Abstract
Human usually uses oximes as acetylcholinesterase (AChE)-activated antidotes to treat organophosphorus (OP) compound poisoning. In addition, drugs such as atropine can also be used for its detoxification treatment. However, the natural blood-brain barrier (BBB) severely limits the penetration of these drugs into the central nervous system. As a widely used reactivator, HI-6 is difficult to penetrate the BBB due to its hydrophilicity. Therefore, we hope that a large amount of HI-6 can penetrate the BBB through the drug delivery system. They can quickly release and activate the inhibited AChE in the center. Polybutylcyanoacrylate (PBCA) has good biodegradability and biocompatibility, which ensures the safety of the treatment. Pluronic P85 gets the advantages of inhibiting P-glycoprotein (P-gp) efflux and improving drug solubility. In this study, the HI-6-loaded nanoparticles that conjugated with c(RGDyK) cyclic peptide were successfully synthesized, with encapsulation efficiency 63.69%, drug loading 6.2%, average particle size 166.9 nm, and zeta potential − 22.0 mV. The shape was round and evenly distributed. The BBB model was established by astrocytes and brain capillary endothelial cells, and the transendothelial cell resistance values of the BBB model could reach 183 Ω. The penetration effect of the c(RGDyK)-modified nanoparticles was about 4 times the free HI-6 on the BBB model in vitro. The c(RGDyK)-modified nanoparticles were more effective at targeting the brain than the unmodified nanoparticles in vivo. In addition, reactivation evaluation showed that the modified nanoparticles had a higher reactivation rate for poisoned mice, indicating that the nanoparticles modified with c(RGDyK) cyclic peptide had more central targeting. The successful implementation of this study is expected to improve the treatment level of nerve agents.
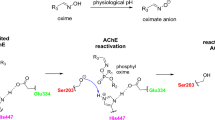
Graphical abstract













Similar content being viewed by others
References
Al-Sarraf H, Malatiali S, Al-Awadi M, Redzic Z (2018) Effects of erythropoietin on astrocytes and brain endothelial cells in primary culture during anoxia depend on simultaneous signaling by other cytokines and on duration of anoxia. Neurochem Int 113:34–45. https://doi.org/10.1016/j.neuint.2017.11.014
Belhadj Z, Zhan C, Ying M, Wei X, Xie C, Yan Z, Lu W (2017) Multifunctional targeted liposomal drug delivery for efficient glioblastoma treatment. Oncotarget 8(40):66889–66900. https://doi.org/10.18632/oncotarget.17976
Bi Y, Liu L, Lu Y, Sun T, Shen C, Chen X, Chen Q, An S, He X, Ruan C, Wu Y, Zhang Y, Guo Q, Zheng Z, Liu Y, Lou M, Zhao S, Jiang C (2016) T7 peptide-functionalized PEG-PLGA micelles loaded with carmustine for targeting therapy of glioma. ACS Appl Mater Interfaces 8:27465–27473. https://doi.org/10.1021/acsami.6b05572
Bohnert S, Vair C, Mikler J (2010) Development and validation of a sensitive HPLC method for the quantification of HI-6 in guinea pig plasma and evaluated in domestic swine. J Chromatogr B Analyt Technol Biomed Life Sci 878:1407–1413. https://doi.org/10.1016/j.jchromb.2010.03.018
Chen Y, Zhang W, Huang Y, Gao F, Fang X (2015) Dual-functional c(RGDyK)-decorated Pluronic micelles designed for antiangiogenesis and the treatment of drug-resistant tumor. Int J Nanomed 10:4863–4888. https://doi.org/10.2147/ijn.s86827
Chen Y, Zhang W, Huang Y, Gao F, Fang X (2016) In vivo biodistribution and anti-tumor efficacy evaluation of doxorubicin and paclitaxel-loaded Pluronic micelles decorated with c(RGDyK) peptide. PloS One 11:e0149952. https://doi.org/10.1371/journal.pone.0149952
Chen X, Zhang Y, Tang C, Tian C, Sun Q, Su Z, Xue L, Yin Y, Ju C, Zhang C (2017) Co-delivery of paclitaxel and anti-survivin siRNA via redox-sensitive oligopeptide liposomes for the synergistic treatment of breast cancer and metastasis. Int J Pharm. 529:102–115. https://doi.org/10.1016/j.ijpharm.2017.06.071
Chung HJ, Go DH, Bae JW, Jung IK, Lee JW, Park KD (2005) Synthesis and characterization of Pluronic? Grafted chitosan copolymer as a novel injectable biomaterial. Curr Appl Phys. 5:485–488. https://doi.org/10.1016/j.cap.2005.01.015
Cucullo L, McAllister MS, Kight K, Krizanac-Bengez L, Marroni M, Mayberg MR, Stanness KA, Janigro D (2002) A new dynamic in vitro model for the multidimensional study of astrocyte–endothelial cell interactions at the blood–brain barrier. Brain Res 951:243–254. https://doi.org/10.1016/s0006-8993(02)03167-0
Dadparvar M, Wagner S, Wien S, Kufleitner J, Worek F, von Briesen H, Kreuter J (2011) HI 6 human serum albumin nanoparticles—development and transport over an in vitro blood–brain barrier model. Toxicol Lett. 206:60–66. https://doi.org/10.1016/j.toxlet.2011.06.027
Deli MA, Ábrahám CS, Kataoka Y, Niwa M (2005) Permeability studies on in vitro blood–brain barrier models: physiology, pathology, and pharmacology. Cell Mol Neurobiol 25:59–127. https://doi.org/10.1007/s10571-004-1377-8
Draffehn S, Eichhorst J, Wiesner B, Kumke MU (2016) Insight into the modification of polymeric micellar and liposomal nanocarriers by fluorescein-labeled lipids and uptake-mediating lipopeptides. Langmuir. 32:6928–6939. https://doi.org/10.1021/acs.langmuir.6b01487
Elsinghorst PW, Worek F, Thiermann H, Wille T (2013) Drug development for the management of organophosphorus poisoning. Expert Opin Drug Dis 8:1467–1477. https://doi.org/10.1517/17460441.2013.847920
Fang Z, Chen S, Qin J, Chen B, Ni G, Chen Z, Zhou J, Ning Y, Zhou L (2016) Pluronic P85-coated poly(butylcyanoacrylate) nanoparticles overcome phenytoin resistance in P-glycoprotein overexpressing rats with lithium-pilocarpine-induced chronic temporal lobe epilepsy. Biomaterials 97:110–121. https://doi.org/10.1016/j.biomaterials.2016.04.02
Figueiredo TH, Qashu F, Apland JP, Aroniadou-Anderjaska V, Souza AP, Braga MFM (2010) The GluK1 (GluR5) kainate/ -amino-3-hydroxy-5-methyl-4-isoxazolepropionic acid receptor antagonist LY293558 reduces soman-induced seizures and neuropathology. J Pharmacol Exp Ther 336:303–312. https://doi.org/10.1124/jpet.110.171835
Garberg P, Ball M, Borg N, Cecchelli R, Fenart L, Hurst RD, Lindmark T, Mabondzo A, Nilsson JE, Raub TJ, Stanimirovic D, Terasaki T, Oberg JO, Osterberg T (2005) In vitro models for the blood–brain barrier. Toxicol In Vitro 19:299–334. https://doi.org/10.1016/j.tiv.2004.06.011
Huang Y, Liu W, Gao F, Fang X, Chen Y (2016) c(RGDyK)-decorated Pluronic micelles for enhanced doxorubicin and paclitaxel delivery to brain glioma. Int J Nanomed 11:1629–1641. https://doi.org/10.2147/ijn.s104162
Järvinen P, Vuorela P, Hatakka A, Fallarero A (2011) Potency determinations of acetylcholinesterase inhibitors using Ellman’s reaction-based assay in screening: effect of assay variants. Anal Biochem 408:166–168. https://doi.org/10.1016/j.ab.2010.09.018
Jun D, Stodulka P, Kuca K, Dolezal B (2010) High-performance liquid chromatography analysis of by-products and intermediates arising during the synthesis of the acetylcholinesterase reactivator HI-6. J Chromatogr Sci. 48:694–696. https://doi.org/10.1093/chromsci/48.8.694
Kassa J, Karasova J, Bajgar J, Kuca K, Musilek K (2008) A comparison of the therapeutic and reactivating efficacy of newly developed bispyridinium compounds (K206, K269) with currently available oximes against tabun in rats and mice. J Enzyme Inhib Med Chem 23:776–780. https://doi.org/10.1080/14756360701809902
Kim DH, Seo YK, Thambi T, Moon GJ, Son JP, Li G, Son JP, Li G, Park JH, Lee J, Kim HH, Bang OY (2015) Enhancing neurogenesis and angiogenesis with target delivery of stromal cell derived factor-1α using a dual ionic pH-sensitive copolymer. Biomaterials 61:115–125. https://doi.org/10.1016/j.biomaterials.2015.05.02
Kreuter J (2012a) Nanoparticulate systems for brain delivery of drugs. Adv Drug Deliv Rev 64:213–222. https://doi.org/10.1016/j.addr.2012.09.015
Kreuter J (2012b) Mechanism of polymeric nanoparticle-based drug transport across the blood-brain barrier (BBB). J Microencapsul 30:49–54. https://doi.org/10.3109/02652048.2012.692491
Kuca K, Musilek K, Korabecny J, Karasova J (2013) Influence of the distance between quaternary nitrogen and oxime group on the reactivation ability of oximes -antidotes against nerve agents[J]. J Environ Immunol Toxicol 1:41–43
Langer K, Balthasar S, Vogel V, Dinauer N, von Briesen H, Schubert D (2003) Optimization of the preparation process for human serum albumin (HSA) nanoparticles. Int J Pharm 257:169–180. https://doi.org/10.1016/s0378-5173(03)00134-0
Li G, Simon MJ, Cancel LM, Shi Z-D, Ji X, Tarbell JM, Morrison B, Fu BM (2010) Permeability of endothelial and astrocyte cocultures: in vitro blood–brain barrier models for drug delivery studies. Ann Biomed Eng 3:2499–2511. https://doi.org/10.1007/s10439-010-0023-5
Lu W, Zhang Y, Tan YZ, Hu KL, Jiang XG, Fu SK (2005) Cationic albumin-conjugated pegylated nanoparticles as novel drug carrier for brain delivery. J Control Release 107:428–448. https://doi.org/10.1016/j.jconrel.2005.03.027
Mc Carthy DJ, Malhotra M, O’Mahony AM, Cryan JF, O’Driscoll CM (2014) Nanoparticles and the blood-brain barrier: advancing from in-vitro models towards therapeutic significance. Pharm Res 32:1161–1185. https://doi.org/10.1007/s11095-014-1545-6
Miura Y, Takenaka T, Toh K, Wu S, Nishihara H, Kano MR, Ino Y, Nomoto T, Matsumoto Y, Koyama H, Cabral H, Nishiyama N, Kataoka K (2013) Cyclic RGD-linked polymeric micelles for targeted delivery of platinum anticancer drugs to glioblastoma through the blood–brain tumor barrier. ACS Nano 7:8583–8592. https://doi.org/10.1021/nn402662d
Molino Y, Jabès F, Lacassagne E, Gaudin N, Khrestchatisky M (2014) Setting-up an in vitro model of rat blood-brain barrier (BBB): a focus on BBB impermeability and receptor-mediated transport. J Vis Exp 28(88):e51278. https://doi.org/10.3791/51278
On NH, Mitchell R, Savant SD, Bachmeier CJ, Hatch GM, Miller DW (2012) Examination of blood–brain barrier (BBB) integrity in a mouse brain tumor model. J Neurooncol 111:133–143. https://doi.org/10.1007/s11060-012-1006-1
Patil-Gadhe A, Pokharkar V (2016) Pulmonary targeting potential of rosuvastatin loaded nanostructured lipid carrier: optimization by factorial design. Int J Pharm 501:199–210. https://doi.org/10.1016/j.ijpharm.2016.01.080
Perrière N, Demeuse P, Garcia E, Regina A, Debray M, Andreux JP, Couvreur P, Scherrmann JM, Temsamani J, Couraud PO, Deli MA, Roux F (2005) Puromycin-based purification of rat brain capillary endothelial cell cultures.Effect on the expression of blood-brain barrier-specific properties. J Neurochem 93:279–289. https://doi.org/10.1111/j.1471-4159.2004.03020.x
Qian T, Maguire SE, Canfield SG, Bao X, Olson WR, Shusta EV, Palecek SP (2017) Directed differentiation of human pluripotent stem cells to blood-brain barrier endothelial cells. Sci Adv 3(11):e1701679. https://doi.org/10.1126/sciadv.1701679
Qiu L, Hu Q, Cheng L, Li L, Tian C, Chen W, Chen Q, Hu W, Xu L, Yang J, Cheng L, Chen D (2016) cRGDyK modified pH responsive nanoparticles for specific intracellular delivery of doxorubicin. Acta Biomater 30:285–298. https://doi.org/10.1016/j.actbio.2015.11.037
Rampino A, Borgogna M, Blasi P, Bellich B, Cesàro A (2013) Chitosan nanoparticles: preparation, size evolution and stability. Int J Pharm 455:219–228. https://doi.org/10.1016/j.ijpharm.2013.07.034
Sánchez-Purrà M, Ramos V, Petrenko VA, Torchilin VP, Borrós S (2016) Double-targeted polymersomes and liposomes for multiple barrier crossing. Int J Pharm 511:946–956. https://doi.org/10.1016/j.ijpharm.2016.08.001
Saraiva C, Praça C, Ferreira R, Santos T, Ferreira L, Bernardino L (2016) Nanoparticle-mediated brain drug delivery: overcoming blood–brain barrier to treat neurodegenerativediseases. J Control Release 235:34–47. https://doi.org/10.1016/j.jconrel.2016.05.044
Shawahna R, Decleves X, Scherrmann JM (2013) Hurdles with using in vitro models to predict human blood-brain barrier drug permeability: aspecial focus on transporters and metabolizing enzymes. Curr Drug Metab 14:120–136
Shih TM, Duniho SM, McDonough JH (2003) Control of nerve agent-induced seizures is critical for neuroprotection and survival. Toxicol Appl Pharmacol 188:69–80. https://doi.org/10.1016/s0041-008x(03)00019-x
Shilo M, Sharon A, Baranes K, Motiei M, Lellouche JPM, Popovtzer R (2015) The effect of nanoparticle size on the probability to cross the blood-brain barrier: an in-vitro endothelial cell model. J Nanobiotechnol 13:19. https://doi.org/10.1186/s12951-015-0075-7
Soukup O, Tobin G, Kumar UK, Binder J, Proska J, Jun D, Fusek J, Kuca K (2010) Interaction of nerve agent antidotes with cholinergic systems. Curr Med Chem 17:1708–1718. https://doi.org/10.2174/092986710791111260
Takeshita Y, Obermeier B, Cotleur A, Sano Y, Kanda T, Ransohoff RM (2014) An in vitro blood–brain barrier model combining shear stress and endothelial cell/astrocyte co-culture. J Neurosci Methods 232:165–172. https://doi.org/10.1016/j.jneumeth.2014.05.013
Tavares MR, de Menezes LR, do Nascimento DF, Souza DHS, Reynaud F, Marques MFV, Tavares MIB (2016) Polymeric nanoparticles assembled with microfluidics for drug delivery across the blood-brain barrier. Eur Phys J Spec Top 225:779–795. https://doi.org/10.1140/epjst/e2015-50266-2
Uchida Y, Ohtsuki S, Terasaki T (2014) Pharmacoproteomics-based reconstruction of in vivo P-glycoprotein function at blood-brain barrier and brain distribution of substrate verapamil in pentylenetetrazole-kindled epilepsy, spontaneous epilepsy, and phenytoin treatment models. Drug Metab Dispos 42:1719–1726. https://doi.org/10.1124/dmd.114.059055
Wagner S, Kufleitner J, Zensi A, Dadparvar M, Wien S, Bungert J, Vogel T, Worek F, Kreuter J, von Briesen H (2010) Nanoparticulate transport of oximes over an in vitro blood- brain barrier model. PLoS ONE 5(12):e14213. https://doi.org/10.1371/journal.pone.0014213
Wang N, Guan Y, Yang L, Jia L, Wei X, Liu H, Guo C (2013) Magnetic nanoparticles (MNPs) covalently coated by PEO–PPO–PEO block copolymer for drug delivery. J Colloid Interface Sci 395:50–57. https://doi.org/10.1016/j.jcis.2012.11.062
Wang F, Li L, Liu B, Chen Z, Li C (2017) Hyaluronic acid decorated Pluronic P85 solid lipid nanoparticles as a potential carrier to overcome multidrug resistance in cervical and breast cancer. Biomed Pharmacother 86:595–604. https://doi.org/10.1016/j.biopha.2016.12.041
Wiener SW, Hoffman RS (2004) Nerve agents: a comprehensive review. J Intensive Care Med 19:22–37. https://doi.org/10.1177/0885066603258659
Wolff A, Antfolk M, Brodin B, Tenje M (2015) In vitro blood–brain barrier models—an overview of established models and new microfluidic approaches. J Pharm Sci 104:2727–2746. https://doi.org/10.1002/jps.24329
Worek F, Thiermann H, Szinicz L, Eyer P (2004) Kinetic analysis of interactions between human acetylcholinesterase, structurally different organophosphorus compoundsandoximes. Biochem Pharmacol 68:2237–2248. https://doi.org/10.1016/j.bcp.2004.07.038
Zhang X, Alakhova DY, Batrakova EV, Li S, Yang Z, Li Y, Kabanov AV (2008) Effect of Pluronic P85 on amino acid transport in bovine brain microvessel endothelial cells. J Neuroimmune Pharmacol 4:35–46. https://doi.org/10.1007/s11481-008-9119-1
Zhang Y, Zhai M, Chen Z, Han X, Yu F, Li Z, Xie X, Han C, Yu L, Yang Y, Mei X (2017) Dual-modified liposome codelivery of doxorubicin and vincristine improve targeting and therapeutic efficacy of glioma. Drug Deliv. 24:1045–1055. https://doi.org/10.1080/10717544.2017.1344334
Zhao H, Sun P, Fan T, Yang XH, Zheng TZ (2018) The effect of glutamate- induced excitotoxicity on DNA methylation in astrocytes in a new in vitro neuron-astrocyte-endothelium co-culture system. Biochem Biophys Res Commun 508:1209–1214. https://doi.org/10.1016/j.bbrc.2018.12.058
Zhu X, Pang Z, Shen S (2016) Tumor microenvironment responsive ACPP-conjugated micelles for targeted treatment of brain glioma. Part Part Syst Charact 34(2):1600201. https://doi.org/10.1002/ppsc.201600201
Zhu B, Zhang H, Yu L (2017) Novel transferrin modified and doxorubicin loaded Pluronic 85/lipid-polymeric nanoparticles for the treatment of leukemia: in vitro and in vivo therapeutic effect evaluation. Biomed Pharmacother. 86:547–554. https://doi.org/10.1016/j.biopha.2016.11.121
Acknowledgments
Top-ranking project of the Army’s Medical Science and Technology Youth Training Program (16QNP012).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
All procedures involving animals were approved by the Xinjiang Medical University IACUC.
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Liu, Y., Zhou, X., Wang, X. et al. c(RGDyK)-mediated Pluronic-PBCA nanoparticles through the blood-brain barrier to enhance the treatment of central organophosphorus intoxication. J Nanopart Res 22, 330 (2020). https://doi.org/10.1007/s11051-020-05039-7
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s11051-020-05039-7