Abstract
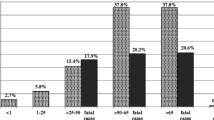
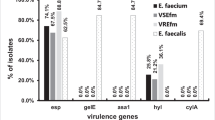
We determined the clinical and molecular epidemiology of emerging nosocomial vancomycin-resistant Enterococcus faecium (VREfm)–causing serious bloodstream infections (BSIs) and the correlations between antibiotic resistance and virulence determinants among isolates. All isolates were confirmed by molecular methods (16SrRNA and E. faecium ddl genes) and tested for disk diffusion. PCR was used to detect aac(6′)-aph(2″), vanA and vanB resistance genes, and asa1, cylA, ace, esp, gelE and hyl virulence genes. VREfm and high-level gentamicin-resistant (HLGR) representative isolates were selected to characterize by pulsed-field gel electrophoresis (PFGE) and multi-locus sequence typing (MLST). Of 173 isolates, 73 (42.2%), 146 (84.4%), and 0 (0.0%) were vanA-containing VREfm, aac(6′)-aph(2″)–positive HLGR, and vanB-positive. Independent predictors of VREfm infection were hematological malignancies (P = 0.001) and previous hospitalizations (P = 0.007). Observed mortality rate was 34.7%. Independent predictors of BSI-related mortality were endotracheal intubations (P < 0.001), gastrointestinal diseases (P = 0.002), and pulmonary disease (P < 0.001). All VREfm were resistant to vancomycin, teicoplanin, ciprofloxacin, and erythromycin. The esp, hyl, ace, asa1, cylA, and gelE genes were detected at 55.9, 22.5, 2.9, 2.3, 1.7, and 1.2%, respectively. The esp gene was significantly associated with VREfm compared to VSEfm (P = 0.001). PFGE analysis revealed 23 clones, with 7 major clones. The MLST analysis revealed the following five sequence types: ST80, ST17, ST117, ST132, and ST280, all belonging to CC17. The emergence and expansion of VREfm CC17 with limited antibiotic options in our hospital present a serious public health menace and represent challenges to infection control.

Similar content being viewed by others
References
Sievert DM, Ricks P, Edwards JR et al (2013) Antimicrobial-resistant pathogens associated with healthcare-associated infections: summary of data reported to the National Healthcare Safety Network at the Centers for Disease Control and Prevention, 2009–2010. Infect Control Hosp Epidemiol 34(1):1–14
Pinholt M, Ostergaard C, Arpi M et al (2014) Incidence, clinical characteristics and 30-day mortality of enterococcal bacteraemia in Denmark 2006–2009: a population-based cohort study. Clin Microbiol Infect 20(2):145–151
Willems RJ, Top J, van Santen M et al (2005) Global spread of vancomycin-resistant Enterococcus faecium from distinct nosocomial genetic complex. Emerg Infect Dis 11(6):821–828
Cattoir V, Leclercq R (2013) Twenty-five years of shared life with vancomycin-resistant enterococci: is it time to divorce? J Antimicrob Chemother 68(4):731–742
Hammerum AM, Baig S, Kamel Y et al (2017) Emergence of vanA Enterococcus faecium in Denmark, 2005–15. J Antimicrob Chemother 72(8):2184–2190
Magiorakos AP, Srinivasan A, Carey RB et al (2012) Multidrug-resistant, extensively drug-resistant and pandrug-resistant bacteria: an international expert proposal for interim standard definitions for acquired resistance. Clin Microbiol Infect 18(3):268–281
Billström H, Lund B, Sullivan A, Nord CE (2008) Virulence and antimicrobial resistance in clinical Enterococcus faecium. Int J Antimicrob Agents 32(5):374–377
Vankerckhoven V, Van Autgaerden T, Vael C et al (2004) Development of a multiplex PCR for the detection of asa1, gelE, cylA, esp, and hyl genes in enterococci and survey for virulence determinants among European hospital isolates of Enterococcus faecium. J Clin Microbiol 42(10):4473–4479
Treitman AN, Yarnold PR, Warren J, Noskin GA (2005) Emerging incidence of Enterococcus faecium among hospital isolates (1993 to 2002). J Clin Microbiol 43(1):462–463
Coombs GW, Pearson JC, Daley DA et al (2014) Molecular epidemiology of enterococcal bacteremia in Australia. J Clin Microbiol 52(3):897–905
Billström H, Top J, Edlund C, Lund B (2010) Frequent occurrence of multidrug-resistant CC17 Enterococcus faecium among clinical isolates in Sweden. J Appl Microbiol 108(5):1810–1816
Charlson ME, Pompei P, Ales KL, MacKenzie CR (1987) A new method of classifying prognostic comorbidity in longitudinal studies: development and validation. J Chronic Dis 40(5):373–383
McCabe WR, Jackson GG (1962) Gram-negative bacteremia: I. Etiology and ecology. Arch Intern Med 110:845–847
Van deKlundert JAM, Vliegenthart JS (1993) PCR detection of genes coding for aminoglycoside-modifying enzymes. In: Persing DH, Smith TF, Tenover FC, White TJ (eds) Diagnostic molecular microbiology. ASM Press, Washington, pp 547–552
Depardieu F, Perichon B, Courvalin P (2004) Detection of the van alphabet and identification of enterococci and staphylococci at the species level by multiplex PCR. J Clin Microbiol 42(12):5857–5860
Clinical and Laboratory Standards Institute (2012) Performance standards for antimicrobial susceptibility testing; twentieth informational supplement M100-S22. CLSI, Wayne
Yean CY, Yin LS, Lalitha P, Ravichandran M (2007) A nanoplex PCR assay for the rapid detection of vancomycin and bifunctional aminoglycoside resistance genes in Enterococcus species. BMC Microbiol 7:112
Dhawan B, Rao C, Udo EE, Gadepalli R, Vishnubhatla S, Kapil A (2015) Dissemination of methicillin-resistant Staphylococcus aureus SCCmec type IV and SCCmec type V epidemic clones in a tertiary hospital: challenge to infection control. Epidemiol Infect 143(2):343–353
Udo EE, Al-Mufti S, Albert MJ (2009) The prevalence of antimicrobial resistance and carriage of virulence genes in Staphylococcus aureus isolated from food handlers in Kuwait City restaurants. BMC Res Notes 2:108
Tzavaras I, Siarkou VI, Zdragas A et al (2012) Diversity of vanA-type vancomycin-resistant Enterococcus faecium isolated from broilers, poultry slaughterers and hospitalized humans in Greece. J Antimicrob Chemother 67(8):1811–1818
Homan WL, Tribe D, Poznanski S et al (2002) Multilocus sequence typing scheme for Enterococcus faecium. J Clin Microbiol 40(6):1963–1971
Enterococcus faecium MLST website. (https://pubmlst.org/efaecium/) sited at the University of Oxford (Jolley et al. Wellcome Open Res 2018, 3:124 [version 1; referees: 2 approved])
Mathur P, Chaudhary R, Dhawan B, Sharma N (1999) Vancomycin-resistant Enterococcus bacteraemia in a lymphoma patient. Indian J Med Microbiol 17:194–195
Mathur P, Kapil A, Chandra R, Sharma P, Das B (2003) Antimicrobial resistance in Enterococcus faecalis at a tertiary care centre of northern India. Indian J Med Res 118:25–28
Dhawan B, Gadepalli R, Rao C, Kapil A, Sreenivas V (2010) Decreased susceptibility to vancomycin in meticillin-resistant Staphylococcus aureus: a 5-year study in an Indian tertiary hospital. J Med Microbiol 59(Pt 3):375–376
Peel T, Cheng AC, Spelman T, Huysmans M, Spelman D (2012) Differing risk factors for vancomycin-resistant and vancomycin-sensitive enterococcal bacteraemia. Clin Microbiol Infect 18(4):388–394
Rangberg A, Larsen AL, Kacelnik O et al (2019) Molecular analysis and epidemiological typing of vancomycin-resistant Enterococcus outbreak strains. Sci Rep 9(1):11917
McCracken M, Wong A, Mitchell R et al (2013) Molecular epidemiology of vancomycin-resistant enterococcal bacteraemia: results from the Canadian Nosocomial Infection Surveillance Program, 1999–2009. J Antimicrob Chemother 68(7):1505–1509
Wardenburg KE, Potter RF, D'Souza AW et al (2019) Phenotypic and genotypic characterization of linezolid-resistant Enterococcus faecium from the USA and Pakistan. J Antimicrob Chemother 74(12):3445–3452
Hegstad K, Mikalsen T, Coque TM, Werner G, Sundsfjord A (2010) Mobile genetic elements and their contribution to the emergence of antimicrobial resistant Enterococcus faecalis and Enterococcus faecium. Clin Microbiol Infect 16(6):541–554
Østergaard L, Bruun NE, Voldstedlund M et al (2019) Prevalence of infective endocarditis in patients with positive blood cultures: a Danish nationwide study. Eur Heart J 40(39):3237–3244
Acknowledgments
We thank H. Billstrom, V. Vankerckhoven, M. Ravichandran, C. Y. Yean, Claverie-Martín, and E. E. Udo for the gift reference strains. This work was completed as part of Dr. Chandranhan Rao’s Ph.D. thesis.
Funding
This work was supported by the Indian Council of Medical Research (ICMR), New Delhi, India (Project File No.: 5/3/3/10/2011-ECD-I).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval and informed consent
This study was approved by the Ethics Committee of the AIIMS, New Delhi, India (Ref. No.: IEST/T-151/2010). The informed consent of each patient included in this study was obtained.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Rao, C., Dhawan, B., Vishnubhatla, S. et al. Clinical and molecular epidemiology of vancomycin-resistant Enterococcus faecium bacteremia from an Indian tertiary hospital. Eur J Clin Microbiol Infect Dis 40, 303–314 (2021). https://doi.org/10.1007/s10096-020-04030-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10096-020-04030-3