Abstract
Introduction
Despite the fact that sexual and reproductive health has been considered key aspects of the individual’s wellbeing and social welfare, there are no adequate policies and programs to deal with sexual health, particularly among young people.
Methods
A qualitative study was conducted from February to December 2015. Twenty-five semi-structured in-depth interviews were conducted with health policymakers in Iran using a purposive sampling method. The qualitative data were analyzed using conventional content analysis with an inductive interpretive approach.
Results
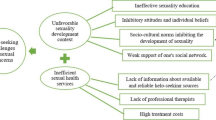
The perceived barriers for sexual health programs generated by health-policymakers reside in three main domains: individual, structural, and socio-cultural. Under the domain of individual, the category of policymakers’ personal barriers comprises: “lack of knowledge,” “misperceptions,” and “stigma,” i.e., threat to their managerial positions. Under the domain of structural barriers, the category of “challenges in policy making processes” comprises: “the abstinence challenge/paradox of sexual health as a strategic goal,” “financial challenges,” “uncoordinated and unstable management of the program,” “challenges for data collection and planning,” and “lack of priority for sexual health.” Finally, under the domain of socio-cultural, the category of “conservative socio-cultural context, sexuality as a social taboo in Iranian society” emerged as a barrier for sexual health programs in Iran.
Conclusions
To introduce sexual health programs in a conservative society, health-policymakers must begin by advocating for sexual health, in order to create positive attitudes toward sexual heath as a component of human wellbeing, and then address social and cultural sensitivities by promoting greater dialogue.
Social and Public Policy Implications
Sexual health and sexual health needs are important aspects of life and warrant further research in Iran. Policy makers of the health system need to correct information of sexual health needs of people to health planning, and this clears barriers of sexual health planning in the health system of Iran.
Similar content being viewed by others
Availability of Data and Material
Data are available on request only, owing to privacy concerns and other restrictions.
Change history
09 April 2021
A Correction to this paper has been published: https://doi.org/10.1007/s13178-021-00583-w
Abbreviations
- SRH:
-
Sexual and reproductive health
- HIV/AIDS:
-
Human immunodeficiency virus infection and acquired immune deficiency syndrome
- PWIDs:
-
People who inject drugs
- DIC:
-
Drop in centers
- MOHME:
-
Ministry of Health and Medical Education
- MAXQDA:
-
MAX Qualitative Data Analysis (MAX is a name)
References
Alomair, N., Alageel, S., Davies, N., & Bailey, J. V. (2020). Factors influencing sexual and reproductive health of Muslim women: A systematic review. Reproductive Health, 17, 33.
Baraitser, P., & Wood, A. (2001). Precarious partnerships: barriers to multidisciplinary sex education in schools - a short communication. Health Education Journal, 60, 127–131.
Bhattacherjee, A. (2012). Social Science Research: Principles, Methods, and Practices. Scholar Commons.
Bostani Khalesi, Z., Simbar, M., & Azin, S. A. (2017). A qualitative study of sexual health education among Iranian engaged couples. African Health Sciences, 17, 382–390.
Ciarrochi, J., Mayer, J. D. (2007). Applying emotional intelligence: A practitioner’s guide. Psychology Press, 186–201.
Daviter, F. (2015). The political use of knowledge in the policy process. Policy Sciences, 48, 491–505.
DeJong, J., Jawad, R., Mortagy, I., & Shepard, B. (2005). The sexual and reproductive health of young people in the Arab countries and Iran. Reproductive Health Matters, 13, 49–59.
Ezeh, A., Bankole, A., Cleland, J., García-Moreno, C., Temmerman, M., & Ziraba, A. (2016). Reproductive, maternal, newborn, and child health: disease control priorities. The International Bank for Reconstruction and Development / The World Bank.
Esmaili, M. R., & Amiri, Z. (2016). The impact of shared leadership on talent management C. management studies in development & evaluation. Management Studies, 25, 47–64.
Elmir, R., Schmied, V., Jackson, D., & Wilkes, L. (2011). Interviewing people about potentially sensitive topics. Nurse Researcher, 19, 12–16.
Friães dos Santos, J. P., Martins Pires, A. M., & Fernandes, P. O. (2018). The importance to financial information in the decision-making process in company’s family structure. Contaduría y Administración, Accounting and Management, 63, 35–36.
Frost, D. M. (2011). Social stigma and its consequences for the socially stigmatized. Social and Personality Psychology Compass, 5, 824–839.
Freud, S. (1913). Totem and Taboo.
Gheshlaghi, F., Dorvashi, G., Aran, F., Shafiei, F., & Montazeri Najafabadi, G. (2014). The study of Sexual satisfaction in Iranian women applying for divorce. International Journal of Fertility & Sterility, 8, 281–288.
Graneheim, U. H., & Lundman, B. (2004). Qualitative content analysis in nursing research: concepts, procedures and measures to achieve trustworthiness. Nurse Education Today, 24, 105–112.
Gruskin, S. (2008). Reproductive and sexual rights: Do words matter? American Journal of Public Health, 98, 1737.
Guba, E. G., & Lincoln, Y. S. (1994). Competing paradigms in qualitative research. In N. K. Denzin & Y. S. Lincoln (Eds.), Handbook of qualitative research (p. 105–117). Sage Publications, Inc.
Javadnoori, M., Latifnejad Roudsari, R., Hasanpour, M., Hazavehei, S. M. M., & Taghipour, A. (2012). Female adolescents’ experiences and perceptions regarding sexual health education in Iranian schools: A qualitative content analysis. Iran J Nurs Midwifery Res, 17, 539–546.
Joulaei, H., Lankarani, K. B., & Shahbazi, M. (2012). Iranian and American health professionals working together to address health disparities in Mississippi Delta based on Iran’s health house model. Archives of Iranian Medicine, 15, 378–380.
Khalajabadi Farahani, F., & Cleland, J. (2015). Perceived norms of premarital heterosexual relationships and sexuality among female college students in Tehran. Culture, Health & Sexuality: An International Journal for Research, Intervention and Care, 17, 700–717.
Larson, J. E., & Corrigan, P. (2008). The stigma of families with mental illness. Academic Psychiatry, 32, 87–91.
Ministry of Health and Medical Education of Islamic Republic of Iran (MOHME). (2015). AIDS Progress Report on Monitoring of the United Nations General Assembly Special Session on HIV and AIDS. National AIDS Committee Secretariat.
Motamedi, M., Merghati-Khoei, E., Shahbazi, M., Rahimi-Naghani, S. H., Salehi, M., & Khalajabadi-Farahani, F. (2016). Paradoxical attitudes toward premarital dating and sexual encounters in Tehran, Iran: a cross-sectional study. Reproductive Health, 13, 102.
Motamedi, M., Merghati-Khoei, E., Salehi, M., Khalajabadi-Farahani, F., & Hajebi, A. (2016). Evaluation of sexual health programs in health system: Gap analysis. Isfahan University of Medical Sciences.
Moradi, G., Piroozi, B., Alinia, C., Akbarpour, S., Gouya, M. M., & Kazaerooni, P. A. (2019). Incidence, mortality, and burden of HIV/AIDS and its geographical distribution in Iran during 2008–2016. Iran Journal of Public Health, 48, 1–9.
Noori, A., Rahimzadeh, Sh., Shahbazi, M., Moradi, G., Saeedi Moghaddam, S., & Shokoohi, M. (2016). The burden of HIV in Iran: Insights from the global burden of disease study 2010. Archives of Iranian Medicine, 19, 329–334.
Quinn, N., & Knifton, L. (2014). Beliefs, stigma and discrimination associated with mental health problems in Uganda: Implications for theory and practice. International Journal of Social Psychiatry, 60, 554–561.
Rahimi-Naghani, S., Merghati-Khoei, E., Shahbazi, M., Khalajabadi Farahani, F., & Motamedi, M. (2016). Sexual and reproductive health knowledge among men and women aged 15 to 49 years in metropolitan Tehran. The Journal of Sex Research, 53, 1153–1164.
Rashidi, H. B., Kiyani, K., & Shahbazi, S. S. (2015). Sexual health definition from the perspective of Iranian experts and description its components. Tehran University Medical Journal, 73, 210–220.
Salo, N. (2009). The implications of knowledge management sustainability for leadership in an organization: An exploration and analysis of leadership theories and knowledge managment practices in Bangwita Flores. Indonesia. The Interdisciplinary Journal of NTT Development Studies, 1, 95–135.
Sex Information and & Education Council of Canada (Sieccan). (2019). Canadian guidelines for sexual health education. Public Health Agency of Canada. Retrieved from ISBN: 978-0-662-48083-9, www.publichealth.gc.ca/sti.
Shariati, M., & Babazadeh., R., Mousavi, S. A., & Mirzaii-Najmabadi, K. . (2014). Iranian adolescent girls’ barriers in accessing sexual and reproductive health information and services: a qualitative study. The Journal of Family Planning and Reproductive Health Care, 40, 270–275.
Shirpak, K. R., Chinichian, M., Maticka-Tyndale, E., Ardebili, H. E., & Pourreza Ramenzankhani, A. (2008). A qualitative assessment of the sex education needs of married Iranian women. Sexuality Culture, 12, 133–150.
Singh, S., Darroch, E. J., & Ashford, D. L. (2014). ADDING IT UP: The cost and benefits of investing in sexual and reproductive health 2014. UNFPA, Guttmacher Institute. Retrieved from ISBN: 978-1-934387-18-4.
Smith, T., McNeil, K., Mitchell, R., Boyle, B., & Ries, N. (2019). A study of macro-, meso- and micro-barriers and enablers affecting extended scopes of practice: The case of rural nurse practitioners in Australia. BMC Nursing, 18, 14. https://doi.org/10.1186/s12912-019-0337-z.
Tabrizi, J. S., Poursaghar, F., & Gholamzade, N. R. (2017). Status of Iran’s primary health care system in terms of health systems. Iranian Journal of Public Health, 46, 1156–1166.
Taylor, A. W., Martin, G., Dal Grande, E., Swannell, S., Fullerton, S., Hazell, P., & Harrison, J. E. (2011). Methodological issues associated with collecting sensitive information over the telephone—Experience from an Australian non-suicidal self-injury (NSSI) prevalence study. BMC Medical Research Methodology, 11, 20.
Teimoori, V. (2012). A review of taboo in Iranian literature. Journal of Basic & Applied Sciences, 2, 7949–7955.
Turan, J. M., Elafros, M. A., Logie, C. H., Banik, S., Turan, B., & Murray, S. M. (2019). Challenges and opportunities in examining and addressing intersectional stigma and health. BMC Med, 17.
WHO. (2004). Reproductive health strategy to accelerate progress towards the attainment of international development goals and targets. Geneva: World Health Organization.
WHO. (2010). Developing sexual health programs: A framework for action. Geneva: World Health Organization.
WHO. (2017). Sexual health and its linkages to reproductive health: an operational approach. Geneva: World Health Organization.
Yari, F., Moghadam, Z., Parvizi, S., Nayeri, N., & Rezaei, E. (2015). Sexual and reproductive health problems of female university students in Iran: A qualitative study. Global Journal of Health Science, 7, 278.
Yarmohammadian, M. H., & Bahrami, S. (2006). Needs assessment in health and educational organizations health system planning needs assessment principles - Needs assessment patterns and techniques. Health Management, 20, 61–67.
Yazdkhasti, M., Pourreza, A., Pirak, A., & Abdi, F. (2015). Unintended pregnancy and its adverse social and economic consequences on health system: A narrative review article. Iranian Journal of Public Health, 44, 12–21.
Zelman, W. N., McCue, M. J., Millikan, A. R., & Glick, N. D. (2009). Financial management of health care organizations: An introduction to fundamental tools, concepts, and applications. John Wiley & Sons: Blackwell Publishing.
Acknowledgements
The authors are indebted to the members of the Ethics Committee of Isfahan University of Medical Sciences (reference: 393460). Our special thanks to Dr. Massoud Kamrava and J.M. Dormon for reviewing and editing the manuscript. We would like to express our gratitude to the study participants who shared their very personal information with us.
Author information
Authors and Affiliations
Contributions
MM designed and directed the study in all steps. MS, SS, and FK aided in analyzing work of the manuscript. MS, EM, and AH analyzed the data. KK and other authors discussed the results and commented on the manuscript.
Corresponding author
Ethics declarations
Ethics Approval
This study was approved by the ethical committee of the Isfahan University of Medical Sciences (reference: 393460). All participants were informed about the aim of the study and also were ensured about the confidentiality of their responses as well as voluntary participation, along with a verbal consent before the interviews were carried out.
Consent for Publication
All participants consented to the publication of this report before the interviews were carried out.
Competing Interests
The authors declare that they have no competing interests.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
The original version of this article unfortunately a mistake. The corresponding author should be Farideh Khalajabadi Farahani.
Rights and permissions
About this article
Cite this article
Motamedi, M., Shahbazi, M., Merghati-Khoei, E. et al. Perceived Barriers to Implementing Sexual Health Programs from the Viewpoint of Health Policymakers in Iran: A Qualitative Study. Sex Res Soc Policy 19, 273–285 (2022). https://doi.org/10.1007/s13178-021-00540-7
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13178-021-00540-7