Abstract
Purpose
It is known that delivery rates from spontaneous conception vary according to season which may be due to cultural or environmental factors; however, conflicting data exist regarding whether outcomes from IVF are also seasonally dependent. The present study was designed to test the hypothesis that the season at oocyte retrieval is associated with livebirth after fresh transfer.
Methods
Dates of oocyte retrieval for all autologous cycles in our IVF program between January 2012 and December 2017 were categorized by season. Dates were linked to local temperature (min, max, average) and day length obtained from meteorological records. Average maximum temperature and day length were categorized into tertiles. Multivariable logistic regression, adjusted for age and quadratic age, were used to model odds (aOR) of implantation, clinical pregnancy, spontaneous abortion, and livebirth.
Results
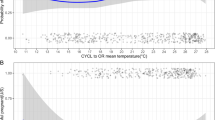
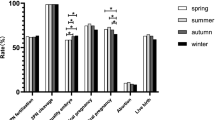
Patient characteristics were similar across seasons. As expected, temperature and day length varied by season. When compared with cycles started during winter, there was no difference in the age-adjusted odds of livebirth for the other three seasons (spring: aOR: 0.97, 95% CI: 0.82–1.13; summer: aOR: 1.05, 0.90–1.23; fall: aOR: 0.98, 0.84–1.15). There was a positive linear trend between temperature and odds of implantation, and clinical pregnancy (p value, test for linear trend (implantation, p = 0.02; clinical pregnancy, p = 0.01)) but no association with livebirth for temperature or day length.
Conclusions
We found that season at oocyte retrieval was not associated with livebirth, contrary to patterns seen in naturally conceived populations. However, our data did suggest modestly higher odds of clinical pregnancy for retrievals in June and July, and that higher temperature at time of retrieval was associated with higher odds of clinical pregnancy but not livebirth.



Similar content being viewed by others
References
Rosenberg HM. Seasonal variation of births, United States, 1933-63. Vital Health Stat 1. 1966;21(9):1–59.
Cowgill U. Season of birth in man, contemporary situation with special refernce to Europe and the Southern Hemisphere. Ecology. 1965;47(4):614–23.
Lam DA, Miron JA. Seasonality of births in human populations. Soc Biol. 1991;38(1-2):51–78.
Becker S. Seasonal patterns of births and conception throughout the world. Adv Exp Med Biol. 1991;286:59–72.
Becker S. Seasonality of deaths in Matlab, Bangladesh. Int J Epidemiol. 1981;10(3):271–80.
James WH. Seasonal variation in human births. J Biosoc Sci. 1990;22(1):113–9.
Wesselink AK, Wise LA, Hatch EE, Mikkelsen EM, Sørensen HT, Riis AH, et al. Seasonal patterns in fecundability in North America and Denmark: a preconception cohort study. Hum Reprod. 2020:dez265. https://doi.org/10.1093/humrep/dez265.
Lam DA, Miron JA. Global patterns of seasonal variation in human fertility. Ann N Y Acad Sci. 1994;709:9–28.
Seiver DA. Trend and variation in the seasonality of U.S. fertility, 1947-1976. Demography. 1985;22(1):89–100.
Russell D, Douglas AS, Allan TM. Changing seasonality of birth--a possible environmental effect. J Epidemiol Community Health. 1993;47(5):362–7. https://doi.org/10.1136/jech.47.5.362.
Bronson FH. Seasonal variation in human reproduction: environmental factors. Q Rev Biol. 1995;70(2):141–64.
Robinson D, Rock J. Intrascrotal hyperthermia induced by scrotal insulation: effect on spermatogenesis. Obstet Gynecol. 1967;29(2):217–23.
Rojansky N, Brzezinski A, Schenker JG. Seasonality in human reproduction: an update. Hum Reprod. 1992;7(6):735–45.
Liu X, Bai H, Mol BW, Shi W, Gao M, Shi J. Seasonal variability does not impact in vitro fertilization success. Sci Rep. 2019;9(1):17185. https://doi.org/10.1038/s41598-019-53919-3.
Kirshenbaum M, Ben-David A, Zilberberg E, Elkan-Miller T, Haas J, Orvieto R. Influence of seasonal variation on in vitro fertilization success. PLoS One. 2018;13(7):e0199210-e. https://doi.org/10.1371/journal.pone.0199210.
Fleming C, Nice L, Hughes AO, Hull MG. Apparent lack of seasonal variation in implantation rates after in-vitro fertilization. Hum Reprod. 1994;9(11):2164–6.
Dunphy BC, Anderson-Sykes S, Brant R, Pattinson HA, Greene CA. Human embryo implantation following in-vitro fertilization: is there a seasonal variation? Hum Reprod. 1995;10(7):1825–7. https://doi.org/10.1093/oxfordjournals.humrep.a136184.
Wunder DM, Limoni C, Birkhäuser MH, Swiss F-G. Lack of seasonal variations in fertilization, pregnancy and implantation rates in women undergoing IVF. Hum Reprod. 2005;20(11):3122–9. https://doi.org/10.1093/humrep/dei177.
Zhao M, Zhang H, Waters THB, Chung JPW, Li TC, Chan DYL. The effects of daily meteorological perturbation on pregnancy outcome: follow-up of a cohort of young women undergoing IVF treatment. Environmental health: a global access science source. 2019;18(1):103. https://doi.org/10.1186/s12940-019-0538-7.
Chamoun D, Udoff L, Scott L, Magder L, Adashi EY, McClamrock HD. A seasonal effect on pregnancy rates in an in vitro fertilization program. J Assist Reprod Genet. 1995;12(9):585–9. https://doi.org/10.1007/bf02212579.
Rojansky N, Benshushan A, Meirsdorf S, Lewin A, Laufer N, Safran A. Seasonal variability in fertilization and embryo quality rates in women undergoing IVF. Fertil Steril. 2000;74(3):476–81.
Stolwijk AM, Reuvers MJ, Hamilton CJ, Jongbloet PH, Hollanders JM, Zielhuis GA. Seasonality in the results of in-vitro fertilization. Hum Reprod. 1994;9(12):2300–5. https://doi.org/10.1093/oxfordjournals.humrep.a138441.
Weigert M, Feichtinger W, Kulin S, Kaali SG, Dorau P, Bauer P. Seasonal influences on in vitro fertilization and embryo transfer. J Assist Reprod Genet. 2001;18(11):598–602. https://doi.org/10.1023/a:1013160905497.
R: A language and environment for statistical computing. Vienna, Austria. R Core Team 2017.
gee: Generalized Estimation Equation Solver. In: Ripley. VJCPtRbTLaB, editor.2015.
Vandekerckhove F, Van der Veken H, Tilleman K, De Croo I, Van den Abbeel E, Gerris J, et al. Seasons in the sun: the impact on IVF results one month later. Facts Views Vis Obgyn. 2016;8(2):75–83.
Khoudja RY, Xu Y, Li T, Zhou C. Better IVF outcomes following improvements in laboratory air quality. J Assist Reprod Genet. 2013;30(1):69–76. https://doi.org/10.1007/s10815-012-9900-1.
Perin PM, Maluf M, Czeresnia CE, Januário DANF, Saldiva PHN. Impact of short-term preconceptional exposure to particulate air pollution on treatment outcome in couples undergoing in vitro fertilization and embryo transfer (IVF/ET). J Assist Reprod Genet. 2010;27(7):371–82. https://doi.org/10.1007/s10815-010-9419-2.
Conforti A, Mascia M, Cioffi G, De Angelis C, Coppola G, De Rosa P, et al. Air pollution and female fertility: a systematic review of literature. Reprod Biol Endocrinol. 2018;16(1):117. https://doi.org/10.1186/s12958-018-0433-z.
Choe SA, Jun YB, Lee WS, Yoon TK, Kim SY. Association between ambient air pollution and pregnancy rate in women who underwent IVF. Hum Reprod. 2018;33(6):1071–8. https://doi.org/10.1093/humrep/dey076.
Mortimer D, Cohen J, Mortimer ST, Fawzy M, McCulloh DH, Morbeck DE, et al. Cairo consensus on the IVF laboratory environment and air quality: report of an expert meeting. Reprod BioMed Online. 2018;36(6):658–74. https://doi.org/10.1016/j.rbmo.2018.02.005.
Dawson J, Adams P, Pandis S. Sensitivity of PM 2.5 to climate in the Eastern US: a modeling case study. Atmos Chem Phys. 2007;7(16):4295–309.
Kroll MH, Bi C, Garber CC, Kaufman HW, Liu D, Caston-Balderrama A, et al. Temporal relationship between vitamin D status and parathyroid hormone in the United States. PLoS One. 2015;10(3):e0118108-e. https://doi.org/10.1371/journal.pone.0118108.
Rudick B, Ingles S, Chung K, Stanczyk F, Paulson R, Bendikson K. Characterizing the influence of vitamin D levels on IVF outcomes. Hum Reprod. 2012;27(11):3321–7. https://doi.org/10.1093/humrep/des280.
Franasiak JM, Molinaro TA, Dubell EK, Scott KL, Ruiz AR, Forman EJ, et al. Vitamin D levels do not affect IVF outcomes following the transfer of euploid blastocysts. Am J Obstet Gynecol. 2015;212(3):315 e1-e6.
Author information
Authors and Affiliations
Corresponding author
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
ESM 1
(DOCX 27 kb)
Rights and permissions
About this article
Cite this article
Farland, L.V., Correia, K.F.B., Missmer, S.A. et al. Seasonal variation, temperature, day length, and IVF outcomes from fresh cycles. J Assist Reprod Genet 37, 2427–2433 (2020). https://doi.org/10.1007/s10815-020-01915-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10815-020-01915-2