Abstract
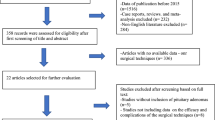
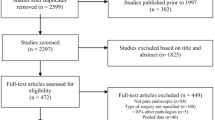
A preferred treatment for residual/recurrent pituitary adenomas has not been established. The existence of higher complication rates for revision surgeries remains under debate. This study aimed to compare complication rates of primary and revision transsphenoidal endoscopic surgeries and to identify risk factors for complications. Data from 144 primary and 39 revision surgeries were analysed. The surgical complications evaluated were intraoperative and postoperative cerebrospinal fluid (CSF) leaks; meningitis; permanent diabetes insipidus (DI) and hypopituitarism; worsening visual acuity; ophthalmoplegias; visual field defects; otorhinolaryngological, systemic and vascular complications; and death. The variables that were potentially associated with surgical complications were gender, age, comorbidities, lumbar drain use, duration of lumbar drain use, invasion of the sphenoid and cavernous sinuses, presence and degree of suprasellar expansion, preoperative identification of the pituitary, CSF leaks and intraoperative pituitary identification. Intraoperative CSF leaks, visual field losses and worsening visual acuity were more common for revision surgeries. There were no between-group differences in the occurrence of postoperative CSF leaks; systemic, vascular and otorhinolaryngological complications; meningitis; DI and hypopituitarism; ophthalmoplegias; or death. Intraoperative identification of the pituitary was associated with lower rates of permanent DI and hypopituitarism, systemic complications, intraoperative CSF leaks and worsening visual acuity. Suprasellar expansion increased the risk of intraoperative CSF leaks but not endocrinological deficits or visual impairment. Intraoperative CSF leaks were associated with postoperative CSF leaks, meningitis, anterior hypopituitarism, DI and worsening visual acuity. Intraoperative CSF leaks, worsening visual acuity and visual field losses were more common in reoperated patients.
Similar content being viewed by others
Data availability
The datasets generated and/or analysed during the current study, including patient-level data, are available from the corresponding author upon request and in the library of the Faculty of Medicine of the Federal University of Minas Gerais.
References
Tajudeen BA, Mundi J, Suh JD, Bergsneider M, Wang MB (2015) Endoscopic endonasal surgery for recurrent pituitary tumors: technical challenges to the surgical approach. J Neurol Surg B Skull Base 76:50–56
Linsler S, Hero-Gross R, Friesenhahn-Ochs B, Sharif S, Lammert F, Oertel J (2017) Preservation of hormonal function by identifying pituitary gland at endoscopic surgery. J Clin Neurosci 43:240–246
Halvorsen H, Ramm-Pettersen J, Josefsen R, Ronning P, Reinlie S, Meling T, Berg-Johnsen J, Bollerslev J, Helseth E (2014) Surgical complications after transsphenoidal microscopic and endoscopic surgery for pituitary adenoma: a consecutive series of 506 procedures. Acta Neurochir 156:441–449
Valderrábano P, Aller J, García-Valdecasas L, García-Uría J, Martín L, Palacios N, Estrada J (2014) Results of repeated transsphenoidal surgery in Cushing’s disease. Long-term follow-up. Endocrinol Nutr 61:176–183
Negm HM, Al-Mahfoudh R, Pai M, Singh H, Cohen S, Dhandapani S, Anand VK, Schwartz TH (2017) Reoperative endoscopic endonasal surgery for residual or recurrent pituitary adenomas. J Neurosurg 127:397–408
Patil CG, Veeravagu A, Prevedello DM, Katznelson L, Vance ML, Laws ER (2008) Outcomes after repeat transsphenoidal surgery for recurrent Cushing’s disease. Neurosurgery 63:266–270; discussion 270–261
Dickerman RD, Oldfield EH (2002) Basis of persistent and recurrent cushing disease: an analysis of findings at repeated pituitary surgery. J Neurosurg 97:1343–1349
Chang EF, Sughrue ME, Zada G, Wilson CB, Blevins LS, Kunwar S (2010) Long term outcome following repeat transsphenoidal surgery for recurrent endocrine-inactive pituitary adenomas. Pituitary 13:223–229
Do H, Kshettry VR, Siu A, Belinsky I, Farrell CJ, Nyquist G, Rosen M, Evans JJ (2017) Extent of resection, visual, and endocrinologic outcomes for endoscopic endonasal surgery for recurrent pituitary adenomas. World Neurosurg 102:35–41
Przybylowski CJ, Dallapiazza RF, Williams BJ, Pomeraniec IJ, Xu Z, Payne SC, Laws ER, Jane JA (2017) Primary versus revision transsphenoidal resection for nonfunctioning pituitary macroadenomas: matched cohort study. J Neurosurg 126:889–896
Knosp E, Steiner E, Kitz K, Matula C (1993) Pituitary adenomas with invasion of the cavernous sinus space: a magnetic resonance imaging classification compared with surgical findings. Neurosurgery 33:610–617; discussion 617–618
Yamada S, Fukuhara N, Oyama K, Takeshita A, Takeuchi Y (2010) Repeat transsphenoidal surgery for the treatment of remaining or recurring pituitary tumors in acromegaly. Neurosurgery 67:949–956
Jahangiri A, Wagner J, Han SW, Zygourakis CC, Han SJ, Tran MT, Miller LM, Tom MW, Kunwar S, Blevins LS, Aghi MK (2014) Morbidity of repeat transsphenoidal surgery assessed in more than 1000 operations. J Neurosurg 121:67–74
Wilson TJ, McKean EL, Barkan AL, Chandler WF, Sullivan SE (2013) Repeat endoscopic transsphenoidal surgery for acromegaly: remission and complications. Pituitary 16:459–464
Dhandapani S, Singh H, Negm HM, Cohen S, Anand VK, Schwartz TH (2016) Cavernous sinus invasion in pituitary adenomas: systematic review and pooled data meta-analysis of radiologic criteria and comparison of endoscopic and microscopic surgery. World Neurosurg 96:36–46
Hardy J (1969) Transphenoidal microsurgery of the normal and pathological pituitary. Clin Neurosurg 16:185–217
Hardy J, Vezina JL (1976) Transsphenoidal neurosurgery of intracranial neoplasm. Adv Neurol 15:261–273
Wilson CB (1984) A decade of pituitary microsurgery. The Herbert Olivecrona lecture. J Neurosurg 61:814–833
Hollander M, Wolfe DA (1999) Nonparametric statistical methods. John Wiley & Sons, New York, Chichester
Agresti A (2002) Categorical data analysis. Wiley-Interscience, New York, Chichester
Efroymson M (1960) Multiple regression analysis. In: Ralston A, Wilf HS (eds) Mathematical methods for digital computers. John Wiley & Sons, New York, NY, pp 191–203
Liu JK, Fleseriu M, Delashaw JB, Ciric IS, Couldwell WT (2007) Treatment options for cushing disease after unsuccessful transsphenoidal surgery. Neurosurg Focus 23:E8
Krings JG, Kallogjeri D, Wineland A, Nepple KG, Piccirillo JF, Getz AE (2015) Complications following primary and revision transsphenoidal surgeries for pituitary tumors. Laryngoscope 125:311–317
Cavallo LM, Solari D, Tasiou A, Esposito F, de Angelis M, D’Enza AI, Cappabianca P (2013) Endoscopic endonasal transsphenoidal removal of recurrent and regrowing pituitary adenomas: experience on a 59-patient series. World Neurosurg 80:342–350
Ciric I, Ragin A, Baumgartner C, Pierce D (1997) Complications of transsphenoidal surgery: results of a national survey, review of the literature, and personal experience. Neurosurgery 40:225–236; discussion 236–227
Berker M, Hazer DB, Yücel T, Gürlek A, Cila A, Aldur M, Onerci M (2012) Complications of endoscopic surgery of the pituitary adenomas: analysis of 570 patients and review of the literature. Pituitary 15:288–300
Magro E, Graillon T, Lassave J, Castinetti F, Boissonneau S, Tabouret E, Fuentes S, Velly L, Gras R, Dufour H (2016) Complications related to the endoscopic endonasal transsphenoidal approach for nonfunctioning pituitary macroadenomas in 300 consecutive patients. World Neurosurg 89:442–453
Zhao B, Wei YK, Li GL, Li YN, Yao Y, Kang J, Ma WB, Yang Y, Wang RZ (2010) Extended transsphenoidal approach for pituitary adenomas invading the anterior cranial base, cavernous sinus, and clivus: a single-center experience with 126 consecutive cases. J Neurosurg 112:108–117
Zhan R, Xu G, Wiebe TM, Li X (2015) Surgical outcomes of the endoscopic transsphenoidal route to pituitary tumours in paediatric patients >10 years of age: 5 years of experience at a single institute. Arch Dis Child 100:774–778
Zhou Q, Yang Z, Wang X, Wang Z, Zhao C, Zhang S, Li P, Li S, Liu P (2017) Risk factors and management of intraoperative cerebrospinal fluid leaks in endoscopic treatment of pituitary adenoma: analysis of 492 patients. World Neurosurg 101:390–395
Boling CC, Karnezis TT, Baker AB, Lawrence LA, Soler ZM, Vandergrift WA, Wise SK, DelGaudio JM, Patel ZM, Rereddy SK, Lee JM, Khan MN, Govindaraj S, Chan C, Oue S, Psaltis AJ, Wormald PJ, Trosman S, Stokken J, Woodard T, Sindwani R, Schlosser RJ (2016) Multi-institutional study of risk factors for perioperative morbidity following transnasal endoscopic pituitary adenoma surgery. Int Forum Allergy Rhinol 6:101–107
Yano S, Hide T, Shinojima N (2017) Efficacy and complications of endoscopic skull base surgery for giant pituitary adenomas. World Neurosurg 99:533–542
Constantino ER, Leal R, Ferreira CC, Acioly MA, Landeiro JA (2016) Surgical outcomes of the endoscopic endonasal transsphenoidal approach for large and giant pituitary adenomas: institutional experience with special attention to approach-related complications. Arq Neuropsiquiatr 74:388–395
Smith TR, Hulou MM, Huang KT, Nery B, de Moura SM, Cote DJ, Laws ER (2015) Complications after transsphenoidal surgery for patients with Cushing’s disease and silent corticotroph adenomas. Neurosurg Focus 38:E12
Zhan R, Ma Z, Wang D, Li X (2015) Pure endoscopic endonasal transsphenoidal approach for nonfunctioning pituitary adenomas in the elderly: surgical outcomes and complications in 158 patients. World Neurosurg 84:1572–1578
Tabaee A, Anand VK, Barrón Y, Hiltzik DH, Brown SM, Kacker A, Mazumdar M, Schwartz TH (2009) Endoscopic pituitary surgery: a systematic review and meta-analysis. J Neurosurg 111:545–554
Jane JA, Thapar K, Laws ER (2011) Pituitary tumors: functioning and nonfunctioning. In: Winn HR (ed) Youmans neurological surgery. Elsevier, Philadelphia, PA, pp 1476–1510
Almeida JP, Ruiz-Treviño AS, Liang B, Omay SB, Shetty SR, Chen YN, Anand VK, Grover K, Christos P, Schwartz TH (2017) Reoperation for growth hormone-secreting pituitary adenomas: report on an endonasal endoscopic series with a systematic review and meta-analysis of the literature. J Neurosurg 129:404–416
Wang F, Zhou T, Wei S, Meng X, Zhang J, Hou Y, Sun G (2015) Endoscopic endonasal transsphenoidal surgery of 1,166 pituitary adenomas. Surg Endosc 29:1270–1280
Gondim JA, Almeida JP, Albuquerque LA, Schops M, Gomes E, Ferraz T, Sobreira W, Kretzmann MT (2011) Endoscopic endonasal approach for pituitary adenoma: surgical complications in 301 patients. Pituitary 14:174–183
Graham SM, Iseli TA, Karnell LH, Clinger JD, Hitchon PW, Greenlee JD (2009) Endoscopic approach for pituitary surgery improves rhinologic outcomes. Ann Otol Rhinol Laryngol 118:630–635
Kumar S, Darr A, Hobbs CG, Carlin WV (2012) Endoscopic, endonasal, trans-sphenoidal hypophysectomy: retrospective analysis of 171 procedures. J Laryngol Otol 126:1033–1040
Hofstetter CP, Nanaszko MJ, Mubita LL, Tsiouris J, Anand VK, Schwartz TH (2012) Volumetric classification of pituitary macroadenomas predicts outcome and morbidity following endoscopic endonasal transsphenoidal surgery. Pituitary 15:450–463
Rudnik A, Zawadzki T, Gałuszka-Ignasiak B, Bazowski P, Duda I, Wojtacha M, Rudnik AI, Krawczyk I (2006) Endoscopic transsphenoidal treatment in recurrent and residual pituitary adenomas—first experience. Minim Invasive Neurosurg 49:10–14
Chowdhury T, Prabhakar H, Bithal PK, Schaller B, Dash HH (2014) Immediate postoperative complications in transsphenoidal pituitary surgery: a prospective study. Saudi J Anaesth 8:335–341
Petry C, Leães CG, Pereira-Lima JF, Gerhardt KD, Sant GD, Oliveira MC (2009) Oronasal complications in patients after transsphenoidal hypophyseal surgery. Braz J Otorhinolaryngol 75:345–349
Benveniste RJ, King WA, Walsh J, Lee JS, Delman BN, Post KD (2005) Repeated transsphenoidal surgery to treat recurrent or residual pituitary adenoma. J Neurosurg 102:1004–1012
Ammirati M, Wei L, Ciric I (2013) Short-term outcome of endoscopic versus microscopic pituitary adenoma surgery: a systematic review and meta-analysis. J Neurol Neurosurg Psychiatry 84:843–849
Heringer LC, de Oliveira MF, Rotta JM, Botelho RV (2016) Effect of repeated transsphenoidal surgery in recurrent or residual pituitary adenomas: a systematic review and meta-analysis. Surg Neurol Int 7:14
D’Anza B, Tien D, Stokken JK, Recinos PF, Woodard TR, Sindwani R (2016) Role of lumbar drains in contemporary endonasal skull base surgery: meta-analysis and systematic review. Am J Rhinol Allergy 30:430–435
Author information
Authors and Affiliations
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
This study was approved by the Research Ethics Committee (Comitê de Ética em Pesquisa, COEP) of the Federal University of Minas Gerais, CAAE project - 54787216.7.0000.5149, on 6 July 2016.
Informed consent
Although informed consent is not required in this type of study, it was obtained from all patients.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
do Amaral, L.C., Reis, B.L., Ribeiro-Oliveira, A. et al. Comparative study of complications after primary and revision transsphenoidal endoscopic surgeries. Neurosurg Rev 44, 1687–1702 (2021). https://doi.org/10.1007/s10143-020-01360-w
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10143-020-01360-w