Abstract
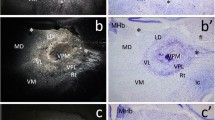
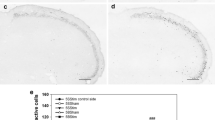
This study explores the involvement of substance P (SP) in the parabrachial nucleus (PBN) and central amygdaloid nucleus (CeA) in the nociception–emotion link and of rats with masticatory myofascial pain (MMP) induced by chronic tetanic eccentric muscle contraction. A total of 18 rats were randomly and equally assigned for MMP (MMP group) and sham-MMP induction (sMMP group). MMP was induced by electrical-stimulated repetitive tetanic eccentric contraction of the masseter muscle for 14 consecutive days. Myofascial trigger points in the masseter muscle were identified by palpable taut bands, increased prevalence of endplate noise (EPN), focal hypoechoic nodules on ultrasound and restricted jaw opening. All animals were killed for morphological and SP immunohistochemical analyses. Chronic tetanic eccentric contraction induced significantly thicker masseter muscle confirmed by hypoechogenicity, increased prevalence and amplitudes of EPN, and limited jaw opening. Immunohistochemically, the SP-like positive neurons increased significantly in PBN and CeA of the MMP group. Our results suggested that MMP increases the SP protein levels in PBN and CeA, which play important roles in MMP-mediated chronic pain processing as well as MMP-related emotional processes.





Similar content being viewed by others
References
Ballyns JJ, Shah JP, Hammond J, Gebreab T, Gerber LH, Sikdar S (2011) Objective sonographic measures for characterizing myofascial trigger points associated with cervical pain. J Ultrasound Med 30:1331–1340. https://doi.org/10.7863/jum.2011.30.10.1331
Bernard JF, Besson JM (1990) The spino(trigemino)pontoamygdaloid pathway: electrophysiological evidence for an involvement in pain processes. J Neurophysiol 63:473–490. https://doi.org/10.1152/jn.1990.63.3.473
Block CH, Hoffman G, Kapp BS (1989) Peptide-containing pathways from the parabrachial complex to the central nucleus of the amygdala. Peptides 10:465–471. https://doi.org/10.1016/0196-9781(89)90060-0
Bullitt E (1990) Expression of c-fos-like protein as a marker for neuronal activity following noxious stimulation in the rat. J Comp Neurol 296:517–530. https://doi.org/10.1002/cne.902960402
Chiang MC, Bowen A, Schier LA, Tupone D, Uddin O, Heinricher MM (2019) Parabrachial complex: a hub for pain and aversion. J Neurosci 39:8225–8230. https://doi.org/10.1523/jneurosci.1162-19.2019
Conti PC, Costa YM, Goncalves DA, Svensson P (2016) Headaches and myofascial temporomandibular disorders: overlapping entities, separate managements? J Oral Rehabil 43:702–715. https://doi.org/10.1111/joor.12410
Dam TV, Martinelli B, Quirion R (1990) Autoradiographic distribution of brain neurokinin-1/substance P receptors using a highly selective ligand [3H]-[Sar9, Met(O2)11]-substance P. Brain Res 531:333–337. https://doi.org/10.1016/0006-8993(90)90796-e
Ding YQ, Takada M, Shigemoto R, Mizuno N (1995) Trigeminoparabrachial projection neurons showing substance P receptor-like immunoreactivity in the rat. Neurosci Res 23:415–418. https://doi.org/10.1016/0168-0102(95)00961-r
Fernandez-de-Las-Penas C (2015) Myofascial head pain. Curr Pain Headache Rep 19:28. https://doi.org/10.1007/s11916-015-0503-2
Fibraio SJ, Finnegan M (2019) Masseter Muscle: Dental Drama. In: Donnelly JM (ed) Travell, Simons & Simons’ myofascial pain and dysfunction: the trigger point manual, 3rd edn. Wolters Kluwer Health, Philadelphia, pp 298–318
Fodor M, Gorcs TJ, Palkovits M (1992) Immunohistochemical study on the distribution of neuropeptides within the pontine tegmentum-particularly the parabrachial nuclei and the locus coeruleus of the human brain. Neuroscience 46:891–908. https://doi.org/10.1016/0306-4522(92)90192-5
Furquim BD, Flamengui LM, Conti PC (2015) TMD and chronic pain: a current view. Dent Press J Orthod 20:127–133. https://doi.org/10.1590/2176-9451.20.1.127-133.sar
Gauriau C, Bernard JF (2002) Pain pathways and parabrachial circuits in the rat. Exp Physiol 87:251–258. https://doi.org/10.1113/eph8702357
Glaros AG (2000) Emotional factors in temporomandibular joint disorders. J Indiana Dent Assoc 79:20–23
Hara K, Shinozaki T, Okada-Ogawa A et al (2016) Headache attributed to temporomandibular disorders and masticatory myofascial pain. J Oral Sci 58:195–204. https://doi.org/10.2334/josnusd.15-0491
Hocking MJ (2013) Exploring the central modulation hypothesis: do ancient memory mechanisms underlie the pathophysiology of trigger points? Curr Pain Headache Rep 17:347. https://doi.org/10.1007/s11916-013-0347-6
Hsieh YL, Chou LW, Joe YS, Hong CZ (2011) Spinal cord mechanism involving the remote effects of dry needling on the irritability of myofascial trigger spots in rabbit skeletal muscle. Arch Phys Med Rehabil 92:1098–1105. https://doi.org/10.1016/j.apmr.2010.11.018
Hutchins MO, Skjonsby HS, Brazeau GA, Parikh UK, Jenkins RM (1995) Weakness in mouse masticatory muscles by repetitive contractions with forced lengthening. J Dent Res 74:642–648. https://doi.org/10.1177/00220345950740020401
Jasmin L, Burkey AR, Card JP, Basbaum AI (1997) Transneuronal labeling of a nociceptive pathway, the spino-(trigemino-)parabrachio-amygdaloid, in the rat. J Neurosci 17:3751–3765
Kato F, Sugimura YK, Takahashi Y (2018) Pain-associated neural plasticity in the parabrachial to central amygdala circuit: pain changes the brain, and the brain changes the pain. Adv Exp Med Biol 1099:157–166. https://doi.org/10.1007/978-981-13-1756-9_14
Khasabov SG, Rogers SD, Ghilardi JR, Peters CM, Mantyh PW, Simone DA (2002) Spinal neurons that possess the substance P receptor are required for the development of central sensitization. J Neurosci 22:9086–9098
Kumbhare DA, Elzibak AH, Noseworthy MD (2016) Assessment of myofascial trigger points using ultrasound. Am J Phys Med Rehabil 95:72–80. https://doi.org/10.1097/phm.0000000000000376
Li H, Li YQ (2000) Collateral projection of substance P receptor expressing neurons in the medullary dorsal horn to bilateral parabrachial nuclei of the rat. Brain Res Bull 53:163–169. https://doi.org/10.1016/s0361-9230(00)00320-8
Manfredini D, Guarda-Nardini L, Winocur E, Piccotti F, Ahlberg J, Lobbezoo F (2011) Research diagnostic criteria for temporomandibular disorders: a systematic review of axis I epidemiologic findings. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 112:453–462. https://doi.org/10.1016/j.tripleo.2011.04.021
Mantyh PW, Hunt SP, Maggio JE (1984) Substance P receptors: localization by light microscopic autoradiography in rat brain using [3H]SP as the radioligand. Brain Res 307:147–165. https://doi.org/10.1016/0006-8993(84)90470-0
Miyazawa Y, Takahashi Y, Watabe AM, Kato F (2018) Predominant synaptic potentiation and activation in the right central amygdala are independent of bilateral parabrachial activation in the hemilateral trigeminal inflammatory pain model of rats. Mol Pain 14:1744806918807102. https://doi.org/10.1177/1744806918807102
Nazeri M, Ghahrechahi HR, Pourzare A et al (2018) Role of anxiety and depression in association with migraine and myofascial pain temporomandibular disorder. Indian J Dent Res 29:583–587. https://doi.org/10.4103/0970-9290.244932
Niddam DM, Chan RC, Lee SH, Yeh TC, Hsieh JC (2008) Central representation of hyperalgesia from myofascial trigger point. Neuroimage 39:1299–1306. https://doi.org/10.1016/j.neuroimage.2007.09.051
Qiao Y, Zhang CK, Li ZH, Niu ZH, Li J, Li JL (2019) Collateral projections from the lateral parabrachial nucleus to the central amygdaloid nucleus and the ventral tegmental area in the rat. Anat Rec (Hoboken) 302:1178–1186. https://doi.org/10.1002/ar.23983
Ren W, Neugebauer V (2010) Pain-related increase of excitatory transmission and decrease of inhibitory transmission in the central nucleus of the amygdala are mediated by mGluR1. Mol Pain 6:93. https://doi.org/10.1186/1744-8069-6-93
Saleh TM, Kombian SB, Zidichouski JA, Pittman QJ (1996) Peptidergic modulation of synaptic transmission in the parabrachial nucleus in vitro: importance of degradative enzymes in regulating synaptic efficacy. J Neurosci 16:6046–6055
Shah JP, Thaker N, Heimur J, Aredo JV, Sikdar S, Gerber L (2015) Myofascial trigger points then and now: a historical and scientific perspective. PM & R 7:746–761. https://doi.org/10.1016/j.pmrj.2015.01.024
Sikdar S, Shah JP, Gebreab T, Yen RH, Gilliams E, Danoff J, Gerber LH (2009) Novel applications of ultrasound technology to visualize and characterize myofascial trigger points and surrounding soft tissue. Arch Phys Med Rehabil 90:1829–1838. https://doi.org/10.1016/j.apmr.2009.04.015
Simons DG (2004) Review of enigmatic MTrPs as a common cause of enigmatic musculoskeletal pain and dysfunction. J Electromyogr Kinesiol 14:95–107. https://doi.org/10.1016/j.jelekin.2003.09.018
Simons DG, Hong CZ, Simons LS (1995) Prevalence of spontaneous electrical activity at trigger spots and at control sites in rabbit skeletal muscle. J Musculoskelet Pain 3:35–48
Simons DG, Hong CZ, Simons LS (2002) Endplate potentials are common to midfiber myofacial trigger points. Am J Phys Med Rehabil 81:212–222. https://doi.org/10.1097/00002060-200203000-00010
Thomas K, Shankar H (2013) Targeting myofascial taut bands by ultrasound. Curr Pain Headache Rep 17:349. https://doi.org/10.1007/s11916-013-0349-4
Turo D, Otto P, Shah JP et al (2012) Ultrasonic tissue characterization of the upper trapezius muscle in patients with myofascial pain syndrome. Conf Proc IEEE Eng Med Biol Soc 2012:4386–4389. https://doi.org/10.1109/embc.2012.6346938
Uddin O, Studlack P, Akintola T, Raver C, Castro A, Masri R, Keller A (2018) Amplified parabrachial nucleus activity in a rat model of trigeminal neuropathic pain. Neurobiol Pain 3:22–30. https://doi.org/10.1016/j.ynpai.2018.02.002
Yamano M, Hillyard CJ, Girgis S, MacIntyre I, Emson PC, Tohyama M (1988) Presence of a substance P-like immunoreactive neurone system from the parabrachial area to the central amygdaloid nucleus of the rat with reference to coexistence with calcitonin gene-related peptide. Brain Res 451:179–188. https://doi.org/10.1016/0006-8993(88)90762-7
Younger JW, Shen YF, Goddard G, Mackey SC (2010) Chronic myofascial temporomandibular pain is associated with neural abnormalities in the trigeminal and limbic systems. Pain 149:222–228. https://doi.org/10.1016/j.pain.2010.01.006
Zimmermann M (1983) Ethical guidelines for investigations of experimental pain in conscious animals. Pain 16:109–110
Zimmermann M (1986) Ethical considerations in relation to pain in animal experimentation. Acta Physiol Scand Suppl 554:221–233
Funding
This work was financially supported by the Ministry of Science and Technology, Taiwan [Grant number: 107-2314-B-039-035] and China Medical University [Grant number: CMU108-MF-99].
Author information
Authors and Affiliations
Contributions
Conceptualization: Y-LH; methodology: Y-LH; formal analysis and investigation: B-TW and C-CY; writing—original draft preparation: Y-LH; writing—review and editing: C-CY; funding acquisition: Y-LH; resources: Ministry of Science and Technology, Taiwan; supervision: Y-LH.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest.
Additional information
Communicated by Bill J. Yates.
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Hsieh, YL., Wu, BT. & Yang, CC. Increased substance P-like immunoreactivities in parabrachial and amygdaloid nuclei in a rat model with masticatory myofascial pain. Exp Brain Res 238, 2845–2855 (2020). https://doi.org/10.1007/s00221-020-05942-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00221-020-05942-4