Abstract
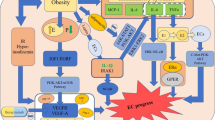
As the obesity rates dramatically increased across the globe, the risk of endometrial cancer (EC) has substantially increased. Measures to improve the EC outcome is utmost important, especially data have shown that women at their reproductive age are commonly affected. No doubt, surgical intervention is a standard treatment for EC. However, the fact that this cancer could arise from metabolic diseases, additional therapy by lipid-lowering agent could be utilized to change the tumour environment. We review available evidence to support the use of this agent in the clinical setting. We search available evidence on the use of statin in EC, in various settings including cell lines, animal and human study. The possible actions at different molecular pathways leading to cellular changes and proliferation of cell were evaluated. The venture in drug repositioning of statins as a chemo-preventive potential agent in EC has gained attention in gynaecological oncology practice worldwide. Lipid-lowering effect by statins may exerted a chemoprotective effect in EC, but there is still lack of evidence on statins use to improve prognosis and survival in EC. Through the cholesterol-lowering effect of statins; theoretically, it could inhibit cell growth, proliferation, migration, and lead to apoptosis. Epidemiological studies suggested that statins may improve survival rate among EC patients. However, some evidence revealed the effects were only more prominent in type II EC. Notwithstanding that several studies also showed no benefit of statins in EC. Hence we highlight the limitations of these studies in this review. In line with recent literature on the topic, statins may play a role in EC management. Future studies for a proper systematic review and randomized controlled study are needed to answer some uncertainties of statins effect in EC.


Similar content being viewed by others
References
Bray F, Ferlay J, Soerjomataram I, Siegel RL, Torre LA, Jemal A (2018) Global cancer statistics 2018: GLOBOCAN estimates of incidence and mortality worldwide for 36 cancers in 185 countries. CA Cancer J Clin 68(6):394–424. https://doi.org/10.3322/caac.21492
Ferlay J, Soerjomataram I, Dikshit R, Eser S, Mathers C, Rebelo M, Parkin DM, Forman D, Bray F (2015) Cancer incidence and mortality worldwide: sources, methods and major patterns in GLOBOCAN 2012. Int J Cancer 136(5):E359–E386. https://doi.org/10.1002/ijc.29210
Kitson SJ, Lindsay J, Sivalingam VN, Lunt M, Ryan NAJ, Edmondson RJ, Rutter MK, Crosbie EJ (2018) The unrecognized burden of cardiovascular risk factors in women newly diagnosed with endometrial cancer: a prospective case control study. Gynecol Oncol 148(1):154–160. https://doi.org/10.1016/j.ygyno.2017.11.019
Onstad MA, Schmandt RE, Lu KH (2016) Addressing the role of obesity in endometrial cancer risk, prevention, and treatment. J Clin Oncol 34(35):4225–4230. https://doi.org/10.1200/JCO.2016.69.4638
Esposito K, Chiodini P, Colao A, Lenzi A, Giugliano D (2012) Metabolic syndrome and risk of cancer: a systematic review and meta-analysis. Diabetes Care 35(11):2402–2411. https://doi.org/10.2337/dc12-0336
Ward KK, Shah NR, Saenz CC, McHale MT, Alvarez EA, Plaxe SC (2012) Cardiovascular disease is the leading cause of death among endometrial cancer patients. Gynecol Oncol 126(2):176–179. https://doi.org/10.1016/j.ygyno.2012.04.013
Bogani G, Dowdy SC, Cliby WA, Ghezzi F, Rossetti D, Frigerio L, Mariani A (2016) Management of endometrial cancer: issues and controversies. Eur J Gynaecol Oncol 37(1):6–12
Shim JS, Liu JO (2014) Recent advances in drug repositioning for the discovery of new anticancer drugs. International Journal of Biological Sciences 10(7):654–663. https://doi.org/10.7150/ijbs.9224
Long J, Zhang C-J, Zhu N, Du K, Yin Y-F, Tan X, Liao D-F, Qin L (2018) Lipid metabolism and carcinogenesis, cancer development. Am J Cancer Res 8(5):778–791
Bottorff MB (2006) Statin safety and drug interactions: clinical implications. Am J Cardiol 97(8):S27–S31. https://doi.org/10.1016/j.amjcard.2005.12.007
Matusewicz L, Meissner J, Toporkiewicz M, Sikorski AF (2015) The effect of statins on cancer cells—review. Tumor Biol 36(7):4889–4904. https://doi.org/10.1007/s13277-015-3551-7
Rutishauser J (2011) Statins in clinical medicine. Swiss Med Wkly 141:w13310
Kato S, Smalley S, Sadarangani A, Chen-Lin K, Oliva B, Brañes J, Carvajal J, Gejman R, Owen GI, Cuello M (2010) Lipophilic but not hydrophilic statins selectively induce cell death in gynaecological cancers expressing high levels of HMGCoA reductase. J Cell Mol Med 14(5):1180–1193. https://doi.org/10.1111/j.1582-4934.2009.00771.x
Baker WL, Talati R, White CM, Coleman CI (2010) Differing effect of statins on insulin sensitivity in non-diabetics: a systematic review and meta-analysis. Diabetes Res Clin Pract 87(1):98–107. https://doi.org/10.1016/j.diabres.2009.10.008
van Stee MF, de Graaf AA, Groen AK (2018) Actions of metformin and statins on lipid and glucose metabolism and possible benefit of combination therapy. Cardiovasc Diabetol 17(1):94. https://doi.org/10.1186/s12933-018-0738-4
Chen H-H, Lin M-C, Muo C-H, Yeh S-Y, Sung F-C, Kao C-H (2015) Combination therapy of metformin and statin may decrease hepatocellular carcinoma among diabetic patients in Asia. Medicine 94(24):e1013. https://doi.org/10.1097/md.0000000000001013
Yeganeh B, Wiechec E, Ande SR, Sharma P, Moghadam AR, Post M, Freed DH, Hashemi M, Shojaei S, Zeki AA, Ghavami S (2014) Targeting the mevalonate cascade as a new therapeutic approach in heart disease, cancer and pulmonary disease. Pharmacol Ther 143(1):87–110. https://doi.org/10.1016/j.pharmthera.2014.02.007
Ding X, Zhang W, Li S, Yang H (2019) The role of cholesterol metabolism in cancer. Am J Cancer Res 9(2):219–227
Sonia NA, Reneta AT, Albena BM, Rumiana DT (2016) Statins and alkylphospholipids as new anticancer agents targeting lipid metabolism. Anticancer Agents Med Chem 16(12):1512–1522. https://doi.org/10.2174/1871520616666160624093955
Warita K, Warita T, Beckwitt CH, Schurdak ME, Vazquez A, Wells A, Oltvai ZN (2014) Statin-induced mevalonate pathway inhibition attenuates the growth of mesenchymal-like cancer cells that lack functional E-cadherin mediated cell cohesion. Scientific reports 4:7593
Tsubaki M, Takeda T, Kino T, Obata N, Itoh T, Imano M, Mashimo K, Fujiwara D, Sakaguchi K, Satou T, Nishida S (2015) Statins improve survival by inhibiting spontaneous metastasis and tumor growth in a mouse melanoma model. Am J Cancer Res 5(10):3186–3197
Schointuch MN, Gilliam TP, Stine JE, Han X, Zhou C, Gehrig PA, Kim K, Bae-Jump VL (2014) Simvastatin, an HMG-CoA reductase inhibitor, exhibits anti-metastatic and anti-tumorigenic effects in endometrial cancer. Gynecol Oncol 134(2):346–355. https://doi.org/10.1016/j.ygyno.2014.05.015
Kim JS, Turbov J, Rosales R, Thaete LG, Rodriguez GC (2019) Combination simvastatin and metformin synergistically inhibits endometrial cancer cell growth. Gynecol Oncol 154(2):432–440. https://doi.org/10.1016/j.ygyno.2019.05.022
Beckwitt CH, Clark AM, Ma B, Whaley D, Oltvai ZN, Wells A (2018) Statins attenuate outgrowth of breast cancer metastases. Br J Cancer 119(9):1094–1105. https://doi.org/10.1038/s41416-018-0267-7
Cho S-J, Kim JS, Kim JM, Lee JY, Jung HC, Song IS (2008) Simvastatin induces apoptosis in human colon cancer cells and in tumor xenografts, and attenuates colitis-associated colon cancer in mice. Int J Cancer 123(4):951–957. https://doi.org/10.1002/ijc.23593
Kodach LL, Bleuming SA, Peppelenbosch MP, Hommes DW, van den Brink GR, Hardwick JCH (2007) The effect of statins in colorectal cancer is mediated through the bone morphogenetic protein pathway. Gastroenterology 133(4):1272–1281. https://doi.org/10.1053/j.gastro.2007.08.021
Yasui Y, Suzuki R, Miyamoto S, Tsukamoto T, Sugie S, Kohno H, Tanaka T (2007) A lipophilic statin, pitavastatin, suppresses inflammation-associated mouse colon carcinogenesis. Int J Cancer 121(10):2331–2339. https://doi.org/10.1002/ijc.22976
Lee KY, Jeong J-W, Wang J, Ma L, Martin JF, Tsai SY, Lydon JP, DeMayo FJ (2007) Bmp2 is critical for the murine uterine decidual response. Mol Cell Biol 27(15):5468–5478. https://doi.org/10.1128/mcb.00342-07
Jacobs EJ, Newton CC, Thun MJ, Gapstur SM (2011) Long-term use of cholesterol-lowering drugs and cancer incidence in a large United States cohort. Can Res 71(5):1763–1771. https://doi.org/10.1158/0008-5472.Can-10-2953
Sperling CD, Verdoodt F, Kjær Hansen M, Dehlendorff C, Friis S, Kjaer SK (2018) Statin use and mortality among endometrial cancer patients: a Danish nationwide cohort study. International journal of cancer 143(11):2668–2676
Li J, Liu R, Sun Z, Tang S, Wang L, Liu C, Zhao W, Yao Y, Sun C (2018) The association between statin use and endometrial cancer survival outcome: a meta-analysis. Med (Baltim) 97(47):e13264. https://doi.org/10.1097/MD.0000000000013264
Arima R, Marttila M, Hautakoski A, Arffman M, Sund R, Ilanne-Parikka P, Kangaskokko J, Urpilainen E, Läärä E, Hinkula M (2018) Antidiabetic medication, statins and the risk and prognosis of non-endometrioid endometrial cancer in women with type 2 diabetes. Anticancer Res 38(7):4169–4178
Feng CH, Miller CM, Tenney ME, Lee NK, Yamada SD, Hasan Y (2016) Statin use significantly improves overall survival in high-grade endometrial cancer. Int J Gynecol Cancer 26(9):1642–1649. https://doi.org/10.1097/igc.0000000000000819
Lavie O, Pinchev M, Rennert HS, Segev Y, Rennert G (2013) The effect of statins on risk and survival of gynecological malignancies. Gynecol Oncol 130(3):615–619. https://doi.org/10.1016/j.ygyno.2013.05.025
Nevadunsky NS, Van Arsdale A, Strickler HD, Spoozak LA, Moadel A, Kaur G, Girda E, Goldberg GL, Einstein MH (2015) Association between statin use and endometrial cancer survival. Obstetrics Gynecology 126(1):144–150
Sanni OB, Mc Menamin ÚC, Cardwell CR, Sharp L, Murray LJ, Coleman HG (2017) Commonly used medications and endometrial cancer survival: a population-based cohort study. Br J Cancer 117(3):432–438. https://doi.org/10.1038/bjc.2017.207
Van Arsdale AR, Strickler H, Goldberg GL, Nevadunsky NS (2017) Association of statin use and disease specific survival for women with type II endometrial cancers: retrospective analysis of a 15-year experience. Gynecol Oncol 145:66
Wang A, Aragaki AK, Tang JY, Kurian AW, Manson JE, Chlebowski RT, Simon M, Desai P, Wassertheil-Smoller S, Liu S, Kritchevsky S, Wakelee HA, Stefanick ML (2016) Statin use and all-cancer survival: prospective results from the Women’s Health Initiative. Br J Cancer 115(1):129–135. https://doi.org/10.1038/bjc.2016.149
Yoon LS, Goodman MT, Rimel BJ, Jeon CY (2015) Statin use and survival in elderly patients with endometrial cancer. Gynecol Oncol 137(2):252–257. https://doi.org/10.1016/j.ygyno.2015.01.549
Liu Y, Qin A, Li T, Qin X, Li S (2014) Effect of statin on risk of gynecologic cancers: a meta-analysis of observational studies and randomized controlled trials. Gynecol Oncol 133(3):647–655. https://doi.org/10.1016/j.ygyno.2014.04.007
Segev Y, Gemer O, Helpman L, Hag-Yahia N, Eitan R, Raban O, Vaknin Z, Arie AB, Amit A, Levy T (2019) An Israeli Gynecologic Oncology Group study of statin use and endometrial cancer prognosis. Int J Gynecol Obstetr. https://doi.org/10.1002/ijgo.12981
Yu O, Boudreau DM, Buist DSM, Miglioretti DL (2009) Statin use and female reproductive organ cancer risk in a large population-based setting. Cancer Causes Control 20(5):609–616. https://doi.org/10.1007/s10552-008-9271-1
Wang Y, Ren F, Song Z, Chen P, Liu S, Ouyang L (2019) Statin use and the risk of ovarian and endometrial cancers: a meta-analysis. BMC Cancer 19(1):730
Yang J, Zhu Q, Liu Q, Wang Y, Xie W, Hu L (2017) Statin use and endometrial cancer risk: a meta-analysis. Oncotarget 8(37):62425–62434. https://doi.org/10.18632/oncotarget.18658
Ramkumar S, Raghunath A, Raghunath S (2016) Statin therapy: review of safety and potential side effects. Acta Cardiol Sin 32(6):631–639. https://doi.org/10.6515/ACS20160611A
Maji D, Shaikh S, Solanki D, Gaurav K (2013) Safety of statins. Indian J Endocrinol Metabol 17(4):636–646. https://doi.org/10.4103/2230-8210.113754
Acknowledgements
This research did not receive any specific grant from funding agencies in the public, commercial, or not-for-profit sectors.
Funding
This project received no funding.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
All authors declare no conflict of interest.
Ethical approval
This article does not contain any studies with human participants performed by any of the authors.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Hafizz, A.M.H.A., Zin, R.R.M., Aziz, N.H.A. et al. Beyond lipid-lowering: role of statins in endometrial cancer. Mol Biol Rep 47, 8199–8207 (2020). https://doi.org/10.1007/s11033-020-05760-5
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11033-020-05760-5