Abstract
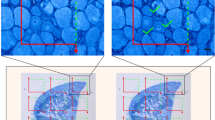
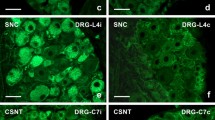
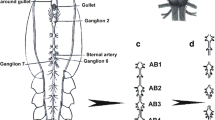
Neurotrauma is among the main causes of human disability and mortality. Nerve injury impairs not only neurons but also causes death of satellite glial cells remote from the injury site. We studied the dynamics of expression of different proapoptotic proteins (E2F1, p53, caspase 3) in the dorsal root ganglia (DRG) of a rat after sciatic nerve transection. TUNEL staining and immunoblotting were used for analysis of cell apoptosis and axotomy-induced biochemical changes. Apoptosis of glial cells was observed at 24 h after sciatic nerve transection and increased on day 7, when apoptosis of some neurons only started. The earliest proapoptotic event in the injured DRG was overexpression of transcription factor E2F1 at 4 h after sciatic nerve transection. This preceded the induction of p53 and cleavage of caspase 3 at 24-h post-axotomy. The nerve injury marker amyloid precursor protein and the nerve regeneration marker GAP-43 were overexpressed in DRG on day 7 after sciatic nerve transection. We also developed a novel fluorescence method for differential visualization of the rat DRG and nerves by means of double staining with propidium iodide and Hoechst 33342 that impart red and blue-green fluorescence, respectively. The present experiments showed that glial cells remote from the nerve transection site were more vulnerable to axotomy than DRG neurons. E2F1 and p53 may be considered promising molecular targets for development of potential neuroprotective agents.






Similar content being viewed by others
References
Atlasi MA, Mehdizadeh M, Bahadori MH, Joghataei MT (2009) Morphological identification of cell death in dorsal root ganglion neurons following peripheral nerve injury and repair in adult rat. Iran Biomed J 13:65–72
Aubrey BJ, Kelly GL, Janic A, Herold MJ, Strasser A (2018) How does p53 induce apoptosis and how does this relate to p53-mediated tumour suppression? Cell Death Differ 25:104–113. https://doi.org/10.1038/cdd.2017.169
Barron KD (2004) The axotomy response. J Neurol Sci 220:119–121. https://doi.org/10.1016/j.jns.2004.03.009
Berezhnaya EV, Bibov MY, Komandirov MA, Neginskaya MA, Rudkovskii MV, Uzdensky AB (2017) Involvement of MAPK, Akt/GSK-3β and AMPK/mTOR signaling pathways in protection of remote glial cells from axotomy-induced necrosis and apoptosis in the isolated crayfish stretch receptor. Mol Cell Neurosci 83:1–5. https://doi.org/10.1016/j.mcn.2017.06.003
Bornstein N, Poon WS (2012) Accelerated recovery from acute brain injuries: clinical efficacy of neurotrophic treatment in stroke and traumatic brain injuries. Drugs Today 48(Suppl A):43–61. https://doi.org/10.1358/dot.2012.48(Suppl.A).1739723
Casas C, Isus L, Herrando-Grabulosa M, Mancuso FM, Borrás E, Sabidó E, Forés J, Aloy P (2015) Network-based proteomic approaches reveal the neurodegenerative, neuroprotective and pain-related mechanisms involved after retrograde axonal damage. Sci Rep 5:9185. https://doi.org/10.1038/srep09185
Corrigan F, Thornton E, Roisman LC, Leonard AV, Vink R, Blumbergs PC, van den Heuvel C, Cappai R (2014) The neuroprotective activity of the amyloid precursor protein against traumatic brain injury is mediated via the heparin binding site in residues 96-110. J Neurochem 128:196–204. https://doi.org/10.1111/jnc.12391
Demyanenko S, Dzreyan V, Uzdensky A (2019) Axotomy-induced changes of the protein profile in the crayfish ventral cord ganglia. J Mol Neurosci 68:667–678. https://doi.org/10.1007/s12031-019-01329-5
Dubový P, Klusáková I, Hradilová-Svíženská I, Joukal M (2018) Expression of regeneration-associated proteins in primary sensory neurons and regenerating axons after nerve injury-an overview. Anat Rec (Hoboken) 301:1618–1627. https://doi.org/10.1002/ar.23843
Engelmann D, Pützer BM (2010) Translating DNA damage into cancer cell death-A roadmap for E2F1 apoptotic signalling and opportunities for new drug combinations to overcome chemoresistance. Drug Resist Updates 13:119–131. https://doi.org/10.1016/j.drup.2010.06.001
Faulkner JR, Herrmann JE, Woo MJ, Tansey KE, Doan NB, Sofroniew MV (2004) Reactive astrocytes protect tissue and preserve function after spinal cord injury. J Neurosci 24:2143–2155. https://doi.org/10.1523/JNEUROSCI.3547-03.2004
Fedorenko GM, Uzdensky AB (2009) Cellular structures involved in the transport processes and neuroglial interactions in the crayfish stretch receptor. J Integr Neurosci 8:433–440
Hill CS (2016) Traumatic axon injury: mechanisms and translational opportunities. Trends Neurosci 39:311–324. https://doi.org/10.1016/j.tins.2016.03.002
Hughes PE, Alexi T, Walton M, Williams CE, Dragunow M, Clark RG, Gluckman PD (1999) Activity and injury-dependent expression of inducible transcription factors, growth factors and apoptosis-related genes within the central nervous system. Prog Neurobiol 57:421–450. https://doi.org/10.1016/s0301-0082(98)00057-4
Julius D, Basbaum AI (2001) Molecular mechanisms of nociception. Nature 413:203–210. https://doi.org/10.1038/35093019
Khaitin AM, Rudkovskii MV, Uzdensky AB (2015) The method of isolation of the crayfish abdominal stretch receptor maintaining a connection of the sensory neuron to the ventral nerve cord ganglion. Invertebr Neurosci 15:1–10. https://doi.org/10.1007/s10158-014-0176-2
Khaitin A, Rudkovskii M, Uzdensky A (2018) Ca2+ mediates axotomy-induced necrosis and apoptosis of satellite glial cells remote from the transection site in the isolated crayfish mechanoreceptor. Mol Cell Neurosci 88:7–15. https://doi.org/10.1016/j.mcn.2017.12.004
Kiryu-Seo S, Hirayama T, Kato R, Kiyama H (2005) Noxa is a critical mediator of p53-dependent motor neuron death after nerve injury in adult mouse. J Neurosci 25:1442–1447. https://doi.org/10.1523/JNEUROSCI.4041-04.2005
Kolosov M, Uzdensky A (2006) Crayfish mechanoreceptor neuron prevents photoinduced apoptosis of satellite glial cells. Brain Res Bull 69:495–500. https://doi.org/10.1016/j.brainresbull.2006.02.018
Laskowitz D, Grant G (eds) (2016) Translational Research in Traumatic Brain Injury. CRC Press/Taylor and Francis Group, Boca Raton (FL)
Lawson SN (1979) The postnatal development of large light and small dark neurons in mouse dorsal root ganglia: a statistical analysis of cell numbers and size. J Neurocytol 8:275–294. https://doi.org/10.1007/BF01236123
Lebrun-Julien F, Suter U (2015) Combined HDAC1 and HDAC2 depletion promotes retinal ganglion cell survival after injury through reduction of p53 target gene expression. ASN Neuro 7(3):175909141559306. https://doi.org/10.1177/1759091415593066
Li GL, Farooque M, Holtz A, Olsson Y (1999) Apoptosis of oligodendrocytes occurs for long distances away from the primary injury after compression trauma to rat spinal cord. Acta Neuropathol 98:473–480. https://doi.org/10.1007/s004010051112
Liu B, Teschemacher AG, Kasparov S (2017) Neuroprotective potential of astroglia. J Neurosci Res 95:2126–2139. https://doi.org/10.1002/jnr.24140
Liu XZ, Xu XM, Hu R, Du C, Zhang SX, McDonald JW, Dong HX, Wu YJ, Fan GS, Jacquin MF, Hsu CY, Choi DW (1997) Neuronal and glial apoptosis after traumatic spinal cord injury. J Neurosci 17:5395–5406. https://doi.org/10.1523/JNEUROSCI.17-14-05395.1997
Ma L, Yu HJ, Gan SW, Gong R, Mou KJ, Xue J, Sun SQ (2017) p53-Mediated oligodendrocyte apoptosis initiates demyelination after compressed spinal cord injury by enhancing ER-mitochondria interaction and E2F1 expression. Neurosci Lett 644:55–61. https://doi.org/10.1016/j.neulet.2017.02.038
Maxwell WL, Donnelly S, Sun X, Fenton T, Puri N, Graham DI (1999) Axonal cytoskeletal responses to nondisruptive axonal injury and the short-term effects of posttraumatic hypothermia. J Neurotrauma1 6:1225–1234. https://doi.org/10.1089/neu.1999.16.1225
McKay Hart A, Brannstrom T, Wiberg M, Terenghi G (2002) Primary sensory neurons and satellite cells after peripheral axotomy in the adult rat. Time course of cell death and elimination. Exp Brain Res 142:308–318. https://doi.org/10.1007/s00221-001-0929-0
Melle C, Ernst G, Grosheva M, Angelov DN, Irintchev A, Guntinas-Lichius O, von Eggeling F (2009) Proteomic analysis of microdissected facial nuclei of the rat following facial nerve injury. J Neurosci Methods 185:23–28. https://doi.org/10.1016/j.jneumeth.2009.09.003
Meng P, Ghosh R (2014) Transcription addiction: can we garner the Yin and Yang functions of E2F1 for cancer therapy? Cell Death Disease 5:e1360. https://doi.org/10.1038/cddis.2014.326
Momeni HR, Soleimani Mehranjani M, Shariatzadeh MA, Haddadi M (2013) Caspase-mediated apoptosis in sensory neurons of cultured dorsal root ganglia in adult mouse. Cell J 15:212–217
Mulder J, Wernérus H, Shi TJ, Pontén F, Hober S, Uhlén M, Hökfelt T (2007) Systematically generated antibodies against human gene products: high throughput screening on sections from the rat nervous system. Neuroscience 146:1689–1703. https://doi.org/10.1016/j.neuroscience.2007.02.054
Muresan V, Ladescu Muresan Z (2015) Amyloid-β precursor protein: Multiple fragments, numerous transport routes and mechanisms. Exp Cell Res 334:45–53. https://doi.org/10.1016/j.yexcr.2014.12.014
Niu J, Li C, Wu H, Feng X, Su Q, Li S, Zhang L, Yew DTW, Cho EYP, Sha O (2015) Propidium iodide (PI) stains Nissl bodies and may serve as a quick marker for total neuronal cell count. Acta Histochem 117:182–187. https://doi.org/10.1016/j.acthis.2014.12.001
Patodia S, Raivich G (2012) Role of transcription factors in peripheral nerve regeneration. Front Mol Neurosci 5:8. https://doi.org/10.3389/fnmol.2012.00008
Pelengaris S, Khan M, Evan G (2002) c-MYC: more than just a matter of life and death. Nature Rev Cancer 2:764–776. https://doi.org/10.1038/nrc904
Perlson E, Hanz S, Medzihradszky KF, Burlingame AL, Fainzilber MJ (2004) From snails to sciatic nerve: retrograde injury signaling from axon to soma in lesioned neurons. Neurobiol 58:287–294. https://doi.org/10.1002/neu.10316
Plummer S, Van den Heuvel C, Thornton E, Corrigan F, Cappai R (2016) The Neuroprotective properties of the amyloid precursor protein following traumatic brain injury. Aging Dis 7:163–179. https://doi.org/10.14336/AD.2015.0907
Raimundo N, Song L, Shutt TE, McKay SE, Cotney J, Guan MX, Gilliland TC, Hohuan D, Santos-Sacchi J, Shade GS (2012) Mitochondrial stress engages E2F1 apoptotic signaling to cause deafness. Cell 148:716–726. https://doi.org/10.1016/j.cell.2011.12.027
Rishal I, Fainzilber M (2014) Axon-soma communication in neuronal injury. Nature Rev Neurosci 15:32–42. https://doi.org/10.1038/nrn3609
Savastano LE, Laurito SR, Fitt MR, Rasmussen JA, Gonzalez Polo V, Patterson S (2014) Sciatic nerve injury: a simple and subtle model for investigating many aspects of nervous system damage and recovery. J Neurosci Meth 227:166–180. https://doi.org/10.1016/j.jneumeth.2014.01.020
Schaeffer V, Meyer L, Patte-Mensah C, Eckert A, Mensah-Nyagan AG (2010) Sciatic nerve injury induces apoptosis of dorsal root ganglion satellite glial cells and selectively modifies neurosteroidogenesis in sensory neurons. Glia 58:169–180. https://doi.org/10.1002/glia.20910
Uzdensky AB (2018) Axotomy induces damage to glial cells remote from the transection site in the peripheral nervous system. Neural Reg Res 13:639–640. https://doi.org/10.4103/1673-5374.230285
Verkhratsky A, Ho MS, Zorec R, Parpura V (Editors) (2019) Neuroglia in neurodegenerative diseases (advances in experimental medicine and biology book (1175) Kindle Edition. Springer
Wan C, Ma X, Shi S, Zhao J, Nie X, Han J, Xiao J, Wang X, Jiang S, Jiang J (2014) Pivotal roles of p53 transcription-dependent and -independent pathways in manganese-induced mitochondrial dysfunction and neuronal apoptosis. Toxicol Appl Pharmacol 281:294–302. https://doi.org/10.1016/j.taap.2014.10.013
Wang J, Hamm RJ, Povlishock JT (2011) Traumatic axonal injury in the optic nerve: evidence for axonal swelling, disconnection, dieback, and reorganization. J Neurotrauma 28:1185–1198. https://doi.org/10.1089/neu.2011.1756
Wang DB, Kinoshita C, Kinoshita Y, Morrison RS (2014) p53 and mitochondrial function in neurons. Biochim Biophys Acta 1842:1186–1197. https://doi.org/10.1016/j.bbadis.2013.12.015
Whiteside G, Munglani R (1998) TUNEL, Hoechst and immunohistochemistry triple-labelling: an improved method for detection of apoptosis in tissue sections--an update. Brain Res Brain Res Protoc 3:52–53. https://doi.org/10.1016/s1385-299x(97)00032-9
Whiteside G, Doyle CA, Hunt SP, Munglani R (1998) Differential time course of neuronal and glial apoptosis in neonatal rat dorsal root ganglia after sciatic nerve axotomy. Eur J Neurosci 10:3400–3408. https://doi.org/10.1046/j.1460-9568.1998.00346.x
Witiw CD, Fehlings MG (2015) Acute spinal cord injury. J Spinal Disorder Techn 28:202–210. https://doi.org/10.1097/BSD.0000000000000287
Yakovlev AG, Faden AI (2001) Caspase-dependent apoptotic pathways in CNS injury. Mol Neurobiol 24:131–144. https://doi.org/10.1385/MN:24:1-3:131
Funding
The work was supported by the Ministry of Science and Higher Education of Russian Federation; grant #0852–2020-0028.
Author information
Authors and Affiliations
Contributions
Dzreyan V.A.: data generation and analysis (western blotting); Rodkin S.V.: data generation (DRG visualization, apoptosis study); Nikul V.V.: data generation (DRG visualization); Pitinova M.A.: design and data generation (fluorescence microscopy); Uzdensky A.B.: Supervision; Conceptualization; data analysis and interpretation, manuscript writing.
Corresponding author
Ethics declarations
Conflict of Interest
The authors declare that they have no conflict of interest. All authors agree to publish this paper.
Ethics Approval
The submitted work is original. It has not been published elsewhere and is not considered for publication and in any form or language (partially or in full).
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Dzreyan, V., Rodkin, S., Nikul, V. et al. The Expression of E2F1, p53, and Caspase 3 in the Rat Dorsal Root Ganglia After Sciatic Nerve Transection. J Mol Neurosci 71, 826–835 (2021). https://doi.org/10.1007/s12031-020-01705-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12031-020-01705-6