Abstract
Objective
IL-6-induced STAT3 activation is associated with various chronic inflammatory diseases. In this study, we investigated the anti-STAT3 mechanism of the dietary polyphenol, biochanin A (BCA), in IL-6-treated macrophages.
Methods
The effect of BCA on STAT3 and p38 MAPK was analyzed by immunoblot. The localization of both these transcription factors was determined by immunofluorescence and fractionation studies. The impact on DNA-binding activity of STAT3 was studied by luciferase assay. To understand which of the isoforms of p38 MAPK was responsible for BCA-mediated regulation of STAT3, overexpression of the proteins, site-directed mutagenesis, pull-down assays and computational analysis were performed. Finally, adhesion-migration assays and semi-quantitative PCR were employed to understand the biological effects of BCA-mediated regulation of STAT3.
Results
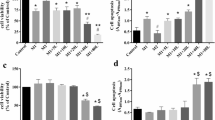
BCA prevented STAT3 phosphorylation (Tyr705) and increased p38 MAPK phosphorylation (Thr180/Tyr182) in IL-6-stimulated differentiated macrophages. This opposing modulatory effect of BCA was not observed in cells treated with other stress-inducing stimuli that activate p38 MAPK. BCA abrogated IL-6-induced nuclear translocation of phospho-STAT3 and its transcriptional activity, while increasing the cellular abundance of phospho-p38 MAPK. BCA-induced phosphorylation of p38δ, but not α, β, or γ was responsible for impeding IL-6-induced STAT3 phosphorylation. Interestingly, interaction with phospho-p38δ masked the Tyr705 residue of STAT3, preventing its phosphorylation. BCA significantly reduced STAT3-dependent expression of icam-1 and mcp-1 diminishing IL-6-mediated monocyte adhesion and migration.
Conclusion
This differential regulation of STAT3 and p38 MAPK in macrophages establishes a novel anti-inflammatory mechanism of BCA which could be important for the prevention of IL-6-associated chronic inflammatory diseases.







Similar content being viewed by others
References
Tanaka T, Narazaki M, Kishimoto T. IL-6 in inflammation, immunity, and disease. Cold Spring Harb Perspect Biol. 2014;6(10):a016295.
Heinrich PC, Behrmann I, Haan S, Hermanns HM, Muller-Newen G, Schaper F. Principles of interleukin (IL)-6-type cytokine signalling and its regulation. Biochem J. 2003;374:1–20.
Johnson DE, O'Keefe RA, Grandis JR. Targeting the IL-6/JAK/STAT3 signalling axis in cancer. Nat Rev Clin Oncol. 2018;15(4):234–48.
Teng Y, Ross JL, Cowell JK. The involvement of JAK-STAT3 in cell motility, invasion, and metastasis. Jak-Stat. 2014;3(1):e28086.
Naugler WE, Karin M. The wolf in sheep's clothing: the role of interleukin-6 in immunity, inflammation and cancer. Trends Mol Med. 2008;14(3):109–19.
Costa-Pereira AP. Regulation of IL-6-type cytokine responses by MAPKs. Biochem Soc Trans. 2014;42(1):59–62.
Meng A, Zhang X, Shi Y. Role of p38 MAPK and STAT3 in lipopolysaccharide-stimulated mouse alveolar macrophages. Exper Ther Med. 2014;8(6):1772–6.
Ahmed ST, Ivashkiv LB. Inhibition of IL-6 and IL-10 signaling and Stat activation by inflammatory and stress pathways. J Immunol. 2000;165(9):5227–37.
Terstegen L, Gatsios P, Bode JG, Schaper F, Heinrich PC, Graeve L. The inhibition of interleukin-6-dependent STAT activation by mitogen-activated protein kinases depends on tyrosine 759 in the cytoplasmic tail of glycoprotein 130. J Biol Chem. 2000;275(25):18810–7.
Scheller J, Chalaris A, Schmidt-Arras D. Rose-John S (2011) The pro-and anti-inflammatory properties of the cytokine interleukin-6. Biochim Biophys Acta (BBA) Mol Cell Res. 1813;5:878–88.
Matsumoto S, Hara T, Mitsuyama K, Yamamoto M, Tsuruta O, Sata M, et al. Essential roles of IL-6 trans-signaling in colonic epithelial cells, induced by the IL-6/soluble–IL-6 receptor derived from lamina propria macrophages, on the development of colitis-associated premalignant cancer in a murine model. J Immunol. 2010;184(3):1543–51.
Egwuagu CE. STAT3 in CD4+ T helper cell differentiation and inflammatory diseases. Cytokine. 2009;47(3):149–56.
He G, Karin M. NF-kappaB and STAT3 - key players in liver inflammation and cancer. Cell Res. 2011;21(1):159–68.
Busbee PB, Rouse M, Nagarkatti M, Nagarkatti PS. Use of natural AhR ligands as potential therapeutic modalities against inflammatory disorders. Nutr Rev. 2013;71(6):353–69.
Mukhtar H, Ahmad N. Tea polyphenols: prevention of cancer and optimizing health. Am J Clin Nutr. 1698S;71(6):1698S–S17021702.
Pan T, Jankovic J, Le W. Potential therapeutic properties of green tea polyphenols in Parkinson’s disease. Drugs Aging. 2003;20(10):711–21.
Strimpakos AS, Sharma RA. Curcumin: preventive and therapeutic properties in laboratory studies and clinical trials. Antioxid Redox Signal. 2008;10(3):511–46.
Yang CS, Chung JY, Yang G-Y, Chhabra SK, Lee M-J. Tea and tea polyphenols in cancer prevention. J Nutr. 2000;130(2):472S–8S.
Wu W-Y, Wu Y-Y, Huang H, He C, Li WZ, Wang H-L, et al. Biochanin A attenuates LPS-induced pro-inflammatory responses and inhibits the activation of the MAPK pathway in BV2 microglial cells. Int J Mol Med. 2015;35(2):391–8.
Kole L, Giri B, Manna SK, Pal B, Ghosh S. Biochanin-A, an isoflavone, showed anti-proliferative and anti-inflammatory activities through the inhibition of iNOS expression, p38-MAPK and ATF-2 phosphorylation and blocking NFκB nuclear translocation. Eur J Pharmacol. 2011;653(1–3):8–15.
Ming X, Ding M, Zhai B, Xiao L, Piao T, Liu M. Biochanin A inhibits lipopolysaccharide-induced inflammation in human umbilical vein endothelial cells. Life Sci. 2015;136:36–41.
Sithisarn P, Michaelis M, Schubert-Zsilavecz M, Cinatl J Jr. Differential antiviral and anti-inflammatory mechanisms of the flavonoids biochanin A and baicalein in H5N1 influenza A virus-infected cells. Antivir Res. 2013;97(1):41–8.
Kalayciyan A, Orawa H, Fimmel S, Perschel FH, González J-B, Fitzner RG, et al. Nicotine and biochanin A, but not cigarette smoke, induce anti-inflammatory effects on keratinocytes and endothelial cells in patients with Behcet's disease. J Investig Dermatol. 2007;127(1):81–9.
Wang W, Tang L, Li Y, Wang Y. Biochanin A protects against focal cerebral ischemia/reperfusion in rats via inhibition of p38-mediated inflammatory responses. J Neurol Sci. 2015;348(1–2):121–5.
Lawrence T, Bebien M, Liu GY, Nizet V, Karin M. IKKα limits macrophage NF-κB activation and contributes to the resolution of inflammation. Nature. 2005;434(7037):1138.
Basu A, Das AS, Sharma M, Pathak MP, Chattopadhyay P, Biswas K, et al. STAT3 and NF-κB are common targets for kaempferol-mediated attenuation of COX-2 expression in IL-6-induced macrophages and carrageenan-induced mouse paw edema. Biochem Biophys Rep. 2017;12:54–61.
Margreitter C, Reif MM, Oostenbrink C. Update on phosphate and charged post-translationally modified amino acid parameters in the GROMOS force field. J Comput Chem. 2017;38(10):714–20.
Abraham MJ, Murtola T, Schulz R, Páll S, Smith JC, Hess B, et al. GROMACS: High performance molecular simulations through multi-level parallelism from laptops to supercomputers. SoftwareX. 2015;1:19–25.
Kozakov D, Hall DR, Xia B, Porter KA, Padhorny D, Yueh C, et al. The ClusPro web server for protein–protein docking. Nat Protoc. 2017;12(2):255.
Lin X, Sun T, Cai M, Shen P. Cell-death-mode switch from necrosis to apoptosis in hydrogen peroxide treated macrophages. Sci China Life Sci. 2010;53(10):1196–203.
Forman HJ, Torres M. Reactive oxygen species and cell signaling: respiratory burst in macrophage signaling. Am J Respir Crit Care Med. 2002;166(supplement_1):S4–S8.
del Arco PG, Martı́nez-Martı́nez S, Maldonado JL, Ortega-Pérez I, Redondo JM. A role for the p38 MAP kinase pathway in the nuclear shuttling of NFATp. J Biol Chemi. 2000;275(18):13872-8
Ruspi G, Schmidt EM, McCann F, Feldmann M, Williams RO, Stoop AA, et al. TNFR2 increases the sensitivity of ligand-induced activation of the p38 MAPK and NF-κB pathways and signals TRAF2 protein degradation in macrophages. Cell Signal. 2014;26(4):683–90.
Zhao Q, Shepherd EG, Manson ME, Nelin LD, Sorokin A, Liu Y. The role of mitogen-activated protein kinase phosphatase-1 in the response of alveolar macrophages to Lipopolysaccharide attenuation of proinflammatory cytokine biosynthesis via feedback control of p38. J Biol Chem. 2005;280(9):8101–8.
Wood CD, Thornton TM, Sabio G, Davis RA, Rincon M. Nuclear Localization of p38 MAPK in Response to DNA Damage. Int J Biol Sci. 2009;5(5):428–37.
Yang J, Stark GR. Roles of unphosphorylated STATs in signaling. Cell Res. 2008;18(4):443–51.
Vogt M, Domoszlai T, Kleshchanok D, Lehmann S, Schmitt A, Poli V, et al. The role of the N-terminal domain in dimerization and nucleocytoplasmic shuttling of latent STAT3. J Cell Sci. 2011;124(Pt 6):900–9.
Choudhury GG, Ricono JM. Increased effect of interferon γ on PDGF-induced c-fos gene transcription in glomerular mesangial cells: differential effect of the transcriptional coactivator CBP on STAT1α activation. Biochem Biophys Res Commun. 2000;273(3):1069–77.
Yurtsever Z, Scheaffer SM, Romero AG, Holtzman MJ, Brett TJ. The crystal structure of phosphorylated MAPK13 reveals common structural features and differences in p38 MAPK family activation. Acta Crystallogr D Biol Crystallogr. 2015;71(4):790–9.
Korb A, Tohidast-Akrad M, Cetin E, Axmann R, Smolen J, Schett G. Differential tissue expression and activation of p38 MAPK α, β, γ, and δ isoforms in rheumatoid arthritis. Arthritis Rheum. 2006;54(9):2745–56.
Pramanik R, Qi X, Borowicz S, Choubey D, Schultz RM, Han J, et al. p38 Isoforms have opposite effects on AP-1-dependent transcription through regulation of c-Jun the determinant role of the isoforms in the p38 MAPK signal specificity. J Biol Chem. 2003;278(7):4831–9.
Piao CS, Che Y, Han P-L, Lee J-K. Delayed and differential induction of p38 MAPK isoforms in microglia and astrocytes in the brain after transient global ischemia. Mol Brain Res. 2002;107(2):137–44.
Lemke LE, Bloem LJ, Fouts R, Esterman M, Sandusky G, Vlahos CJ. Decreased p38 MAPK activity in end-stage failing human myocardium: p38 MAPK α is the predominant isoform expressed in human heart. J Mol Cell Cardiol. 2001;33(8):1527–40.
Mayya V, Lundgren DH, Hwang S-I, Rezaul K, Wu L, Eng JK, et al. Quantitative phosphoproteomic analysis of T cell receptor signaling reveals system-wide modulation of protein-protein interactions. Sci Signal. 2009;2(84):ra46-ra.
Kumar ND, Damle NP, Mohanty D. Getting phosphorylated: is it necessary to be solvent accessible? Proc Indian Natn Sci Acad. 2015;81(2):493–507.
Ashida N, Arai H, Yamasaki M, Kita T. Distinct signaling pathways for MCP-1-dependent integrin activation and chemotaxis. J Biol Chem. 2001;276(19):16555–60.
Papayianni A, Alexopoulos E, Giamalis P, Gionanlis L, Belechri AM, Koukoudis P, et al. Circulating levels of ICAM-1, VCAM-1, and MCP-1 are increased in haemodialysis patients: association with inflammation, dyslipidaemia, and vascular events. Nephrol Dial Transpl. 2002;17(3):435–41.
Mashili F, Chibalin AV, Krook A, Zierath JR. Constitutive STAT3 phosphorylation contributes to skeletal muscle insulin resistance in type 2 diabetes. Diabetes. 2013;62(2):457–65.
Kuuliala K, Kuuliala A, Koivuniemi R, Oksanen S, Hämäläinen M, Moilanen E, Kautiainen H, Leirisalo-Repo M, Repo H. Constitutive STAT3 phosphorylation in circulating CD4+ T lymphocytes associates with disease activity and treatment response in recent-onset rheumatoid arthritis. PLoS One. 2015;10(9):e0137385.
Briviba K, Pan L, Rechkemmer G. Red wine polyphenols inhibit the growth of colon carcinoma cells and modulate the activation pattern of mitogen-activated protein kinases. J Nutr. 2002;132(9):2814–8.
Chen C, Yu R, Owuor ED, Kong A-NT. Activation of antioxidant-response element (ARE), mitogen-activated protein kinases (MAPKs) and caspases by major green tea polyphenol components during cell survival and death. Archi Pharm Res. 2000;23(6):605.
Mansuri ML, Parihar P, Solanki I, Parihar MS. Flavonoids in modulation of cell survival signalling pathways. Genes Nutr. 2014;9(3):400.
Huang C-C, Wu W-B, Fang J-Y, Chiang H-S, Chen S-K, Chen B-H, et al. (-)-Epicatechin-3-gallate, a green tea polyphenol is a potent agent against UVB-induced damage in HaCaT keratinocytes. Molecules. 2007;12(8):1845–58.
Obata T, Brown GE, Yaffe MB. MAP kinase pathways activated by stress: the p38 MAPK pathway. Crit Care Med. 2000;28(4):N67–N77.
Clark AR, Dean JL, Saklatvala J. The p38 MAPK pathway mediates both antiinflammatory and proinflammatory processes: comment on the article by Damjanov and the editorial by Genovese. Arthritis Rheum. 2009;60(11):3513–4.
Szelenyi J, Selmeczy Z, Brozik A, Medgyesi D, Magocsi M. Dual β-adrenergic modulation in the immune system: Stimulus-dependent effect of isoproterenol on MAPK activation and inflammatory mediator production in macrophages. Neurochem Int. 2006;49(1):94–103.
Kim C, Sano Y, Todorova K, Carlson BA, Arpa L, Celada A, et al. The kinase p38 alpha serves cell type-specific inflammatory functions in skin injury and coordinates pro- and anti-inflammatory gene expression. Nat Immunol. 2008;9(9):1019–27.
Guma M, Hammaker D, Topolewski K, Corr M, Boyle DL, Karin M, et al. Antiinflammatory functions of p38 in mouse models of rheumatoid arthritis advantages of targeting upstream kinases MKK-3 or MKK-6. Arthritis Rheum-Us. 2012;64(9):2887–955.
Bellon S, Fitzgibbon MJ, Fox T, Hsiao HM, Wilson KP. The structure of phosphorylated P38 gamma is monomeric and reveals a conserved activation-loop conformation. Struct Fold Des. 1999;7(9):1057–65.
Shen Y, Schlessinger K, Zhu X, Meffre E, Quimby F, Levy DE, et al. Essential role of STAT3 in postnatal survival and growth revealed by mice lacking STAT3 serine 727 phosphorylation. Mol Cell Biol. 2004;24(1):407–19.
Lin G-S, Chen Y-P, Lin Z-X, Wang X-F, Zheng Z-Q, Chen L. STAT3 serine 727 phosphorylation influences clinical outcome in glioblastoma. Int J Clin Exp Pathol. 2014;7(6):3141.
Cross TG, Scheel-Toellner D, Henriquez NV, Deacon E, Salmon M, Lord JM. Serine/threonine protein kinases and apoptosis. Exp Cell Res. 2000;256(1):34–41.
Zhang CC, Li YL, Wu YN, Wang LY, Wang XN, Du J. Interleukin-6/signal transducer and activator of transcription 3 (STAT3) pathway is essential for macrophage infiltration and myoblast proliferation during muscle regeneration. J Biol Chem. 2013;288(3):1489–99.
Han X, Wang YX, Chen HL, Zhang JW, Xu CM, Li J, et al. Enhancement of ICAM-1 via the JAK2/STAT3 signaling pathway in a rat model of severe acute pancreatitis-associated lung injury. Exp Ther Med. 2016;11(3):788–96.
Acknowledgements
This study was supported by the Department of Biotechnology, Govt. of India (Twining project: BT/469/NE/TBP/2013 & U-Excel project: BT/410/NE/U-Excel/2013). We also acknowledge the High-Performance Computing Centre, Tezpur University (India), for use of the PARAM Shavak. We thank Dr. Sougata Saha and Dr. Suman Dasgupta, Department of MBBT, Tezpur University, for their technical help.
Author information
Authors and Affiliations
Contributions
The experimental studies, data analyses, and manuscript preparation were performed by Anandita Basu and Anindhya Sundar Das. The computational study and data analysis were performed by Pallab Kumar Borah and Raj Kumar Duary. Experiment designing, data analyses, manuscript preparation, and fund acquisition were done by Rupak Mukhopadhyay. The final version of the manuscript was approved by all the authors.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Human and animal rights
Studies on human peripheral blood mononuclear cells (PBMCs) were performed with due approval from the Tezpur University Ethics Committee (IEC No: 01/2014, dated 30/4/2014) with informed consent from healthy volunteers.
Additional information
Responsible Editor: John Di Battista.
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Basu, A., Das, A.S., Borah, P.K. et al. Biochanin A impedes STAT3 activation by upregulating p38δ MAPK phosphorylation in IL-6-stimulated macrophages. Inflamm. Res. 69, 1143–1156 (2020). https://doi.org/10.1007/s00011-020-01387-1
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00011-020-01387-1