Abstract
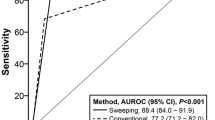
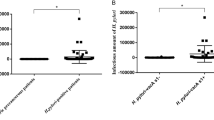
Background: Helicobacter pylori (H. pylori) is one of the most prevalent pathogenic bacteria globally. Choosing reliable methods will lead to a correct diagnosis of infection. The aim of this study was to evaluate four H. pylori infection diagnostic methods from dispeptic patients. Methods: In this descriptive cross-sectional study, 165 antrum biopsy specimens were obtained from dyspeptic patients referred to the endoscopy unit of Shariati Hospital, Isfahan, Iran, and collected in 2018. Four diagnostic methods of H. pylori, namely histology, culture, rapid urease test (RUT) and fluorescence in situ hybridisation (FISH) were tested for each patient. The gold standard of the study was for positive confirming one of the two tests, RUT or histology. Results: According to the predefined criteria, the prevalence of H. pylori infection was 55.2%. Among the four diagnostic methods, the most sensitive ones were FISH and RUT, respectively (95.7 and 92.3%). Despite the high specificity of the histological examination (100%), its NPV was lower than the other methods (88%). The kappa coefficient of agreement between the gold standard and the tested techniques was perfect (P < 0.001). Conclusion: FISH and histology are recommended in combination with diagnosis of H. pylori infection, which can manage its complications in the most optimal manner.

Similar content being viewed by others
REFERENCES
Kalali, B., Formichella, L., and Gerhard, M., Diagnosis of Helicobacter pylori: Changes towards the future, Diseases, 2015, vol. 3, pp. 122–135.
Mandal, A.K., Kafle, P., Puri, P., Chaulagai, B., Sidhu, J.S., and Hassan, M., An association of Helicobacter pylori infection with endoscopic and histological findings in the Nepalese population, J. Fam. Med. Primary Care, 2019, vol. 8, p. 1227.
Yantiss, R.K. and Lamps, L.W., To stain or not to stain… that remains the question, Am. J. Clin. Pathol., 2012, vol. 137, pp. 343–345.
Contreras, M., Salazar, V., García-Amado, M.A., Reyes, N., Aparcero, M., and Silva, O., High frequency of Helicobacter pylori in the esophageal mucosa of dyspeptic patients and its possible association with histopathological alterations, Int. J. Infect. Dis., 2012, vol. 16, pp. 364–370.
Khalifehgholi, M., Shamsipour, F., Ajhdarkosh, H., Daryani, N.E., Pourmand, M.R., and Hosseini, M., Comparison of five diagnostic methods for Helicobacter pylori,Iran. J. Microbiol., 2013, vol. 5, p. e396.
Fakheri, H., Firoozi, M.S., and Bari, Z., Eradication of Helicobacter pylori in Iran: A review, Middle East J. Dig. Dis., 2018, vol. 10, p. e5.
Talebi Bezmin Abadi, A., Diagnosis of Helicobacter pylori using invasive and noninvasive approaches, J. Pathog., 2018, vol. 2018, pp. 1–13.
Pastukh, N., Binyamin, D., On, A., Paritsky, M., and Peretz, A., GenoType® Helico DR test in comparison with histology and culture for Helicobacter pylori detection and identification of resistance mutations to clarithromycin and fluoroquinolones, Helicobacter, 2017, vol. 22, p. e12 447.
Patel, S.K., Pratap, C.B., Jain, A.K., Gulati, A.K., and Nath, G., Diagnosis of Helicobacter pylori: What should be the gold standard?, World J. Gastroenterol., 2014, vol. 20, p. e12 847.
Nafisi, M.R., Alipour, S.M., Karimi, A., Rahimian, G.A., and Imani, F.A., PCR and RFLP of ureC (glmM) gene for identification and typing of Helicobacter pylori strains isolated from gastric biopsy specimens of gastric patients, Kowsar Med. J., 2009, vol. 14, pp. 143–148.
Trebesius, K., Panthel, K., Strobel, S., Vogt, K., Faller, G., and Kirchner, T., Rapid and specific detection of Helicobacter pylori macrolide resistance in gastric tissue by fluorescent in situ hybridization, Gut, 2000, vol. 46, pp. 608–614.
Demiray-Gürbüz, E., Yılmaz, Ö., Olivares, A.Z., Gönen, C., Sarıoğlu, S., and Soytürk, M., Rapid identification of Helicobacter pylori and assessment of clarithromycin susceptibility from clinical specimens using FISH, J. Pathol., 2017, vol. 3, pp. 29–37.
Redéen, S., Petersson, F., Törnkrantz, E., Levander, H., Mårdh, E., and Borch, K., Reliability of diagnostic tests for Helicobacter pylori infection, Gastroenterol. Res. Pract., 2011, vol. 2011, pp. 1–6.
Garza-González, E., Perez-Perez, G.I., Maldonado-Garza, H.J., and Bosques-Padilla, F.J., A review of Helicobacter pylori diagnosis, treatment, and methods to detect eradication, World J. Gastroenterol., 2014, vol. 20, p. 1438.
Tzeng, J.-E., Lin, Y.-L., Chung, S.-M., and Chu, Y.-T., Comparison of four diagnostic methods for Helicobacter pylori,Tzu Chi Med. J., 2005, vol. 17, pp. 339–343.
Kocsmár, É., Szirtes., I., Kramer, Z., Szijártó, A., Bene, L., and Buzás, G.M., Sensitivity of Helicobacter pylori detection by Giemsa staining is poor in comparison with immunohistochemistry and fluorescent in situ hybridization and strongly depends on inflammatory activity, Helicobacter, 2017, vol. 22, p. 12387.
Aftab, H., Yamaoka, Y., Ahmed, F., Khan, A.A., Subsomwong, P., and Miftahussurur, M., Validation of diagnostic tests and epidemiology of Helicobacter pylori infection in Bangladesh, J. Infect. Dev. Countries, 2018, vol. 12, pp. 305–312.
Tongtawee, T., Kaewpitoon, S., Kaewpitoon, N., Dechsukhum, C., Leeanansaksiri, W., and Loyd, A., Diagnosis of Helicobacter pylori infection, Asian Pac. J. Cancer Prev., 2016, vol. 17, pp. 1631–1635.
Lopes, A.I., Vale, F.F., and Oleastro, M., Helicobacter pylori infection: Recent developments in diagnosis, World J. Gastroenterol., 2014, vol. 20, p. e9299.
Ramis, I.B., Moraes, E.Pd., Fernandes, M.S., Mendoza-Sassi, R., Rodrigues, O., and Juliano, C.R.V., Evaluation of diagnostic methods for the detection of Helicobacter pylori in gastric biopsy specimens of dyspeptic patients, Braz. J. Microbiol., 2012, vol. 43, pp. 903–908.
Mnena, E., Emmanuel, N., and Ega, R., Assessing the reliability of PCR, microbiological and histologic methods in detecting Helicobacter pylori in gastric biopsies, J. Biomed. Sci., 2017, vol. 6, p. 32.
Peretz, A., On, A., Koifman, A., Brodsky, D., Isakovich, N., and Glyatman, T., An efficiency comparison between three invasive methods for the diagnosis of Helicobacter pylori infections: culture from stomach biopsy, rapid urease test (CUTest®), and histologic examination of gastric biopsy, Ann. Clin. Lab. Sci., 2015, vol. 45, pp. 148–151.
Frickmann, H., Zautner, A.E., Moter, A., Kikhney, J., Hagen, R.M., and Stender, H., Fluorescence in situ hybridization (FISH) in the microbiological diagnostic routine laboratory: a review, Crit. Rev. Microbiol., 2017, vol. 43, pp. 263–293.
Ciftci, I.H., Ugras, M., and Acarturk, G., Comparison of FISH, RFLP and agar dilution methods for testing clarithromycin resistance of Helicobacter pylori,Turk. J. Gastroenterol., 2014, vol. 25, pp. 75–80.
Samarbaf-Zadeh, A.R., Tajbakhsh, S., Moosavian, S.M., Sadeghi-Zadeh, M., Azmi, M., and Hashemi, J., Application of fluorescent in situ hybridization (FISH) for the detection of Helicobacter pylori,Med. Sci. Monit., 2006, vol. 12, pp. CR426–CR430.
Funding
This study was supported by Department of Microbiology, Faculty of Medicine, Isfahan University of Medical Sciences, Isfahan, Iran. Grant no. 127639.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interests. The authors declare that they have no conflict of interest.
Statement of compliance with standards of research involving humans as subjects. The study was approved by the Ethics Committee of Isfahan University of Medical Sciences, and the patients declared their consent.
About this article
Cite this article
Jina Vazirzadeh, Moghim, S., Falahi, J. et al. Comparison of Four Invasive Methods for Diagnosis of Helicobacter pylori Infection: Fluorescence in situ Hybridization, Histology, Culture, Rapid Urease Test. Mol. Genet. Microbiol. Virol. 35, 123–128 (2020). https://doi.org/10.3103/S0891416820020111
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.3103/S0891416820020111