/berh.2001.0187
Shah K, Lee WW, Lee SH et al (2010) Dysregulated balance of Th17 and Th1 cells in systemic lupus erythematosus. Arthritis Res Ther 12(2):R53. https://doi.org/10.1186/ar2964
Shao S, Yu X, Shen L (2018) Autoimmune thyroid diseases and Th17/Treg lymphocytes. Life Sci 192:160–165. https://doi.org/10.1016/j.lfs.2017.11.026
Shin JH, Zhang L, Murillo-Sauca O et al (2013) Modulation of natural killer cell antitumor activity by the aryl hydrocarbon receptor. Proc Natl Acad Sci USA 110(30):12391–12396. https://doi.org/10.1073/pnas.1302856110
Simoneit BRT (2002) Biomass burning—a review of organic tracers for smoke from incomplete combustion. Appl Geochem 17(3):129–162. https://doi.org/10.1016/S0883-2927(01)00061-0
Spencer LA, Weller PF (2010) Eosinophils and Th2 immunity: contemporary insights. Immunol Cell Biol 88(3):250–256. https://doi.org/10.1038/icb.2009.115
Stephens GL, Wang Q, Swerdlow B, Bhat G, Kolbeck R, Fung M (2013) Kynurenine 3-monooxygenase mediates inhibition of Th17 differentiation via catabolism of endogenous aryl hydrocarbon receptor ligands. Eur J Immunol 43(7):1727–1734. https://doi.org/10.1002/eji.201242779
Stevens EA, Mezrich JD, Bradfield CA (2009) The aryl hydrocarbon receptor: a perspective on potential roles in the immune system. Immunology 127(3):299–311. https://doi.org/10.1111/j.1365-2567.2009.03054.x
Sugita S, Kawazoe Y, Imai A et al (2013) Role of IL-22- and TNF-alpha-producing Th22 cells in uveitis patients with Behcet’s disease. J Immunol 190(11):5799–5808. https://doi.org/10.4049/jimmunol.1202677
Tajima H, Tajiki-Nishino R, Watanabe Y, Fukuyama T (2019) Direct activation of aryl hydrocarbon receptor by benzo[a]pyrene elicits T-helper 2-driven proinflammatory responses in a mouse model of allergic dermatitis. J Appl Toxicol 39(7):936–944. https://doi.org/10.1002/jat.3782
Takatori H, Kanno Y, Watford WT et al (2009) Lymphoid tissue inducer-like cells are an innate source of IL-17 and IL-22. J Exp Med 206(1):35–41. https://doi.org/10.1084/jem.20072713
Trikha P, Lee DA (2020) The role of AhR in transcriptional regulation of immune cell development and function. Biochim Biophys Acta Rev Cancer 1873(1):188335. https://doi.org/10.1016/j.bbcan.2019.188335
Trinchieri G (2007) Interleukin-10 production by effector T cells: Th1 cells show self control. J Exp Med 204(2):239–243. https://doi.org/10.1084/jem.20070104
Veldhoen M, Hirota K, Westendorf AM et al (2008) The aryl hydrocarbon receptor links TH17-cell-mediated autoimmunity to environmental toxins. Nature 453(7191):106–109. https://doi.org/10.1038/nature06881
Wang Y, Pan T, Li L, Wang H, Zhang D, Yang H (2018) Benzo(a)pyrene promotes Hep-G2 cell migration and invasion by upregulating phosphorylated extracellular signal-regulated kinase expression. Oncol Lett 15(6):8325–8332. https://doi.org/10.3892/ol.2018.8379
Wei Y, Zhao L, He W et al (2016) Benzo[a]pyrene promotes gastric cancer cell proliferation and metastasis likely through the Aryl hydrocarbon receptor and ERK-dependent induction of MMP9 and c-myc. Int J Oncol 49(5):2055–2063. https://doi.org/10.3892/ijo.2016.3674
Wheeler JL, Martin KC, Resseguie E, Lawrence BP (2014) Differential consequences of two distinct AhR ligands on innate and adaptive immune responses to influenza A virus. Toxicol Sci 137(2):324–334. https://doi.org/10.1093/toxsci/kft255
Yeh N, Glosson NL, Wang N et al (2010) Tc17 cells are capable of mediating immunity to vaccinia virus by acquisition of a cytotoxic phenotype. J Immunol 185(4):2089–2098. https://doi.org/10.4049/jimmunol.1000818
Youakim S (2006) Risk of cancer among firefighters: a quantitative review of selected malignancies. Arch Environ Occup Health 61(5):223–231. https://doi.org/10.3200/AEOH.61.5.223-231
Zhao Y, Han P, Liu L et al (2019) Indirubin modulates CD4(+) T-cell homeostasis via PD1/PTEN/AKT signalling pathway in immune thrombocytopenia. J Cell Mol Med 23(3):1885–1898. https://doi.org/10.1111/jcmm.14089
Zhou L (2016) AHR function in lymphocytes: emerging concepts. Trends Immunol 37(1):17–31. https://doi.org/10.1016/j.it.2015.11.007
Zhu J, Yamane H, Cote-Sierra J, Guo L, Paul WE (2006) GATA-3 promotes Th2 responses through three different mechanisms: induction of Th2 cytokine production, selective growth of Th2 cells and inhibition of Th1 cell-specific factors. Cell Res 16(1):3–10. https://doi.org/10.1038/sj.cr.7310002
Acknowledgements
The authors would like to thank the volunteers who participated in this study as well as nurse Alexandre Arsenault.
Author information
Authors and Affiliations
Contributions
JB conceived the study; GR, DL, and JB designed the study; GR and DL performed the experiments; GR, DL, and JB analyzed, interpreted the data, and wrote the paper; JB supervised the study.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no conflicts of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Ricaud, G., Lim, D. & Bernier, J. Environmental Exposition to Aromatic Hydrocarbon Receptor Ligands Modulates the CD4+ T Lymphocyte Subpopulations Profile. Expo Health 13, 307–322 (2021). https://doi.org/10.1007/s12403-021-00385-w
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12403-021-00385-w