Abstract
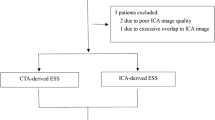
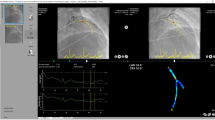
Endothelial shear stress (ESS) identifies coronary plaques at high risk for progression and/or rupture leading to a future acute coronary syndrome. In this study an optimized methodology was developed to derive ESS, pressure drop and oscillatory shear index using computational fluid dynamics (CFD) in 3D models of coronary arteries derived from non-invasive coronary computed tomography angiography (CTA). These CTA-based ESS calculations were compared to the ESS calculations using the gold standard with fusion of invasive imaging and CTA. In 14 patients paired patient-specific CFD models based on invasive and non-invasive imaging of the left anterior descending (LAD) coronary arteries were created. Ten patients were used to optimize the methodology, and four patients to test this methodology. Time-averaged ESS (TAESS) was calculated for both coronary models applying patient-specific physiological data available at the time of imaging. For data analysis, each 3D reconstructed coronary artery was divided into 2 mm segments and each segment was subdivided into 8 arcs (45°).TAESS and other hemodynamic parameters were averaged per segment as well as per arc. Furthermore, the paired segment- and arc-averaged TAESS were categorized into patient-specific tertiles (low, medium and high). In the ten LADs, used for optimization of the methodology, we found high correlations between invasively-derived and non-invasively-derived TAESS averaged over segments (n = 263, r = 0.86) as well as arcs (n = 2104, r = 0.85, p < 0.001). The correlation was also strong in the four testing-patients with r = 0.95 (n = 117 segments, p = 0.001) and r = 0.93 (n = 936 arcs, p = 0.001).There was an overall high concordance of 78% of the three TAESS categories comparing both methodologies using the segment- and 76% for the arc-averages in the first ten patients. This concordance was lower in the four testing patients (64 and 64% in segment- and arc-averaged TAESS). Although the correlation and concordance were high for both patient groups, the absolute TAESS values averaged per segment and arc were overestimated using non-invasive vs. invasive imaging [testing patients: TAESS segment: 30.1(17.1–83.8) vs. 15.8(8.8–63.4) and TAESS arc: 29.4(16.2–74.7) vs 15.0(8.9–57.4) p < 0.001]. We showed that our methodology can accurately assess the TAESS distribution non-invasively from CTA and demonstrated a good correlation with TAESS calculated using IVUS/OCT 3D reconstructed models.








Similar content being viewed by others
References
Barbato, E., G. G. Toth, N. P. Johnson, N. H. J. Pijls, W. F. Fearon, P. A. L. Tonino, N. Curzen, Z. Piroth, G. Rioufol, P. Jüni, and B. De Bruyne. A prospective natural history study of coronary atherosclerosis using fractional flow reserve. J. Am. Coll. Cardiol. 68:2247–2255, 2016.
Bech, G. J. W., B. De Bruyne, N. H. J. Pijls, E. D. De Muinck, J. C. A. Hoorntje, J. Escaned, P. R. Stella, E. Boersma, J. Bartunek, J. J. Koolen, and W. Wijns. Fractional flow reserve to determine the appropriateness of angioplasty in moderate coronary stenosis: a randomized trial. Circulation 103:2928–2934, 2001.
Benjamin, E. J., M. J. Blaha, S. E. Chiuve, and M. Cushman. Heart Disease and Stroke Statistics—2017 Update. 2017, 146–603 pp.
Berger, S. A., E. W. Goldsmith, and E. R. Lewis. Introduction to Bioengineering. Oxford: Oxford University Press, 2000.
Bernardini, F., J. Mittleman, H. Rushmeier, C. Silva, and G. Tuabin. The Ball-Pivoting algorithm for surface reconsturction. IEEE Trans. Vis. Comput. Graph. 5:349–359, 1999.
Bezerra, H. G., M. A. Costa, G. Guagliumi, A. M. Rollins, and D. I. Simon. Intracoronary optical coherence tomography: a comprehensive review: clinical and research applications. JACC Cardiovasc Interv. 2:1035–1046, 2009.
Bourantas, C. V., L. Räber, A. Sakellarios, Y. Ueki, T. Zanchin, K. C. Koskinas, K. Yamaji, M. Taniwaki, D. Heg, M. D. Radu, M. I. Papafaklis, F. Kalatzis, K. K. Naka, D. I. Fotiadis, A. Mathur, P. W. Serruys, L. K. Michalis, H. M. Garcia-Garcia, A. Karagiannis, and S. Windecker. Utility of multimodality intravascular imaging and the local hemodynamic forces to predict atherosclerotic disease progression. JACC Cardiovasc. Imaging 2019. https://doi.org/10.1016/j.jcmg.2019.02.026.
Bulant, C. A., P. J. Blanco, G. D. Maso-Talou, C. G. Bezerra, P. A. Lemos, and R. A. Feijóo. A head-to-head comparison between CT- and IVUS-derived coronary blood flow models. J. Biomech. 51:65–76, 2017.
Burattini, R., P. Sipkema, G. A. van Huis, and N. Westerhof. Identification of canine coronary resistance and intramyocardial compliance on the basis of the waterfall model. Ann. Biomed. Eng. 13:385–404, 1985.
Chatzizisis, Y. S., M. Jonas, R. Beigel, A. U. Coskun, A. B. Baker, B. V. Stone, C. Maynard, R. G. Gerrity, W. Daley, E. R. Edelman, C. L. Feldman, and P. H. Stone. Attenuation of inflammation and expansive remodeling by Valsartan alone or in combination with Simvastatin in high-risk coronary atherosclerotic plaques. Atherosclerosis 203:387–394, 2009.
Chatzizisis, Y. S., M. Jonas, A. U. Coskun, R. Beigel, B. V. Stone, C. Maynard, R. G. Gerrity, W. Daley, C. Rogers, E. R. Edelman, C. L. Feldman, and P. H. Stone. Prediction of the localization of high-risk coronary atherosclerotic plaques on the basis of low endothelial shear stress-an intravascular ultrasound and histopathology natural history study. Circulation 117:993–1002, 2008.
Choi, G., J. M. Lee, H. J. Kim, J. B. Park, S. Sankaran, H. Otake, J. H. Doh, C. W. Nam, E. S. Shin, C. A. Taylor, and B. K. Koo. Coronary artery axial plaque stress and its relationship with lesion geometry application of computational fluid dynamics to coronary CT angiography. JACC Cardiovasc. Imaging 8:1156–1166, 2015.
Collet, C., B. Chevalier, A. Cequier, J. Fajadet, M. Dominici, S. Helqvist, A. J. Van Boven, D. Dudek, D. McClean, M. Almeida, J. J. Piek, E. Tenekecioglu, A. Bartorelli, S. Windecker, P. W. Serruys, and Y. Onuma. Diagnostic accuracy of coronary CT angiography for the evaluation of bioresorbable vascular scaffolds. JACC Cardiovasc. Imaging 11:722–732, 2018.
Costopoulos, C., L. H. Timmins, Y. Huang, O. Y. Hung, D. S. Molony, A. J. Brown, E. L. Davis, Z. Teng, J. H. Gillard, H. Samady, and M. R. Bennett. Impact of combined plaque structural stress and wall shear stress on coronary plaque progression, regression, and changes in composition. Eur. Heart J. 2019. https://doi.org/10.1093/eurheartj/ehz132.
Doh, J. H., B. K. Koo, C. W. Nam, J. H. Kim, J. K. Min, R. Nakazato, T. Silalahi, H. Prawira, H. Choi, S. Y. Lee, J. Namgung, S. U. Kwon, J. J. Kwak, and W. R. Lee. Diagnostic value of coronary CT angiography in comparison with invasive coronary angiography and intravascular ultrasound in patients with intermediate coronary artery stenosis: results from the prospective multicentre FIGURE-OUT (Functional Imaging crite. Eur. Heart J. Cardiovasc. Imaging 15:870–877, 2014.
Eshtehardi, P., M. C. McDaniel, J. Suo, S. S. Dhawan, L. H. Timmins, J. N. G. Binongo, L. J. Golub, M. T. Corban, A. V. Finn, J. N. Oshinski, A. A. Quyyumi, D. P. Giddens, and H. Samady. Association of coronary wall shear stress with atherosclerotic plaque burden, composition, and distribution in patients with coronary artery disease. J. Am. Heart Assoc. 1:e002543–e002543, 2012.
Eslami, P., J. Tran, Z. Jin, J. Karady, R. Sotoodeh, M. T. Lu, U. Hoffmann, and A. Marsden. Effect of wall elasticity on hemodynamics and wall shear stress in patient-specific simulations in the coronary arteries. J. Biomech. Eng. 2019. https://doi.org/10.1115/1.4043722.
Esmaily-Moghadam, M., Y. Bazilevs, and A. L. Marsden. A new preconditioning technique for implicitly coupled multidomain simulations with applications to hemodynamics. Comput. Mech. 52:1141–1152, 2013.
Giannopoulos, A. A., C. S. Yiannis, P. Maurovich-Horvat, A. P. Antoniadis, U. Hoffmann, M. L. Steigner, F. J. Rybicki, and M. Dimitrios. Quantifying the effect of side branches in endothelial shear stress estimates. Atherosclerosis 30:873–882, 2016.
Van Der Giessen, A. G., M. Schaap, F. J. H. Gijsen, H. C. Groen, T. Van Walsum, N. R. Mollet, J. Dijkstra, F. N. Van De Vosse, W. J. Niessen, P. J. De Feyter, A. F. W. Van Der Steen, and J. J. Wentzel. 3D fusion of intravascular ultrasound and coronary computed tomography for in-vivo wall shear stress analysis: a feasibility study. Int. J. Cardiovasc. Imaging 26:781–796, 2010.
Gijsen, F., Y. Katagiri, P. Barlis, C. Bourantas, C. Collet, U. Coskun, J. Daemen, J. Dijkstra, E. Edelman, P. Evans, K. Van Der Heiden, R. Hose, B. K. Koo, R. Krams, A. Marsden, F. Migliavacca, Y. Onuma, A. Ooi, E. Poon, H. Samady, P. Stone, K. Takahashi, D. Tang, V. Thondapu, E. Tenekecioglu, L. Timmins, R. Torii, J. Wentzel, and P. Serruys. Expert recommendations on the assessment of wall shear stress in human coronary arteries: existing methodologies, technical considerations, and clinical applications. Eur. Heart J. 40:3421–3433, 2019.
Han, D., A. Starikov, B. Hartaigh, H. Gransar, K. K. Kolli, J. H. Lee, A. Rizvi, L. Baskaran, J. Schulman-Marcus, F. Y. Lin, and J. K. Min. Relationship between endothelial wall shear stress and high-risk atherosclerotic plaque characteristics for identification of coronary lesions that cause ischemia: a direct comparison with fractional flow reserve. J. Am. Heart Assoc. 5:1–9, 2016.
Holland, P. W., and R. E. Welsch. Robust regression using iteratively reweighted least-squares. Commun. Stat. Theory Methods 6:813–827, 1977.
Hoogendoorn, A., A. M. Kok, E. M. J. Hartman, G. de Nisco, L. Casadonte, C. Chiastra, A. Coenen, S.-A. Korteland, K. Van der Heiden, F. J. H. Gijsen, D. J. Duncker, A. F. W. van der Steen, and J. J. Wentzel. Multidirectional wall shear stress promotes advanced coronary plaque development: comparing five shear stress metrics. Res Cardiovasc 2019. https://doi.org/10.1093/cvr/cvz212.
Johnson, K., P. Sharma, and J. Oshinski. Coronary artery flow measurement using navigator echo gated phase contrast magnetic resonance velocity mapping at 3.0 T. J. Biomech. Eng. 41:595–602, 2008.
Kim, H. J., I. E. Vignon-Clementel, J. S. Coogan, C. A. Figueroa, K. E. Jansen, and C. A. Taylor. Patient-specific modeling of blood flow and pressure in human coronary arteries. Ann. Biomed. Eng. 38:3195–3209, 2010.
Koskinas, K., Y. S. Chatzizisis, M. I. Papafaklis, A. U. Coskun, A. B. Baker, P. Jarolim, A. P. Antoniadis, E. R. Edelman, P. H. Stone, and C. L. Feldman. Synergistic effect of local endothelial shear stress and systemic hypercholesterolemia on coronary atherosclerotic plaque progression and composition in pigs konstantinos 119:5124–5136, 2010.
Kumar, A., O. Y. Hung, M. Piccinelli, P. Eshtehardi, M. T. Corban, D. Sternheim, B. Yang, A. Lefieux, D. S. Molony, E. W. Thompson, W. Zeng, Y. Bouchi, S. Gupta, H. Hosseini, M. Raad, Y.-A. Ko, C. Liu, M. C. McDaniel, B. D. Gogas, J. S. Douglas, A. A. Quyyumi, D. P. Giddens, A. Veneziani, and H. Samady. Low coronary wall shear stress is associated with severe endothelial dysfunction in patients with nonobstructive coronary artery disease. JACC Cardiovasc. Interv. 11:2072–2080, 2018.
Kumar, A., E. W. Thompson, A. Lefieux, D. S. Molony, E. L. Davis, N. Chand, S. Fournier, H. S. Lee, J. Suh, K. Sato, Y. A. Ko, D. Molloy, K. Chandran, H. Hosseini, S. Gupta, A. Milkas, B. Gogas, H. J. Chang, J. K. Min, W. F. Fearon, A. Veneziani, D. P. Giddens, S. B. King, B. De Bruyne, and H. Samady. High coronary shear stress in patients with coronary artery disease predicts myocardial infarction. J. Am. Coll. Cardiol. 72:1926–1935, 2018.
Lee, J. M., G. Choi, B. K. Koo, D. Hwang, J. Park, J. Zhang, K. J. Kim, Y. Tong, H. J. Kim, L. Grady, J. H. Doh, C. W. Nam, E. S. Shin, Y. S. Cho, S. Y. Choi, E. J. Chun, J. H. Choi, B. L. Nørgaard, E. H. Christiansen, K. Niemen, H. Otake, M. Penicka, B. de Bruyne, T. Kubo, T. Akasaka, J. Narula, P. S. Douglas, C. A. Taylor, and H. S. Kim. Identification of high-risk plaques destined to cause acute coronary syndrome using coronary computed tomographic angiography and computational fluid dynamics. JACC Cardiovasc. Imaging 12:1032–1043, 2019.
Lu, M. T., M. Ferencik, R. S. Roberts, K. L. Lee, A. Ivanov, E. Adami, D. B. Mark, F. A. Jaffer, J. A. Leipsic, P. S. Douglas, and U. Hoffmann. Noninvasive FFR derived from coronary CT angiography. Management and outcomes in the PROMISE trial. JACC Cardiovasc: Imaging, 2016. https://doi.org/10.1016/j.jcmg.2016.11.024.
Nakazato, R., H. B. Park, D. S. Berman, H. Gransar, B. K. Koo, A. Erglis, F. Y. Lin, A. M. Dunning, M. J. Budoff, J. Malpeso, J. Leipsic, and J. K. Min. Noninvasive fractional flow reserve derived from computed tomography angiography for coronary lesions of intermediate stenosis severity results from the DeFACTO study. Circ. Cardiovasc. Imaging 6:881–889, 2013.
Papafaklis, M. I., S. Takahashi, A. P. Antoniadis, A. U. Coskun, M. Tsuda, S. Mizuno, I. Andreou, S. Nakamura, Y. Makita, A. Hirohata, S. Saito, C. L. Feldman, and P. H. Stone. Effect of the local hemodynamic environment on the de novo development and progression of eccentric coronary atherosclerosis in humans: Insights from PREDICTION. Atherosclerosis 240:205–211, 2015.
Parikh, N. I., P. Gona, M. G. Larson, C. S. Fox, R. S. Vasan, and D. Levy. Long-term trends in myocardial infarction incidence and case-fatality in the national heart, lung, and blood institute’s Framingham heart study. Circulation 119:1203–1210, 2010.
Samady, H., P. Eshtehardi, M. C. McDaniel, J. Suo, S. S. Dhawan, C. Maynard, L. H. Timmins, A. A. Quyyumi, and D. P. Giddens. Coronary artery wall shear stress is associated with progression and transformation of atherosclerotic plaque and arterial remodeling in patients with coronary artery disease. Circulation 124:779–788, 2011.
Si, H. TetGen, a quality tetrahedral mesh generator. AMC Trans. Math. Softw. 41:11, 2015.
Stone, P. H., A. U. Coskun, S. Kinlay, M. E. Clark, M. Sonka, A. Wahle, O. J. Ilegbusi, Y. Yeghiazarians, J. J. Popma, J. Orav, R. E. Kuntz, and C. L. Feldman. Effect of endothelial shear stress on the progression of coronary artery disease, vascular remodeling, and in-stent restenosis in humans: In vivo 6-month follow-up study. Circulation 108:438–444, 2003.
Stone, P. H., A. Maehara, A. U. Coskun, C. C. Maynard, M. Zaromytidou, G. Siasos, I. Andreou, D. Fotiadis, K. Stefanou, M. Papafaklis, L. Michalis, A. J. Lansky, G. S. Mintz, P. W. Serruys, C. L. Feldman, and G. W. Stone. Role of low endothelial shear stress and plaque characteristics in the prediction of nonculprit major adverse cardiac events: the PROSPECT study. JACC Cardiovasc. Imaging 11:462–471, 2018.
Stone, P. H., S. Saito, S. Takahashi, Y. Makita, S. Nakamura, T. Kawasaki, A. Takahashi, T. Katsuki, S. Nakamura, A. Namiki, A. Hirohata, T. Matsumura, S. Yamazaki, H. Yokoi, S. Tanaka, S. Otsuji, F. Yoshimachi, J. Honye, D. Harwood, M. Reitman, A. U. Coskun, M. I. Papafaklis, and C. L. Feldman. Prediction of progression of coronary artery disease and clinical outcomes using vascular profiling of endothelial shear stress and arterial plaque characteristics: the PREDICTION study. Circulation 126:172–181, 2012.
Tran, J. S., D. E. Schiavazzi, A. M. Kahn, and A. L. Marsden. Uncertainty quantification of simulated biomechanical stimuli in coronary artery bypass grafts. Comput. Methods Appl. Mech. Eng. 345:402–428, 2019.
Updegrove, A., N. M. Wilson, J. Merkow, H. Lan, A. L. Marsden, and S. C. Shadden. SimVascular: an open source pipeline for cardiovascular simulation. Ann. Biomed. Eng. 45:525–541, 2017.
Van Soest, G., E. Regar, T. P. M. Goderie, N. Gonzalo, S. Koljenovi, G. J. L. H. Van Leenders, P. W. Serruys, and A. F. W. Van Der Steen. Pitfalls in plaque characterization by OCT: image artifacts in native coronary arteries. JACC Cardiovasc. Imaging 4:810–813, 2011.
Vergallo, R., M. I. Papafaklis, T. Yonetsu, C. V. Bourantas, I. Andreou, Z. Wang, J. G. Fujimoto, I. McNulty, H. Lee, L. M. Biasucci, F. Crea, C. L. Feldman, L. K. Michalis, P. H. Stone, and I. K. Jang. Endothelial shear stress and coronary plaque characteristics in humans combined frequency-domain optical coherence tomography and computational fluid dynamics study. Circ. Cardiovasc. Imaging 7:905–911, 2014.
Veselka, J., P. Cadova, P. Tomasov, A. Theodor, and D. Zemanek. Dual-source CT angiography for detection and quantification of in-stent restenosis in the left main coronary artery: comparison with intracoronary ultrasound and coronary angiography. J. Invasive Cardiol. 23:460–464, 2011.
Wilson, N. M., A. K. Ortiz, and A. B. Johnson. The vascular model repository: a public resource of medical imaging data and blood flow simulation results. J. Med. Dev. 7:040923, 2013.
Author information
Authors and Affiliations
Corresponding author
Additional information
Associate Editor Lakshmi Prasad Dasi oversaw the review of this article.
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Eslami, P., Hartman, E.M.J., Albaghadai, M. et al. Validation of Wall Shear Stress Assessment in Non-invasive Coronary CTA versus Invasive Imaging: A Patient-Specific Computational Study. Ann Biomed Eng 49, 1151–1168 (2021). https://doi.org/10.1007/s10439-020-02631-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10439-020-02631-9