Abstract
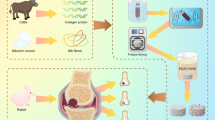
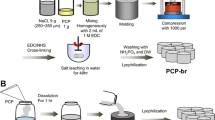
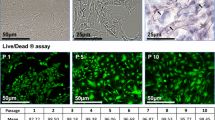
Engineered cartilage has several applications in treating cartilage ossification, however, its use is restricted clinically. We explored the feasibility of engineered cartilage in constructing tissues using gelatin/curcumin nano-fiber membranes as scaffolds in subcutaneous models. We constructed cartilage with gelatin nano-fiber membrane (control group) and gelatin/curcumin nano-fiber membrane (experimental group) as scaffolds. After the material was implanted into the back of BALB/c mice, gross view observation was performed. Histological examination was performed 3 and 12 weeks after implantation in vivo, and cartilage formation at different time points was compared. Gross observation showed that compared to the control group, the vascularization of nearby tissues in the experimental group was significantly inhibited. The Scanning electron microscope observation showed that the chondrocytes in both groups adhered well. The growth curve of the chondrocytes showed that curcumin had no significant effect on cell growth. Histological observation showed that the cell-material complexes in both groups had cartilage lacuna formation at 3 and 12 weeks. However, compared with that of the control group, the experimental group showed obvious absorption and thicker cartilage matrix with more homogenization. Gelatin/curcumin scaffolds were successfully used to construct engineered cartilage tissues in subcutaneous animal models. Our findings demonstrate that curcumin-loaded scaffolds have great clinical applications.








Similar content being viewed by others
References
Fan-Fan S, Zhang M-C (2008) Inhibitory effect of curcumin on rat corneal neovascularization. Int J Ophthalmol 8(9):1806–1808
Gao W, He Y-J, Liang F-M (2016) Advancement on effects of curcumin for molecular mechanism of anti-tumor-angiogenesis. Int Eye Sci 16(3):466–468
Gao W, Chen L-X, He Y-J et al (2017) Inhibitory effects of curcumin on vasculogenic mimicry in choroid melanoma cell line OCM-1 and its mechanisms. Recent Adv Ophthalmol 37(11):1018–1021
Han J-r, Zhang L-x et al (2013) Effect and mechanism of curcumin on antitumor. J Int Oncol 40(11):823–826
Huo Y, Zhou G, Zehng R (2017) The construction of tissue engineered cartilage by using GT/PCL nanofiberes membranes in porcine model. J Tissue Eng Reconstruct Surg 13(1):1–4
Ke J, Wang L et al (2011) A comparative study on bone marrow mesenchymal stem cells differentiated into chondrocytes induced by co-culture with chondrocytes and conditioned medium. J Clin Rehab Tissue Eng Res 15(19):3421–3426
Kusafuka K, Hiraki Y, Shukunami C et al (2002) Cartilage-specific matrix protein, chondromodulin-I (Chm-1), is a strong angio-inhibitor in endochondral ossification of human neonatal vertebral tissues in vivo: relationship with angiogenic factors in the cartilage. Acta Histochem 104(2):167–175
Pelttari K, Winter A, Steck E et al (2006) Premature induction of hypertrophy during in vitro chondrogenesis of human mesenchymal stem cells correlates with calcification and vascular invasion after ectopic transplantation in SCID mice. Arthritis Rheum 54(10):3254–3266
Shukunami C, Iyama K, Inoue H et al (1999) Spatiotemporal pattern of the mouse chondromodulin-I gene expression and its regulatory role in vascular invasion into cartilage during endochondral bone formation. Int J Dev Biol 43(1):39–49
Shukunami C, Takimoto A, Miura S et al (2008) Chondromodulin-I and tenomodulin are differentially expressed in the avascular mesenchyme during mouse and chick development. Cell Tissue Res 332(1):111–122
Song L, Baksh D, Tuan RS (2004) Mesenchymal stem cell-based cartilage tissue engineering: cells, scaffold and biology. Cytotherapy 6(6):596–601
Sun S, Yang D, Dai N et al (2017) Effect and mechanism of curcumin acetylsalicylate on angiotensin II induced proliferation in vascular smooth muscle cells. J Tradit Chin Med Univ Hunan 37(11):1222–1225
Wang X-q, Liang Z-q, Gu H-l et al (2004) Study on antiangiogenesis effects of curcumin. Suzhou Univ J Med Sci 24(3):277–279
Zehng R, Zhao S, Zhu Y et al (2017) The feasibility of the macroporous GT/PCL electrospun material as scaffold for cartilage tissue engineering. J Tissue Eng Reconstruct Surg 13(2):66–69
Zheng W, Yang X, Wu L (2007) Potential molecular mechanisms behind the anti-angiogenesis effects of Curcumin. Chin J Clin Oncol 34(12):683–685
Zhou G, Liu W, Cui L et al (2006) Repair of porcine articular osteochondral defects in non-weight bearing areas with autologous bone marrow stromal cells. Tissue Eng 12(11):3209–3221
Acknowledgements
This work was supported by National Natural Science Foundation of China (81871502), Youth program of National Natural Science Foundation of China(8180080719) and The National Key Research and Development Program of China (2017YFC1103900). The authors appreciate technical support and other assistance from Junming Lu, Xiansong Wang and Lijuan Zong.
Funding
All authors declare no competing financial interests.
Author information
Authors and Affiliations
Contributions
BkK contributed to the conception and design, follow-up and data collection, analysis and interpretation of data of this study and wrote this manuscript. ZY contributed to the conception and design, acquisition of data, analysis and interpretation of data of this study and the draft and revision of this manuscript for important intellectual content. WC, TJ, Y-hS, JG contributed to the acquisition of data of this study and revision of the article. GZ contributed to the analysis and interpretation of data of this study. DC contributed to the concept and design and acquisition of data of this study. All authors give final approval of this version to be published.
Corresponding authors
Ethics declarations
Conflict of interest
All authors declare that we have no conflicts of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Kang, B.K., Yu, Z., Chen, W. et al. Using gelatin/curcumin nano-fiber membranes as scaffolds in a subcutaneous model for tissue engineered cartilages. Cell Tissue Bank 22, 443–451 (2021). https://doi.org/10.1007/s10561-020-09892-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10561-020-09892-7